
A Nodule of Recent onset with Blue and Black Color on Dermoscopy: Pigmented Epithelioid Melanocytoma
*Corresponding Author(s):
Florentina Silvia DelliState Hospital For Skin And Venereal Diseases, Hippokration Hospital, 124 Delfon Street, 546 43, Thessaloniki, Greece
Email:delliflorentina@ymail.com
Abstract
The combination of blue and black color is frequent in nodular melanoma and extremely rare in benign tumors. The Dermoscopy symmetry and homogeneity are findings compatible with the diagnosis of PEM. We present of case of PEM and discuss the importance of clinical diagnosis and histological confirmation.
Keywords
Epithelioid; Melanocytoma; Pigmented
introduction
Pigmented Epithelioid Melanocytoma (PEM) is a rare melanocytic neoplasm mostly seen in children and young adults, but can practically affect all age groups. Genital and other mucosae involvement has been also described. Its occurrence is unrelatedto sun exposure, and displays no ethnic susceptibility. PEMoccurs as a sporadic lesion, or in patients with familial cancer syndrome and frequently involves regional lymph nodes. It was previously described with the terms “animal-type melanoma” and epitheliod blue nevus of Carney complex [1]. Deaths due to PEMs are very rare and can be associated with additional mutations in metastatic cases, such as in BRAF V600E, TP53 or PIK3CA [2,3].
Case Presentation
Α 43-year-old female patient presented for evaluation of a recently observed black nodular lesion on the upper back (Figure 1A). Dermatoscopy revealed homogenous predominant blue but also black pigmentation as irregularly shaped areas (Figure 1B). The lesion was excised. Histopathologic examination revealed pigmented parakeratosis and a dense infiltrate of melanocytes with heavy pigmentation in the papillary and reticular dermis (Figure 1C). The tumor cells were epithelioid or spindle shaped and arranged in fascicles or nodules . The intratumoral and peritumoral lymphocyte infiltration were absent, without any evident signs of vascular invasion and neurotropism. The melanocytes were uniform, displayed minimal atypia, and had low mitotic activity. Necrosis was absent. Immunohistochemical analysis showed strong positivity for Melan A (Figure 1D) and HMB-45 (Figure 1E). Based on the above features the diagnosis of PEM was established. Computed Tomographic (CT) scans were unremarkable. Based on clinical, histological and CT results, sentinel lymph node biopsy was considered not necessary.
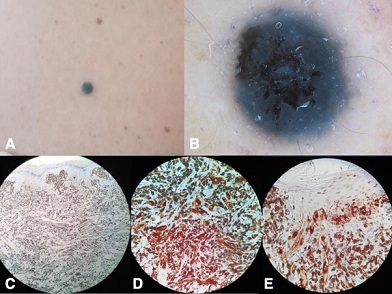 Figure 1: A) Black nodular lesion on her upper back; B) Dermoscopy revealed homogenous blue pigmentation, but also black, irregularly shaped areas in the center and eccentrically. C) Histopathologic examination revealed a dense infiltrate of melanocytes with copious amounts of melanin in the papillary and reticular dermis. Epithelioid or spindle shaped tumor cells, arranged in fascicles or nodules. Uniform melanocytes with minimal atypia, and low mitotic activity; D) Positivity of pigmented cells for Melan A; E) Positivity of pigmented cells forHMB-45.
Figure 1: A) Black nodular lesion on her upper back; B) Dermoscopy revealed homogenous blue pigmentation, but also black, irregularly shaped areas in the center and eccentrically. C) Histopathologic examination revealed a dense infiltrate of melanocytes with copious amounts of melanin in the papillary and reticular dermis. Epithelioid or spindle shaped tumor cells, arranged in fascicles or nodules. Uniform melanocytes with minimal atypia, and low mitotic activity; D) Positivity of pigmented cells for Melan A; E) Positivity of pigmented cells forHMB-45.
Discussion
PEM is a rare low-grade melanocytic tumor first described in gray horses, which led to the term “animal-type melanoma” also in humans [4]. From the clinical point of view, a blue coloured tumor suggests two main differential diagnoses: blue nevus and melanoma.
In a similar way, the same dilemma is also confronted in dermatopathology. In 2004, Mones and Ackerman publish a detailed article where they analyzed certain histological characteristics that facilitate the correct diagnosis of melanocytoma, atypical blue nevus, melanoma with features of blue nevus and regressed melanoma with nodular melanosis [5]. Neither wide local excision, nor sentinel lymph node biopsy are considered standard of care.
A clinical picture of a homogenous blue nodular lesion in young patients revealing dermoscopic blue-nevus-like appearance with the presence of variable combination of homogenous black, brown or white pigmentation areas, might be highly suggestive of PEM. Usually, the patients refer the growing tendency of the lesion. Although the differential diagnosis of PEM versus common blue nevus and melanoma is made only based on histological examination, clinical suspicion of PEM is essential for the patient, especially when it concerns children and young adults. Dermatoscopy is an additional tool for the dermatologist, but also for the pathologist, guiding the correct diagnosis. Moscarella et al. were the first to describe PEM’s dermoscopy features, including homogenous blue pigment, blue and black pigment, brown comedo-like openings, crystalline structures and blue pigment extending into lymphatic vessels [6]. The symmetry and the homogeneity are compatible with the diagnosis of PEM, while the asymmetric pigmentation, the disorganized pattern, the abnormal vascular structures and the presence of other colored structures (milky-red globules, red areas) are suggestive for pigmented nodular melanoma [7]. Furthermore, the presence of crystalline structures along with the combination of blue and black color are features that lead to excision.
In conclusion, PEM is a diagnostic challenge, displaying misleading features for both, clinicians and pathologists.
References
- Ramondetta A, Ribero S, Conti L, Quaglino P, Broganelli P (2020) A Case of a Pigmented Epithelioid Melanocytoma on a Mucosal Site. Dermatol Pract Concept 10: 2020070.
- Bayraktar EC, Jour G (2021) Pigmented Epithelioid Melanocytomas and Their Mimics; Focus on Their Novel Molecular Findings. Biology (Basel) 10: 1290.
- Benton S, Zhao J, Asadbeigi S, Kim D, Zhang B, et al. (2021) Pigmented Epithelioid Melanocytoma: Morphology and Molecular Drivers. Surg Pathol Clin 14: 285-292.
- Levene A (1979) Disseminated dermal melanocytosis terminating in melanoma. A human condition resembling equine melanotic disease. Br J Dermatol 101: 197-205.
- Mones JM, Ackerman AB (2004) "Atypical" blue nevus, "malignant" blue nevus, and "metastasizing" blue nevus: a critique in historical perspective of three concepts flawed fatall. Am J Dermatopathol 26: 407-430.
- Moscarella E, Ricci R, Argenziano G, Lallas A, Longo C, et al. (2016). Pigmented epithelioid melanocytoma: clinical, dermoscopic and histopathological features. Br J Dermatol 174: 1115-1117.
- Pizzichetta MA, Kittler H, Stanganelli I, Bono R, Cavicchini S, et al. (2015) Pigmented nodular melanoma: the predictive value of dermoscopic features using multivariate analysis. Br J Dermatol 173: 106-114.
Citation: Delli FS, Apalla Z, Grammatikopoulou J, Nikolaidou C, Lallas A (2022) A Nodule of Recent onset with Blue and Black Color on Dermoscopy: Pigmented Epithelioid Melanocytoma. J Clin Dermatol Ther 9: 0109.
Copyright: © 2023 Florentina Silvia Delli, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

