
Effectiveness and Safety of Sleeve Gastrectomy in Elderly Patients above 60 Years
*Corresponding Author(s):
Emad AljohaniGeneral Surgery, King Abdulaziz Medical City, Riyadh, Saudi Arabia
Tel:+966 555597192,
Email:dr.aljohani@hotmail.com
Abstract
Background
As the obesity is pandemic, the requisite for bariatric treatment and novel interventions has surged substantially. Among various bariatric strategies to cope with the obesity challenge, sleeve gastrectomy has proved to be the most effective.
Aim
To evaluate the effectiveness and safety of sleeve gastrectomy for weight loss in morbidly obese elderly Saudi patients (60 years).
Methodology
A prospective cohort study on 205 patients undergoing Laparoscopic Sleeve Gastrectomy (LSG) was carried out from January 2013 to August 2016, with a follow up time of 6 months and then 1 year. The study included patients of >60 years of age who have a Body Mass Index (BMI) of >40 kg/m2. The primary objective of this study includes the percent Excess Weight Loss (%EWL), Length of Stay (LOS), 30-days and 1-year mortality and morbidity rates.
Results
The mean age of patients was 65 years, of which 60% were females. The Mean weight before the surgery was 120 Kg with a pre-operative BMI of 44 kg/m2. Patients underwent vertical sleeve gastrectomy laparoscopically with a mean LOS of 2 days. Follow-up was performed twice, within 6 months and then 1 year after the operation, which showed statistically significant reduction in the average weight and BMI (P-value= <0.001). Percent EWL was 48% and 59% at the 6 and 12 months follow ups, respectively. In all patients, the 30-days and 1-year mortality and morbidity rate was 0%.
Conclusion
laparoscopic sleeve gastrectomy is effective and safe surgery for significant %EWL in morbidly obese elderly patients in Saudi Arabia.
Keywords
ABBREVIATIONS
• Laparoscopic Sleeve Gastrectomy (LSG)
• Body Mass Index (BMI)
• Percent Excess Weight loss (%EWL)
• Length of Stay (LOS)
INTRODUCTION
Obesity which is currently affecting more than 600 million adults worldwide is a big challenge of contemporary times. Obesity is a multifactorial metabolic disorder which is characterized by BMI >30 kg/m2 [1]. Challenges presented by obesity in aged subjects are different from those in other age groups owing to associated intricate pattern of comorbidities. Changes encountered by body during ageing such as Lean Body Mass (LBM), frailty, high fat content, when accompanied by obesity leads to functional deterioration and comorbidities [2]. Although adverse consequences of obesity such as diabetes, cardiovascular diseases, depression and even malignancies [3] are observed in all age groups, elderly patients are more prone to these disorders mainly because of frailty.
With obesity pandemic the requisite for bariatric treatment and novel interventions has surged substantially. Amongst various bariatric strategies to cope with the obesity challenge, bariatric surgery has proved to be the most effective [4]. Gastric bypass, gastric band, gastric sleeves, gastric balloons and bilio-pancreatic diversion with duodenal switch are the usual options in bariatric surgery. Gastric Sleeve surgery also known as sleeve gastrectomy was first presented as part of bilio-pancreatic diversion but currently it has become an attractive stand-alone procedure and has replaced gastric bypass and gastric banding in several hospitals around the globe [5].
Gastric sleeve works on the principle of restricting total area used for energy intake producing a feeling of satiety by removing ghrelin-producing stomach spot [6,7]. It has become a preferred choice due to excessive weight loss, being a simple procedure, and having few complications [8]. Laparoscopic Sleeve Gastrectomy involves a longitudinal resection of the stomach on the greater curvature from the antrum. The procedure consists of two key steps: division of the vascular supply of the greater curvature of the stomach, achieved with the dissection section of the gastro-colic and gastro-splenic ligaments, and longitudinal gastrectomy that “sleeves” the stomach to reduce it to a tube. Gastric sleeve had been carried out on obese patients and resulted in excessive weight loss in various studies; yet the literature was meager in reporting its effectiveness for elderly obese patients [9-11].
METHODOLOGY
Patients’ selection
Intervention and followup
Statistical analysis
Results
|
Variables |
Results |
|
Total number of patients |
N= 205 |
|
Gender |
60% Female 40% male |
|
Age |
60 years |
|
Mean pre-operative Weight |
120 kg |
|
Mean pre-operative BMI1 |
44 kg/m2 |
|
Mean %EWL2 at 6 months |
48% |
|
Mean %EWL at 12 months |
59% |
|
LOS3 |
2 days |
|
6 & 12 months Mortality |
0% |
Table 1: Summary of the results.
1 Body Mass Index (BMI); 2 Percent Excess Weight Loss (%EWL); 3 Length of Stay (LOS).
DISCUSSION
Laparoscopic Sleeve Gastrectomy is one of the more invasive procedures compared to gastric banding, and does not have the possibility of restitutio-ad-integrum. As far as post-operative complications are concerned, Sleeve Gastrectomy has been reported to decrease the absorption of vitamin B12 and iron [12]. It also gives rise to gastroesophageal reflux “de novo” and difficulty in gastric emptying and suture line fistula (2.7%), requiring multidisciplinary follow up for success of surgery [13,14]. On the other hand, LSG has many advantages, with the literature reporting %EWL varying from 33% to 83% in various series post LSG [6,15-18]. The riddance from comorbidities is promising [19] with significant improvements in QOL postoperatively, whereas pylorus-preserving also eliminates the risk of post-op dumping syndrome [20,21]. In terms of %EWL, the results of the current study were in accordance with the literature [9]. Despite the advanced age, the patients experienced a clinically significant reduction in weight, with an average of 55% EWL at 1 year, as well as a reduction in daily medication use. Figure-1 summarized the average % EWL of the published studies to date.
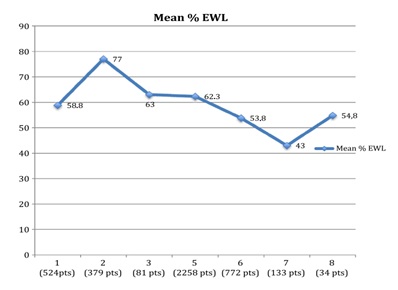 Figure 1: Mean % EWL at different follow-up intervals in the literature. The vertical axis indicates the mean % EWL, while the horizontal axis indicates the years.
Figure 1: Mean % EWL at different follow-up intervals in the literature. The vertical axis indicates the mean % EWL, while the horizontal axis indicates the years.
CONCLUSION
This study showed promising %EWL post Laparoscopic Sleeve Gastrectomy for elderly patients, accompanied with no post-op morbidity or mortality after one year which demonstrated efficacy and safety of weight loss surgery as a treatment for morbid obesity in patient’s ≥60 years of age. This study shows comparable complication and mortality rate results to studies examining weight-loss surgery in younger patients, which might be attributed to thorough preoperative evaluation in this traditionally higher-risk cohort. Age should not be a barrier for patients who desire weight-loss surgery. Long-term follow up studies will enhance our knowledge in terms of improvement in associated comorbidities.
CONFLICTING INTERESTS
None declared.
REFERENCES
- Ogden CL, Carroll MD (2010) Prevalence of overweight, obesity, and extreme obesity among adults: United States, trends 1960-1962 through 2007-2008. National Center for Health Statistics 6: 1-6.
- Villareal DT, Banks M, Siener C, Sinacore DR, Klein S (2004) Physical frailty and body composition in obese elderly men and women. Obes Res 12: 913-920.
- Schelbert KB (2009) Comorbidities of obesity. Primary Care: Clinics in Office Practice 36: 271-285.
- Buchwald H, Avidor Y, Braunwald E, Jensen MD, Pories W, et al. (2004) Bariatric surgery: A systematic review and meta-analysis. JAMA 292: 1724-1737.
- Bohdjalian A, Langer FB, Shakeri-Leidenmühler S, Gfrerer L, Ludvik B, et al. (2010) Sleeve gastrectomy as sole and definitive bariatric procedure: 5-year results for weight loss and ghrelin. Obes Surg 20: 535-540.
- Baltasar A, Serra C, Pérez N, Bou R, Bengochea M, et al. (2005) Laparoscopic sleeve gastrectomy: A multi-purpose bariatric operation. Obes Surg 15: 1124-1128.
- Jen S, Simillis C, Efthimiou E (2013) A very challenging leak from a sleeve gastrectomy. Surg Obes Relat Dis 4: 56-59.
- Weber M, Müller MK, Bucher T, Wildi S, Dindo D, et al. (2004) Laparoscopic gastric bypass is superior to laparoscopic gastric banding for treatment of morbid obesity. Ann Surg 240: 975-983.
- Brethauer SA, Hammel JP, Schauer PR (2009) Systematic review of sleeve gastrectomy as staging and primary bariatric procedure. Surg Obes Relat Dis 5: 469-475.
- Dapri G, Vaz C, Cadière GB, Himpens J (2007) A prospective randomized study comparing two different techniques for laparoscopic sleeve gastrectomy. Obes Surg 17: 1435-1441.
- Melissas J, Koukouraki S, Askoxylakis J, Stathaki M, Daskalakis M, et al. (2007) Sleeve gastrectomy: A restrictive procedure? Obes Surg 17: 57-62.
- Lazear J, Lintner NC, Bode C, Zimberg P (2012) Reproductive concerns and pregnancy after bariatric surgery: Practice implications. Bariatric Nursing and Surgical Patient Care 7: 75-82.
- Moon RC, Teixeira AF, Jawad MA (2017) Safety and effectiveness of anterior fundoplication sleeve gastrectomy in patients with severe reflux. Surg Obes Relat Dis 13: 547-552.
- Daes J, Jimenez ME, Said N, Daza JC, Dennis R (2012) Laparoscopic sleeve gastrectomy: Symptoms of gastroesophageal reflux can be reduced by changes in surgical technique. Obes Surg 22: 1874-1879.
- Himpens J, Dobbeleir J, Peeters G (2010) Long-term results of laparoscopic sleeve gastrectomy for obesity. Ann Surg 252: 319-324.
- Milone L, Strong V, Gagner M (2005) Laparoscopic sleeve gastrectomy is superior to endoscopic intragastric balloon as a first stage procedure for super-obese patients (BMI > or =50). Obes Surg 15: 612-617.
- Uglioni B, Wölnerhanssen B, Peters T, Christoffel-Courtin C, Kern B, et al. (2009) Midterm results of primary vs. secondary laparoscopic sleeve gastrectomy (LSG) as an isolated operation. Obes Surg 19: 401-406.
- Fuks D, Verhaeghe P, Brehant O, Sabbagh C, Dumont F, et al. (2009) Results of laparoscopic sleeve gastrectomy: A prospective study in 135 patients with morbid obesity. Surgery 145: 106-113.
- Cottam D, Qureshi FG, Mattar SG, Sharma S, Holover S, et al. (2006) Laparoscopic sleeve gastrectomy as an initial weight-loss procedure for high-risk patients with morbid obesity. Surgical Endosc 20: 859-863.
- Imada T, Rino Y, Takahashi M, Suzuki M, Tanaka J, et al. (1998) Postoperative functional evaluation of pylorus-preserving gastrectomy for early gastric cancer compared with conventional distal gastrectomy. Surgery 123: 165-170.
- Hasler WL (2002) Dumping syndrome. Current treatment options in gastroenterology 5: 139-145.
Citation: Alqahtani A, Almadi F, Aljohani E (2019) Effectiveness and Safety of Sleeve Gastrectomy in Elderly Patients above 60 Years. J Surg Curr Trend Innov 3: 016.
Copyright: © 2019 Awadh Alqahtani, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

