
Clinical Features of Sporotrichosis
*Corresponding Author(s):
Ana San Juan RomeroMycology Section, “Dr. Manuel GeaGonzalez” General Hospital, Mexico City, Mexico
Email:anasjr@hotmail.com
Abstract
Sporotrichosis is a mycosis caused by Sporothrixschenckii complex. Generallyoccurs by traumatic inoculation. It has a wide variety of clinical presentations and can affect the skin, lungs, bones, joints and other organs. The paper reviews the current scientific literature data on sporotrichosisand the different clinical presentations.
Results: Sporotrichosis is classified as primary cutaneous disease, with three main clinical presentations: lymphocutaneous, fixed-cutaneous and disseminated; and the systemic disease. The predominant form is lymphangitic sporotrichosis, which represents 60-80% of cases in Mexico.
Keywords
Clinical types; Mycosis; Sporothrixschenckii; Sporotrichosis
Introduction
Sporotrichosis is caused by the dimorphic fungus Sporothrix schenckii complex which includes S. brasiliensis, S. albicans, S. mexicana, S. schenckiisensustricto and S. globose [1]. It has a worldwide distribution, especially in the tropical and subtropical zones [2]. The infection generally occurs by traumatic inoculation of plants, soil and organic matter that contains the fungus. It can also be acquired by inhalation of spores, although this form of transmission is not common. It has a wide variety of clinical presentations. Hematogenous dissemination can also occur, especially in immunocompromised hosts. It can affect the skin, lungs, bones, joints and other organs [3]. Animals can act as vectors of the disease, cats in particular have been shown to carry a large number of fungus in their nails and oral cavity [4]. Treatment options include solution of potassium iodide, itraconazole, fluconazole, amphotericin B and terbinafine [5].
Purpose of the Study
Study the course of sporotrichosis and the different clinical presentations.
Materials and Methods
A systematic search on the subject was performed in PubMed, EmbaseandGoogle Scholar databases. The key-words used from the Medical Searching Heading (MeSH) were: ‘Sporotrichosis’ or ‘Sporothrixschenckii’, and ‘Clinical Features’ or ‘Clinical Manifestations’ and ‘cutaneous’ or ‘Systemic’. We selected manuscripts written in English or Spanish between January 2000 and October 2020. Literature sources published in another languagewere excluded from the study.
Results
The host immune state, the size of the inoculum and the depth of traumatic inoculation have all been attributed to play a role in the development of infection by Sporothrix. It is classified as primary cutaneous disease, with three main clinical presentations:
- Lymphocutaneous
- Fixed-cutaneous
- Disseminated
The lymphangitic sporotrichosis represents 60-80% of cases in Mexico, fixed cutaneous 10-30% and disseminated 2-5% [6]. In cutaneous manifestations we can include cutaneous disseminated and systemic disseminated. Extracutaneous disease includes osteoarticular [7], which is the most common; pulmonary and mucous.
Lymphocutaneous
After penetrating through the skin, the fungus converts into the yeast form and extends along the adjacent lymphatic vessels, constituting the lymphocutaneous form. The primary lesion is usually located on the extremities, especially hands and forearms, corresponding to the sites most exposed to trauma [8]. The first symptoms appear approximately 3 weeks after the infection is acquired, but this may be delayed up to 6 months. Initially a small indurated papule or pustule is followed by slowly enlargement and becomes nodular. This lesion, exerting pressure beneath the skin, causes ischemia under the epidermis, evolves into gum, ulcerates and oozes a purulent secretion. As the disease progresses, secondary lesions arise along the path of regional lymphatics (Figure 1) [9]. Lymph node involvement is unusual. Important differential diagnosis of this form of sporotrichosis include leishmaniasis, atypical mycobacterial infection, tularemia, nocardiosis and other inoculation fungal infections.
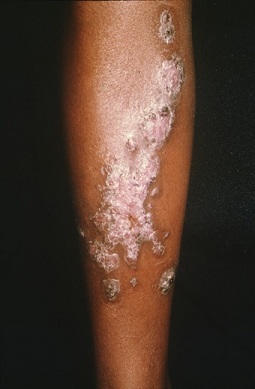 Figure 1: Lymphocutaneous sporotrichosis.
Figure 1: Lymphocutaneous sporotrichosis.
Fixed-Cutaneous
Fixed cutaneous sporotrichosis occurs less often and is characterized by localized lesions without lymphatic involvement. Sites affected most often are the face, neck, trunk or legs. These lesions are characterized by a painless, infiltrated, erythematous, or violaceous plaque that may become verrucous or ulcerated. The lesions may show spontaneous resolution, but they usually return and persist for years if not treated [10]. Differential diagnosis include leishmaniasis, verrucous tuberculosis, syphilis, leprosy and other inoculation fungal infections.
Disseminated
Disseminated sporotrichosis (5%) has two variants: disseminated cutaneous and systemic; in the latter there is weight loss, fever, disseminated skin lesions and there may be fungemia. It occurs as a result of hematogenous spread from the primary inoculation. Disseminated cutaneous only affects the skin, and shows an adequate response to treatment; it has been considered that it may depend on multiple inoculations or self-inoculation. Clinical picture are multiple lesions scattered over several body sites. Skin lesions consist of gums that may ulcerate, or even warty or scaly plaques. It tends to affect immunocompromised patients [11]. In transmission by cats, several inoculations in different locations may occur [12].
A mucosal form has been described as a variant of the cutaneous form. They are consequence of self-inoculation through hands contaminated with the fungus, hematogenous dissemination or inhalation of conidia [13]. In the conjunctiva, the granulomatous lesion is accompanied by a serous or purulent discharge, redness and lid edema [14]. Nasal mucosa lesions often involve drainage of bloody secretions and detachment of crusts, and can affect the septum. Mucosal forms often are accompanied by submandibular and preauricular lymph node involvement [15].
Systemic Disease
Systemic involvement usually occurs with immunosuppression; thus, the infection may be considered opportunistic and carries a bad prognosis. It may manifest in the form of arthritis (it is the most important mycotic arthropathy, and has a tendency to affect mainly the knee), osteomyelitis, pyelonephritis, orchitis and mastitis. Sporotrichosis may affect the central nervous system, causing meningitis, [16] or it may affect the peripheral nerves, resulting in neuropathy [17]. Pulmonary sporotrichosis is not common, nonetheless several cases have been reported. It can be accompanied by fever, weight loss and fungemia. Dermatologic syndromes, such as erythema nodosum and erythema multiforme, have been described in association with sporotrichosis [18].
Conclusion
The clinical picture of sporotrichosis is heterogeneous and has its own characteristics. It affects both men and women of any age group, but is most commonly found in people aged 16 to 30 years. The main clinical presentations are the lymphocutaneous, fixed-cutaneous, disseminated and the extracutaneous disease, which can affect any organ. Treatment regimens last for several months and in HIV-patients can be for a lifetime. Further study of the characteristics of sporotrichosis will make it possible to develop more effective measures for the timely diagnosis of this disease.
References
- Marimon R, Cano J, Gene J, Sutton DA, Kawasaki M, et al. (2007) Sporothrix brasiliensis, S. globosa, and S. mexicana, three new Sporothrix species of clinical interest. J Clin Microbiol45:3198-206.
- Neyra E, Fonteyne PA, Swinne D, Fauche F, Bustamante B, et al. (2005) Epidemiology of human sporotrichosis investigated by amplified fragment length polymorphism. J Clin Microbiol 43: 1348-1352...
- Rivitti EA, Aoki V (2000) Deep fungal infections in tropical countries. Clin Derm 17: 171-190.
- Reis RS, Almeida-Paes R, Muniz MM, Tavares PMS, Monteiro PCF, et al.(2009) Molecular characterisation of Sporothrix schenckii isolates from humans and cats involved in the sporotrichosis epidemic in Rio de Janeiro, Brazil. Mem Inst Oswaldo Cruz 104: 769-774.
- Kauffman CA, Hajjeh R, Chapman SW (2000) Practiceguidelines for the management of patients withsporotrichosis. CID 30: 684-687.
- Arenas R (2008) Micologia Medica Ilustrada. 3rdedn. Mexico City, Mexico: McGraw-Hil, Page no: 149-160.
- Orofino-Costa R, Boia MN, Magalhaes GA, Damasco PS, Bernardes-Engemann AR, et al. (2010) Arthritis as a hypersensitivity reaction in a case of sporotrichosis transmitted by a sick cat: clinical and serological follow up of 13 months. Mycoses 53: 81-83.
- Pappas PG, Deep AE, Nolasco D, Holgado W, et al. (2000) Sporotrichosis in Peru: Description of an area of hyperendemicity. Clin Inf Dis 20: 65-70.
- Bonifaz A, Vazquez-Gonzalez D, Perusquia-Ortiz AM (2010) Subcutaneous mycoses: chromoblastomycosis, sporotrichosis and mycetoma. J Dtsch Dermatol Ges 8: 619-627.
- Shiraishi H, Gomi H, Kawada A, Matsuo I, Hiruma M (2000) Solitary sporotrichosis lasting for 10 years. Dermatology 198: 100-101.
- Carvalho MTM, Castro AP, Baby C, Werner B, Neto JF, et al. (2002) Disseminated cutaneous sporotrichosis in a patient with AIDS: report of a case. Rev Soc Bras Med Trop 35: 655-659.
- Barros MBL, Schubach ADO, Galhardo MCG, Schubach TMP, dos Reis RS, et al. (2003) Sporotrichosis with widespread cutaneous lesions: report of 24 cases related to transmission by domestic cats in Rio de Janeiro, Brazil. Int J Dermatol 42: 677-681.
- Barros MBL, Schubach AO, Schubach TM, Wanke B (2008) An epidemic of sporotrichosis in Rio de Janeiro, Brazil: epidemiological aspects of a series of cases. Epidemiol Infect 136: 1192-1196.
- Schubach A, de Lima Barros MB, Schubach TM, Francesconi-do-Valle AC, Gutierrez-Galhardo MC, et al. (2005) Primary conjunctival sporotrichosis: two cases from a zoonotic epidemic in Rio de Janeiro, Brazil. Cornea 24: 491-493.
- Hardman S, Stephenson I, Jenkins DR, Wiselka MJ, Johnson EM (2005) Disseminated Sporothix schenckii in a patient with AIDS. J Infect 51: 73-77.
- Villela R, Souza GF, Cota GF, Mendoza L (2007) Cutaneous and meningeal sporotrichosis in a HIV patient. Rev Iberoam Micol 24: 161-163.
- Mauermann ML, Klein CJ, Orenstein R, Dyck PJB (2007) Disseminated sporotrichosis presenting with granulomatous inflammatory multiple mononeuropathies. MuscNerv 36:866-72.
- Gutierrez-Galhardo MC, Barros MB, Schubach AO, Cuzzi T, Schubach TMP, et al. (2005) Erythema multiforme associated with sporotrichosis. J Eur Acad Dermatol Venereol 19: 507-509.
Citation: San Juan Romero A, Arenas R (2021) Clinical Features of Sporotrichosis. J Clin Dermatol Ther 7: 084.
Copyright: © 2021 Ana San Juan Romero, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

