
Diagnosis and Management of Acute Limb Ischemia
*Corresponding Author(s):
Hafedh DalyDepartment Cardiovascular Surgery, Gafsa Regional Hospital, Tunisia
Tel:+216 98100809,
Email:daly.hafedh@yahoo.fr
Abstract
Introduction: Acute limb ischemia is considered as a life threatening disease .After twelve hours of ischemia, chances of saving the ischemic limb are lower (78%), with higher mortality (31%) as well.
Methods: A total of 54 patients who underwent surgery for acute non traumatic limb ischemia between January 2013 and December 2020 were retrospectively reviewed.
Results: We included 30 women and 24 men; median age was 69 years. Twenty patients (37%) were presented with upper limb ischemia, where as 34 patients (63%) with lower limb ischemia. Mean delay between the onset of symptoms and hospital admission of upper limb ischemia was 22 hours, 35% of Patients were diagnosed at the stage IIA of Rutherford classification, while 65% were diagnosed at the stage of II B. Lower limb ischemia patients were admitted after 28.5 hours, 64.8% of patients were diagnosed at the stage of II A of Rutherford, while 32.3% were diagnosed at the stage of II B of Rutherford. Revascularization of all ischemic upper limbs (100%) and the majority of ischemic lower limbs (94.1%) were carried out through endovascular thromboembolectomy with Fogarty ballooncathete. Meanlength of hospitalstaywas 8.3 days for upper limb ischemia cases ; while lower limb ischemia patients required 9.2 days of mean hospitalstay. We report a total of 4 deaths (7.4%).
Conclusion: Acute limb ischemia remains a challenging entity for clinicians with significant risk of patient limbloss and mortality. Prompt diagnosis, anticoagulation, and timely revascularization are crucial to minimize the risk of limbloss.
Keywords
Acute ischemia; Embolism; Limb; Surgery; Thrombosis
Introduction
Acute arterial ischemia of the limbis an acute circulatory insufficiency caused by the sudden and complete obliteration of the main arterial vascularization of the limb [1]. A serious pathology, it can compromise the vitality and the function of the affected limb [2]. The time of ischemia is an important prognostic factor.
When adequate care is instituted less than 12 hours after the onset of symptoms, the mortality rate is 19% andthelimb salvage reaches 93%. On the other hand, beyond 12 hours, mortality rises to 31% and the limb salvage rate drops to 78% [3]. The advent of the FOGARTY catheter in 1963 revolutionized the surgical management of this condition [4].
The main objective of this study is to evaluate the epidemiological and clinical profile of acute ischemia of the limbs and to analyze the results of the surgery in the Cardiovascular Surgery Department of the regional hospital of Gafsa.
Patients and Methods
This is a retrospective study about 54 patients operated on for acute ischemia of the limbs during the period between January 1, 2013 and December 31, 2020 in the Cardiovascular Surgery department of the Gafsa hospital. To limit ourselves to the study of non-traumatic acute ischemia of the limbs, we included patients presenting with acute ischemia of the limbs (< 15 days) whose age is greater than 15 years at the time of the intervention and acute ischemia stage I, IIA or IIB of Rutherford.
We excluded from this study patients suffering from acute limb ischemia following multi-organ failure in intensive care and treated with high doses of vasopressor drugs, acute limb ischemia secondary to bypass thrombosis, acute post-traumatic ischemia and phlegmatia coerulea dolens.
The data studied were collected from hospitalization records, operating reports, anesthesia and resuscitation records, outpatient records and records from the original departments. They were entered using Excel software and analyzed using SPSS version 23 software. We calculated simple and relative frequencies (percentages) for the qualitative variables. Means and extreme values for quantitative variables were determined.
Results
During the study period, 54 patients were diagnosed with acute non-traumatic limb ischemia. That of the lower limbs was observed in 34 cases (63%) and that of the upper limbs in 20 cases (37%). The average age of the patients was 69 years old with extremes of 33 and 95 years old and a sex ratio of 0.8.
Acute Ischemia Of The Lower Limbs
The average age of the patients was 65.9 years with extremes of 37 and 94 years, with a slight male predominance (19 men and 15 women). Comorbidities were present in 31 patients (91.2%). The most common risk factor was high blood pressure, which accounted for 58.8% (n=20).
The patients were smokers (38.2%, n=13), diabetics (29.4%, n=10) and carriers of heart disease (41.17%, n=14). The average treatment time was 28.5 hours with extremes of 4 hours and 5 days. Only 6 patients were admitted before 6 hours (17.6%) (Table 1).
|
Treatment Time |
Number of Patients |
Percentage (%) |
|
≤ 6 h |
6 |
17.6 |
|
Bettween 6 et 24 h |
19 |
55.9 |
|
Bettween 24 et 48 h |
2 |
5.9 |
|
>48 h |
7 |
20.6 |
Table 1: Admission time for acute lower limb ischemia.
The reason for consultation was coldness of the limb in 100% of cases, pain in 97% of cases, pallor in 58.8% of patients, cyanosis in 38.2% of cases and paralysis in 32.3% of cases.
According to the Rutherford classification, 64.8% of patients were diagnosed at stage IIA and 32.3% of patients at stage IIB. Only one patient is at the sub-clinical stage.
Involvement of the left lower limb was dominant with 55.9% (n = 19) and bilateral in 5.9% of cases (n = 2). All the pulses were absent in 9 cases. The popliteal pulse was abolished in 24 cases and the the distal onalone (tibialis posterior and pedis) in 1 case (Table 2).
|
Pulse Examination |
Number of Patients |
Percentage (%) |
|
Abolition of all pulses in one lower limb |
9 |
26.5 |
|
Abolition of the popliteal and distal pulses of a lower limb |
24 |
70.5 |
|
Abolition of distal pulses only of a lowerlimb |
1 |
3 |
Table 2: Distribution of patients according to lower limb pulse examination.
The Doppler ultrasound was performed in 23 cases (67.6%) and the CT angiography of the aorta and lower limbs in 9 cases (26.4%).
The level of occlusion was: the superficial femoral artery in 19 cases (55.9%), external iliac or ilio-femoral junction in 4 cases (11.7%), commoniliac in 3 cases (8.8%), bilateral commoniliac in 2 cases (5.9%), popliteal artery in 4 cases (11.7%), leg arteries in one case and occlusion of the terminal abdominal aorta in one patient. The curative dose heparin therapy was started in the emergency room and continued per and postoperatively at a dose of 3 mg/kg/24 h in all patients.
The Fogarty catheter embolectomy was successfully performed in 32 patients (94.1%), in 31 cases via the femoral route and one case via the popliteal sub-articular route.
The crossed femoro-femoral bypass and crossed ilio-femoral bypass (Figure 1) were performed in one case each after failure of Fogarty catheter embolectomy. The decompressive aponeurotomy was performed in addition to emb olectomy in 11 patients (32.2%). 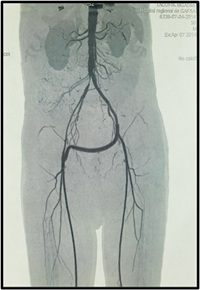 Figure 1: Cross ilio-femoral bypass.
Figure 1: Cross ilio-femoral bypass.
Minor amputation was performed in 4 cases (11.7%) including two of the big toe and two Trans-metatarsal.
No major amputations were performed.
The average length of stay was 9.2 days with extremes ranging from 2 to 28 days. There were 3 deaths (8.82%); a 34-year-old patient, carrier of healthy coronary dilated cardio myopathy, with an ejection fraction of 20%, the others were multitared, with postoperative revascularization syndrome. The latter was observed in 5 patients (14.7%). He associated renal failure with hyperkalemia. Three patients evolved well after medical treatment.
All our patients benefited from a cardiac assessment, using an electrocardiogram and a cardiac Doppler ultrasound which showed: a complete Arrhythmia by Atrial Fibrillation (ACFA) in 15 patients, a collapsed ejection fraction (<40%) in 2 patients, tight mitral stenos is in one patient and left intraventricular thrombus in one patient.
In our study the thrombotic etiology was observed in 55.9% (n=19) of the cases and the embolic etiology in 44.1% (n=15).
Acute ischemia of the upper limbs
Twenty patients were operated on for acute ischemia of the upper limb. The average age of our population was 74.3 years with extremes of 33 and 95 years. The sex ratio was 0.3.
The patients were in complete arrhythmia by atrial fibrillation in 85% (n=17) of the cases, hypertensive (35%, n=7), smokers (10%, n=2) and diabetics (10%, n=2).
The average support time was 21.9 hours with extremes of 2 and 72 hours. Only 8 patients, or 40%, were admitted before 6 hours (Table 3).
|
Treatment time |
Number of Patients |
Percentage (%) |
|
≤ 6 h |
8 |
40 |
|
Between 6 and 24 h |
6 |
30 |
|
Between 24 and 48 h |
4 |
20 |
|
>48 h |
2 |
10 |
Table 3: Admission time for acute upper limb ischemia.
The reason for consultation was coldness and pain in the limb in 100% of cases (n=20), pallor in 60% (n=12) of patients, cyanosis in 40% (n=8) of cases and paralysis in 65% (n=13) of cases.
According to the Rutherford classification, 35% (n=7) of patients were diagnosed at stage IIA and 65% (n=13) of patients at stage IIB.
Involvement of the left upper limb was dominant with 60% (n=12).
All pulses were absent in 14 cases (70%), the axillary pulse was present in 6 cases (30%).
The Doppler ultrasound was performed in 16 cases (80%) and the CT angiography of the upper limbs in 1 case (5%) (Figure 2).
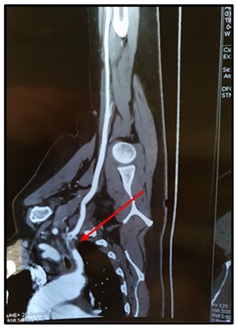 Figure 2: CT angiography showing thrombosis of the left subclavian artery
Figure 2: CT angiography showing thrombosis of the left subclavian artery
The level of occlusion was: the subclavian artery in 6 cases (30%), axillary or axillo-humeral junction in 8 cases (40%) and humeral with extension towards the radial or ulnar artery in 6 cases (30%)).
The Fogarty catheter embolectomy was performed successfully in all patients. No aponeurotomy or amputation were performed.
The etiological diagnosis was made preoperatively in 85% (n=17) of cases. It was a previously known complete Atrial Fibrillation Arrhythmia (ACFA) heart rhythm disorder. In 15% (n=3) of the remaining cases, the etiological diagnosis was made postoperatively and was made according to clinical and paraclinical arguments. The electrocardiogram was done in all patients. It showed ACFA in 17 patients and was normal in 3 patients. A rhythmic holter was performed in 1 patient and returned to normal. Cardiac ultrasound, performed in all patients, revealed the presence of aortic valve disease in one patient.
Two patients had ischaemia of paraneoplastico rigin, 1 of which was related to pulmonary neoplasia and 1 to ovarian neoplasia.
At the end of this clinical and paraclinical etiological assessment, the etiological diagnosis retained was of embolicorigin in 18 cases (90%), thrombotic in 2 cases (10%).
Discussion
Acute ischemia of the lower limbs
The epidemiological data of our series are consistent with those of the literature [5-8]. The cardiovascular risk factors were different from those observed by Duval, et al. [7]. Indeed our population seems to be more frequently smokers (38.2% versus 21.4%), less frequently diabetic (29.4.2% versus 37.8%). We often found atrial fibrillation (41.2% versus 23%). The majority of patients with acute ischemia of the lower limbs belonged to class IIA at the time of diagnosis [9-11].
According to our study, the average treatment time was 28.5 hours, 25 patients (73.5%) were admitted within the first 24 hours following the appearance of the first symptom, the 9 others were only seen beyond this established deadline.
In the literature, the admission time of the patient with an ischemic limbis often short and lower than that of our study, it varies from 11.35 hours to 23 hours [10,12,13]. This is explained by the rural origin and the low socio economic level of the patients who lived far from our hospital structure.
In our regional hospital, we do not have a technical platform for endovascular procedures, hence all our patients have been treated by conventional surgery; Fogarty catheter embolectomy in 94.1% (n=32) and vascular bypass in 5.9% (n=2) of cases.
According to an Italian study, over a period of 7 years, 322 patients with ischemia were admitted and 112 of them received Fogarty tube embolectomyonly, and the estimated freedom from reoperation at 1 year was 82, 1%. The efficacy of embolectomy has been demonstrated [14].
Baril DT, et al. [15], in an observational study analyzing 99,982 hospitalizations for acute ischemia of the limbs between 1998 and 2009 (average age of 80.6 years) described the incidences of acute ischemia of the limbs but also the mortality rates at in-hospital and one-year amputation rates, as well as per-hospital and one-year amputation rates. Mortality rates decreased from 12.0% to 9.0% significantly (p<0.001), while one-year mortality rates stabilized at 41.0% and 42.5% (p not significant ). In-hospital amputation rates remained stable at 8.1% and 6.4% (p not significant), while 1-year amputation rates decreased from 14.8% to 11.0% in a significative way. Amputation-free hospitalization-free survival after hospitalization for acute limb ischemia increased significantly from 81.2% to 85.4% (p <0.001). However, the one-year amputation-free survival remained unchanged. The risk of early amputation was increased in men, as well as by age, the presence of diabetes, a history of arteriopathy and in black subjects. Factors associated with early mortality are age, the presence of renal failure, dementia, cancer and atrial fibrillation.
The local and general prognosis of acute lower limb ischemia in ourstudy seems to be less unfavorable than in other observational studies [15,16].
The etiologies of acute ischemia are dominated by embolism and thromboses.
Arterial embolism comes in 85% of cases from the migration of clots from the heart [17-20]. Atrial fibrillation causes blood stasis in the atrium, where an atrial thrombus forms. It is the most common form (70%) of arterial embolism. An intraventricular parietal thrombus, typically in the region of the apex, can form in contact with a transmural myocardial infarction, most often in the first months following the infarction. About 11% of myocardial infarctions are complicated by an intra cardiac mural thrombus. Ten percent of cardiac emboli come from a post-infarction intraventicular thrombus [17,18].
Acute thrombosis in the presence of pre-existing arteriopathy is the second cause of limb ischemia [21]. It is estimated that 55% of acute limb ischemia is of embolic origin and 45% of thrombotic origin [22].
This frequency ratio tends to be reversed, with an increasing prevalence of acute thrombosis due to the aging of the population and better medical or surgical management of emboligenic heart disease [17,18,23].
In our work, the thrombotic etiology was more frequent than the embolic etiology (55.9% against 44.1%).
Acute ischemia of the upperlimbs
Acute ischemia of the upper limb is a rare condition, this is confirmed by all the series published until now; the incidence of acute ischemia of the arm, for example, was five times less than that of acute ischemia of the leg according to an Anglo-Saxon study [24].
In our study, the average treatment time was 21.9 hours, only 8 patients (40%) were admitted before 6 hours.
Abbott, et al. [25] reported that patients treated within 12 hours had a lower mortality rate and a higher limb salvage rate.
Miju Bae, et al. have shown that the delay in treatment has no influence on mortality but rather on neurological sequelae [26].
The treatment of choice for acute ischemia of the upper limbs is embolectomy using a Fogarty catheter. The approach to the humeral artery at the level of the bend of the elbow is the gold standard [27].
Revascularization by upper limb bypass is used less than the other techniques, representing about 4% of revascularization procedures [28].
Although this procedure is rarely used, the results of upper limb bypass surgery are excellent, even superior to those reported for the treatment of acute ischemia of the lower limbs [29].
Despite the progress made, published series show high overall mortality. Mortality after upper limb ischemia was 5.6% versus 12.8% after lower limb ischemia [30]. This high mortality is essentially explained, because of the general complications that these ischemias cause, the increasingly high age of patients in Europe and the United States.
Morbidity and mortality are far from negligible. They are often related to heart disease or associated cerebral events [31].
A Danish cohort estimated a low risk of amputation (1.5%, n=2) but high hospital mortality (9%, n=13) [32]. In this retrospective analysis, the amputation rate mainly predominated in per hospitalization; this rate was negligible at one year; the general long-term prognosis is favorable.
In our study the mortality was 5% (n=1) and no amputation was performed.
In the literature and contrary to acute ischemia of the lower limbs, there is a great etiological diversity concerning the upper limbs; but cardiac causes remain among the most common causes [33,34]. Among these causes, atrial fibrillation ranks first. Its rate varies from 46% to 82.7% [33,35]. It is followed by valve disease reported in 17% to 33% of cases [36-38]. Embolic causes predominate over thrombotic causes, which remain difficult to diagnose (88% embolic versus 10% thrombotic) [39,40].
Conclusion
Acute limb ischemia is the most common emergency of all vascular surgery. This pathology raises both the problem of limb salvage and that of vital prognosis.
In our study, most of our patients were at Rutherford stage IIA. Embolectomy by Fogarty probe remains the "gold standard" for ischemia of embolic origin, we were able to perform it in 52 patients.
The Doppler ultrasound was the imaging examination that allowed us to make the diagnosis of acute ischemia in ourstudy. In developed countries, the reference examination is currently digitized arteriography.
The medical treatment is essential in the management of ischemia of the limbs both preoperatively and during follow-up, it must not be isolated at the present time from surgical treatment, which for the moment calls for conventional revascularization techniques. The endovascular techniques will probably have a role to play in the years to come.
Conflict of Interest
The authors declare no conflict of interest.
Contribution of Authors
Hafedh DALY: Acquisition, data analysis and writing
Abderrahim HMIDI, Islem CHNITI, Sandess SMARI and Cyrine MNASSRI: Acquisition, and analysis of results
References
- Norgren L, Hiatt WR, Dormandy JA, Nehler MR, Harris KA, et al. (2007) Inter-society Consensus for the Management of Peripheral Arterial Disease (TASC II). J VascSurg 45: 5-67.
- Koskas F. Kieffer E (1993) Conduite a tenir devant une ischemie aigue des membres. Enc cl Med Chir Urgences Page no: 9.
- Abbott WM, Maloney RD, McCabe CC, Lee CE, Wirthlin LS (1982) Arterialembolism: A 44- year perspective. Am J Surg 143: 460
- Fogarty TJ, Cranley JJ, Krause RJ, Strasser ES, Hafner CD (1963) A method for extraction of arterial emboli and thrombi. Surg Gynecol Obstet 116: 241-244.
- Langenskild M, Smidfelt K, Karlsson A, Bohm C, Herlit J et al. (2017) Weak Links in the Early Chain of Care of Acute LowerLimbIschaemia in Terms of Recognition and Emergency Management. Eur J Vasc Endovasc Surg 54: 235-240.
- Genovese EA, Chaer RA, Taha AG, Marone LK, Avgerinos E, et al. (2016) Risk Factors for Long-Term Mortality and Amputation after Open and Endovascular Treatment of Acute Limb Ischemia. Ann Vasc Surg 30: 82- 92.
- Duval S, Keo HH, Oldenburg NC, Baumgartner I, Jaff MR, Peacock JM, et al. (2014) The impact of prolonged lower limb ischemia on amputation, mortality, and functional status: the FRIENDS registry. Am Heart J Oct 168: 577-587.
- Grip O, Wanhainen A, Acosta S, Björck M (2017) Long-term Outcome after Thrombolysis for Acute Lower Limb Ischaemia. Eur J Vasc Endovasc Surg 53: 853-861.
- Wang SK, Murphy MP, Gutwein AR, Drucker NA, Dalsing MC, et al. (2018) Perioperative Outcomes are Adversely Affected by Poor Pretransfer Adherence to Acute Limb Ischemia Practice Guidelines. Ann Vasc Surg 50: 46-51.
- Genovese EA, Chaer RA, Taha AG, Marone LK, Makaroun MS, et al. (2016) Risk Factors for Long-Term Mortality and Amputation after Open and Endovascular Treatment of Acute Limb Ischemia. Ann Vasc Surg 30: 82-92.
- Byrne RM, Taha AG, Avgerinos E, Marone LK, Makaroun MS, et al. (2014) Contemporary outcomes of endovascular interventions for acute limb ischemia. J Vasc Surg 59: 988-995.
- Normahani P, Standfield NJ, Jaffer U (2017) Sources of Delay in the Acute Limb Ischemia Patient Pathway. Ann Vasc Surg 38: 279-285.
- Langenskild M, Smidfelt K, Karlsson A, Bohm C, Herlitz J, et al. (2017) Weak Links in the Early Chain of Care of Acute Lower Limb Ischaemia in Terms of Recognition and Emergency Management. Eur J Vasc Endovasc Surg 54: 235-240.
- de Donato G, Setacci F, Sirignano, Galzerano G, Massaroni R, et al (2014) The combination of surgical embolectomy and endovascular techniques may improve outcomes of patients with acute lower limb ischemia. J Vasc Surg 59: 729-736.
- Baril DT, Ghosh K, Rosen AB (2014) Trends in the incidence, treatment, and outcomes of acute lower extremity ischemia in the United States Medicare population. J Vasc Surg 60: 669-677.
- Eliason JL, Wainess RM, Proctor MC, Dimick JB, Cowan JA Jr, et al. (2003) A National and Single Institutional Experience in the Contemporary Treatment of Acute Lower Extremity Ischemia. Ann Surg. 238: 382-389.
- Dormandy J, Heeck L, Vig S (2001) Acute Limb Ischemia. Sem Vasc Surg 12: 148-153.
- Earnshaw J (2001) Demography and etiology of acute leg ischemia. SeminVasc Surg 14: 86-92.
- Brewster D, Chin A, Hermann G (1995) Acute limbischemia in Vascular Surgery. Wb Saunders, Philadelphia, USA, Page no: 648-668.
- Mills J, Porter J (1991) Donnees de base concernant les ischemies aigues des membres. Ann Chir Vasc, 5: 96-98.
- Cambria R, Abbott W (1984) Acute arterial thrombosis of the lower extremity. Arch Surg 119: 784-787.
- Pietri G, Alagni R (1975) Acute ischemia of peripheralarte- ries. Angiology 29: 161-165.
- Davies B, Braithwaite BD, Birch PA, Poskitt KR, Heather BP, et al. (1997) Acute leg ischemia in Gloucestershire. Br J Surg 84: 504- 508.
- Eyers P, Earnshaw JJ (1998) Acute non-traumatic arm ischaemia. Br J Surg 85: 1340-1346.
- Abbott WM, Maloney RD, McCabe CC, Lee CE, Wirthlin LS (1982) Arterialembolism : A 44 years perspective. Am J Surg 143: 460-464.
- Bae M, Chung SW, Lee CW, Choi J, Song S, et al. (2015) Upper Limb Ischemia: Clinical Experiences of Acute and Chronic Upper Limb Ischemia in a Single Center. Korean J Thorac Cardiovasc Surg 48: 246-251.
- Deguara J, Ali T, Modarai B, Burnand KG (2005) Upper limb ischemia: 20 years experience from a single center. Vascular 13: 84-91.
- Bergqvist D, Ericsson BF, Konrad P, Bergentz SE (1983) Arterial surgery of the upper extremity. World J Surg 7: 786-791.
- Alef MJ, Hamdan A (2014) Upper extremity arterial disease: general considerations. In : Rutherford RB (ed.). Vascularsurgery 8th edn, Philadelphia: Elsevier Saunders, Amsterdam, Netherlands Page no: 1868-1874.
- Kuukasjarvi P, Salenius JP, Pentti J (1995) Differences entre le Haut non traumatiques aigus et ischemie du membre inferieur. Chirurgie Vasculaire et Endovasculaire 29: 129-133.
- Blaisdell WF, Steele M, Allen RE (1978) Management of acute lower extremity arterial ischemia due to embolism and thrombosis. Surgery 84: 822-834.
- Licht PB, Balezantis T, Wolff B, Baudier JF, Røder OC (2004) Long-term outcome following thrombembolectomy in the upper extremity. Eur J Vasc Endovasc Surg 28: 508-512.
- Dag O, Ka GM, Erkut MA (2012) Analysis of risk factors for amputation in 822 cases with acute arterial emboli. Scientific. World Journal 2012: 673483.
- Vrt K, Ernovick F, Kubis J, Simo JD, Matis P (2001) Arterial embolisms in the extremities. Chirspol 2001;80(9):465-9.
- Hernandez-Richter T, Angele MK, Helmberger T, Jauch KW, Lauterjung L, et al. (2001) Acute ischemia of the upper extremity: Long-term results following thrombembolectomy with the Fogarty catheter. Langenbeck’s Archives of Surgery 386: 261-266.
- Davies MG, O’Malle K, Feele M, Colgan MP, Moore DJ, et al. (1991) Upper limb embolus: a timely diagnosis. Ann Vascsurg 5: 85-87.
- Magishi K, Izumi Y, Shimizu N (2010) Short- and long-term outcomes of acute upper extremity arterial thromboembolism. Ann Thorac Cardiovascsurg 16: 31-34.
- Karapolat S, Dag o, Abanoz M, Aslan M (2006) Arterial embolectomy: a retrospective evaluation of 730 cases over 20 years. Surg Today 36: 416-419.
- Wirsing P, Andriopoulos A, Bötticher R (1983) Arterial embolectomies in the upper extremity after acute occlusion. Report on 79 cases. J Cardiovascsurg (Torino) 24: 40-42.
- Skeik N, Soo-Hoo SS, Porten BR, Graber J, Alden P, et al. (2015) Arterial Embolisms and Thrombosis in Upper Extremity Ischemia. Vasc Endovascular Surg 49: 100-109.
Citation: Daly H, Hmidi A, Chniti I, Smari S, Mnassri C (2022) Diagnosis and Management of Acute Limbischemia J Angiol Vasc Surg 7: 089.
Copyright: © 2022 Hafedh Daly, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

