ABSTRACT
Extra skeletal osteochondroma is a rare benign soft tissue tumor. We report the case of a 50-year-old male who presented with a painful nodular mass in the plantar aspect of his left forefoot. Radiological findings showed ill-defined mineralization centered at the base of the proximal phalanx of third toe with no significant articular erosions or osteoarthrosis at the third MTP joint. Excision biopsy of the nodule was done. The lesion was sent off for histopathology, confirming diagnosis of benign osteochondromatous lesion beneath the left 3rd MTP joint with no evidence of malignancy. Intraoperatively, it was visible that the lesion was exclusively in soft tissue, there was no bony connection. There was no post-operative complication and no signs of relapse on 6 months follow up after surgery. In conclusion, an osteochondromatous lesion should be considered when a distinct, ossified mass is localized in the fibro-connective soft tissues of the distal extremities.
Keywords: Benign osteochondromatous lesion; Bone tumors; Extraskeletal osteochondroma; Osteo chondroma; Metatarsophalangeal joint; Proximal phalanx; Soft tissues
Introduction
The occurrence of osteochondroma, a benign bone lesion, is common, constituting to 20-50% of all benign bone tumors, 10-15% of all bone tumors; 3-5% of these occur in foot [1,2]. Long bones such as femur, tibia and humerus are most commonly affected. Bony sites of involvements in the foot include the calcaneus and talus [3-5]. Also, there are juxtacortical or surface osteochondromas of bone, that arise just outside the cortex and are composed of different histologic types are reported in the literature [6,7]. Among these, there may be fibrous variety which may be counted as extraskeletal [6,7]. Osteochondromas are generally not found in soft tissues, and if they occur without any osseous or intra-articular involvement, they are described as extra skeletal osteochondromas. Extraskeletal or soft tissue chondroma, extra osseous chondroma, chondroma of soft parts, tenosynovial chondroma and cartilaginous tumor of the soft tissue are just of the few other names used to describe this benign solitary cartilaginous mass in the extra synovial tissue [8]. Extra skeletal osteochondromas arising in the foot and ankle are reported in literature [9-11]. Local recurrence after resection is uncommon, which is reported to be <2% [12].Extra skeletal osteochondroma is relatively rare benign soft tissue tumor. It is slow growing and mostly arises within the soft tissues of hands and feet. It presents itself as a small discrete calcified mass that rarely exceeds 2-3cm in its greatest dimension [13,14]. This tumor is not specific to either gender, or many studies show that it mainly occurs in patients that are 20 years or older with peak occurrence during the 3rd and 6th decades [14]. It can present itself in many ways initially. Few osteochondromas develop in an idiopathic manner and it is common to have the lesion in association with trauma [14,15]. Literature also shows that the selesions have developed post radiotherapy in children up to 10 years. Because of its variable and worrisome radiological features and histological presentation, it is usually mistaken for an osteosarcoma [13,14]. Local excision is known as the standard treatment if tumor is symptomatic [16].We report a case of benign osteochondromatous lesion in the soft tissue on the plantar aspect of the left 3rd MTP joint and proximal phalanx.
Case Report
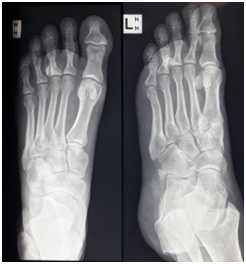
A 50-year-old man, who worked as an operator of Coal Loader presented with a nodular mass in the plantar aspect of his left forefoot. He reported that he has had for many years. It had become so painful, that he could hardly walk or stand and was struggling to do his daily activities. This related back to an injury to the left forefoot when he was riding motorcycle in 1995 and had collision with a stump. He did have significant contusions and soft tissue swelling at that time, as he visited the hospital, but was treated conservatively. He was not diabetic, a nonsmoker, had no medical co morbidities. He slept comfortably at night and had been able to get back to riding motorcycles. He was unable to do mountain biking and if he would stand for greater than an hour, it became very painful.On examination, he was a fit looking man who walked with a subtle limp. Getting up on tiptoes aggravated his limp. His left forefoot was well-aligned, but he had a hard-nodular mass beneath his 3rd MTP joint. This measured approximately 3 × 2cm. He had associated callus over the lesion on the plantar aspect of his left forefoot. He had an intact sensation and blood supply was satisfactory. His plain radiograph (Figure 1and 2) showed mineralization mimicking heterotrophic ossification centered at the base of the proximal phalanx of third toe with no significant articular erosions or osteoarthrosis at the third MTP joint. This picture was similar to heterotopic ossification in the soft tissues on the plantar aspect of the left 3rd MTP joint and proximal phalanx. It looked consistent with heterotopic bone secondary to trauma, as described. On CT scan (Figure 3A, 3B and Figure 4), there was an area of hyper-density in relation to the lateral aspect of the base of the proximal phalanx of the 3rd toe extending over around a centimeter. Separate to the phalanx and extending laterally between the 3rd and 4th toes and over the plantar aspect of the 3rd toe there was a mixed density calcified/soft tissue mass which in total measured 20mm × 24mm × 19mm. The soft tissue component was mainly medial. It measured 14mm × 14mm. The joint space was intact. There was no other focal abnormality.
Excision biopsy was planned for this mass, suspecting a myositis, heterotopic ossification or a possible fragment of an osteochondroma. Patient was informed before the surgery regarding the risks, which included infection, DVT, neurovascular damage or recurrence. Under general anesthesia, 3cm incision was performed on the plantar aspect of forefoot, just beneath the palpable lump and excision of the mass was done. The lesion was sent off for histopathology to exclude any neoplasia. Intraoperatively, it was visible that this mass with a thin capsule was exclusively in the soft tissues and there were no adhesions to the bone.On histopathology, sections were reported as benign osteochondromatous lesion within fibro connective tissue. The lesion showed hyaline cartilage, enchondral ossification and bone trabeculae. Many bone trabeculae showed osteoblastic rimming and occasional osteoclastic activity. Vascular congestion and pigment laden macrophages were present. There was no evidence of malignancy. These features were those of an osteochondroma which could be connected to adjacent long bone or purely soft tissue (soft tissue osteochondroma. During his last follow up, which is 6 months post-surgery, there were no signs of local recurrence?
Discussion
Extra skeletal osteochondroma is a slow-growing tumor. The highest incidences reported are in the hands and feet. The foot is the second most common are after the fingers, where more than 80% of soft tissue chondroma are found [17]. Sporadic cases have been reported in the skin, nape of the neck, oral cavity, buttocks, thighs, knees, pharynx and parotid gland [13,18-21]. The causes of extra skeletal osteochondroma are still unknown, but there is one.Hypothesis that it originates from pluripotent cell lines derived from the joint synovium, tenosynovium, or connective tissue. Another theory states, that it originates from metaplasia tendon sheaths in the hands and feet [1,8,17-21]. There is one more theory, that extraskeletal osteochondroma arises from fibroblasts in the connective tissue distant from bone and joints because of unknown stimuli [21]. Extra skeletal osteochondroma generally presents itself clinically as a painless, slowly enlarging nodular soft tissue mass that is usually present for some time before diagnosis. In 20% patients however, the lesion is painful and tender, especially if located on the plantar side of the foot [14]. A case of a 49-year-old female was reported by Estil JC et al. [14], who had a slow-growing mass of 4 years duration, located on the plantar aspect of her left foot. The mass was slowly becoming more palpable as it increased in size and was progressively causing pain and discomfort during ambulation. Imaging studies revealed an ossified mass bearing no connection to any other structure on the plantar aspect of her foot. An excision biopsy was performed, and the easily dissectible mass, although much larger than its usual presentation, proved to be an extra skeletal osteochondroma. In 2015, Bilgin Y et al. [22], reported the case of a 56-year-old woman with an extra skeletal osteochondroma of the heel. In another case of slow-growing, relatively painful mass on the dorsal side of his right foot, in the 3rd toe web, reported by Kho et al. [23] found that an extraskeletal osteochondroma should be considered when a discrete, ossified mass is localized in the soft tissues of the distal extremities. Although cellular a typia is described on histological examination, there is no known malignant transformation or metastatic lesion. Marginal excision is the recommended treatment of choice, with preservation of the adjacent bone and soft tissue structures. A local recurrence rate of up to 18% has been reported, and such recurrence is best treated with re-excision.In our present case of benign osteochondromatous lesion, the nodular mass was there beneath the 3rd MTP Joint. The clinic pathological and radiological features of our case excluded the likelihood of myositis, lipomatous lesion, tumoral calcinosis, ossifying fibro myxoid tumor, or malignancy which may present as discrete soft tissue masses. Although mature ossifications generally associated with a benign lesion, sarcomatous lesions such as synovial sarcomas, soft tissue chondrosarcoma and Osteosarcoma can also present with dense calcification and ossification [8]. Thus, close histopathology and clinical correlations are essential to differentiate a chondrosarcoma from an extra skeletal osteochondroma.In conclusion, an osteochondromatous lesion should be considered when a distinct, ossified mass is localized in the soft tissues of the distal extremities. It has been reported that they have low risk of malignant degeneration. Marginal excision is the recommended treatment, with preservation of the adjacent bone and soft tissue structures.
Figures
Figure 1: X-ray antero-posterior and oblique view of left foot showing abnormal ossification around 3rd MTP Joint.
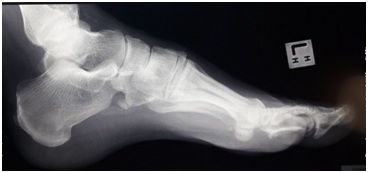
Figure 2: Lateral view of left foot showing ill-defined mineralization centered at the base of the proximal phalanx of 3rd toe.
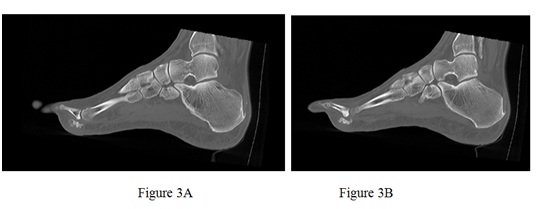
Figure 3: Lateral view of left foot showing ill-defined mineralization centered at the base of the proximal phalanx of 3rd toe.
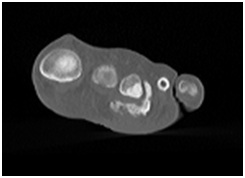
Figure 4: Coronal view of foot at metatarsophalangeal joint level showing hyper dense lesion beneath the 3rd MTP Joint.