
Congenital Morphea: Two Case Reports
*Corresponding Author(s):
Guerra ABDepartment Of Pediatrics, Hospital Do Espírito Santo De Évora, Évora, Portugal
Tel:+351 967985208,
Email:a.bentoguerra@gmail.com
Abstract
Congenital morphea is a rare and underestimated form of localized scleroderma that presents at birth. From the five known subtypes, linear and plaque morphea are the most common and benign forms and are both described in these cases. Extracutaneous manifestations are rare. Prognosis is usually good. Long-term follow-up is important to prevent complications during growth. Spontaneous resolution may occur and mild forms have a great response to topical corticosteroids or calcineurin inhibitors.
Keywords
Congenital morphea; Localized scleroderma; Linear; Plaque
INTRODUCTION
Localized scleroderma, also called morphea, is a connective tissue disease, presenting with cutaneous sclerosis and usually a benign and self-limited evolution. There are five subtypes of morphea: Plaque, linear, generalized, pansclerotic, and mixed [1]. Linear morphea is the most frequent form of scleroderma in childhood and the face may be involved as well as the trunk and limbs. Plaque morphea is the most benign form with few discrete plaques confined to one to two anatomic areas [1]. Acquired morphea is the most frequent form of localized scleroderma and the congenital form has been reported rarely [1,2]. This article reports two infants with superficial cutaneous sclerotic lesions from birth, histologically compatible with congenital morphea.
CASE REPORT- 1
One-month-old female with an uneventful pregnancy, term delivery, and unremarkable family history. She presented with hypopigmented, indurated, and retracted skin plaques with linear distribution along the lateral side of the right thigh (Figure 1). These lesions were noted since birth. Skin biopsy was performed and showed mild thickening and hyalinization of collagen fibers and normal epidermis. Orcein and Verhoeff stains revealed preserved elastic fibers (Figure 2). Due to the absence of skin inflammation both macroscopic and microscopically, a conservative wait-and-see approach was adopted. After three months of follow-up, spontaneous near-total remission of described lesions was reported. At twelve-month-old follow-up dermatology consultation, localized marmorated hypopigmentation persisted without cutaneous thickening. No pharmacological therapy was introduced to date. The infant was discharged with required lower limbs symmetry and joint mobility regular evaluation. No extracutaneous manifestations were described to date.
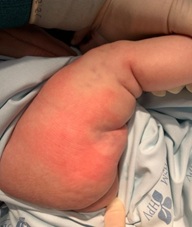 Figure 1: Hypopigmented, indurated and retracted skin plaques with linear distribution along the right thigh.
Figure 1: Hypopigmented, indurated and retracted skin plaques with linear distribution along the right thigh.
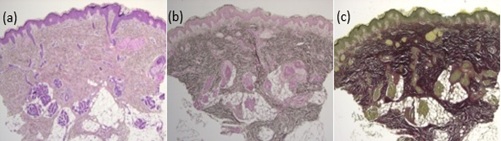 Figure 2: Hematoxylin and eosin (a) Orcein (b) Verhoeff stains (c) (25x). Mild thickening and hyalinization of collagen fibers with preserved elastic fibers.
Figure 2: Hematoxylin and eosin (a) Orcein (b) Verhoeff stains (c) (25x). Mild thickening and hyalinization of collagen fibers with preserved elastic fibers.
CASE REPORT - 2
A two-month-old male with an uneventful pregnancy and term delivery, previously healthy and without a family history of autoimmune diseases or connective tissue disorders, presented at birth with three grouped skin lesions on the gluteal region and right thigh. These were three rounded macules, measuring 15, 20 and 8 millimeters, with central ivory induration and violaceous halo (Figure 3). The remaining physical examination was normal. Histopathological findings on skin biopsy performed at 2,5 months of age established the diagnosis of morphea. Topical treatment with tacrolimus twice daily was initiated with good response (Figure 4). After three months of treatment, only the smaller lesion persisted on the thigh with some pallor and lilac peripheral hue (Figure 5).
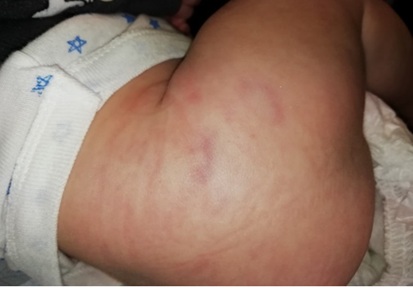 Figure 3: Threeoval circumscribed areas with central ivory color and violaceous halo.
Figure 3: Threeoval circumscribed areas with central ivory color and violaceous halo.
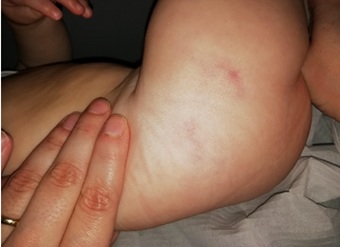 Figure 4: Improved skin lesions after treatment with tacrolimus.
Figure 4: Improved skin lesions after treatment with tacrolimus.
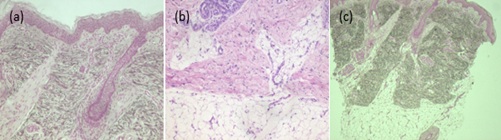 Figure 5: Hematoxylin and eosin 40x (a), 100x (b): Thickening and hyalinization of collagen fibers, with mild chronic infiltrate composed of lymphocytes and histiocytes. Orcein 40x (c): Preservation of elastic fibers.
Figure 5: Hematoxylin and eosin 40x (a), 100x (b): Thickening and hyalinization of collagen fibers, with mild chronic infiltrate composed of lymphocytes and histiocytes. Orcein 40x (c): Preservation of elastic fibers.
DISCUSSION
In literature, congenital morphea has been reported sparsely which leads to a lack of awareness of this condition and late diagnosis [3]. Morphea identification and classification may be difficult, particularly in small infants, because of its clinical spectrum and unknown progression [4]. About half of the patients present with an association of linear and plaque morphea [1]. Skin biopsy is very important to establish the diagnosis [2]. Extracutaneous manifestations are rarely associated with the described forms [1,4]. Nevertheless, lower limbs symmetry of length, creases, muscle, and joint mobility must be assessed in regular pediatric consultation, to diagnose and prevent orthopedic complications during the growth period [4,5]. Treatment is challenging and depends on location, severity, and disease activity. Spontaneous remission of sclerotic linear lesions was seen in case one. Topical treatment with calcineurin inhibitor (tacrolimus) twice daily was initiated on the second case with partial resolution of plaque lesions [2]. Despite the good prognosis of these mild forms of congenital morphea, prompt diagnosis is important to reduce long-term physical and psychological comorbidities [2].
DECLARATION OF INTEREST
The Authors declare that there is no conflict of interest.
REFERENCES
- Torok KS (2012) Pediatric scleroderma-Systemic and localized forms. Pediatr Clin North Am 59: 381-405.
- George R, George A, Kumar TS (2020) Update on management of morphea (Localized Scleroderma) in children. Indian DermatolOnline J 11: 135-145.
- Zulian F, C Vallongo, de Oliveira SKF, Punaro MG, Ros J, et al. (2006) Congenital localized scleroderma. J Pediatr 149: 248-251.
- Mansour M, Wong CL, Zulian F, Li S, Morishita K, et al, (2018) Natural history and extracutaneous involvement of congenital morphea: Multicenter retrospective cohort study and literature review. Pediatric Dermatology 35: 761-768.
- Najeeb N, Thomas J, Manoharan D (2015) Linear morphea in a child: A case report. Biomed Pharmacol J 8: 583-585.
Citation: Guerra AB, Almeida TL, Lara PE, Tapadinhas MC (2020) Congenital Morphea: Two Case Reports. J Neonatol Clin Pediatr 7: 062.
Copyright: © 2020 Guerra AB, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

