
Debulking of Keloid Combined with Intralesional Injection of Methotrexate and Triamcinolone versus Intralesional Injection of Methotrexate and Triamcinolone
*Corresponding Author(s):
Khalifa E SharquieDepartment Of Dermatology And Venereology, Scientific Council Of Dermatology & Venereology-Iraqi Board For Medical Specializations, College Of Medicine, University Of Baghdad, Baghdad, Iraq
Tel:+009647901468515,
Fax:+00964153721
Email:ksharquie@ymail.com
Abstract
Background: Keloid is a major health problem all over the world, where its management is a complex problem.
Objective: To find new mode of therapy for keloid by using intralesional injection of methotrexate and triamcinolon with or without debulking.
Patient and Methods: This single blinded comparative therapeutic outpatient based study was done at the Department of Dermatology, Baghdad Teaching Hospital during the period from February 2011 to February 2013. A total of 27 patients with 61 lesions were enrolled in this work and consisted of 2groups; Group A (30 lesions): Treated by intralesional injection of combination of methotrexate and triamcinolone acetonide and repeated every month. Group B (31 lesions) Debulking was carried out first and then injection of combination of methotrexate and triamcinolone acetonide at time of operation similar to Group A.
Evaluation was performed by scoring system with 5 criteria (redness, elevation, hardness, itching and tenderness). The response was graded as no response, minimal, moderate or complete response.
Results: Results were evaluated on the basis of overall response, recurrence and prolonged side-effects after the completion of treatment. The mean of score before treatment was (9.63) and after the end of therapy was (4.40) (P< 0.0001) for Group A. The mean of score before treatment was (9.06) and after treatment was (2.32) (P< 0.0001) for Group B. When the two groups compared with each other it was found the debulking group was statistically significant than the intralesional group (p value=0.001).Itching in both groups was stopped after the first injection in the majority of patients.
All lesions in both groups showed response to both types of treatments, while the moderate response was seen in 85.5% in Group B and 50% in Group A.
The relapse was very low in both groups (10%) but there was no statistical significant difference in the recurrence rate in both treatment modalities (p value=0.65).
In patient who had debulking, the size of relapsed keloid was either similar to that before debulking or could be smaller and the side effects in both groups were low and comparable. Also, no local or systemic adverse effects were noticed.
Conclusion: The new two modes of therapy were shown to be highly statistically significantly effective in treatment of keloid but the group with debulking was statistically much better. The side effects and the recurrence rate were minimal but comparable.
Keywords
INTRODUCTION
Keloid represents a benign growth of fibrous tissue originating from an abnormal healing response to cutaneous injury. It is one of the commonest skin lesions encountered in clinical practice. Estimated incidences vary from 0.09% to 16% in some random sampling of some African populations [1]. Infants under 1 year and adults over 70 years old have also been affected. Apart from the distinct increased tendency for keloids among black populations, they also appear to have a genetically more aggressive variety. There is a strong familiar tendency and slight female preponderance among patients who present for treatment [1].
Clinically keloids extend beyond the margins of the original injury, while hypertrophic scars always remain within the confines of the original injury and show regression with time unlike a keloid. Both show predominantly extracellular matrix with predominantly types 1 and 3collagen, though type 1 collagen predominates in keloids [2].
Their clinical significance of keloid and hypertrophic scars lies in the distressing aesthetic problem when they occur over the exposed part of the body in addition to irritating pruritus and tendency to suppurate [3].
The etiology of keloid is still largely unknown. In many cases however, trauma is the most frequently associated event. The observation that cutaneous lesions on the palms and soles of the feet in keloid patients do not form keloidal lesions led to "sebum autoimmune hypothesis" which proposes that intradermally secreted sebum triggers an autoimmune granulomatous response [4]. The association with hormones has also been found with increased susceptibility in acromegalics, increased growth during pregnancy, puberty and hyperthyroidism [5]. Over the years, treating keloids scars has proved to be challenging [2]. Numerous advances have been made in understanding the process of formation of wound healing and scar formation. This increased knowledge has led to the introduction of new treatments as well as to a better understanding of how older treatments work [2]. The limited success of one technique has given rise to numerous treatment protocols. However, most of these treatment protocols are plagued with spectra of recurrence [2,6] These include surgical excision, intralesional steroid injection, cryotherapy, laser therapy, use of ionizing radiation, mechanical compression dressing, silicone sheet applications, ultrasound and heat therapy, intralesional interferon injection, or combination of techniques, and many others (Table 1) [6-11].
| Modality or treatment option | Response rate (%) | Recurrence rate (%) | Comments | Study design |
| Preventive silicone sheeting as post surgery care | 0 - 75 | 25 - 36 | Multiple preparations available; tolerated by children | Review of multiple case studies [7] |
| Postsurgical intralesional corticosteroid injection | 0 -100 | 0 -100 (mean 50) | Patient acceptance and safety | Review of multiple case studies [8] |
| Postsurgical topical imiquimod 5% cream | 80 | 28 | May cause hyperpigmentation, irritation | Case study [9] |
| Cryotherapy | 50 -76 | 23 | Useful on small lesions; easy to perform | Review of multiple case studies [8] |
| Intralesional corticosteroid injection (triamcinolone acetonide 10 -40 mg per ml at 6 week intervals) | 50 - 100 | 9 - 50 | Inexpensive; available | Review of multiple case studies [8] |
| Surgical excision | variable | 50 - 100 | Review of multiple case studies [8] | |
| "Triple keloid therapy" (surgery, corticosteroids, and silicone sheeting) | 88 at 13 months | 12.5 at 13 months | Time intensive; expensive | Case study [9] |
| Postsurgical interferon alfa-2b 1.5 million IU intralesional injection twice daily for 4 days | 30 -50 | 8 -19 | Expensive | Review of multiple case studies [8] |
| Pulsed dye laser | 30 -40 | 30 | Expensive; variable results depending on trial (controversial) | Case studies [10,11] |
Table 1: Showing the different modalities of therapy [6-11].
Surgical excision of keloids is a common management option. Excision of keloids is not only invasive but also marked by a high recurrence rate [12-15]. Recurrence rate of 50% to 100% have been reported [12-14]. Small keloids can be excised and closed primarily, whereas larger keloids may require skin grafting. Other different techniques of closure after surgical excision like Z-plasty and healing by secondary intention have also been reported [16,17]. Excision of keloids followed by skin grafting alone resulted in 59% recurrence rate [14]. Skin grafting is also complicated by the potential of keloids development at the donor site [2]. There is no generally accepted surgical protocol for keloids excision. Both extralesional [18,19] and intralesional excisions [6,20] have been reported. Advocates of intralesional excision believe that leaving a thin rim of keloid on the wound edges avoids the risk of inducing an intense inflammatory response in the surrounding, unaffected "keloid-prone" skin, which could lead to the formation of new and possibly bigger Keloid [6]. Regardless of the surgical technique, there is further injury to the dermis that leads to proliferation of fibroblasts and extreme amounts of collagen formation, and thus, keloid scar formation [21].
Therefore, during surgical excision, it is essential that tissue trauma be minimal. Many factors may enhance the possibility of recurrences. Such factors include dead space, foreign material, hematoma, infection and wound tension [22].
Due to high recurrence following surgical excision alone, combination therapies with intralesional steroid, cryotherapy, pressure therapy, radiotherapy, laser therapy, silicone sheet application have been advocated [22-24].
Methotrexate (MTX) is used for the treatment of cancer, psoriasis, and rheumatoid arthritis, and works by inhibiting dihydrofolate reeducates, which prevents the reduction of dihydrofolate to its active form, [25] but MTX has not been tried as intralesional treatment for keliod. Researchers are always looking for new therapy that could be more satisfactory than old treatment. By present work, we are trying new modes of treatment by the debulking of keloid without suturing combined by intralesional injection of methotrexate and triamcinolone to be compared with intralesional injection of methotrexate and triamcinolone alone.
PATIENTS AND METHODS
A total of 27 patients with 61 lesions satisfied the selection criteria and they were 21 (34.4 %) lesions found in males and 40 (65.6%) lesions found in females were enrolled in the study. This study consisted of two groups,
Group A: (n=30 lesions) Methotrexate 1ml(10mg with up to a maximum of 2ml being used per dose)and 0.5ml triamcinolone acetonide(20mg) and 1 ml 2% xylocain as combination to infiltrate the keloid without removal.
Group B: (n=31 lesions) Debulking was carried out first and then injection of methotrexate and triamcinolone acetonide and 2% xylocain in dose similar to Group A.
Patients with single lesion were treated by either Group A or Group B, while patients with multiple keloidal lesions were treated by more than one group in the same patient. Then the score of two groups were compared with each other to demonstrate any difference between them.
The nature and target of this study were explained for each patient and formal consent was taken for each patient before starting the therapy, after full explanation about the nature of the disease, course, the procedure of treatment, follow up, prognosis and the need for pre and post treatment photographs by Sony-Digital, high sensitivity, 16.1megapixels, 5 x optical zoom camera in the same place with fixed illumination and distance. Also, ethical approval was given by the scientific committee of the Scientific Council of Dermatology and Venereology-Arab Board for Medical Specializations.
Inclusion criteria included: extension of the growth beyond the boundaries of the original lesion or injury, at least 1 year duration keloid, the last modality of treatment used at least 6 months ago with either no response or recurrence.
Exclusion criteria included: pregnant women or if want to be pregnant, lactating women, hepatic dysfunction, renal dysfunction, active infectious disease and blood dyscrasia.
Complete Blood Cells (CBC) count, liver function, renal function and blood sugar were performed prior to initiation of therapy. CBC was repeated every week for the first 2 weeks and then once every 4 weeks, while blood chemistry was repeated once every 4 weeks during treatment.
Technique of injection
Follow up: Patients were seen first after two weeks with no injection and then monthly injections were carried with maximum of 6 sessions. The scoring for the response was carried out. Also, followed up was done for 5 months after stopping the injection to watch any recurrence of keloid.
Evaluation of the lesion: The lesions were evaluated according to the score system employing in 5 criteria (Table 2).
The evaluation of response was graded as follows:
- No response.
- Minimal response:
- Change of one score in no more than 3 criteria.
- Change of one score in no more than 2 criteria provided that one or more criterion was ranking 0 score before embarking upon our treatment.
- Moderate response: improvement more than minimal and less than complete.
- Complete: change of the score into 0 in all criteria.
| Criteria | Score |
| A. Redness | 3: Severe redness associated with telangiectasia. 2: Redness disappears with pressure. 1: No redness but a dark appearance. 0: Normal skin color. |
| B. Elevation | 3: More than 8 mm in height above the surrounded skin. 2: 4-8 mm. 1: 1-4 mm. 0: Flat or depressed scar. |
| C. Hardness | 3: Very hard, like a cartilage. 2: Rubbery hard. 1: Partially soft. 0: Soft. |
| D. Itching | 3: Severe itching sensation, or constantly itchy with signs of scratching. 2: Occasional itchy sensation, moderate and tolerable. 1: Sometimes itchy. 0: No itchy sensation. |
| E. Tenderness and pain | 3: Severe irritable pain. 2: Moderately irritable pain. 1: Sometimes painful. 0: Without pain. |
Table 2: The scoring criteria [24].
RESULTS
The groups were analyzed for different parameters like overall response, recurrence and prolonged side-effects after the completion of treatment, and a comparison between the groups was done.
The mean of score before treatment was (9.63) and after the end of therapy was (4.40) (P< 0.0001) for Group A (Figure 1). The mean of score before treatment was (9.06) and after treatment was (2.32) (P< 0.0001) for Group B (Figure 2). When the two groups compared with each other it was found the debulking group was statistically significant than the intralesional group (p value=0.001).
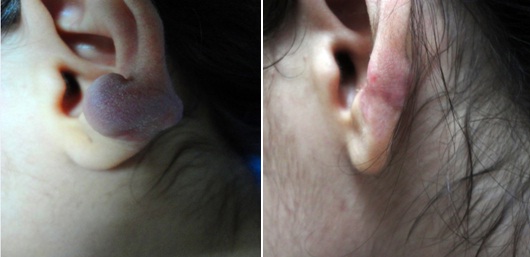
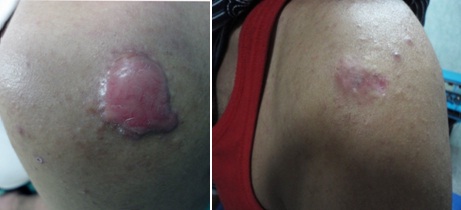
Itching in both groups was stopped after the first injection in the majority of patients (Table 3).
| Treatment category | Score criteria before treatment mean±SD | Score criteria after treatment mean±SD | Paired t-test | P-value |
| GroupA(intralesional) | 2.14±0.803 | 0.93±0.766 | 7.718 | < 0.001 |
| GroupB (intralesional with debulking) | 2.32±0.670 | 1.54±0.693 | 8.337 | < 0.001 |
Table 3: Showing improvement in itching of keloid in both groups.
The evaluation of the response was recorded in Table 4. All lesions in both groups showed response to both types of treatments, while the moderate response was seen in 85.5% in Group B and 50% in Group A.
| Response to treatment | Type of treatment | |||
| Group A (intralesional) | Group B (intralesional with debulking) | |||
| N | % | N | % | |
| No response | 0 | 0.0% | 0 | 0.0% |
| Minimal response | 15 | 50.0% | 6 | 19.5% |
| Moderate response | 15 | 50.0% | 25 | 80.5% |
| Total | 30 | 100.0% | 31 | 100.0% |
There was no statistical significant difference in the recurrence rate in both treatment modalities (p value=0.65) (Table 5).
| Recurrence after treatment | Type of treatment | |||
| Group A (intralesional) | Group B (intralesional with debulking) | |||
| N | % | N | % | |
| No | 27 | 90.0% | 28 | 90.3% |
| Yes | 3 | 10.0% | 3 | 9.7% |
| Total | 30 | 100.0% | 31 | 100.0% |
In patient who had debulking, the size of relapsed keloid was either similar to that before debulking or could be smaller. Regarding the side effects in both groups were shown in Table 6, there were no statistical significant differences. Also, no systemic adverse effects like anemia, leucopenia, and thrombocytopenia were noticed.
| The side effects | Type of treatment | |||
| Group A (intralesional) | Group B (intralesional with debulking) | P value | ||
| Hyperpigmentation | N | 2 | 2 | 0.68 |
| % | 6.7% | 6.5% | ||
| Atrophy | N | 2 | 1 | 0.49 |
| % | 6.7% | 3.2% | ||
| Ulceration | N | 1 | 1 | 0.75 |
| % | 3.3% | 3.2% | ||
Table 6: Showing the side effects of both groups.
DISCUSSION
Treatment of keloid is still a major problem and great challenge for the dermatologist and plastic surgeon as all medical and surgical therapies are still unsatisfactory, and often fail in clearing keloid lesion [2].
The limited success of one technique has given rise to numerous treatment protocols. However, most of these treatment protocols are plagued with a high of recurrence [2,6-11].
Since the mid-1960s intralesional steroid injections have gained popularity as one of the most common approaches to attenuate hypertrophic scar and keloid formation. Most of the known effects of corticosteroids are thought to result primarily from its suppressive effects on the inflammatory process in the wound, [26] and secondarily from diminished collagen and glycosaminoglycan synthesis, inhibition of fibroblast growth [27] and enhanced collagen and fibroblast degeneration [28].
Methotrexate (MTX) is used for the treatment of cancer, psoriasis, and rheumatoid arthritis, and works by inhibiting dihydrofolate reeducates, which prevents the reduction of dihydrofolate to its active form, [29] and the present work is the first study that showed MTX could be used as effective intralesional treatment of keliod in such extensive research work.
The addition of MTX to TAC is expected to induce better results than any of these drugs alone because keloid results from uncontrolled overgrowth of dense fibrous scar tissue resulting from the presence of increased number and activity of fibroblasts. So, that as MTX and TAC are a well-known anti-proliferative and anti-inflammatory medications and they exert their effects when injected intralesionally by inhibiting fibroblast proliferation and activity thus reducing the volume of keloid tissue.
In addition, this combination therapy relieves itching that is mediated by the increased amount of histamine secreted by mast cells in keloid tissue [20,25-27].
The present work had proved that debulking of keloid combined by intralesional injection of MTX+TAC is a new effective mode of therapy of keloid and was much better than intralesional injection of MTX+TAC alone.
Regarding the recurrence rate in both groups where almost comparable, this was estimated around 10.0%. In keloid surgery especially when the lesion excised and sutured, the relapsed keloid usually bigger in size than before surgery, [30] while in present study, the relapsed lesions were either the same size or could be smaller than before surgery.
The side effects in both groups were comparable like hyperpigmentation, atrophy and ulceration, without difference in the side effects in both grupos. No systemic side effects were reported in both groups over 6 months follows up period and as confirmed by laboratory test.
In conclusion, the present work demonstrated new, effective modalities of therapy by using intralesional injection of methotrexate and triamcinolone with or without debulking. Although when combined with debulking the results was much more superior, but with very low recurrence rates and local and systemic side effects. These modes of therapy are much more effective and safe than previously surgical and topical therapies.
REFERENCES
- Thompson LD (2004) Skin keloid. Ear Nose Throat J 83: 519.
- Gauglitz GG, Kunte C (2011) [Recommendations for the prevention and therapy of hypertrophic scars and keloids]. Hautarzt 62: 337-346.
- Onwukwe MF (1978) The suppurative keloid. J Dermatol Surg Oncol 4: 333-335.
- Verhaegen PD, van Zuijlen PP, Pennings NM, van Marle J, Niessen FB, et al. (2009) Differences in collagen architecture between keloid, hypertrophic scar, normotrophic scar, and normal skin: An objective histopathological analysis. Wound Repair Regen 17: 649-656.
- Kim HD, Hwang SM, Lim KR, Jung YH, Ahn SM, et al. (2013) Recurrent Auricular Keloids during Pregnancy. Arch Plast Surg 40: 70-72.
- Donkor P (2007) Head and neck keloid: treatment by core excision and delayed intralesional injection of steroid. J Oral Maxillofac Surg 65: 1292-1296.
- Berman B, Perez OA, Konda S, Kohut BE, Viera MH, et al. (2007) A review of the biologic effects, clinical efficacy, and safety of silicone elastomer sheeting for hypertrophic and keloid scar treatment and management. Dermatol Surg 33: 1291-1302.
- Niessen FB, Spauwen PH, Schalkwijk J, Kon M (1999) On the nature of hypertrophic scars and keloids: a review. Plast Reconstr Surg 104: 1435-1458.
- Chuangsuwanich A1, Gunjittisomram S (2007) The efficacy of 5% imiquimod cream in the prevention of recurrence of excised keloids. J Med Assoc Thai 90: 1363-1367.
- Agbenorku P (2000) Triple keloid therapy: a combination of steroids, surgery and silicone gel strip/sheet for keloid treatment. Eur J Plast Surg 23: 150-151.
- Alster TS (1994) Improvement of erythematous and hypertrophic scars by the 585-nm flashlamp-pumped pulsed dye laser. Ann Plast Surg 32: 186-190.
- Wolfram D, Tzankov A, Pulzl P, Piza-Katzer H (2009) Hypertrophic scars and keloids-a review of their pathophysiology, risk factors, and therapeutic management. Dermatol Surg 35: 171-181.
- Hackert I, Aschoff R, Sebastian G (2003) [The treatment of keloids]. Hautarzt 54: 1003-1015.
- Mofikoya BO, Adeyemo WL, Abdus-salam AA (2007) Keloid and hypertrophic scars: a review of recent developments in pathogenesis and management. Nig Q J Hosp Med 17: 134-139.
- Ziccardi VB, Lamphier J (2000) Use of keloid skin as an autograft for earlobe reconstruction after excision. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 89: 674-675.
- Guix B, Henriquez I, Andres A, Finestres F, Tello JI, et al. (2001) Treatment of keloids by high-dose-rate brachytherapy: A seven-year study. Int J Radiat Oncol Biol Phys 50: 167-172.
- Maarouf M, Schleicher U, Schmachtenberg A, Ammon J (2002) Radiotherapy in the management of keloids. Clinical experience with electron beam irradiation and comparison with X-ray therapy. Strahlenther Onkol 178: 330-335.
- Ogawa R, Mitsuhashi K, Hyakusoku H, Miyashita T (2003) Postoperative electron-beam irradiation therapy for keloids and hypertrophic scars: Retrospective study of 147 cases followed for more than 18 months. Plast Reconstr Surg 111: 547-553.
- Pai VB, Cummings I (2011) Are there any good treatments for keloid scarring after sternotomy? Interact Cardiovasc Thorac Surg 13: 415-418.
- Baisch A, Riedel F (2006) [Hyperplastic scars and keloids: part II: Surgical and non-surgical treatment modalities]. HNO 54: 981-992.
- Sanders KW, Gage-White L, Stucker FJ (2005) Topical mitomycin C in the prevention of keloid scar recurrence. Arch Facial Plast Surg 7: 172-175.
- Baisch A, Riedel F (2006) [Hyperplastic scars and keloids. Part I: basics and prevention]. HNO 54: 893-904.
- Jalali M, Bayat A (2007) Current use of steroids in management of abnormal raised skin scars. Surgeon 5: 175-180.
- Mustoe TA, Cooter RD, Gold MH, Hobbs FD, Ramelet AA, et al. (2002) International clinical recommendations on scar management. Plast Reconstr Surg 110: 560-571.
- Tolerton SK, Tonkin MA (2011) Keloid formation after syndactyly release in patients with associated macrodactyly: management with methotrexate therapy. J Hand Surg Eur Vol 36: 490-497.
- Muzaffar AR, Rafols F, Masson J, Ezaki M, Carter PR (2004) Keloid formation after syndactyly reconstruction: associated conditions, prevalence, and preliminary report of a treatment method. J Hand Surg Am 29: 201-208.
- Reish RG, Eriksson E (2008) Scar treatments: preclinical and clinical studies. J Am Coll Surg 206: 719-730.
- Cruz NI, Korchin L (1994) Inhibition of human keloid fibroblast growth by isotretinoin and triamcinolone acetonide in vitro. Ann Plast Surg 33: 401-405.
- Boyadjiev C, Popchristova E, Mazgalova J (1995) Histomorphologic changes in keloids treated with Kenacort. J Trauma 38: 299-302.
- Robles DT, Berg D. Abnormal wound healing: keloids. Clin Dermatol. 2007; 25:26–32.
Citation: Sharquie KE, Noaimi AA, Al-karhi MR (2014) Debulking of Keloid Combined with Intralesional Injection of Methotrexate and Triamcinolone versusIntralesional Injection of Methotrexate and Triamcinolone. J Clin Dermatol Ther 1: 003.
Copyright: © 2014 Khalifa E Sharquie, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

