
Diaphragmatic Stab Lesion in a 3-Year-Old Girl - The Importance of Prompt Diagnosis and Prevention
*Corresponding Author(s):
Gabriela ReisPaediatrics Department, Unidade Local De Saúde Do Baixo Alentejo EPE, Portugal
Email:gabrielarmesquita90@gmail.com
Abstract
Domestic childhood accidents are a global health problem worldwide, representing a significant cause of mortality and morbidity, with hundreds of thousands of admissions in emergency departments. Most of these injuries happen in households, and the majority of the population is not aware of the dangers of some domestic devices. The authors present an unusual, but potentially deathly injury caused by a fall on a dishwasher.
Three-year-old girl observed in the emergency department for a penetrating thoracic injury. She was brought in the operating room for surgical exploration, showing diaphragm laceration. The diaphragmatic injury was repaired, free of complications.
Traumatic diaphragmatic injuries are rare, easily missed and require prompt diagnosis and intervention. With this case, the authors highlight, not only the importance of keeping a high level of suspicious for this conditions, but also of preventing these events.
Keywords
Accidents; Children; Diaphragm; Knife; Laceration; Prevention
Introduction
Accidents involving children are considered a significant global health problem that requires urgent attention, especially in the first year of life [1-2]. Child unintentional injuries include traffic accidents, falls, burns, drowning, poisonings and intoxication [3] and are one of the leading causes of death, hospitalization and disability across the world [1-2,4]. Moreover, tens of millions of children require hospital care, and many others are left with some form of disability, often with lifelong consequences [2].
Domestic accidents represent the most common cause of death in children above 1 year of age and annually, over one million children under 15 years old present to emergency departments in the United Kingdom with household-related injuries. Kitchen appliances are the main sources of domestic injuries in children living in urban areas [5]. According to a survey study of English households, five per cent of the children had suffered an injury during domestic activities and just under half of the household’s loaded sharp utensils with the serrated, spiky or pointy ends positioned upward [6].
Additionally, the dishwasher’s door average height is estimated to be 26 cm [7], which makes them especially dangerous to stab injuries. However, data on stabbing injuries in children caused by kitchen devices, in English literature, is null.
The risk of diaphragmatic injury in stab wounds in the lower segment of the chest and the upper segment of the abdomen has been an issue of importance for surgeons throughout time [8]. Traumatic Diaphragmatic Injury (TDI) has an incidence of 0.46%-8% and a penetrating versus blunt trauma ratio of 2:1 [9]. Besides its rareness, timely diagnosis in paediatric age is a challenge, since both clinical and radiological signs are unreliable, requiring a high level of suspicion [10]. Some TDI might not be promptly diagnosed and the estimated rate of occult injury of 15 to 20% [11]. The delay in diagnosis may lead to severe complications, since these injuries are often associated with laceration of other intra-abdominal organs and due to the difference in pressures, small injuries often become large injuries after a short time, with a 4.4-48.1% mortality rate [11].
The authors present a rare case of a 3-year-old girl, with a stab wound with TDI resulting from a fall on the dishwasher.
Case Report
In September 2020, a previously healthy 3-year-old girl, was admitted to the emergency department, after being transferred from another hospital, with a penetrating thoracic injury with a knife, after falling on an open dishwasher.
On examination, the child was hemodynamically stable (MAP 75 mmHg; HR 90 bpm; RF 40 cpm; T 36ºC), eupneic and alert. She presented a penetrating wound on the lower third of the right hemi thorax, with muscle and aponeurosis exposure (Figure 1). Cardiac and pulmonary sounds were normal. Otherwise, physical examination was unremarkable.
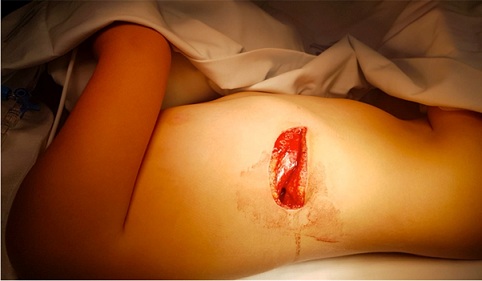 Figure 1: Penetrating wound on the lower third of the right hemi thorax, with muscle and aponeurosis exposure
Figure 1: Penetrating wound on the lower third of the right hemi thorax, with muscle and aponeurosis exposure
From the additional evaluation, blood tests showed no alterations (HB 12.3 g/dL; WBC 16090/uL; PLT 481.000; ASTL 48 UI/L; ALT 21 UI/L; GGT 13; AF 254; normal Coagulation study). She underwent CT scan, which showed a small hemo-pneumothorax, intra abdominal air bubble, with no apparent hepatic bleeding. Diaphragm was reported as normal.
On the suspicion of diaphragmatic rupture, the child was brought in the operating room for surgical exploration under general anesthesia. Wound exploration was accomplished directly through the wound and also with thoracoscopic assistance. After entering the thoracic cavity, a 2-3 cm diaphragm laceration was promptly identified (Figure 2). The video-assisted inspection of the thoracic cavity and (partially) of the peritoneal space allowed to exclude other associated lesions besides a small hepatic subcapsular haematoma. The diaphragmatic injury was primarily closed with interrupted sutures without tension. No chest drain was inserted. The procedure underwent free of complications. The postoperative course was uneventful and she was discharged on the second postoperative day, on antibiotics (Amoxiciline-Clavulanic acid).
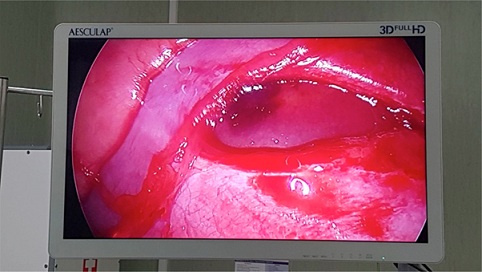 Figure 2: Video-assisted image capture during thoracic inspection. Diaphragmatic tear with a liver hematoma was easily identified.
Figure 2: Video-assisted image capture during thoracic inspection. Diaphragmatic tear with a liver hematoma was easily identified.
Discussion
Injuries are a leading cause of death and disability among children [2]. Their propensity for accidents may be explained for some authors by their degrees of dependence, activities and risk behaviors, physical and cognitive abilities that change as they grow older [12-17]. Besides, injuries from others need to be considered as well [18]. The age of this patient combines the free mobility of a human being that has no consciousness to predict/avoid harmful event, making her more prone to these accidents.
Traumatic Diaphragmatic Injury (TDI) is a rare complication of abdominal trauma [19]. A high index of suspicion is required to diagnose this injury, considering its incidence, the lack of specificity of clinical and radiological findings and the severity of associated lesions [19].
Hence, TDI is easily missed and delayed emergent presentations can occur with an increased rate of morbidity and mortality [19]. Clinical findings albeit scarce and nonspecific are still recognized in some cases. The most common reported signs/symptoms are dyspnea (86%) and reduction in breath sounds on the affected side (73%) [19]. Chest X-ray and Computorized Tomography (CT) are frequently used to support the diagnosis. The pathognomonic sign of TDI is the presence of abdominal organs in the pleural space. Since TDI can occur without herniation, imaging studies might be negative or show nonspecific alterations [19]. In the case presented, besides the thoracic penetrating wound, no additional sign/symptom was depicted. The thoracic CT showed signs of peritoneal cavity violation but no specific sign of TDI.
TDI management when preoperatively recognized is surgical approach by exploratory laparotomy in most cases (81.1%) [19]. In our case, TDI was diagnosed in the course of surgical exploration of a penetrating wound in the chest. This typifies the missed diaphragmatic injury in the course of traumatic chest injury, as previously stated, and highlights the importance of maintain a high suspicion of associated injuries in penetrating thoracic and abdominal trauma.
Accidents may be considered the result of random, uncontrolled factors, however, still preventable. Parents and caregivers’ supervision is fundamental to protect children from harm. It is estimated that 90% of young children’s injuries occur in their home when an adult is supposedly supervising them [2]. According to WHO Report on child on Injury prevention (2008), some approaches may include implementation of proven prevention methods and a model of primary, secondary and tertiary measures is suggested [2]. Family counselling, changes in home environment and identification of risk factors, according to the stage of the child development are important factors for developing effective preventive interventions, according to four randomized studies [20-23]. In most of the reviewed studies, educational interventions to reduce risk factors and control behavior were effective [20-23].
School and home are the most frequently attended places by children and therefore, where much of the preventive interventions must take place. The most commonly addressed risk factors for home-based accident prevention were those identified in previous etiological studies of childhood accidents, such as presence of bunk beds, stoves, chairs, electrical outlets and toxic products within easy reach [24,25]. A study from MuhsenandKhadim (2014) highlights the potential danger to children of kitchen devices such as the dishwasher. They emphasise the unsafe design of most of the devices that, in itself puts children running around in the kitchen at risk of easily tripping and landing on pointy utensils. Furthermore, these authors point out some common and dangerous practices of dishwasher users, such as not reading the manual prior to using the machine, encouraging the participation of children in loading and unloading dishwashers and the placement of some pointy or sharp utensils with their sharp ends upwards [6]. In our case report, parents were not aware of the dangers of placing pointy and sharp devices upwards and they were never elucidated by a health professional about the dangers and preventive measures. This epitomize the need of better educate and aware both parents and caregivers to prevent harmful accidents and injuries in dependent and unenlightened subjects. With this case report, the authors aim to highlight the importance of preventing domestic accidents, especially the most severe, that usually take place in the kitchen.
The authors recommend that manufacturers should pay special attention to highlight the dangers of some kitchen appliances, but also that parents should be alert to the security measures while a child is around.
Furthermore, it is important to keep a high level of suspicious of a diaphragmatic injury in lower thoracic or high abdominal stab wounds.
Funding Sources
There were no external funding sources for the realization of this paper.
Consent for Publication
Consent for publication was obtained.
Confidentiality of Data
The authors declare that they have followed the protocols of their work centre on the publication of patient data.
Statement of Conflict of Interests
The authors have nothing to disclosure
References
- Barcelos RS, Del-Ponte B, Santos IS (2018) Interventions to reduce accidents in childhood: A systematic review. J Pediatr (Rio J) 94: 351-367.
- Peden M, Oyegbite K, Ozanne-Smith J, Hyder AA, Branche C, et al. (2008) World report on child injury prevention. World Health Organization, Geneva. Pg no: 1-232.
- Hyder AA, Sugerman D, Ameratunga S, Callaghan JA (2007) Falls among children in the developing world: A gap in child health burden estimations? Acta Paediatr 96: 1394-1398.
- Gordon JE (1949) The epidemiology of accidents. Am J Public Health Nations Health 39: 504-515.
- MacIntyre BH (1997) The dangerous kitchen. Ugeskr Leager 159: 4533.
- Muhsen WS, Khadim MF (2014) Dishwasher-related injuries: Survey and literature review. Int J Inj Contr Saf Promot 22: 86-88.
- https://www.cdc.gov/growthcharts/html_charts/lenageinf.htm
- Sullivan RE (1966) Strangulation and obstruction in diaphragmatic hernia due to direct trauma. Report of two cases and review of the English literature. J Thorac Cardiovasc Surg 52: 725-734.
- Koto MZ, Matsevych OY, Nsakala L (2019) Evaluation of thoracoscopy with single-lumen endotracheal tube intubation and laparoscopy in the diagnosis of occult diaphragmatic injuries in penetrating thoracoabdominal trauma. J Laparoendosc Adv Surg Tech A 29: 785-789.
- Ghionzoli M, Bongini M, Piccolo RL, Martin A, Persano G, et al. (2016) Role of thoracoscopy in traumatic diaphragmatic hernia. Pediatr Int 58: 601-603.
- Bagheri R, Tavassoli A, Sadrizadeh A, Mashhadi MR, Shahri F, et al. (2009) The role of thoracoscopy for the diagnosis of hidden diaphragmatic injuries in penetrating thoracoabdominal trauma. Interact Cardiovasc Thorac Surg 9: 195-197.
- Prüss-Ürsün A, Corvalán C (2006) Preventing disease through healthy environments: A global assessment of the burden of disease from environmental risks. World Health Organization, Geneva.
- Rivara FP (1995) Developmental and Behavioral Issues in Childhood Injury Prevention. Journal of Developmental & Behavioral Pediatrics 16: 362-370.
- Agran PF, Winn D, Anderson C, Trent R, Walton-Haynes L (2001) Rates of pediatric and adolescent injuries by year of age. Pediatrics 108: 45.
- Agran PF, Anderson C, Winn D, Trent R, Walton-Haynes L, et al. (2003) Rates of pediatric injuries by 3-month intervals for children 0 to 3 years of age. Pediatrics 111: 683-692.
- Towner E, Therese D, Errington G, Burkes M, Towner J (2005) Injuries in children aged 0-14 years and inequalities.
- Flavin MP, Dostaler SM, Simpson K, Brison RJ, Pickett W (2006) Stages of development and injury patterns in the early years: A population-based analysis. Bio Med Central Public Health 6.
- Grossman DC (2000) The history of injury control and the epidemiology of child and adolescent injuries. The Future of Children 10: 23-52.
- Marzona F, Parri N, Nocerino A, Giacalone M, Valentini E, et al. (2019) Traumatic diaphragmatic rupture in pediatric age: Review of the literature. Eur J Trauma Emerg Surg 45: 49-58.
- Gielen AC, McKenzie LB, McDonald EM, Shields WC, Wang MC, et al. (2007) Using a computer kiosk to promote child safety: results of a randomized, controlled trial in an urban pediatric emergency department. Pediatrics 120: 330-339.
- Phelan K, Khoury J, Xu Y, Liddy S, Hornung R, et al. (2011) A randomized controlled trial of home injury hazard reduction: The HOME injury study. Arch Pediatr Adolesc Med 165: 339-345.
- Odendaal W, van Niekerk A, Jordaan E, Seedat M (2009) The impact of a home visitation programme on household hazards associated with unintentional childhood injuries: A randomised controlled trial. Accidents; Analysis and prevention 41: 183-190.
- van Beelen MEJ, Beirens TMJ, den Hertog P, van Beeck EF, Raat H (2014) Effectiveness of web-based tailored advice on parents’ child safety behaviors: Randomized controlled trial. J Med Internet Res 16: 17.
- Khambalia A, Joshi P, Brussoni M, Raina P, Morrongiello B, et al. (2006) Risk factors for unintentional injuries due to falls in children aged 0-6 years: A systematic review. Inj Prev 12: 378-381.
- Atak N, Karaoglu L, Korkmaz Y, Usubutun S (2010) A household survey: Unintentional injury frequency and related factors among children under five years in Malatya. Turk J Pediatr 52: 285-293.
Citation: Reis G, Fernandes, Oliveira MS (2022) Diaphragmatic Stab Lesion in a 3-Year-Old Girl - The Importance of Prompt Diagnosis and Prevention. J Neonatol Clin Pediatr 9: 090.
Copyright: © 2022 Gabriela Reis, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

