
Calciphylaxis or Calcific Uremic Arteriolopathy: Diagnosis not to be Overlooked in Hemodialysis Patients
*Corresponding Author(s):
Dina Ibrahim MontasserNephrology Department, Military Hospital Of Instruction Mohmmed V, University Of Medicine And Pharmacology, Rabat, Morocco
Email:dirm80@hotmail.com
Abstract
Calciphylaxis or calcific uremic arteriolopathy is a rare and severe condition due to its painful ischemic necrosis cutaneous and sometimes systemic lesions, whose functional and vital prognosis is reserved due to infectious complications. Several factors are implicated, but the physiopathology is not yet fully understood. Its treatment is poorly codified based mainly on a treatment of pain, tissue oxygenation, the release of calcium salts of vessels and the elimination of factors and promoting drugs. We illustrate through a clinical case the essential points to recognize on this pathology.
INTRODUCTION
Calcific Uremic Arteriolopathy (CUA) or "Calciphylaxis" is an ischemic necrosis, cutaneous and sometimes systemic, mainly affecting chronic Hemodialysis (HDC), due to the obliteration of the arterioles first by subintimal calcium deposits, then by thrombosis. Its diagnosis is rarely mentioned, leading the clinician to multiple differential diagnoses.
CLINICAL OBSERVATION
A 75-year-old, hemodialysis patient with diabetic nephropathy, treated with Anti-Vitamin K (AVK) for a complete arrhythmia by atrial fibrillation, presenting a cutaneous necrosis of the lower limbs (MI) evolving in recent weeks (Figure 1). A skin biopsy brings up at first reading the diagnosis of bullous dermatitis justifying treatment with immunosuppressant but without improvement after several days. Upon arrival in our unit, the patient had a fever at 38°C and very painful necrotic skin lesions sitting along the right MI and left heel. The biological assessment reveals a hyperleukocytosis with neutrophils at 13,800 elements/mm3, hemoglobin at 6.8g/dl, TP at 39%. An inflammatory syndrome with a CRP at 230 mg/l, a fibrinogen at 7g/l and a ferritinemia at 400μg/l. The calcemia is at 92mg/dl, the phosphoremia at 74mg/dl or a Ca×P product at 6808mg²/dl²; parathormone 1-84 at 591pg/ml. The rereading of the skin biopsy reveals an infiltration of the wall of the small and medium-sized vessels by calcium deposits by standard and Von Kossa stains, indicating the stopping of immunosuppressants and AVK with regular skin care and daily dialysis by low baths calcium concentration 1.25mmol/l.
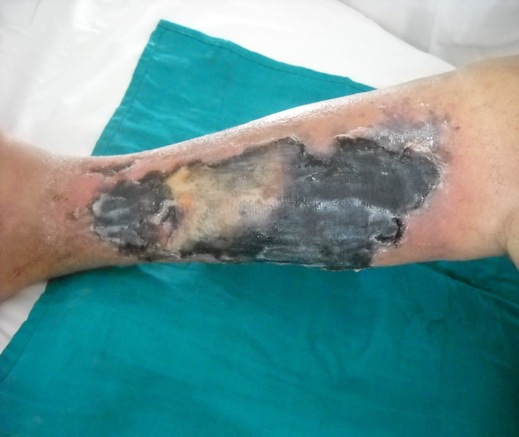 Figure 1: A skin biopsy.
Figure 1: A skin biopsy.
At 3 months of the onset of symptoms, the patient reveals hepatocellular insufficiency and dies in a table of pseudomonas aeruginosa and staphylococcus aureus septicemia.
DISCUSSION
Calcifying uremic arteriolopathy "AUC" is a rare pathology, its incidence is variable according to the literature ranging from 0.04% according to the American register [1] and reaches 4% according to the Martinique register [2]. Many risk factors are raised, in particular diabetes, obesity and the female sex with an average age of 50 years, as well as the use of AVK, with presence of risk factor superadded in hemodialysis patients like hyperphosphoremia, seniority in dialysis> 10 years and VIT D and Ca supplementation treatments, martial supplementation or even corticotherapy-based treatments [3,4].
The pathogenesis of AUC remains poorly understood and incomplete since not all patients who have its risk factors will develop calciphylaxis lesions; nevertheless the process of systemic vascular and soft tissue calcifications is responsible for the reduction of arteriolar blood flow with calcification and fibrosis and the formation of thrombi in the dermo-hypodermic arterioles with the installation of a state of hypercoagulability and tissue ischemia, associated with this mechanism the elevation of the phospho-calcic product incriminated as well as the hyperparathyroidism in the hemodialysis patients and the chronic inflammatory states which can also be responsible for the appearance of CUA as in the case of connectivites "crohn, auto disease -immune ”or neoplastic disorders reported by certain publications [5,6,7].
The diagnosis must be urgent. The clinic is dominated by lesions of livedo, ulcers or necrotic plaques of locations often distal as in our patient who had lesions in the leg and heel, or proximal or in the fatty areas (trunk, abdomen) [7]. It can pose a problem of differential diagnosis with cholesterol embolism, anti-phospholipid syndrome, anti-vitamin k necrosis, bullous dermatitis, ocher ulcer of venous insufficiency and nephrogenic systemic fibrosis [8].
The treatment is less well codified but the most specific treatment used in the first intention is sodium thiosulfate with a dose adapted to renal function from 12.5 to 25mg/day without exceeding 2.5mg/kg which allows dissociation of the salts calcium with antioxidant effect and local vasodilation [9].
The treatment is also based on hemodialysis patients on the reduction of the calcium-phsphorus product and the correction of risk factors by the use of baths low in calcium 1.25mmol/l as well as the non-calcium phosphorus chelators "sevelamer carbonate or lanthanum carbonate and the use of calcimimetic “cinacalcet” for treatment of PHT and avoiding low blood pressure.
Martial therapy should be discontinued in dialysis patients.
If despite the therapeutic measures and beyond 3 months the patient is declared in therapeutic failure and resistant to treatment with indication of hyperbaric oxygen therapy, some writings recommend the use of biphosphonates if treatment failure [10].
This treatment can be accompanied by local treatment of necrosis by surgical debridement and dressing with MEOPA. Other treatments are being tested such as plasminogen activators and treatment with green larvae of the "lucilia sericata" fly or the rheopherae [11].
The life prognosis is poor (60 to 80% of mortality) given the high risk of systemic infection linked to skin lesions [6]; increased by the female sex 59%, the advanced stage of renal failure, insulin-dependent diabetes, obesity as well as the potential deleterious effect of AVK and insulin injections aggravating the lesions as in our patient associated with disturbances phosphocalcic balance such as hypercalcemia, hyperphosphoremia, hyperparathyoidism and hypervitaminosis D.
CONCLUSION
AUC is a thrombotic cutaneous microangiopathy responsible for ischemia phenomena and particularly painful skin necrosis of dialysis patients. Several factors are incriminated, mainly obesity, diabetes, female gender, AVK, elevated phosphocalcic product, hyperparathyroidism, overdoses of calcium and vitamin supplements, and chronic inflammatory phenomena. The treatment consists in quickly restoring a normal phospho-calcium balance. The vital prognosis is often engaged.
No conflicts of interest.
REFERENCES
- Arch-Ferrer JE, Beenken SW, Rue LW, Blanda KI, Diethelm AG (2003) Therapy for calciphylaxis: An outcome analysis. Surgery 134: 941-945.
- Nigwekar SU, Solid CA, Ankers E, Malhotra R, Eggert W, et al. (2014) Quantifyinga rare disease in administrative data: The example of calciphylaxis. J Gen Intern Med 29: 724-731.
- Hafner J, Keuch G, Wahl C, Sauter B, Hurlimann A, et al. (1995) Uremicsmall-artery disease with medial calcification and intimal hyperplasia (socalled calciphylaxis): A complication of chronic renal failure and benefit from parathyroidectomy. J Am Acad Dermatol 33: 954-962.
- Leray H, Dereure O, Canaud B, Teot L, Guilhou JJ, et al. (1995) Necrotic angiodermitis revealing a florid hyperparathyroidism secondary to a chronic renal insufficiency: Healing after subtotal parathyroidectomy. Nephrologie 16: 427-4230.
- Galloway PA, El-Damanawi R, Bardsley V, Pritchard NR, Fry AC, et al. (2015) Vitamin K antagonists predispose to calciphylaxis in patients with end-stagerenal disease. Nephron 129: 197-201.
- Chettati M, Adnouni A, Fadili W, Laouad I (2018) Calcific uremic arteriolopathy in hemodialysis patient, review of literature through five cases reports. Nephrol Ther 14: 439-445.
- Nigwekar SU, Han I, Turchin A, Skentzos SC, Hajhosseiny R, et al. (2013) Statin use and calcific uremic arteriolopathy: A matched case-control study. Am J Nephrol 37: 325-332.
- Mazhar AR, Johnson RJ, Gillen D, Stivelman JC, Ryan MJ, et al. (2001) Risk factors and mortality associated with calciphylaxis in end-stage renal disease. Kidney Int 60: 324-332.
- Fine A, Zacharias J (2002) Calciphylaxis isusually non-ulcerating: Risk factors, outcome and therapy. Kidney Int 61: 2210-2217.
- Nigwekar SU, Kroshinsky D, Nazarian RM, Goverman J, Malhotra R, et al. (2015) Calciphylaxis: Risk factors, diagnosis, and treatment. Am J Kidney Dis 66: 133-146.
- Hackett BC, McAleer MA, Sheehan G, Powell FC, O’Donnell BF (2009) Calciphylaxis in a patient with normal renal function: response to treatment with sodium thiosulfate. Clin Exp Dermatol 34: 39-42.
Citation: Montasser DI, Issouani J, Belmajdoub G, Kabbaj D (2020) Calciphylaxis or Calcific Uremic Arteriolopathy: Diagnosis not to be Overlooked in Hemodialysis Patients. J Nephrol Renal Ther 6: 032.
Copyright: © 2020 Dina Ibrahim Montasser, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

