
Journal of Surgery Current Trends & Innovations Category: Clinical
Type: Research Article
Choosing the Appropriate Reconstructive Technique for Eyelid Defects after Tumor Excision
*Corresponding Author(s):
Sokol IsarajDepartment Of Surgery, “Mother Theresa” University Hospital Center Of Tirana, Tirana, Albania
Tel:+355 682235355,
Email:sokol.isaraj@gmail.com
Received Date: Oct 16, 2019
Accepted Date: Oct 30, 2019
Published Date: Nov 06, 2019
Abstract
Background
Due to the anatomic location reconstruction of the eyelids after tumor removal remains one of the most challenging tasks in reconstructive surgery. Our strategy favors a progression from direct closure, when possible, to use of local flaps in combination with chondro-mucosal grafts for bi-lamellar reconstruction.
Material and methods
After institutional review board approval, we collected and analyzed the medical records of 97 patients who underwent eyelid surgery for skin cancer between May 2016-May 2019 in a tertiary care center.
Results
97 patients were operated for a skin cancer of the eyelid over the 3 years period. There were 52 males and 45 females aged between 36 to 84 years. The lower eyelid was the most common site involved, followed by the medial canthus, upper eyelid and the lateral canthus. The histopathological report classified basal cell carcinoma as the most common type. Surgical techniques progressed from simple excision and direct closure, to complex reconstructions such as skin grafting, cantholysis, flaps plus septal chondro-mucosal grafts for subtotal or total eyelid reconstruction.
Conclusion
This is a retrospective, descriptive study with emphasis on the different surgical techniques along with the outcomes of three patients after eyelid reconstruction with chondro-mucosal graft and skin flaps. The present study emphasizes the advantages of using chondro-mucosal grafts in comparison to other grafts. We were able to achieve excellent aesthetic outcomes without facing any structural complications such as flap failure, dehiscence, infection, ectropion, recurrence, irregular eyelid margins.
Due to the anatomic location reconstruction of the eyelids after tumor removal remains one of the most challenging tasks in reconstructive surgery. Our strategy favors a progression from direct closure, when possible, to use of local flaps in combination with chondro-mucosal grafts for bi-lamellar reconstruction.
Material and methods
After institutional review board approval, we collected and analyzed the medical records of 97 patients who underwent eyelid surgery for skin cancer between May 2016-May 2019 in a tertiary care center.
Results
97 patients were operated for a skin cancer of the eyelid over the 3 years period. There were 52 males and 45 females aged between 36 to 84 years. The lower eyelid was the most common site involved, followed by the medial canthus, upper eyelid and the lateral canthus. The histopathological report classified basal cell carcinoma as the most common type. Surgical techniques progressed from simple excision and direct closure, to complex reconstructions such as skin grafting, cantholysis, flaps plus septal chondro-mucosal grafts for subtotal or total eyelid reconstruction.
Conclusion
This is a retrospective, descriptive study with emphasis on the different surgical techniques along with the outcomes of three patients after eyelid reconstruction with chondro-mucosal graft and skin flaps. The present study emphasizes the advantages of using chondro-mucosal grafts in comparison to other grafts. We were able to achieve excellent aesthetic outcomes without facing any structural complications such as flap failure, dehiscence, infection, ectropion, recurrence, irregular eyelid margins.
Keywords
Basal cell carcinoma; Chondro-mucosal graft; Eyelid tumor; Reconstruction technique; Skin flaps
INTRODUCTION
Approximately 5-10% of all skin cancers occur in the eyelid [1]. The eyelids represent a site with high ultraviolet exposure and predisposition to various cutaneous lesions, hence recently an increasing incidence in eyelid tumors, especially malignant ones [2]. Surgical management of eyelid cancers has always been a challenge because it requires careful surgical planning in order to achieve adequate oncologic control and minimize functional and cosmetic consequences of surgery [3]. Our reconstructive strategy favors a progression from direct closure, when possible, to using local flapsin combination with chondro-mucosal grafts for bi-lamellar reconstruction [4].
A single-stage reconstruction has been our target, without compromising the functional and aesthetic results [5].
A single-stage reconstruction has been our target, without compromising the functional and aesthetic results [5].
Objectives
The aim of this study is twofold-firstly, to provide current information about epidemiological data of eyelid cancers in our country since the patients analyzed are from a tertiary referral center; secondly, to evaluate the surgical treatment options in order to achieve the best surgical result.
MATERIALS AND METHODS
After institutional review board approval, we analyzed the medical records of 97 patients who underwent eyelid surgery between May 2016- May 2019 at the Service of Burns and Plastic Surgery, ‘’Mother Theresa” University Hospital Center of Tirana, Albania, after eyelid cancer resection. Data were collected from the medical records on patients’ charts, as well as from the records on the OR register and histopathology results register with regard to demographic information (age, gender), size of the lesion, location of the lesion, size of the defect, type of reconstructive surgery, histopathological report, eyelid opening, presence of ectropion, and aesthetic balance. This is a retrospective study of descriptive-observational nature, with emphasis on the surgical techniques used, dependent on the specific size of the defect. Along with that, we aimed to show the outcomes of three patients after eyelid reconstruction with chondro-mucosal grafts and skin flaps.
Results
A total of 97 histologically confirmed eyelid cancers where included in our study of which, 52 were males and 45 females (Figure 1). The mean age of the patients analyzed was 62.6 years, ranging from 36 to 84 years old. All the patients underwent excision of the tumor followed by immediate reconstruction of the eyelid.
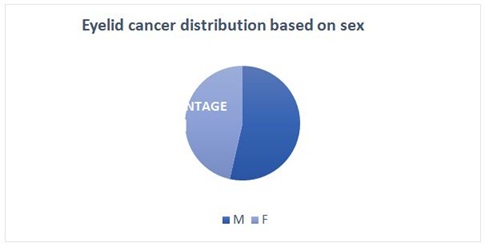
Figure 1: Eyelid cancer distribution based on sex.
Tumors were located on the lower eyelid in 46 patients (48%), on the upper eyelid in 9patients (9%), involvement of the medial canthus was found in 37 patients (38%) and the lateral can thus was affected in only in 5 patients (5%) (Figure 2).
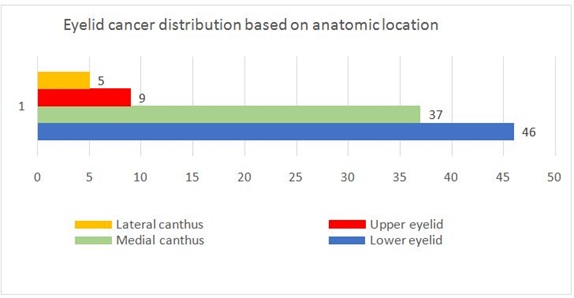
Figure 2: Effect of formaldehyde concentration on immobilization of pectin lyase from Bacillus cereus onto chitosan matrix.
Based on the histopathological report, basal cell carcinoma was the most frequent type of cancer, present in 73 patients (75%), followed by squamous cell carcinoma in 19 patients (2%), sebaceous gland carcinoma in two patients (2%), keratoachanthoma in two patients (2%) and fibrous histiocytoma in only one patient (1%) (Figure 3).
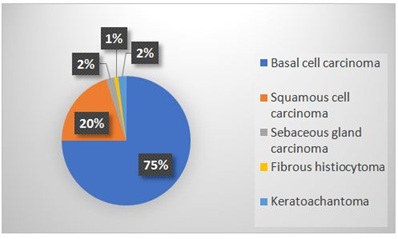 Figure 3: Histopathologic classification of eyelid cancers.
Figure 3: Histopathologic classification of eyelid cancers.Surgical technique
Surgery was carried out as a single procedure, i.e the same surgeon doing the excision and the reconstruction at the same time.
Small-sized tumors located on the lower eyelid skin with less than 3 mm in diameter, which involved less than 20% of the lid margin were excised with healthy tissue margin and closed primarily. This approach was used in 20 patients (Figure 4).
Small-sized tumors located on the lower eyelid skin with less than 3 mm in diameter, which involved less than 20% of the lid margin were excised with healthy tissue margin and closed primarily. This approach was used in 20 patients (Figure 4).
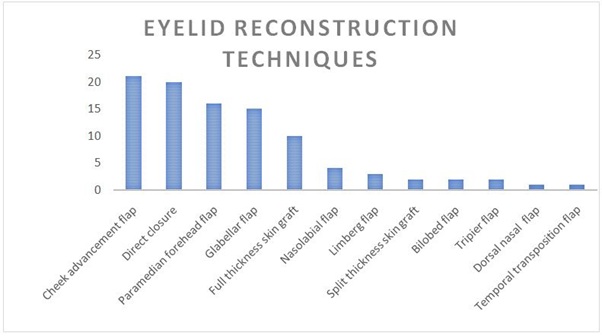
Figure 4: Eyelid reconstruction techniques used in our patients included in the study.The cheek advancement flap was the most used technique.
Medium-sized tumors located on the lower eyelid, larger than 4 mm in diameter, were excised with 3-4 mm healthy tissue margin. For the reconstruction, neighboring tissue flaps are preferred such as cheek advancement flap, glabellar flap, paramedian forehead flap, nasolabial flap, Trippier flap, dorsal nasal flap and transposition flap. Alternative options involve full-thickness skin graft harvested from the postauricular region, supraclavicular region and split-thickness skin grafts.
In patients with large-sized tumors that affected more than 50 percent of the lower eyelid or full defect of the eyelid, the internal layer was reconstructed with a chondro-mucosal graft and the external layer was reconstructed with cheek advancement flap or paramedian forehead flap. Although grafts can be harvested from the ear (as a composite chondro-cutaneous graft) or the hard palate mucosa, in our patients, grafts were, in all cases, taken from the nasal septum. A large nasal septal chondro-mucosal graft was harvested and divided to separately reconstruct the lower eyelid posterior lamella and in one case the upper eyelid. In brief, an incision through one layer of mucosa and cartilage was followed by sub-perichondrial freeing of cartilage from the mucosa of the other side. Grafts were secured to medial and lateral tissues with absorbable sutures. The nasal mucosa was used as coverage of conjunctival defect, whereas the septal cartilage used as supporting material. The outer layer of the lower eyelid was covered with a cheek advancement flap in two patients (for lower lid reconstruction), and in one patient the paramedian forehead flap was used (for upper lid reconstruction). The ultimate goal in eyelid reconstruction for full-thickness defect, should address the inner layer (conjunctiva and tarsus), and the outer layer (skin and muscle).
In 37 patients, the tumor was located in the region of the medial canthus. In two patients with small defects, they were closed by direct suturing. In 35 patients with medium to larger defects, glabellar flap, paramedian forehead flap, nasolabial flap, Limberg flap and a rotation flap from the dorsal nasal skin and full-thickness skin graft harvested from the retro auricular region, supraclavicular region, were used.
In 5 patients the tumor was located in the region of lateral canthus. In one of those the defect was closed primarily after a cantholysis, and in three others cheek advancement flap, bilobed flap and temporal transposition flap were used.
In 9 patients the tumor was located in the upper eyelid. In four of them the defect was small and closed primarily and in five others the resultant defect was of medium size and was closed by means of a flap: paramedian forehead flap, bilobed flap. In one patient with full-thickness defect with total eyelid removal, the chondro-mucosal graft was used for the posterior lamellar reconstruction and a paramedian forehead flap (on a subcutaneous pedicle) for skin resurfacing.
Case presentation 1
A 68-year-old man presented at the Dermatology Department with a pink nodule in the right lower eyelid area, which became of notice six months prior to presenting at the hospital and grew in size over the last months (Figure 5A). Aclinical diagnosis of basal cell carcinoma was made by the dermatologist.The patient underwent surgical excision under endovenous anesthesia.The carcinoma and the tarsal plate of the lower eyelid were removed with a 4 mm free margin (Figure 5B). The full thickness defect, constituting more than 1/3 of the palpebral fissure length (Figure 5C), was reconstructed with a chondro-mucosal graft harvested from the nasal septum. The length of the cartilage was fitted to the defect width. The harvested mucosa was sutured to the defect margin using an absorbable suture. The cartilage graft was sutured to the stumps of the tarsal plate and fixed to the canthal tendon. The outer layer of the defect was covered by cheek advancement flap and sutured with nonabsorbable suture (Figure 5D).The histopathological report was a basal cell carcinoma with >2mm free margin.
Postoperative functional and cosmetic results were satisfactory (Figures 5E and 5F). In long-term follow up, no signs of ectropion were seen; the septal donor site showed good healing, scar formation was minimal.
Postoperative functional and cosmetic results were satisfactory (Figures 5E and 5F). In long-term follow up, no signs of ectropion were seen; the septal donor site showed good healing, scar formation was minimal.
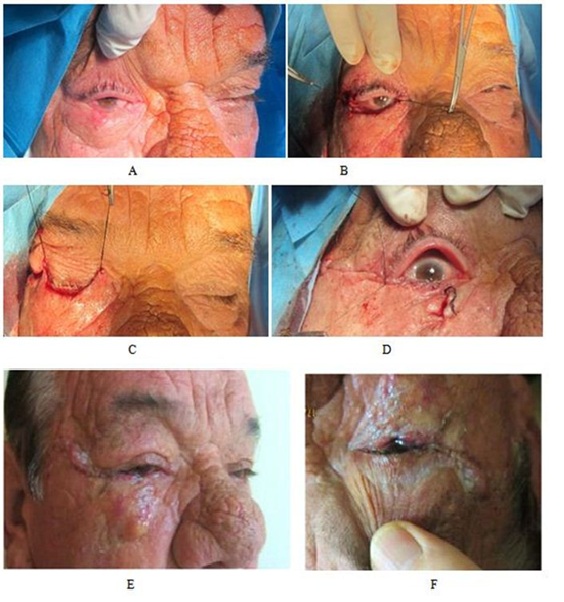
Figure 5: Patient 1 with a lower eyelid tumor, reconstructed with a chondromucosal graft from the nasalseptum and a cheek advancement flap. Defect after resection (above). Intraoperative view (center). One-week postoperative view (below).
Case presentation 2
A-56-year old woman was referred to our Department from the ophthalmologist for a recurrent lesion on the lower lid of the left eye (Figure 6A). She had two surgeries before for a BCC of the eyelid. The cancer was removed three years ago, and the defect was closed primarily. However, soon thereafter the lesion reappeared, and another procedure was done by the same surgeon: Excision and reconstruction with a Trippier flap. However, this was unsuccessful, with a recurrence of the carcinoma within months from the surgery. The third time she underwent a subtotal excision of the lower lid, followed by reconstruction with a chondro-mucosal septal graft and cheek-advancement flap (Figures 6B and 6C). The histopathological result showed total removal of the lesion with 3 mm of free margins. One year after surgery, no signs of recurrence were found; the reconstructed lid could achieve full closure of the eye, without signs of dry or infected conjunctiva (Figures 6D and 6E).
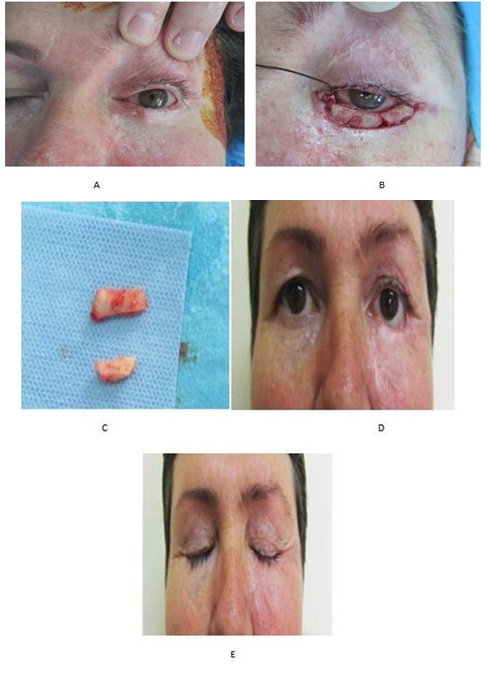 Figure 6: Patient 2 with a lower eyelid tumor, reconstructed with a chondro-mucosal graft and a cheekadvancement flap. Defect after resection (above). Intraoperative view (center). 6-months postoperative view (below).
Figure 6: Patient 2 with a lower eyelid tumor, reconstructed with a chondro-mucosal graft and a cheekadvancement flap. Defect after resection (above). Intraoperative view (center). 6-months postoperative view (below).Case presentation 3
A 75-year-old woman presented to our service after recurrence of a skin cancer on the upper eyelid. She reported that the medical historystarted 2 years ago, with the appearance of a pink bump on the upper eyelid. After being consulted by and eye surgeon, she underwent surgery by the same surgeon and the defect was closed primarily. After a couple of months the lesion reappeared (Figure 7A) and she was referred to our clinic for a wider and more radical excision with supposed need for a reconstructive procedure. A complete excision of the upper lid was done (Figure 7B). Reconstruction of the lid then followed with a nasal septal chondro-mucosal graft, and a paramedian forehead flap on a subcutaneous pedicle (Figures 7C and 7D). Flap suffered some venous congestion initially (Figure 7E), which resolved spontanously. Patient showed no recurrence of the disease one-year after the surgery with excellent functional and aesthetic result (Figures 7F and 7G).
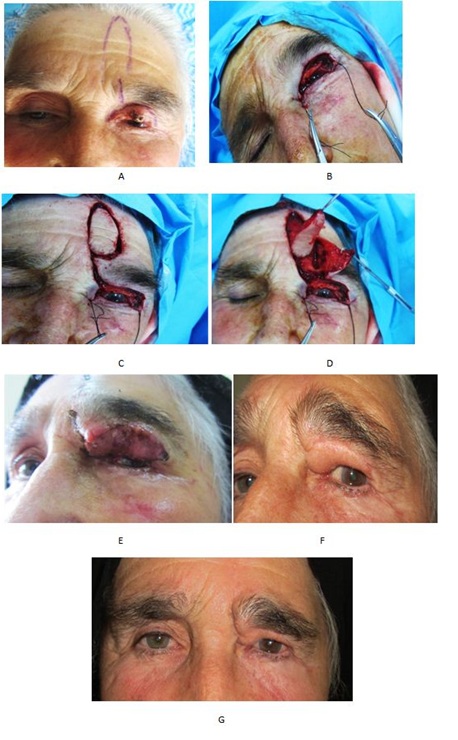 Figure 7: Patient 3 with upper eyelid tumor, reconstructed with a chondro-mucosal graft from and a paramedian forehead flap. Defect after resection (above). Intraoperative view (center). One-week postoperative view (below) and 4 months postoperative appearance (below).
Figure 7: Patient 3 with upper eyelid tumor, reconstructed with a chondro-mucosal graft from and a paramedian forehead flap. Defect after resection (above). Intraoperative view (center). One-week postoperative view (below) and 4 months postoperative appearance (below).Postoperative functional and cosmetic results were acceptable, four months follow-up showing very good cosmetic results.
DISCUSSION
Despite the clinical features, prevalence and outcome of various eyelid tumor subtypes vary significantly, related to the different geographic locations, genetic background, socio-economic status, and healthcare policies, among other factors, for the affected patients [6]. The increasing incidence in eyelid tumors is explained by several risk factors implied to the pathogenesis of these diseases. Malignant tumors of the eyelid constitute about 40% of all soft tissue tumors around the orbital region, the remaining cases being benign lesions [7].
In our series of patients, we noticed a slight predominance of males, and the major part of them, were at the sixth decade of life when diagnosed. After critical review of the literature we noticed that in various different studies the lower eyelid was the most common site affected by malignant tumors [6]. The left eyelid was most commonly associated with malignant tumors. These results are explained by the chronic UV exposure, that makes the lower eyelid more predisposed to various types of skin cancers. On the other hand, driving is linked to more skin cancers on the left part of the face, consequently the eyelid tumors are not symmetrically distributed [8].
Histologically, basal cell carcinoma was the most common type [9]. Basal cell carcinoma based on its biological behavior, most commonly presents as ulceration on the surface that doesn’t go away, hence it raises concerns and make patients seek medical advice earlier [10]. However, we encountered a lot of cases who presented with bigger lesions. This is due to their negligence to seek medical advice or to health infrastructure making it sometimes difficult to present sooner, because of their slow growth and resemblance, to benign lesions especially in the initial stage. Late surgical treatment is a significant negative prognostic factor.
Tumors located in the immediate vicinity of the eyelid margin require prompt and radical management [4]. As a basic principle in plastic surgery, grafts should be used when there is an adequate vascular bed to enhance their survival. Therefore, combining a nonvascularized graft for one lamella with a vascularized flap for the other should be the rule [7]. Mustardé incorporates the cheek advancement into defects >25% of the lower lid up to total lower lid losses, he prefers a free composite graft of nasal septum covered by the flap (30). We believe that the cheek advancement flap procedure is the most effective procedure for the reconstruction of the outer layer of the lower eyelid, as other reports have also indicated [11]. It offers considerable amount of skin with very little deformity of the donor area, while the flap is thin and no bulkiness is generally seen when healing is completed. For larger eyelid defects, the surgeon should evaluate the degree of horizontal eyelid laxity before choosing the reconstructive procedure [12]. An ideal eyelid reconstruction should be by replacing the missing tarso-conjunctival structures and skin, protecting the globe, giving the area a natural appearance, with only minor donor defect morbidity, being completed as a one-stage procedure [13]. These preliminary results show that the technique can be used in both lower and upper eyelid full thickness reconstructions [13]. Reconstruction of upper eyelid defect is very intricate, because, unlike the lower eyelid, there is not enough available tissue around it and preservation of function and contour is more demanding to achieve [14].
As a graft for an inner layer, chondro-mucosal grafts from the nasal septum have been used, for many years. Grafts from other sites including upper lateral nasal cartilages, full-thickness grafts from the contralateral lid, ear cartilage, buccal mucosa, and hard palate mucosa have also been reported to provide good results [15]. According to some authors, mucous membrane harvested from the palate together with the stroma resembles histologically the tarso-conjunctival component [16]. The disadvantages of this type of graft are as follows: (1) the surgeon may be unfamiliar with the donor region; (2) the graft may contain a minor salivary gland, leading tomucoid secretion that is difficult to treat; and (3) metaplasia of the epithelium occurs 3 to 6 months after surgery, making the technique unadvisable for upper eyelid repair because of the risk of corneal abrasion. Postoperative pain and discomfort were also reported with this type of graft [17]. The harvest of ear cartilage is simple, and its morbidity is minimal. Moreover, ear cartilage has a spherical surface and fits well to a bulbar surface [18]. The disadvantage of using ear cartilage graft is that there is no mucosa combined with the ear cartilage grafts. According to us, referring to Marks and coworkers, auricular composite grafts are too thick to be considered perfect for eyelid replacement [19]. Where as Matsuo and associates feel that conchal cartilage is ideally suited for lower eyelid reconstruction, as it is thin and supple and resembles the curvature of the globe. They report using conchal cartilage grafts alone when eyelid support and lining are needed, placing the graft in such a way that the graft perichondrium forms the posteriorlamella. Epithelialization from the surrounding mucosa is noted in 3-4 weeks [20].
Both a chondro-mucosal graft from the nasal septum and an ear cartilage graft are free grafts without a blood supply. Nasal chondro-mucosal grafts have been recommended because of the strong hyaline cartilage of the nose, which is closely associated with the mucus secreting lining of the nasal mucosa [21]. To prevent corneal irritation, a small fringe of nasal mucosa must be turned anteriorly over the cartilage to meet the remaining skin of the eyelid so that squamousepithelium does not come into contact with the globe [22]. Mustardé favors septal mucosal grafts because of the long-term stability of this cartilage [13]. The disadvantage is the length of the procedure, as the dissection of the chondro-mucosal flap should be careful and gentle, to reduce chances of perforation of the nasal septum and nasal bleeding [23].
In our series of patients, we noticed a slight predominance of males, and the major part of them, were at the sixth decade of life when diagnosed. After critical review of the literature we noticed that in various different studies the lower eyelid was the most common site affected by malignant tumors [6]. The left eyelid was most commonly associated with malignant tumors. These results are explained by the chronic UV exposure, that makes the lower eyelid more predisposed to various types of skin cancers. On the other hand, driving is linked to more skin cancers on the left part of the face, consequently the eyelid tumors are not symmetrically distributed [8].
Histologically, basal cell carcinoma was the most common type [9]. Basal cell carcinoma based on its biological behavior, most commonly presents as ulceration on the surface that doesn’t go away, hence it raises concerns and make patients seek medical advice earlier [10]. However, we encountered a lot of cases who presented with bigger lesions. This is due to their negligence to seek medical advice or to health infrastructure making it sometimes difficult to present sooner, because of their slow growth and resemblance, to benign lesions especially in the initial stage. Late surgical treatment is a significant negative prognostic factor.
Tumors located in the immediate vicinity of the eyelid margin require prompt and radical management [4]. As a basic principle in plastic surgery, grafts should be used when there is an adequate vascular bed to enhance their survival. Therefore, combining a nonvascularized graft for one lamella with a vascularized flap for the other should be the rule [7]. Mustardé incorporates the cheek advancement into defects >25% of the lower lid up to total lower lid losses, he prefers a free composite graft of nasal septum covered by the flap (30). We believe that the cheek advancement flap procedure is the most effective procedure for the reconstruction of the outer layer of the lower eyelid, as other reports have also indicated [11]. It offers considerable amount of skin with very little deformity of the donor area, while the flap is thin and no bulkiness is generally seen when healing is completed. For larger eyelid defects, the surgeon should evaluate the degree of horizontal eyelid laxity before choosing the reconstructive procedure [12]. An ideal eyelid reconstruction should be by replacing the missing tarso-conjunctival structures and skin, protecting the globe, giving the area a natural appearance, with only minor donor defect morbidity, being completed as a one-stage procedure [13]. These preliminary results show that the technique can be used in both lower and upper eyelid full thickness reconstructions [13]. Reconstruction of upper eyelid defect is very intricate, because, unlike the lower eyelid, there is not enough available tissue around it and preservation of function and contour is more demanding to achieve [14].
As a graft for an inner layer, chondro-mucosal grafts from the nasal septum have been used, for many years. Grafts from other sites including upper lateral nasal cartilages, full-thickness grafts from the contralateral lid, ear cartilage, buccal mucosa, and hard palate mucosa have also been reported to provide good results [15]. According to some authors, mucous membrane harvested from the palate together with the stroma resembles histologically the tarso-conjunctival component [16]. The disadvantages of this type of graft are as follows: (1) the surgeon may be unfamiliar with the donor region; (2) the graft may contain a minor salivary gland, leading tomucoid secretion that is difficult to treat; and (3) metaplasia of the epithelium occurs 3 to 6 months after surgery, making the technique unadvisable for upper eyelid repair because of the risk of corneal abrasion. Postoperative pain and discomfort were also reported with this type of graft [17]. The harvest of ear cartilage is simple, and its morbidity is minimal. Moreover, ear cartilage has a spherical surface and fits well to a bulbar surface [18]. The disadvantage of using ear cartilage graft is that there is no mucosa combined with the ear cartilage grafts. According to us, referring to Marks and coworkers, auricular composite grafts are too thick to be considered perfect for eyelid replacement [19]. Where as Matsuo and associates feel that conchal cartilage is ideally suited for lower eyelid reconstruction, as it is thin and supple and resembles the curvature of the globe. They report using conchal cartilage grafts alone when eyelid support and lining are needed, placing the graft in such a way that the graft perichondrium forms the posteriorlamella. Epithelialization from the surrounding mucosa is noted in 3-4 weeks [20].
Both a chondro-mucosal graft from the nasal septum and an ear cartilage graft are free grafts without a blood supply. Nasal chondro-mucosal grafts have been recommended because of the strong hyaline cartilage of the nose, which is closely associated with the mucus secreting lining of the nasal mucosa [21]. To prevent corneal irritation, a small fringe of nasal mucosa must be turned anteriorly over the cartilage to meet the remaining skin of the eyelid so that squamousepithelium does not come into contact with the globe [22]. Mustardé favors septal mucosal grafts because of the long-term stability of this cartilage [13]. The disadvantage is the length of the procedure, as the dissection of the chondro-mucosal flap should be careful and gentle, to reduce chances of perforation of the nasal septum and nasal bleeding [23].
CONCLUSION
This is a retrospective, descriptive study with emphasis on the different surgical techniques along with the outcomes of three patients after eyelid reconstruction with chondro-mucosal graft and skin flaps. We were able to achieve excellent aesthetic outcomes without facing any structural complications such as flap failure, dehiscence, infection, ectropion, recurrence, irregular eyelid margins.
Most of cases are cancers of basal cell type and, if treated early, can result in better functional and cosmetic result. Customizingre construction is necessary to provide the proper surgery for each patient. Excision of the lesion with a 3- to 4-mmmargin is believed to be a safe management in basal cell carcinoma.
Reconstruction of the defect is done according to the size of the defect and the involvement of the different layers of the lids, from simple closure for defects of less than 1/3 of the palpebral fissure, to skin grafts for defects only of the skin, and complex reconstruction with chondro-mucosal grafts and flaps for skin replacement. Appropriate reconstruction surgery management requires a specialized plan for each patient.
This study has demonstrated the two most significant factors in achieving good reconstruction results: The composition of the graft for internal lining and the design of the flap for external cover.
Most of cases are cancers of basal cell type and, if treated early, can result in better functional and cosmetic result. Customizingre construction is necessary to provide the proper surgery for each patient. Excision of the lesion with a 3- to 4-mmmargin is believed to be a safe management in basal cell carcinoma.
Reconstruction of the defect is done according to the size of the defect and the involvement of the different layers of the lids, from simple closure for defects of less than 1/3 of the palpebral fissure, to skin grafts for defects only of the skin, and complex reconstruction with chondro-mucosal grafts and flaps for skin replacement. Appropriate reconstruction surgery management requires a specialized plan for each patient.
This study has demonstrated the two most significant factors in achieving good reconstruction results: The composition of the graft for internal lining and the design of the flap for external cover.
REFERENCES
- Cook BE Jr, Bartley GB (2001) Treatment options and future prospects for the management of eyelid malignancies: an evidence-based update. Ophthalmology 108: 2088-2098.
- Lin HY, Cheng CY, Hsu WM, Kao WH, Chou P (2006) Incidence of eyelid cancers in Taiwan: a 21-year review. Ophthalmology 113: 2101-2107.
- Zimmerman AC, Klauss V (2001) [Predictors of recurrent basalioma of the eyelids and periorbital region]. Ophthalmologe 98: 555-559.
- Alghoul M, Pacella SJ, McClellanT, Codner MA (2013) Eyelid reconstruction. Plastic and Reconstructive Surgery 132: 288-302.
- Holds JB (2016) Lower Eyelid Reconstruction. Facial Plast Surg Clin North Am 24: 183-191.
- Deprez M, Uffer S (2009) Clinicopathological features of eyelid skin tumors. A retrospective study of 5504 cases and review of literature. Am J Dermatopathol 31: 256-262.
- Wójcicki P, Zachara M (2010) Surgical Treatment of Eyelid Tumors. J Craniofac Surg 21: 520-525.
- Butler ST, Fosko SW (2010) Increased prevalence of left-sided skin cancers. J Am Acad Dermatol 63: 1006-1010.
- Rowe DE, Carroll RJ, Day CL Jr (1989) Mohs surgery is the treatment of choice for recurrent (previously treated) basal cell carcinoma. J Dermatol Surg Oncol 15: 424-431.
- Mak ST, Wong AC, Io IY, Tse RK (2011) Malignant eyelid tumors in Hong Kong 1997-2009. Jpn J Ophthalmol 55: 681-685.
- Millard DR Jr (1962) Eyelid repairs with a chondromucosal graft. Plast Reconstr Surg Transplant Bull 30: 267-272.
- Kakizaki H, Malhotra R, Madge SN, Selva D (2009) Lower eyelid anatomy: An update. Ann Plast Surg 63: 344-351.
- Scuderi N, Rubino C (1994) Island chondro-mucosal flap and skin graft: a new technique in eyelid Reconstruction. Br J Plast Surg 47: 57-59.
- Scuderi N, Ribuffo D, Chiummariello S (2005) Total and subtotal upper eyelid reconstruction with the nasal chondromucosal flap: A 10-year experience. Plast Reconstr Surg 115: 1259-1265.
- Werner MS, Olson JJ, Putterman AM (1993) Composite grafting for eyelid reconstruction. Am J Ophthalmol 116: 11-16.
- Cheng JX, Zuo L, Huang XY, Cui JZ, Wu S, et al. (2015) Full-thickness reconstruction of the eyelid with rotation flaps through “subcutaneous tunnel” and palatal mucosal grafts. Int J Ophthalmol 8: 794-799.
- Fernandes JBVD, Nunes TP, Matayoshi S, Moura EM (2003) Enxerto de mucosa do palato duro: complicações na área doadora - Relato de casos. Arq Bras Oftalmol 66: 884-886.
- Su SY, Giorlando F, Ek EW, Dieu T, et al. (2007) Incomplete excision of basal cell carcinoma: A prospective trial. Plast Reconstr Surg 120: 1240-1248.
- Marks MW, Argenta LC, Friedman RJ, Hall JD (1989) Conchal cartilage and composite grafts for correction of lower lid retraction. Plast Reconstr Surg 83: 629-635.
- Matsuo K, Hirose T, Takahashi N, Iwasawa M, Satoh R (1987) Lower eyelid reconstruction with a conchal cartilage graft. Plast Reconstr Surg 80: 547-552.
- Thornton JF, Kenkel JM (2005) Eyelid reconstruction. SRPS 10: 1-50.
- Mustarde JC (1980) Repair and Reconstruction in the Orbital Region. Edinburgh, Churchill-Livingstone, London, UK.
- Wójcicki P, Zachara M (2010) Surgical Treatment of Eyelid Tumors. J Craniofac Surg 21: 520-525.
Citation: Isaraj S, Kola I, Kola E (2019) Choosing the Appropriate Reconstructive Technique for Eyelid Defects after Tumor Excision. J Surg Curr Trend Innov 3: 023.
Copyright: © 2019 Sokol Isaraj, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

Journal Highlights
© 2026, Copyrights Herald Scholarly Open Access. All Rights Reserved!
