Design and Fabrication of a Pressure Sensing Device to Aid with Fitting Lower Limb Prostheses
*Corresponding Author(s):
Ed HanadaDepartment Of Medicine, Nova Scotia Health Authority, Dalhousie University, Halifax, Nova Scotia, Canada
Tel:+1 9024733232,
Fax:+1 9024733204
Email:edwin.hanada@nshealth.ca
Abstract
Keywords
INTRODUCTION
Previous methods of measuring skin-socket interface pressures include use of electrical strain-gauge transducers, which were accurate and sensitive but required that the socket be significantly modified to accommodate the bulk of the transducers [4]. More recent use of fiber bragg grating sensors demonstrated that it was accurate in measuring pressures at the patellar tendon bearing area in a model transtibial amputee, but there was significant work to fabricate the sensors [4]. Furthermore, the sensors needed protection and were not tested in the dynamic setting with a suitable data acquisition system [4,5].
For this reason, a quantitative method for measuring pressure at the socket interface was developed to help determine areas of excessive pressure in the skin-socket interface to prevent potential complications during prosthesis fitting.
OBJECTIVES
The objective of this project was to build an economical proof of concept system that was:
- Easy to use
- Robust and portable
- Insensitive to heat within the socket
- Thin enough to fit unnoticeably between the limb and the socket, without requiring significant alterations to the socket.
METHODS
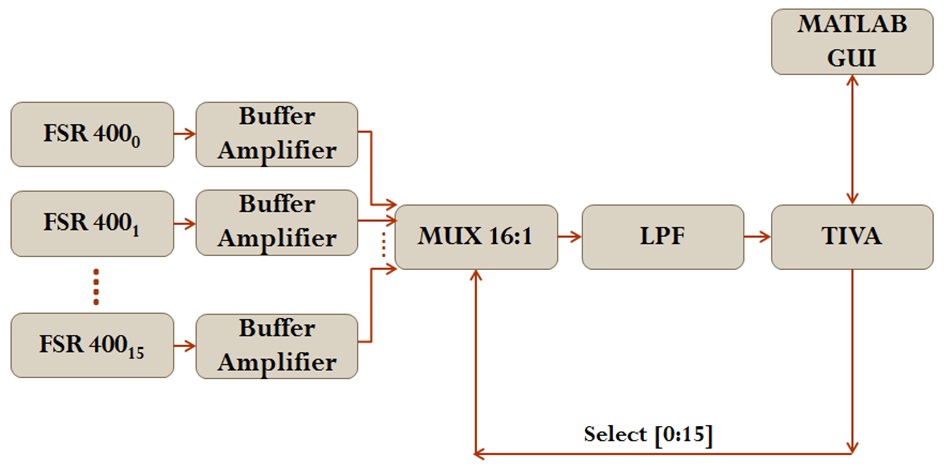
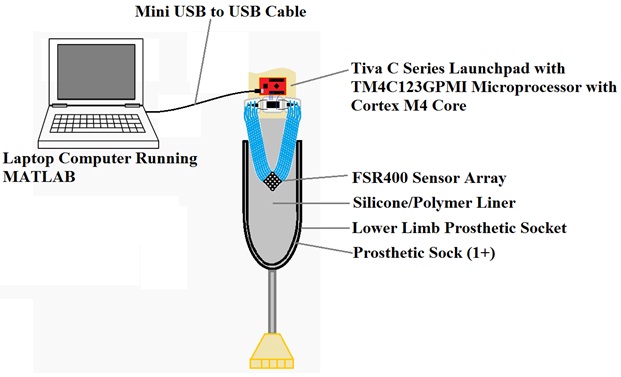
An array of 16 thin and flexible Force Sensitive Resistors (FSR) coupled with a buffer amplifier and multiplexing circuitry (MUX 16:1) allowed for pressure readings to be taken in the form of a voltage differential.The signal then passed through a Low-pass Filter (LPF) to produce a smoother output. The readings were sampled by a programmed microcontroller that translated the average of a sequence of voltages into the corresponding pressure value in kilopascals (kPa).The data was passed from the microcontroller to a PC via USB, where it was displayed on the User Interface (GUI).The final system architecture is displayed in figure 1. Sensor device is designed to be worn by a patient while in use. Straps can be fastened around the leg above the socket, or around the socket itself. Wires to the sensor array are formed into ribbons to reduce their profile inside the socket, ensuring a better fit. The set up of the pressure sensing system is displayed in figure 2.
RESULTS
Many trials of pressure values from able bodied persons were detected by the sensing layer and successfully sent from the controller and mapped with little delay. Near real time plotting was demonstrated with a 250ms refresh rate for pressures up to 350kPa with a sensitivity of 1kPa. To test the accuracy of the sensors, an object of known mass (275g) was isolated on sensor 15 to compare the expected pressure reading to observed readings.
The expected pressure was calculated as follows: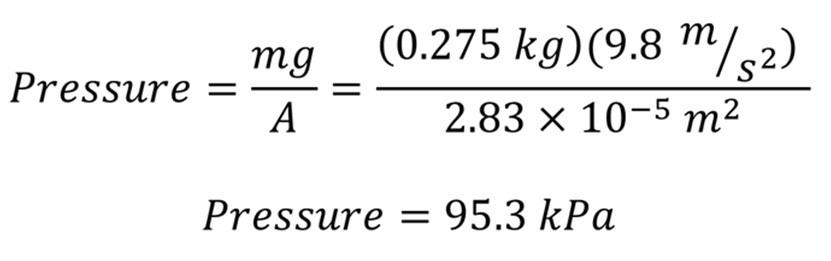
As an example, one sensor showed a reading of 89kPa to 96kPa(maximum error = 6.3%) after at least ten trials.
High pressure areas were color coded and mapped to location as in figure 3.

The sensor array fit inside the prosthetic socket without impeding the fit when it is worn by a subject. Pressure readings were sampled then transmitted at a rate that could accurately reflect changes in pressure as the patient moved. Pressure was displayed in an intuitive manner that could be interpreted easily by a prosthetist or clinician [4]. However, the sensor array requires further development and needs to be expanded to cover the entire residual limb at the socket-skin interface. Its efficacy and safety also have to be assessed to a greater extent and tested.
CONCLUSION
REFERENCES
- Bryon B (2005) Problems in Lower Limb Socket Fit and Present Clinical Solutions. American Academy of Orthotists and Prosthetists, Washington, USA.
- Levy SW (2004) Skin Problems of the Amputee. In: Smith DG, Michael JW, Bowker JH (eds.). Atlas of Amputations and Limb Deficiencies, (3rdedn).Digital Resource Foundation for the Orthotics and Prosthetics Community, Gainesville, Florida, USA.
- Canadian Association of Wound Care (2013) Statistics. Canadian Association of Wound Care, Canada.
- Al-Fakih EA, Abu Osman NA, Eshraghi E, Adikan FRM (2013)The Capability of Fiber Bragg Grating Sensors to Measure Amputees’ Trans-Tibial Stump/Socket Interface Pressures. Sensors 13:10348-10357.
- Polliack AA, Landsberger S, Mcneal DR, Craig D, Sieh R, et al. (1998) Scientific Characterization of the Rincoe Socket and Tekscan F-Socket Interface Pressure Measurement Systems: Implications for Clinical Utility. Rancho Los Amigos Medical Centre, Rehabilitation Engineering Program, California, USA.
Citation: EdHanada, Benstead T, Keeble R, Brown J (2015) Design and Fabrication of a Pressure Sensing Device to Aid with Fitting Lower Limb Prostheses. J Phys Med Rehabil Disabil 1: 006.
Copyright: © 2015 Ed Hanada, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.