
Pseudo-Foster Kennedy Syndrome: A Rare Presentation of Diabetes Mellitus
*Corresponding Author(s):
Pirasath SProfessorial Medical Unit, Teaching Hospital Jaffna, Jaffna, Sri Lanka
Tel:+94775122995,
Email:selladuraipirasath81@gmail.com
Abstract
Pseudo-Foster Kennedy Syndrome is defined as unilateral optic atrophy with optic disc swelling in the contralateral eye in the absence of an intracranial mass. We reported an uncommon manifestation of nonarteritic ischemic optic neuropathy presenting as Pseudo-Foster Kennedy Syndrome in a fifty years old male.
Keywords
INTRODUCTION
Pseudo-Foster Kennedy syndrome is defined as ipsilateral optic atrophy with disc edema in the contralateral eye with absence of intracranial mass [1]. It has been usually reported in cases of Benign Intracranial hypertension [2]. Ischemic optic neuropathies and Optic nerve hypoplasia in literature. Here, we describe a case of Pseudo-Foster Kennedy Syndrome in a patient presenting with visual impairment of both eyes and high blood glucose level on first medical consultation.
CASE PRESENTATION
A 50 year-old, previously healthy male presented with a history of sudden deterioration of painless vision for two weeks duration. It was associated with photopsia. He had no history of chronic early morning headache with nausea or vomiting and anosmia. He was nonsmoker and nonalcoholic. On clinical examination, Best-Corrected Visual Acuity (BCVA) was 6/60 and 6/24 in right and left eye respectively. Fundus examination revealed hyperemic disc edema in left eye (Figure 1A) and optic atrophy in right eye (Figure 1B). His blood pressure was 110/70 mmHg. Further systemic examintion was unremarkable. His basic biochemical and haematological investigations including ESR, C-reactive Protein (CRP) and platelet levels were normal. He was found to have high fasting blood sugar (248mg/dL) on admission with a HbA1C level of 9.1%. MRI study of brain showed no abnormalites. He was treated with metformin 500mg three times daily and Gliclazide 40mg twice daily with a target HbA1C of 7%. He was educated about his condition and was followed up closely once a month in clinic for glycemic control and vision. On assessment at six months he showed improvement in best corrected vision on left eye by two lines (6/60 in right eye, 6/12 in left eye). Fundus examination optic disc of left eye showed resolving disc odema with early optic atrophy (Figure 2 A&B). His HbA1C has declined to level of 6.1%. These findings were described as Pseudo-Foster Kennedy Syndrome.
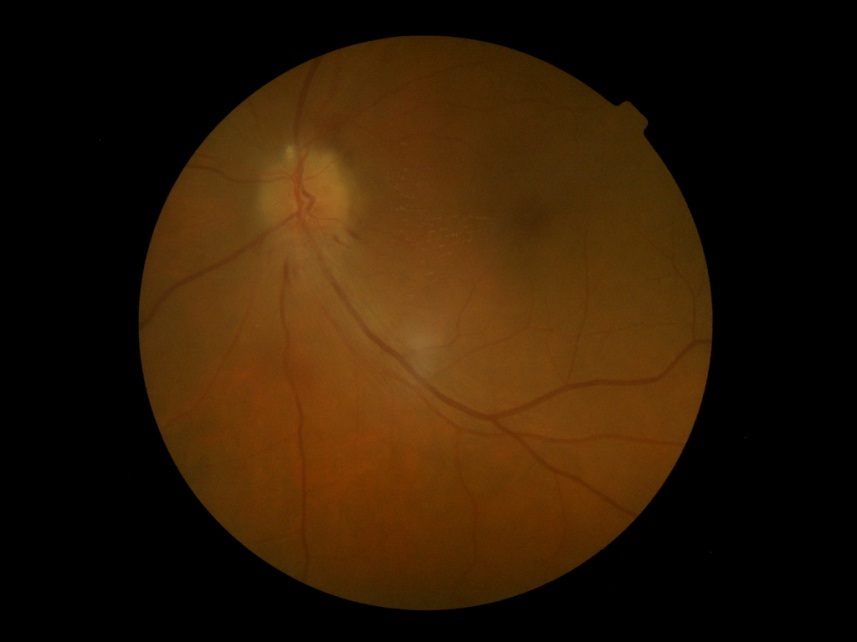 Figure 1A: Fundal photograph showing severe papilloedema in the left eye.
Figure 1A: Fundal photograph showing severe papilloedema in the left eye.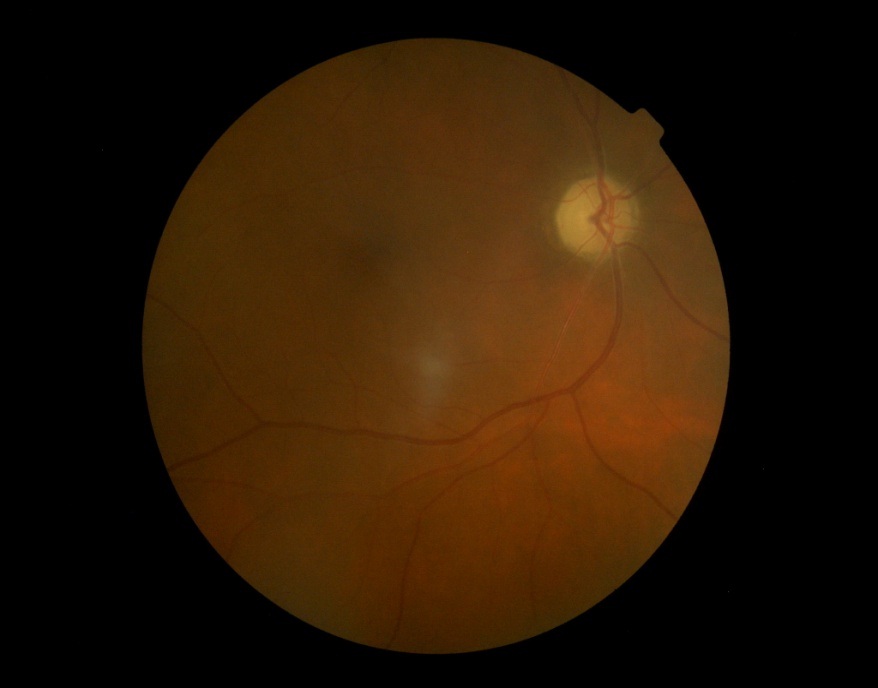 Figure 1B: Fundal photograph showing severe optic atrophy in right eye.
Figure 1B: Fundal photograph showing severe optic atrophy in right eye.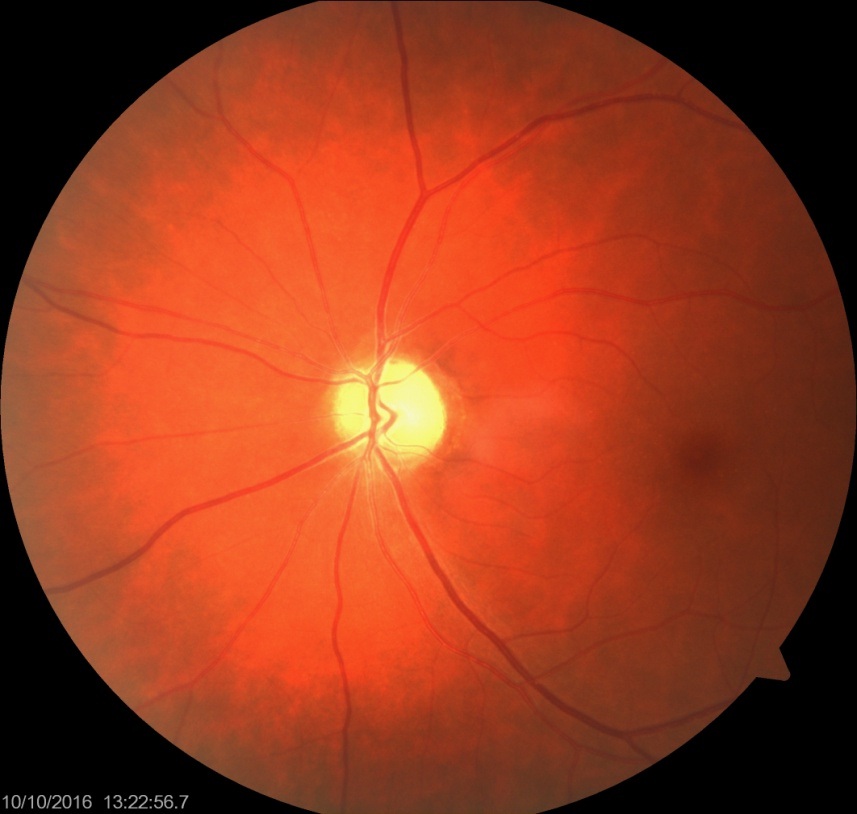 Figure 2A: Fundal photograph showing pale optic disc in the left eye.
Figure 2A: Fundal photograph showing pale optic disc in the left eye.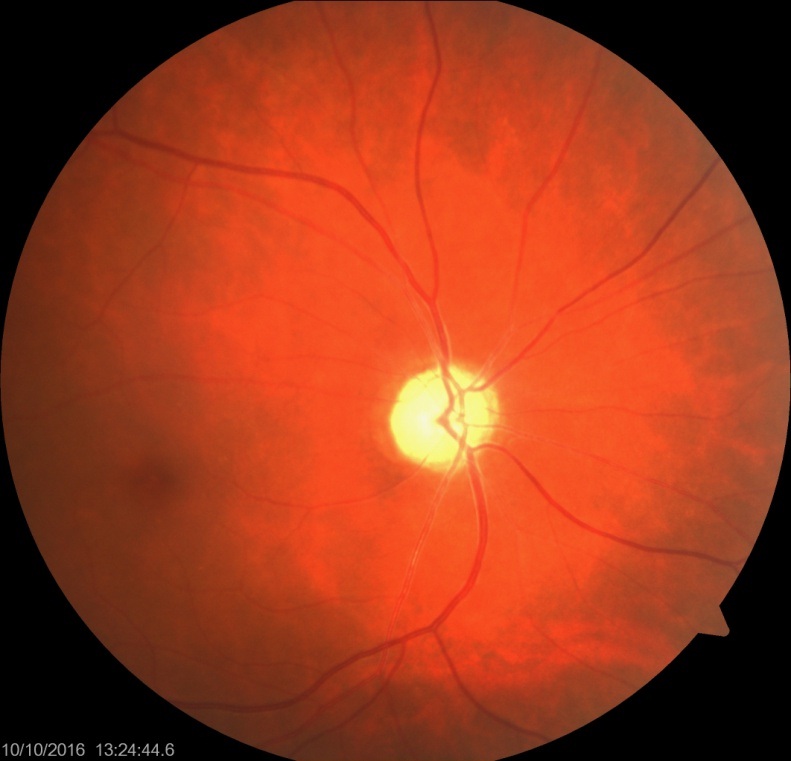 Figure 2B: Fundal photograph showing pale optic disc in the right eye.
Figure 2B: Fundal photograph showing pale optic disc in the right eye.
DISCUSSION
Anterior Ischemic Optic Neuropathy (AION) is categorized into Arteritic (AAION) and Non-arteritic (NAION) types. NAION typically occurs among middle age males with systemic vascular risk factors such as smoking and diabetes, causing hyperemic edema with disc hemorrhage, segmental pallor and attenuated blood vessels [3]. ESR, C-reactive Protein (CRP) and platelet levels are normal. AAION cause the swollen nerve-the one affected more recently-often displays pallid edema. It affects older people more common among female and has worse visual outcomes than NAAION patients with rare late improvement. They usually have elevated ESR, CRP and platelet levels. A 2- to 3-cm temporal artery biopsy with pathologic examination of consecutive slices spaced at 0.25 cm is the gold standard for diagnosis.
The first case of Foster Kennedy Syndrome was described by British neurologist Robert Foster Kennedy in 1911 [4]. Pseudo-Foster Kennedy syndrome has been reported in Nonarteritic ischemic optic neuropathy, optic neuritis and optic disc hypoplasia in literature [2]. Pseudo-Foster Kennedy is usually a diagnosis of exclusion. There was no other cause for the disc edema except the high blood sugar leading to non-arteritic anterior ischemic optic neuropathy in our patient. The disc edema in left eye and pallor optic disc in right eye have been set in due to untreated diabetic non-arteritic anterior ischemic optic neuropathy and poor glycemic control. Few cases of diabetic papillopathy mimicking non-arteritic anterior ischemic optic neuropathy were reported presenting as Pseudo-Foster Kennedy syndrome in literature [5].
Follow-up is essential during period of four to eight weeks to be sure that the swelling is resolving and is being replaced by pallor [6]. There have been case reports of patients who were initially diagnosed with bilateral sequential NAION and later proved to have a compressive lesion with development of neurologic symptoms [7]. On strict glycemic control, the disc edema was resolved in our patient during follow up at six months.
CONCLUSION
We concluded that the Pseudo-Foster Kennedy syndrome in our patient was due to diabetic non-arteritic anterior ischemic optic neuropathy.
REFERENCES
- Bansal S, Dabbs T, Long V (2008) Pseudo-Foster Kennedy Syndrome due to unilateral optic nerve hypoplasia: a case report. J Med Case Rep 2: 86.
- Micieli JA, Al-Obthani M, Sundaram AN (2014) Pseudo-Foster Kennedy syndrome due to idiopathic intracranial hypertension. Can J Ophthalmol 49: 99-102.
- Beck RW (1995) The optic neuritis treatment trial: three-year follow-up results. Arch Ophthalmol 113: 136-137.
- Kennedy F (1911) Retrobulbar neuritis as an exact diagnostic sign of certain tumors and abscesses in the frontal lobe. Am J Med Sci 142: 355-368.
- Mallika PS, Aziz S, Asok T, Chong MS, Tan AK (2012) Severe diabetic papillopathy mimicking non-arteritic anterior ischemic optic neuropathy (NAION) in a young patient. Med J Malaysia 67: 228-230.
- https://books.google.co.in/books?id=nd4_lnTzKdYC&printsec=frontcover&dq=How+do+you+evaluate+nonarteritic+anterior+ischemic+optic+neuropathy%3F&hl=en&sa=X&redir_esc=y#v=onepage&q=How%20do%20you%20evaluate%20nonarteritic%20anterior%20ischemic%20optic%20neuropathy%3F&f=false
- Gelwan MJ Mitchell S, Mark JK (1988) Pseudo-Pseudo-Foster Kennedy Syndrome. J Clin Neuro-Ophthalmology 8: 49-52.
Citation: Pirasath S, Suganthan N, Malaravan M (2017) Pseudo-Foster Kennedy Syndrome: A Rare Presentation of Diabetes Mellitus. J Clin Stud Med Case Rep 4: 037.
Copyright: © 2017 Pirasath S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

