
Autoimmune Progesterone Dermatitis Imitating Eczematous Dermatitis
*Corresponding Author(s):
Tavlene BanwaithDepartment Of Endocrinology, Hereford County Hospital, Hereford, United Kingdom
Email:tavlenebanwaith@gmail.com
Abstract
Autoimmune progesterone dermatitis is a rare, cyclic premenstrual reaction to progesterone. It affects young women of childbearing age with an increased prevalence during the third decade of life. Autoimmune progesterone dermatitis should be considered in women with recurrent cyclic skin eruptions who exhibit flares at the height of progesterone levels, 3-10 days before menses. Presentation can overlap with other forms of dermatosis such as urticaria, eczema, erythemamultiforme and lupus erythematosus. The diagnosis is confirmed via an intradermal test, with an immediate or late reaction observed following the introduction of exogenous progesterone. Despite variable clinical manifestations, the management of autoimmune progesterone dermatitis remains the same; it relies on hormone suppression. Identifying the correct diagnosis before treatment is essential in preventing this autoimmune disease. This articledescribes a patient initially diagnosed and treated for eczematous dermatitis then correctly diagnosed with autoimmune progesterone dermatitisand, subsequently, treated with progesterone therapy.
Case Report
A 34-year-old woman developed a widespread, pruritic, eczematous eruption during pregnancy 8 years earlier. The ongoingrash affected all areas of her body; primarily focused on the face, neck, upper trunk, legs and arms with relative sparing of the flexural sites. Regular exacerbations occurred before menses, with improvement a few days into the cycle and 10 days of remission between menses. Further exacerbation occurred following the insertion of asubcutaneous progesterone implant, but no improvement was seen on removal. She noted that sun exposure improved therash. Her GP prescribed topical steroids including hydrocortisone, dermovate and betnovate, which had little positive effect.
Her past medical history consisted of mild asthma and hay fever. Her drug history included the topical steroid agents mentioned above, as well as over the counter antihistamines. She had no allergies.
Upon examination, there was a widespread eczematous rash over 50% of her body surface, principally affecting her scalp, neck, hands and wrists, spreading over her shoulders to the abdomen and involving her arms and legs, with interspersed areas throughout (Figures 1&2). There was relative sparing of the flexural sites, periorbital areas and eyelids. The rash was symmetrical with evidence of excoriation and lichenification, most noticeable at the hands and wrists (Figure 3). No lymphadenopathy was noted. Blood work was unremarkable. Differential diagnoses included atopic dermatitis, eczematous dermatitis, progesterone autoimmune dermatitis and mycosis fungoides. She was advised to continue topical steroids with plentiful use of emollients.
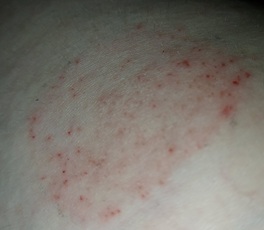 Figure 1: Interspersed eczematous dermatitis on the upper leg.
Figure 1: Interspersed eczematous dermatitis on the upper leg.
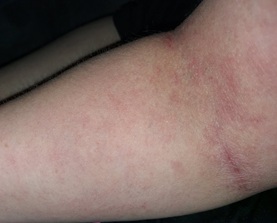 Figure 2:Widespread eczematous dermatitis over the flexor surface of the left arm.
Figure 2:Widespread eczematous dermatitis over the flexor surface of the left arm.
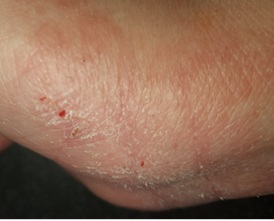 Figure 3: Eczematous dermatitis with evidence of excoriation on the palmar surface of the right hand.
Figure 3: Eczematous dermatitis with evidence of excoriation on the palmar surface of the right hand.
An incisional biopsy of the left side of the neck revealed ‘rather non-specific features, with a hint of eczema and a T-cell predominant lymphocyte population, in keeping with a diagnosis of superficial dermatitis’. After consideration of the direct correlation between rash onset, menses and pregnancy, a clinical diagnosis of autoimmune progesterone dermatitis was confirmed by a consultant dermatologist. The patient was commenced on cetirizine 10 mg twice daily, topical hydrocortisone for her face and neck, and topical betnovate and dermovate for the trunk and limbs. Regular emollients were advised and Protopic 0.1% ointment was prescribed for once to twice daily use on active areas, then twice weekly use to maintain remission. She was alsoreferred to an allergy specialist for intradermal testing.
Further specialist opinion was sought from an endocrinologist, who advised additional treatment through hormone replacement therapy (Evorel Conti Transdermal patch containing oestradiol3.2 mg and norethisterone11.2 mg). Within 3 weeks of receiving progesterone therapy the patient’s need for topical steroids reduced significantly. By 3 months, her rash resolved entirely without altering her menses. The occasional exacerbation was well controlled by topical steroids.
Discussion
Autoimmune progesterone dermatitis is a rare autoimmune response to endogenous progesterone, thought to be caused by a type 1 hypersensitivity reaction to the hormone [1]. Onset is variable,with the earliest age reported at menarche and the highest prevalence during the third decade of life [2].
Autoimmune progesterone dermatitis presents as a cyclical cutaneous eruption during the luteal phase of the menstrual cycle [3]. The nature of the eruption varies widely, with the most common clinical manifestations being urticaria, angioedema and erythema multiforme [4]. The difficulty in diagnosis is differentiation between other skin disorders with similar manifestations: lupus erythematosus, psoriasis and acne also exacerbate before menstruation and exhibit features reactive to sunlight. In contrast to other differential diagnoses, there are no histopathological findings or definitive diagnostic laboratory tests for autoimmune progesterone dermatitis. Instead, autoimmune progesterone dermatitis can be diagnosed by fulfilling the following clinical criteria: premenstrual flare in skin lesions, reproducibility of these lesions with an intradermal or intramuscular test, and symptomatic improvement from inhibiting progesterone [4].
Treatment for autoimmune progesterone dermatitisis directed by itsaetiology. Exogenous progesterone via hormone replacement therapy, as used in this case, suppresses ovulation and subsequently inhibits progesterone secretion [4]. Alternatively, treatment via bilateral salpingo-oophrectomyalso results in remission of symptoms by averting an immune response [1], although this would only be performed as a last resort, as it would induce menopause.
Understanding the aetiology of autoimmune progesterone dermatitis and its correlation with the menstrual cycle is fundamental in obtaining an accurate diagnosis and management plan and improving patient outcomes. For a timely diagnosis of autoimmune progesterone dermatitis, it is essential to raise awareness of this condition among healthcare professionals. The polymorphic characteristics of autoimmune progesterone dermatitis and its propensity to mimic other disorders, such as eczematous dermatitis, can make diagnosis challenging. Thus, it is imperative to consider this as a differential diagnosis of dermatitis in all women of childbearing age.
Learning Points
- The clinical mimicry between autoimmune progesterone dermatitis and other skin disorders, such as eczematous dermatitis, must be considered when formulating differential diagnoses for dermatosis, especially in women of childbearing age.
- Given the differing treatment regimens required for various skin conditions (topical steroids vs hormone replacement therapy in this case), healthcare workers must have the knowledge required to accurately diagnose autoimmune progesterone dermatitis and provide appropriate treatment.
References
- Whitt W, Stiegler J, Richardson C (2020) Autoimmune progesterone dermatitis mimicking facial erythromelalgia successfully treated with hysterectomy and bilateral salpingo-oophorectomy. Am Acad Dermatol 6: 1104-
- DetrixheA, NikkelsAF, DezfoulianB (2017) Autoimmune progesterone dermatitis. Arch Gynecol Obstet 296: 1013-
- OzdemirO, YhasiGG, Ataly CR (2019) Autoimmune progesterone dermatitis: a case report. Rev Bras Ginecol Obset 41: 203-
- You HR, Yun SJ, Kim SJ, Lee S-C, Won YH, et al. (2017) Three cases of autoimmune progesterone dermatitis. Ann Dermatol 29: 479-
Citation: Banwaith T, Acharya J (2022) Autoimmune Progesterone Dermatitis Imitating Eczematous Dermatitis. J Clin Dermatol Ther 8: 0100.
Copyright: © 2022 Tavlene Banwaith, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

