Bilateral Acute Anterior Uveitis from Sinusitis Complicated by Optic Disc Oedema in a Child: A Case Report and Review of the Literature
*Corresponding Author(s):
Alessandro BagnisDepartment Of Neuroscience Rehabilitation Ophthalmology Genetics Maternal And Child Health, Clinica Oculistica, University Of Genoa, Azienda Policlinico Ospedaliero San Martino, Genoa, Italy
Tel:+39 0103538469,
Email:alebagnis@libero.it
Abstract
Background
To describe an unusual case in which bilateral sinusitis was followed by bilateral anterior uveitis complicated by bilateral papillitis that completely resolved after appropriate treatment of the sinusitis.
Case presentation
A 11-year-old caucasian child presented with bilateral anterior uveitis and a diagnosis of poststreptococcal uveitis was made after a complete clinical examination. After 1 week course of topical and parabulbar steroid and systemic benzylpenicillin a bilateral optic disc edema was also detected. The treatment was then continued, leading to complete remission. After 2 months from diagnosis the situation recurred bilaterally. An encephalic Magnetic Resonance Imaging (MRI) showed bilateral maxillary sinusitis and both topical steroids and systemic clarithromycin were then administered, leading again to bilateral remission. One month after the treatment had been stopped a monolateral recurrence occurred in his right eye and MRI showed persistent inflammation in the omolateral right maxillary sinus. Clarithromycin was then switched to systemic ciprofloxacin. A complete resolution of both uveitis and disc edema along with the improvement of the sinusitis occurred. Omolateral turbinate hypertrophy with nasal valve impairment was subsequently diagnosed and no recurrences occurred only after a surgical repair of the condition.
Conclusion
Based on our report, sinusitis should always be considered in children with anterior uveitis and/or papilledema. A prompt and adequate antibiotic treatment is essential in order to avoid potentially severe complications.
Keywords
ABBREVIATIONS
BACKGROUND
CASE PRESENTATION
A 4mg dose of parabulbar Betamethasone was immediately injected (RE) and Tobramycin + dexamethasone eye drops were started 5 times daily OU.
A thorough pediatric examination revealed no systemic abnormalities.
Several clinical investigations were performed: C-reactive protein, angiotensin-converting enzyme, plasma viscosity, antinuclear antibody, antineutrophil cytoplasmic antibody and chest X-ray, all of which proved normal. HLA-B27 was negative. Calcium, potassium, magnesium, phosphorus and creatinine were normal. Although a throat swab was negative, the patient had recurrent sore throats and blood testing revealed an elevated ASO titer (1150 IU/mL). Rheumatoid factor was negative and CRP was at the upper limit of the standard range. Post-streptococcal uveitis was diagnosed and following a rheumatological evaluation a treatment with benzatinic Benzylpenicillin 1,200,000 IU. once a week was started.
After 7 days the clinical picture was further complicated by the appearance of bilateral Optic Disc Edema (ODE), which was monitored by Optical Coherence Tomography (OCT) imaging. The visual field testing was normal OU.
The treatment was continued and the patient showed a significant improvement during the following days; three weeks after the acute event the situation completely resolved and steroid treatment was then tapered.
After 2 months from diagnosis the child had a recurrence of bilateral uveitis and ODE, despite the continuation of penicillin therapy. An encephalic Magnetic Resonance Imaging (MRI) was then performed. The exam (Figure 1a) showed normal globes and optic nerves bilaterally with no signs of orbital inflammation but revealed a maxillary sinusitis which was more severe on the right side, despite the absence of subjective symptoms like cheek pain or rhinorrhea. A topical corticosteroid (dexamethasone 0,1% four times daily) was restarted along with clarithromycin 250 mg BID for 7 days. Again, the uveitis promptly improved and the topical steroid treatment was gradually tapered in 4 weeks. One month after the treatment had been stopped, a monolateral relapse occurred in his RE, while LE showed no signs of active inflammation. The ODE was still detectable, although the OCT revealed a reduction in OU.
A further MRI of the maxillary sinuses was performed (Figure 1b), which revealed a persistent inflammation in the posterior portion of the right maxillary sinus. The presence of a residual inflammation in the right sinus was related to a microbial resistance to clarithromycin. It was then decided to change the antibiotic and ciprofloxacin 250 mg BID for 7 days was started along with the topical steroid.
After about 1 month, no signs of active inflammation were detectable and the OCT showed a further reduction of the ODE in OU and a bilateral resolution of the sinusitis was confirmed by a further MRI (Figure 1c). The ODE, which had improved during the administration of ciprofloxacin, completely disappeared after 3 weeks. The patient was completely asymptomatic during the following 6 years when he returned to our attention complaining again about redness ad photophobia in his RE. The clinical examination revealed flare and cells within the anterior chamber (1+) but no posterior chamber involvement. An MRI was immediately performed, revealing omolateral turbinate hypertrophy associated with nasal valve impairment and initial signs of sinusitis. The decision was taken to correct surgically the nasal condition. The patient did not had any relapse since then and at the last follow-up visit 1year after surgery he showed no signs of active nor previous ocular inflammation.
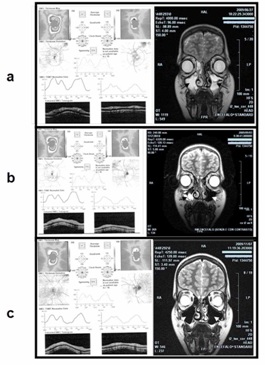
Figure 1: (a) MRI image (right column) showing bilateral sinusitis of the maxillary sinuses (black arrows). OCT (left column) revealed ONH edema immediately after the first episode of acute bilateral anterior uveitis. (b): After the first course of antibiotics, MRI showed that the maxillary sinusitis had resolved in the left sinus (white arrow) but persisted in the right sinus. The OCT revealed an ONH edema improvement bilaterally. (c): OCT revealed a further improvement after treatment with ciprofloxacin, although a minimum edema persisted during the following 3 weeks before the complete resolution occurred. MRI showed complete remission of the sinusitis (white arrows) in both sinuses.
DISCUSSION
Nevertheless, the use of benzyl penicillin did not prevent relapse and MRI led us to suppose that the origin of the ocular inflammation was the bilateral asymptomatic maxillary sinusitis. The literature on uveitis as a complication of sinusitis is very scant and little is known about the mechanisms that lead anterior uveitis to cause ODE, which has been reported to occur in 7-29% of chronic uveitis but it is not reported as a complication of anterior chronic uveitis [4,11,12] In our case, both cells and flare were very evident, but were not proportional to the severity of the disease. Indeed, the correlation between flare and ODE is uncertain, even though flare is normally associated with a variety of disease manifestations, including uveitic complications [11,13]. Bilateral optic disc swelling is an important clinical sign that can reflect a variety of inflammatory, infectious, toxic, metabolic, genetic or vascular conditions, such as hypertension or ischemia [14]. The related venous obstruction can result in unilateral or bilateral involvement, with minimal optic neuropathy and no apparent visual loss resulting from ischemic or edematous retina [15]. Concerning our case we suppose the following mechanism: the sinusitis induced severe inflammation causing a massive release of proinflammatory cytokines that reached the orbit and involved the pre-laminar portion of the optic nerve. Common complications of ocular inflammation, such as retinal edema, may be due to the effects of cytokines [16], which could have produced flare in the AC and a partial axoplasmic block secondary to intra-axonal edema in the optic nerve. Recent studies on the role of cytokines in uveitis support our hypothesis [17]. Conversely, a rise in cerebrospinal fluid pressure in the cranial subarachnoid space and its transmission to the sheath of the optic nerve was not essential in our case. Indeed, when the inflammation of the sinus improved, both eyes completely healed and no more relapses occurred after the condition predisposing to sinusitis was finally resolved.
It should be emphasized that ODE due to anterior uveitis appears to have a more favorable prognosis than post-sinusitis papillitis which may lead to severe visual complications [6,18,19] and this can explain the good visual outcome of our patient.
Finally, our report highlights the importance of antibiotic treatment in order to shorten the duration of infection and illness, to reduce mucosal damage and to prevent contiguous infectious involvement of the orbit. In our patients we used clarithromycin and ciprofloxacin. The former was used because it probably exerts its beneficial effect not only by inhibiting or killing bacterial pathogens, but also by down-regulating pro-inflammatory mechanisms. The latter antibiotic was used in order to destroy any remaining clarithromycin-resistant bacteria. Quinolone-induced arthropathic toxicity has largely restricted the use of ciprofloxacin in children and adolescents. It is now known, however, that this drug does not engender an important risk of arthropathy or tendinopathy in humans [20]; indeed, the treatment has been effective and devoid of side effects in our case.
CONCLUSION
AUTHORS’ CONTRIBUTIONS
REFERENCES
- Cunningham ET, Suhler EB (2008) Childhood uveitis-young patients, old problems, new perspectives. J AAPOS 12: 537-538.
- Cunningham ET (2000) Uveitis in children. Ocul Immunol Inflamm 8: 251-261.
- Rothova A, Suttorp-van Schulten MS, Frits Tretters W, Kijlstra A (1996) Causes and frequency of blindness in patients with intraocular inflammatory disease. Br J Ophthalmol 80: 332-336.
- Rosenberg KD, Feuer WJ, Davis JL (2004) Ocular complications of pediatric uveitis. Ophthalmology 111: 2299-2306.
- Levy-Clarke GA, Nussenblatt RB, Smith JA (2005) Management of chronic pediatric uveitis. Curr Opin Ophthalmol 16: 281-288.
- Monheit BE, Read RW (2005) Optic disk edema associated with sudden-onset anterior uveitis. Am J Ophthalmol 140: 733-735.
- Kumar RK, Ghali M, Dragojevic F, Young F (1999) Papilloedema secondary to acute purulent sinusitis. J Paediatr Child Health 35: 396-398.
- Newton DA (1996) Sinusitis in children and adolescents. Primary Care: Clinics in Office Practice 23: 701-717.
- Paroli MP, Spinucci G, Liverani M, Monte R, Pezzi PP (2009) Uveitis in childhood: an Italian clinical and epidemiological study. Ocul Immunol Inflamm 17: 238-242.
- Ur Rehman S, Anand S, Reddy A, Backhouse OC, Mohamed M, et al. (2006) Poststreptococcal syndrome uveitis: a descriptive case series and literature review. Ophthalmology 113: 701-706.
- Menezo V, Lightman S (2005) The development of complications in patients with chronic anterior uveitis. Am J Ophthalmol 139: 988-992.
- De Boer J, Wulffraat N, Rothova A (2003) Visual loss in uveitis of childhood. Br J Ophthalmol 87: 879-884.
- Holland GN (2007) A reconsideration of anterior chamber flare and its clinical relevance for children with chronic anterior uveitis (an American Ophthalmological Society thesis). Trans Am Ophthalmol Soc 105: 344-364.
- Lee AG, Beaver HA (2002) Acute bilateral optic disk edema with a macular star figure in a 12-year-old girl. Surv Ophthalmol 47: 42-49.
- Vaphiades MS (2002) The discdisc edema dilemma. Surv Ophthalmol 47: 183-188.
- Wakefield D, Lloyd A (1992) The role of cytokines in the pathogenesis of inflammatory eye disease. Cytokine 4: 1-5.
- Sijssens KM, Rijkers GT, Rothova A, Stilma JS, de Boer JH (2008) Distinct cytokine patterns in the aqueous humor of children, adolescents and adults with uveitis. Ocul Immunol Inflamm 16: 211-216.
- Kozak I, Robbins SL, Freeman WR (2007) Bilateral papillitis associated with bilateral anterior uveitis in a child. J Pediatr Ophthalmol Strabismus 44: 374-376.
- Jüngert JM, Uberall M, Mayer UM, Guggenbichler JP, Heininger U (2001) Papilledema and acute bilateral amaurosis accompanying acute sinusitis. Klin Padiatr 213: 343-346.
- Sendzik J, Lode H, Stahlmann R (2009) Quinolone-induced arthropathy: an update focusing on new mechanistic and clinical data. Int J Antimicrob Agents 33: 194-200.
Citation: Saccà SC, Bagnis A, Traverso CE (2017) Bilateral Acute Anterior Uveitis from Sinusitis Complicated by Optic Disc Oedema in a Child: A Case Report and Review of the Literature. J Otolaryng Head Neck Surg 3: 015.
Copyright: © 2017 Sergio Claudio Saccà, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.