
Anaesthetic Concerns in a Child with Lesch-Nyhan Syndrome
*Corresponding Author(s):
Sheetal KotegarDepartment Of Anesthesiology, Indira Gandhi Institute Of Child Health, Bangalore, India
Tel:+91 9972323069,
Email:sheetal.kotegar@gmail.com
Abstract
Lesch-Nyhan syndrome is a rare X-linked recessive disorder caused by a deficiency of Hypoxanthine-Guanine Phosphoribosyl Transferase (HGPRT) enzyme. The patients with Lesch-Nyhan Syndrome will have spasticity due to which there could be several problems such as positioning, difficult intravenous cannulation and difficult airway. And these patients will have self-mutilating behavior and lack of pain sensation. Bradycardia, pulmonary aspiration, convulsion are the important causes of death. Anesthetic management of these patients in pediatric age group is not well described. Here, we report our anesthesia experience in a 3 years-old child who was posted for debridement of right great toe with Lesch-Nyhan syndrome. Patients with Lesch-Nyhan syndrome should be induced in titrated doses and no analgesia is required because of lack of sensation. Careful monitoring is required during perioperative and post-operative period as they are more prone for bradycardia, apnea and aspiration.
Keywords
INTRODUCTION
Lesch-Nyhan syndrome is a rare, sex linked recessive anomaly consisting of a deficiency in the production of hypoxanthine phosphoribosyl- transferase that leads to the overproduction of purine and the accumulation of uric acid [1]. Lesch–Nyhan syndrome almost always affects males, with very few cases reported in females [2]. Certain characteristic neurological features include choreoathetosis, spasticity and mental retardation resulting in self-mutilation through biting and scratching [1]. Although complete HPRT deficiency typically results in the stereotypical LND syndrome, partial deficiency more often causes a phenotype in which some features are attenuated or absent [3]. Collectively, these patients are labelled LND variants. All of these patients produce excess uric acid, but broad variations in the neurological and behavioral features have been described [3]. Hyperuricemia is associated with nephropathy, urinary tract calculi, arthritis, tophi. So these children may present for urinary tract, orthopedic surgeries or any unrelated surgical problems. There are only a few case reports regarding the anesthetic experience with these patients [2]. This report will present our anesthetic experience in a patient with Lesch-Nyhan syndrome who underwent surgery for debridement of right great toe.
CASE REPORT
A 3 year old boy weighing 15kg was scheduled for debridement of right great toe under general anesthesia. Child had a history of self-mutilating behavior of biting fingers, multiple injuries due to lack of sensation, delayed development, impaired sensation and speech disorder (Figure 1). Preoperative airway evaluation of the child revealed micrognathia, short neck, absent teeth and large glossy tongue (Figure 2). Laboratory test reports were as follows: Hemoglobin-12.4gm/dl, platelets-1.8lakh, Total count-6800, Serum creatinine-1mg/dl, blood urea- 15mg/dl, serum uric acid levels were raised to 10.2 mg/dl. Serum electrolytes were in the normal range. Chest x-ray was normal. There was no cardiac or renal defect in this case.
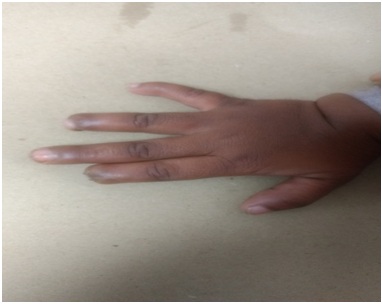
Figure 1: Injured fingers.
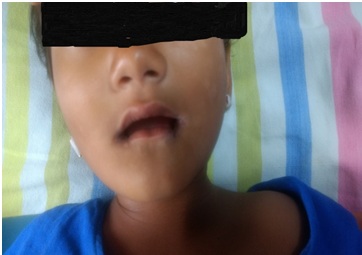
Figure 2: Erosions of cornera of lips.
The above physical findings predicted a difficult airway management. Therefore, before anesthesia induction all equipments were organized for difficult airway management. Child was premedicated with oral midazolam 0.5mg/kg in the recovery room 30minutes before induction. Child was shifted to operation theatre and all the monitors connected. Baseline recording of heart rate, blood pressure, oxygen saturation with pulse oximeter, temperature was made. Child was induced with sevoflurane + Oxygen mixture, 22G intravenous cannula secured. Intravenous fluids RL was connected and fluids given based on Holiday segar formula. Cannulation was not difficult in this case. Sevoflurane decreased and injection propofol 1mg/kg and fentanyl 1.5µg/kg given intravenously in titrated dose. Child was mask ventilated with Jackson rees circuit with oxygen + air + sevoflurane during induction. Injection dexamethasone 0.1mg/kg and ondansetron 0.1mg/kg was given after induction of anaesthesia. There was no difficulty in mask ventilation in this case. After confirming the depth of anaesthesia IGEL 2 size was inserted. Bilateral equal air entry was confirmed. Suction catheter passed into the gastric port of IGEL and fixed in place. Anaesthesia was maintained with O2 + Air + isoflurane 0.6% + IPPV. No other analgesics or regional block was given. There was no response to pain. Child was properly positioned in supine position with padding of the pressure points. Pressure points were padded and the surgical team was warned so as not to compress the extremities. Heart rate, SpO2, blood pressure, ECG, ETco2 and temperature was monitored throughout the surgery. Vitals were normal and stable during surgery. Surgery lasted for 45min.
During recovery occasional ectopics were noted, bardycardia was noted with lowest recorded heart rate of 60bpm. Bradycardia did not respond to injection glycopyrrolate 0.01mg/kg so injection atropine 0.02mg/kg was given intravenously. Heart rate resumed to normal values. Child was extubated once there was adequate spontaneous respiration. There was decreased requirement of anaesthetic drugs throughout the surgery. The extremities were safe and there were no other complications.
Child was shifted to recovery and put in left lateral chin up position with oxygen 4L with facemask. Child was monitored and kept in the recovery till he was fully awake and then transferred to ward. There were no postoperative complications. There was no postoperative pain. Post-operative pain score recorded 3 hours after surgery on visual analog scale was 0.
DISCUSSION
Lesch-Nyhan syndrome is characterized by cognitive impairment, hypotonia at rest, choreoathetosis, hyperuricaemia and the hallmark symptom of severe and involuntary self-mutilation. The patients with Lesch-Nyhan Syndrome have several problems like positioning in operating room, difficult intravenous cannulation and difficult airway because of the spasticity [4]. Also, these patients are at risk of bradycardia, pulmonary aspiration, convulsion and sudden death, and an increased incidence of vomiting. The anesthetic considerations in Lesch–Nyhan syndrome are because of the functional disturbances created by the disorder and the effect on metabolism and excretion of drugs [2].
In our case we used propofol because of its antiemetic properties. It also increases urine uric acid excretion and is beneficial for such patients [5]. These children are more prone to nausea, vomiting [2].Metabolism of barbiturates, ketamine, or etomidate remains unaffected and isoflurane can also be safely used [6]. Succinylcholine is preferably avoided because of abnormal potassium influx [7]. Atracurium is safe for muscle relaxation [8]. These children will have congenital insensitivity to pain [9]. There was no response to pain in this case. There was no postoperative pain.
Perioperative proper positioning, use of protective padding, and avoidance of contact with hard surfaces are the protective measures to avoid direct pressure on susceptible skin and peripheral nerves [10].
In our case, there was decreased anaesthetic requirement throughout the procedure. There was delayed recovery for 15min. Child was intermittently going into apnea during which there were occasional ectopics and bradycardia which responded to injection atropine. These children are more prone to bradycardia and apnea so vigilant monitoring and intervention is required for such cases [2].
A case report published by Salhotra R et al., reports the rare occurrence of a tracheal diverticulum associated with Lesch-Nyhan syndrome in a 11 year old boy [11]. They had difficulty in securing the airway.
In conclusion, thorough preoperative evaluation of the child to assess the airway, cannulation and any associated abnormalities. Induction should be done with titrated doses. Precautions should be taken to avoid aspiration. Careful monitoring throughout the surgery to prevent complications and sudden death. No analgesics required due to lack of sensation in these patients. Patients should be closely monitored in the postoperative period because of the risk of sudden death and aspiration. Anaesthetic management should be individualized for each case of Lesch-Nyhan syndrome based on the associated conditions.
REFERENCES
- Pralong E, Pollo C, Coubes P, Bloch J, Roulet E, et al. (2005) Electrophysiological characteristics of limbic and motor globus pallidus internus (GPI) neurons in two cases of Lesch-Nyhan syndrome. Neurophysiol Clin 35: 168-173.
- Larson LO, Wilkins RG (1985) Anesthesia and the Lesch Nyhan syndrome. Anesthesiology 63: 197-199.
- Jinnah HA, Ceballos-Picot I, Torres RJ, Visser JE, Schretlen DJ, et al. (2010) Attenuated variants of Lesch-Nyhan disease. Brain 133: 671-689.
- Nyhan WL (1974) The Lesch Nyhan Syndrome. Adv Nephrol Necker Hosp 3: 59-70.
- Masuda A, Asahi T, Sakamaki M, Nakamaru K, Hirota K, et al. (1997) Uric acid excretion increases during propofol anesthesia. Anesth Analg 85: 144-148.
- Katz J, Benumof J, Kadis LB (1981) Anesthesia and uncommon diseases : pathophysiologic and clinical correlations (2ndedn)., Saunders, Philadelphia, USA.
- Gronert GA, Theye RA (1975) Pathophysiology of hyperkalemia induced by succinylcholine. Anesthesiology 43: 89-99.
- Stenlake JB, Waigh RD, Urwin J, Dewar GH, Coker BB (1983) Atracurium: Conception and inception. Br J Anaesth. 55: 3-10.
- Kapasi AY, Trasi SS, Khopkar US, Wadhwa SL (1992) Congenital indifference to pain. Indian J Dermatol Venereol Leprol 58: 273-276.
- Sawyer RJ, Richmond MN, Hickey JD, Jarratt JA (2000) Peripheral nerve injuries associated with anaesthesia. Anaesthesia 55: 980-991.
- Salhotra R, Sharma C, Tyagi A, Kumar S, Sethi A, et al. An unanticipated difficult airway in Lesch-Nyhan syndrome. J Anaesthesiol Clin Pharmacol 28: 239-241.
Citation: Reddy R, Sheetal K (2018) Anaesthetic Concerns in a Child with Lesch-Nyhan Syndrome. J Anesth Clin Care. 5: 026.
Copyright: © 2018 Rachana Reddy, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

