
Blast Overpressure Induced Pulmonary and Intestinal Damage is Ameliorated by Post-injury Decay Accelerating Factor Injection
*Corresponding Author(s):
Jurandir J Dalle LuccaTri Services Research Laboratory, Joint Base San Antonio, Joint Inflammation Modulation Of Trauma Program, Fort Sam Houston, Texas, United States
Tel:210-539-7399,
Email:Jurandir.J.DalleLucca.mil@mail.mil
Abstract
Blast Overpressure (BOP) inflicts severe immediate physical and continuous inflammatory injury upon air/gas filled-hollow organs, i.e., lungs and intestines. Sprague-Dawley rats were subjected to BOP (120 kilopascals) to study military relevant injuries. Recombinant human DAF (rhDAF) was administered (50μg/kg body weight) 30minutes post-blast to simulate expected emergency care chronology. The rhDAF treatment group was compared to 1) sham control group- no BOP exposure with no saline injection, and 2) BOP with saline injection group (30minutes post-blast). Within each group, animals underwent recovery (simulated or veritable) and were sacrificed at 3, 24 and 48hours post-blast. Lung and small intestine tissue samples were prepared for pathology injury assessments, microscopic evaluations and immunohistochemistry assessment of tissue marker deposition (rhDAF, complement C5, Neutrophil Elastase (NE), and caspase-1). BOP resulted in pulmonary and intestinal damage that was mitigated by post-blast administration of rhDAF. Complement activator C5/C5a, NE, and caspase-1 increased during 3 to 48h following BOP. rhDAF treatment significantly reduced levels of C5/C5a, and NE after their induction, but did not alter caspase-1 levels. These novel findings suggest early complement inhibition via rhDAF administration is a promising new therapeutic strategy to decrease BOP-induced pulmonary and intestinal tissue injury.
Keywords
INTRODUCTION
Pure blast injuries resulting from High-Energy (HE) explosions were first studied during WWI by Hooker. Those studies determined the nature of primary blast injury to be independent of secondary (flying “missiles” of shrapnel and debris), and tertiary (the propelling blast wind and subsequent impact). Outside of a zone of death, described as a short radius of proximity emanating out from the point of explosion, another zone exists that promotes a shock syndrome of blood pressure collapse which indicate some physical injury, however, without any external manifestation [1]. Lung and visceral organ hemorrhage was common in his blast model animals whereas intracranial lesions were absent. WWII studies reported that Blast Overpressure (BOP) waves injure the lungs via impact with the body wall [2]. Case studies at that time supported findings that lungs were the primary organ injured by a BOP yet further suggested ubiquitous damage throughout lung tissue through gross examination assessment of cases that went to necropsy [3]. More recent studies have described these injuries as being owed to the great heterogeneity of solids, liquids, and gasses all occupying a small space in which BOP effects each in unique fashion. However, the primary cause of injury has been shown to be the result of rapid compression and expansion of the gaseous component of anatomical structure [4]. Gastrointestinal tract tissues and organs are also highly susceptible to BOP due to retention and generation of gasses [5,6]. A thorough review of blast-related injury is available [7].
Only from HE explosives does a BOP wave propagate that may induce a primary blast injury. HE explosions occur on American soil in both deliberate and accidental manner, i.e., HE explosions occurred at the 1993 world trade center bombing, the 1998 Alfred P Murray building/Oklahoma city bombing, and constituted the disaster of the 2012 city of West, Texas fertilizer plant. HE explosions are ever increasing in incidence on the global scale with continued blasts in Israeli-Palestinian conflicts and the threat of terrorist attacks in the developed world is constant: London 2005 [8,9], Madrid 2004 [10], and Moscow 2010 [11]. Blast injuries, simulated by the immediately sub-lethal yet tissue-damaging model employed in this manuscript, are a real and present danger with which few civilian physicians have experience in treating [12].
BOP pulmonary and intestinal tissue injury shows general similarity to Ischemia/Reperfusion (I/R) injury in its subsequent increased inflammation and delayed injury response. Complement inhibition therapy have been demonstrated to decrease severity of I/R injuries to these tissues [13,14]. Decay Accelerating Factor (DAF) is a naturally present complement-inhibitory protein in humans that binds cells and prevents assembly of both C4b2a and C3bBb, the classical and alternative pathway C3 convertases. DAF thereby blocks these two complement amplification convertase enzymes and provide protection from the subsequent complement cascade activation which involves the formation of C5 convertase and the membrane attack complex (C5b-9) that creates pores in membrane causing the cell lysis [15]. Our research has shown pharmacologic supplementation of DAF to be neuroprotective to blast effects by suppressing the systemic and local inflammatory response, improving blood-brain barrier integrity, reducing tau phosphorylation and decreasing cytotoxic edema [16]. DAF administration following hemorrhage and/or I/R also has been shown to limit lung and intestine tissue damage, decrease complement activation and tissue deposition, decrease IL-6 production and improve survival chances [17-20]. We therefore hypothesized that DAF administration would ameliorate pulmonary and intestinal damage commonly produced by blast injury. In order to test this hypothesis, we administered rhDAF to rats that were subjected to BOP and assessed the lung and intestinal tissue injury benefits. We demonstrate in this study that DAF administration 30minutes post-blast exposure decreases complement activation and mitigates tissue damage. Early administration of DAF to a victim of blast exposure may ameliorate intestinal and pulmonary injury and improve recovery.
MATERIALS AND METHODS
Animals
Reagents
Experimental design and administration of DAF
Immunohistochemical staining
Immunofluorescent quantification
Statistical analysis
RESULTS
Recombinant human DAF deposits in pulmonary tissue
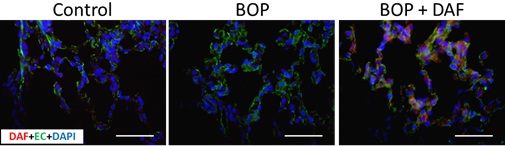
Figure 1: Deposition of rhDAF in the rat lung. Representative photomicrographs of the frozen sections from rat lungs immunostained by anti-human DAF (red), anti-Endothelial Cell (EC, green) antibodies, and DAPI (4′, 6-Diamidino-2-phenylindole dihydrochloride). Original magnification of x 200. Scale bar, 200 µm. n=8 for both control and experimental groups.
Administration of rhDAF mitigates pulmonary tissue injury in a murine model of BOP
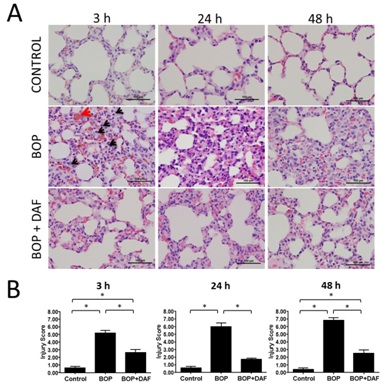
Figure 2: Early treatment of rhDAF attenuates lung tissue injury in a murine model of BOP. A) All were representative photomicrographs of lung paraffin sections with H&E of BOP-3h, BOP-24h and BOP-48h control, untreated and treated with rhDAF (50µg/kg) 30min post blast exposure. Original magnification of x 400. Scale bar, 100µm. B) Mean lung injury scores were graphed. n=8 for all control, BOP-3h and BOP-24h groups and n=5 for BOP-48h group. n=6, 8 and 5 for BOP+DAF-3h, BOP+DAF-24h and BOP+DAF-48h respectively. Injury scores calculated using the criteria as described in the Methods. Graphical data expressed as mean ± SEM, and compared using one-way ANOVA followed by Bonferroni test.
Administration of rhDAF mitigates intestinal tissue injury in a murine model of BOP
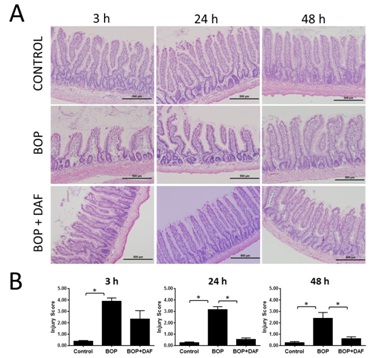
Figure 3: Early treatment of rhDAF attenuates intestinal tissue injury in a murine model of BOP. A) All were representative photomicrographs of intestine paraffin sections with H&E of BOP-3h, BOP-24h and BOP-48h untreated and treated with rhDAF (50µg/kg) 30min post blast exposure. Original magnification of x 400. Scale bar, 500µm. B) Mean intestine injury scores were graphed. n=8 for all control, BOP-3h and BOP-24h groups and n=5 for BOP-48h group. n=6, 8 and 5 for BOP+DAF-3h, BOP+DAF-24h and BOP+DAF-48h respectively. Injury scores calculated using the criteria as described in the Methods. Graphical data expressed as mean ± SEM, and compared using one-way ANOVA followed by Bonferroni test.
rhDAF attenuates complement expression and deposition in lung tissue promoted by BOP injury
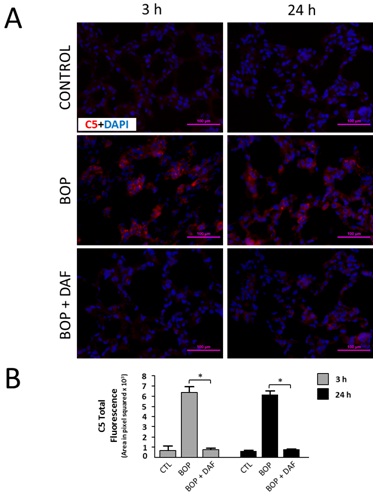
Figure 4: rhDAF decreases C5/C5a deposition in lung tissue from BOP exposed rats. A) Representative photomicrographs of the lung frozen sections were stained with anti-C5/C5a antibodies and DAPI. Original magnification of x 400. Scale bar, 100µm. B) Mean fluorescence intensities were graphed. n=8 for all control, BOP-3h and BOP-24h groups. n=6 and 8 for BOP+DAF-3h and BOP+DAF-24h respectively. Total immunofluorescences were calculated using the criteria as described in the Methods. Graphical data expressed as mean ± SEM, and compared using one-way ANOVA followed by Bonferroni test.
rhDAF reduces NE deposition in lung tissue in a murine model of BOP
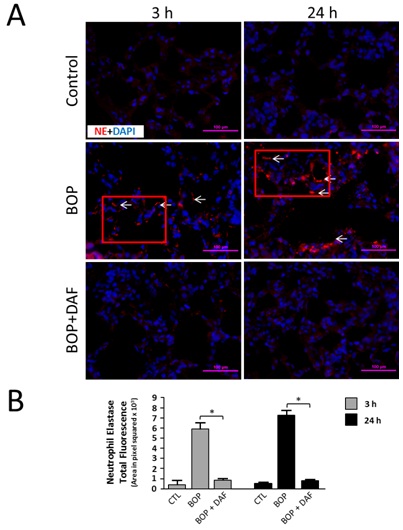
Figure 5: rhDAF decreases NE deposition in lung tissue from BOP exposed rats. A) Representative photomicrographs of the lung frozen sections were stained with anti-NE antibodies and DAPI. Original magnification of x 400. Scale bar, 100µm. Red boxes indicate region of interest for measurement whereas white arrows represent clusters of activity rather than ubiquitous activation. B) Mean fluorescence intensities were graphed. n=8 for all control, BOP-3h and BOP-24h groups. n=6 and 8 for BOP+DAF-3h and BOP+DAF-24h respectively. Total immunofluorescences were calculated using the criteria as described in the Methods. Bar graph values were expressed as mean ± SEM and compared using one-way ANOVA followed by a Bonferroni test.
rhDAF prevents increases in caspase-1 levels in the lung following BOP exposure
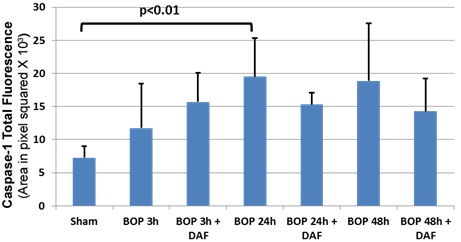
Figure 6: Caspase-1 was increased in the respiratory organ from BOP exposed rats. Mean fluorescence intensities were graphed. n=8 for sham control, BOP-3h and BOP-24h groups and n=5 for BOP-48h group. n=6, 8 and 5 for BOP+DAF-3h, BOP+DAF-24h and BOP+DAF-48h respectively. Total immunofluorescences were calculated using the criteria as described in the Methods. Graphs expressed as mean ± SEM, and compared using one-way ANOVA followed by Bonferroni test.
DISCUSSION
Blast-injury is a real and present danger for the civilian population and a greater danger to those exposed to military conflict [22]. Clinicians have very little experience in treating blast overpressure-injured patients and the best way forward for immediate and continued treatment is unknown [12]. We demonstrated in a previous manuscript that recombinant human Decay Accelerating Factor (rhDAF) administration protected a BOP animal model against Blast-Induced Neurotrauma (BINT) by suppression of both systemic and local inflammatory responses [16,20,23]. As a result, modulation of complement activation after simulated blast injury was hypothesized as a novel and significant therapeutic tool aimed at injury prevention via administration of rhDAF.
In this manuscript, we continued to evaluate the beneficial effects of complement inhibition using DAF for prevention of BOP-induced inflammatory damage to the lung and intestine, two highly susceptible organs to blast injury. There were several major findings. 1) Our model of moderate blast exposure (120kPa) induces histopathological, structural, and morphological disruptions and damage that was significantly elevated at 3, 24, and 48h post-BOP exposure per injury score assessment. 2) Intravenous rhDAF administration 30min post-BOP exposure significantly mitigated BOP induced immediate (3hours post-BOP) and delayed injury (24hours and 48hours post-BOP) (Figure 2). 3) Our data showed rhDAF deposition upon the surface of lung tissues (Figure 1) and suggest the beneficial mechanism of rhDAF treatment occurred via reduced BOP activation of C5 or competitive inhibition of C5 deposition (Figure 4), and reduction of neutrophil elastase as a marker of inflammation (Figure 5). The data presented support our hypothesis that DAF administration post-BOP ameliorates pulmonary and intestinal damage commonly produced by blast injury.
rhDAF administration promotes preservation of normal alveoli and villi structures following BOP injured lung and intestine. This finding, when considered in combination with our data of no significant differences in the mRNA expression of complement C3/C3a and C5/C5a as well as inflammatory markers IL-1β and TNFα (data not shown) between BOP and BOP+DAF groups, supports the mechanism of DAF tissue preservation as being in agreement with its previously characterized function. DAF does not interfere with lower orders of complement activation but rather prevents enzyme complex assembly upon a cellular surface [15]. However, DAF may interrupt C3a-C3aR and/or Ca-C5aR signal pathways for inhibition of cell death [24], which is supported by our findings that a trend of less caspase-1 levels with DAF administration (p>0.05, figure 6). Additionally, these signaling pathways are involved in neutrophil recruitment and activation [25], which is supported by our decrease in detection of NE in the lungs following rhDAF administration (Figure 5).
Pulmonary and intestinal tissue preservation in the trauma scenario represents tremendous leverage in survival outcomes as increase in mortality strongly correlates with Multi-Organ Dysfunction (MOD) and Failure (MOF) [26,27]. Although BOP has not been studied or shown to precipitate into MOD/F, BOP rarely occurs as a singular insult. Accompanying secondary and tertiary blast injuries contribute to the propensity for major trauma and blood loss that may lead to MOD/F. When it comes to MOD/F, prevention is the best medicine [28] which is seemingly the case with DAF administration following BOP exposure. Neutrophil Elastase (NE) data in this study cannot be clinically correlated yet strong evidence supports NE in the pathophysiology of acute lung injury and in the development of acute respiratory distress syndrome [29]. DAF significantly diminished NE concentration following BOP (Figure 5) and may therefore represent a partial mechanism for the decrease in severity of lung injury. The precise mechanism is unknown but may be related to suppression of neutrophil activation and/or inhibition of neutrophil recruitment. Injury-preventing results of DAF administration following blast are consistent with our findings of DAF therapy-induced decreases in tissue injury following hemorrhagic shock [17,18] and ischemia/reperfusion injury [19].
CONCLUSION
DAF protects lung and intestine from BOP-induced injury by direct suppression of C5/C5a deposition and therefore assembly of complement enzymatic complexes. The observed improvements in tissues investigated in the groups that received DAF administration suggest similar improvements may also be gained with DAF therapy following blast exposure in humans. DAF may represent an attractive option for use by first-responders or emergency medical technicians for improved preservation of pulmonary and intestinal tissues and allow for patient arrival at a primary point of care in a lesser critical condition.
DISCLOSURES
The views expressed in this article are those of the author and do not necessarily reflect the official policy or position of the Department of the Air Force, Department of the Navy, US Army, Department of Defense, or the US Government.
The study protocol was reviewed and approved by the Walter Reed Army Institute of Research/Naval Medical Research Center Institutional Animal Care and Use Committee in compliance with all applicable Federal regulations governing the protection of animals in research.
The authors are military members or employee of the US Government. This work was prepared as part of their official duties. Title 17 U.S.C. §105 provides that ‘‘Copyright protection under this title is not available for any work of the United States Government.’’ Title 17 U.S.C. §101 defines a US Government work as a work prepared by a military service member or employee of the US Government as part of that person’s official duties. The authors declare no competing interests or conflicts of interest.
ACKNOWLEDGEMENTS
Authorship: JJD designed the study. JEC, TO, and BJH analyzed and interpreted data. JJD, DN, and FRS supplied critical evaluation. JEC, TO, and BJH drafted the paper. This work was supported by a grant from the US Army Medical Research and Materiel Command, Fort Detrick, MD. The authors are thankful to Lingamanaidu V Ravichandran, PhD for critical review and, for the help in the revision and editorial assistance with the manuscript.
REFERENCES
- Hooker DR (1924) Physiologic effects of air concussion. American Journal of Physiology 67: 219-274.
- Zuckermann S (1940) Experimental study of blast injury to lungs. Lancet 236: 219-224.
- O'Reilly JN, Gloyne SR (1941) Blast Injury of the Lungs. The Lancet 238: 423-428.
- Fung YC, Yen RT, Tao ZL, Liu SQ (1988) A hypothesis on the mechanism of trauma of lung tissue subjected to impact load. J Biomech Eng 110: 50-56.
- Irwin RJ, Lerner MR, Bealer JF, Lightfoot SA, Brackett DJ, et al. (1998) Global primary blast injury: a rat model. J Okla State Med Assoc 91: 387-392.
- Wani I, Parray FQ, Sheikh T, Wani RA, Amin A, et al. (2009) Spectrum of abdominal organ injury in a primary blast type. World J Emerg Surg 4: 46.
- Stuhmiller JH (2010) Blast injury: Translating research into operational medicine. In: Friedl K, Santee WR (eds.). Military quantitative physiology: problems and concepts in military operational medicine. Borden Institute Monograph, USA.
- Hepper AE, Pope DJ, Bishop M, Kirkman E, Sedman A, et al. (2014) Modelling the blast environment and relating this to clinical injury: experience from the 7/7 inquest. J R Army Med Corps 160: 171-174.
- Radford P, Patel HD, Hamilton N, Collins M, Dryden S (2011) Tympanic membrane rupture in the survivors of the July 7, 2005, London bombings. Otolaryngol Head Neck Surg 145: 806-812.
- de Ceballos JP, Turegano-Fuentes F, Perez-Diaz D, Sanz-Sanchez M, Martin-Llorente C, et al. (2005) 11 March 2004: The terrorist bomb explosions in Madrid, Spain-an analysis of the logistics, injuries sustained and clinical management of casualties treated at the closest hospital. Critical Care 9: 104-111.
- Pan PP (2010) Russia braces for terrorism's return as 38 die in subway bombings. The Washington Post.
- CDC (2003) Explosions and blast injuries: A primer for clinicians. US. Department of Health & Human Services, GA, USA.
- Dalle Lucca JJ, Li Y, Simovic M, Pusateri AE, Falabella M, et al. (2012) Effects of C1 inhibitor on tissue damage in a porcine model of controlled hemorrhage. Shock 38: 82-91.
- Ioannou A, Lieberman LA, Dalle Lucca JJ, Tsokos GC (2013) Complement depletion protects lupus-prone mice from ischemia-reperfusion-initiated organ injury. American Journal of Physiology - Gastrointestinal & Liver Physiology 304: 283-292.
- Fujita T, Inoue T, Ogawa K, Iida K, Tamura N (1987) The mechanism of action of Decay-Accelerating Factor (DAF). DAF inhibits the assembly of C3 convertases by dissociating C2a and Bb. J Exp Med 166: 1221-1228.
- Li Y, Chavko M, Slack JL, Liu B, McCarron RM, et al. (2013) Protective effects of decay-accelerating factor on blast-induced neurotrauma in rats. Acta Neuropathol Commun 1: 52.
- Dalle Lucca JJ, Li Y, Simovic MO, Slack JL, Cap A, et al. (2013) Decay-accelerating factor limits hemorrhage-instigated tissue injury and improves resuscitation clinical parameters. J Surg Res 179: 153-167.
- Dalle Lucca JJ, Simovic M, Li Y, Moratz C, Falabella M, et al. (2011) Decay-accelerating factor mitigates controlled hemorrhage-instigated intestinal and lung tissue damage and hyperkalemia in swine. J Trauma 71: 151-160.
- Lu X, Li Y, Simovic MO, Peckham R, Wang Y, et al. (2011) Decay-accelerating factor attenuates C-reactive protein-potentiated tissue injury after mesenteric ischemia/reperfusion. J Surg Res 167: 103-115.
- Wang Y, Li Y, Dalle Lucca SL, Simovic M, Tsokos GC, et al. (2010) Decay accelerating factor (CD55) protects neuronal cells from chemical hypoxia-induced injury. J Neuroinflammation 7: 24.
- Weeks C, Moratz C, Zacharia A, Stracener C, Egan R, et al. (2007) Decay-accelerating factor attenuates remote ischemia-reperfusion-initiated organ damage. Clin Immunol 124: 311-327.
- Mackenzie IM, Tunnicliffe B (2011) Blast injuries to the lung: epidemiology and management. Philos Trans R Soc Lond B Biol Sci 366: 295-299.
- Dalle Lucca JJ, Chavko M, Dubick MA, Adeeb S, Falabella MJ, et al. (2012) Blast-Induced moderate Neurotrauma (BINT) elicits early complement activation and Tumor Necrosis Factor alpha (TNFα) release in a rat brain. J Neurol Sci 318: 146-154.
- Salter MW, Kalia LV (2004) Src kinases: a hub for NMDA receptor regulation. Nat Rev Neurosci 5: 317-328.
- Guo RF, Ward PA (2005) Role of C5a in inflammatory responses. Annu Rev Immunol 23: 821-852.
- Fry DE (1988) Multiple system organ failure. Surg Clin North Am 68: 107-122.
- Khwannimit B (2008) Serial evaluation of the MODS, SOFA and LOD scores to predict ICU mortality in mixed critically ill patients. J Med Assoc Thai 91: 1336-1342.
- Baue AE (1999) Sepsis, Multi-Organ Dysfunction Syndrome (MODS) and Multiple Organ Failure (MOF). Prevention is better than treatment. Minerva Anestesiol 65: 477-480.
- Kawabata K, Hagio T, Matsuoka S (2002) The role of neutrophil elastase in acute lung injury. Eur J Pharmacol 451: 1-10.
Citation: Campbell JE, Oh T, Hurtgen BJ, Niemeyer DM, Sheppard FR, et al. (2015) Blast Overpressure Induced Pulmonary and Intestinal Damage is Ameliorated by Post-injury Decay Accelerating Factor Injection. J Clin Immunol Immunother 2: 007.
Copyright: © 2015 James E Campbell, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

