
Journal of Gerontology & Geriatric Medicine Category: Medical
Type: Case Report
Elderly Patient with Hematuria and Lithiasis: The Point of View of the Geriatrician through the Analysis of a Case Report
*Corresponding Author(s):
Valerio Massimo MagroDepartment Of Internal Medicine And Geriatry, University Of Campania Luigi Vanvitelli, Piazza L Miraglia 2, 80100, Naples, Italy
Tel:+39 3492224922,
Email:valerio_magro@hotmail.com
Received Date: Jun 13, 2019
Accepted Date: Jun 26, 2019
Published Date: Jul 03, 2019
Abstract
The effective management of hematuria requires a careful evaluation in the elderly patient. However, the evaluation of urinary stones is an aspect of the patient taken as a whole. From the urological point of view, the measurement of the size of the stones, their positioning and the evaluation of the most suitable and least traumatic technique for the patient to remove the stones are certainly important elements to be taken into consideration by the doctor. From the geriatric point of view, it is also necessary to take into consideration the degree of fragility of the patient, keeping in mind the comorbidities that afflict him and their treatment. The consideration of all these aspects generates a global take that is certainly more complex than the management of stones only, but more attentive to the patient itself in its individuality as a sick person. We took the opportunity of the management of a patient with lithiasis to discuss here conditions of studying the quantification of the stones by invasive or noninvasive assessments and above all in a multidimensional perspective.
Keywords
Biopsy; Geriatrician; Hematuria; Lithiasis; Uro-CT
INTRODUCTION
The genesis of hematuria does not grant any superficiality, especially in elderly patients, because next to no medical conditions it can grow for several diseases, some even poor prognosis (it is the first sign of the bladder cancer or kidney cancer) [1,2]. The duties of the Geriatrician in these cases are an exact assessment of internal medicine sign with a comprehensive and multidimensional assessment of the patient, collaborating and interacting with their colleagues (nephrologist, urologist; general practitioner) in the medical management of the lithiasis, of the urological procedures and with a follow-up as a going concern hospital-Territory care [3,4].
CASE PRESENTATION
We considered a studied patient for this purpose and we draw some considerations on the study of patients with lithiasis. We saw a 73 years old patient, who was married with four grown children. He suffered from hypertension, hyperuricemia, hypercholesterolemia, carotid atherosclerosis, Prostatic Hyperplasia (BPH) with frequent dysuria, a previous tibial-fibular fracture (screw-plate carrier) and a preexistent endoscopic excision (2015) of a hairy-tubule polyp in the rectum-sigmoid tract. His therapy was: ramipril 5 mg, allopurinol 150 mg, Acetylsalicylic Acid (ASA) 100 mg, atorvastatin 20 mg, dutasteride 0.5 mg (Figure 1).
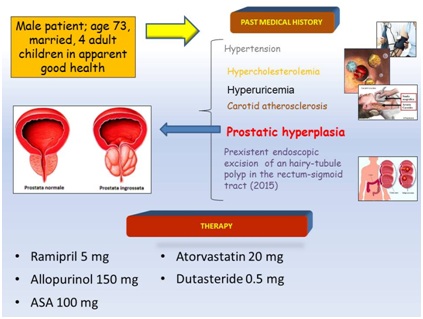 Figure 1: Patient's clinical history and home therapy at the time of taking charge.
Figure 1: Patient's clinical history and home therapy at the time of taking charge.Physical examination and geriatric evaluation
We saw this patient for the appearance, in the last week, of the accentuation of dysuria with the presence of urinary urgency and occasional strangury, up to two episodes of gross hematuria interspersed with a week of normochromic urine in the absence of trauma/exercise, with a change of the humor in anxiety-depression and a reduced quality of life. The patient was lucid and alert (Mini Mental State Examination - MMSE 30/30), Activity Daily Living - ADL 5/6; Instrumental Activity Daily Living - IADL 7/8; marked deflection of the humoral tone (Geriatric Depression Scale - GDS 15). Vital signs limits except blood pression. The patient showed a pain rated as moderate according to the numerical scale (Number Rating Scale, NRS 5/10). Nothing overall objective examination. On examination urogenital Giordano’s sign was negative bilaterally (the manual percussion of the renal lodges did not evoke an accentuation of the pain), absence of globe bladder and urethral injuries on inspection. No tenderness to pyelo-ureteral points. Remaining objectivity normal.
Laboratory and radiological examinations
Blood tests showed blood glucose 103 mg/dl, urea 53 mg/dL, creatinine 0.89 mg/dl, serum sodium 145 mEq/L, potassium 4.5 mEq/L, serum calcium 9.9 mg/dl (normoalbuminemia) and serum chloride 111 mEq/L, PCR 0.063 mg/dl, the remaining parameters were in the limits.
Urinalysis: Acid pH and presence of erythrocytes in the urinary sediment, in the absence of nitrites and bacteriuria. We suspended ASA and other imaging tests were performed. The Rx direct abdomen brought to light "kidney shadows in the partially masked by gas with evidence right training radiopaque with other radiopaque formations in the pelvic cavity"; Abdominal echo "kidney normoconformati to inhomogeneous hypoechoic cortical for cysts, no noticeable signs of obstructed urinary flow, adjusted index nefrometrico and report cortico-pielico; expanse bladder, to thickened walls, with evidence of numerous intraluminal calculations, most subcentimetric (the higher 13 mm); of increased prostate volume, post-void residual 23 cc".
Urinalysis: Acid pH and presence of erythrocytes in the urinary sediment, in the absence of nitrites and bacteriuria. We suspended ASA and other imaging tests were performed. The Rx direct abdomen brought to light "kidney shadows in the partially masked by gas with evidence right training radiopaque with other radiopaque formations in the pelvic cavity"; Abdominal echo "kidney normoconformati to inhomogeneous hypoechoic cortical for cysts, no noticeable signs of obstructed urinary flow, adjusted index nefrometrico and report cortico-pielico; expanse bladder, to thickened walls, with evidence of numerous intraluminal calculations, most subcentimetric (the higher 13 mm); of increased prostate volume, post-void residual 23 cc".
Management
The patient was started on uro-CT [5,6]. The tomographic examination showed at the level of the medium calyceal group to the right of 10 mm lithiasic formation, without dilation of the urinary tract, detrusor hypertrophy and distended bladder with multiple sub and pericentimetric calculi; prostate volume was increased with uneven contrastographic impregnation, especially in the middle lobe, with bladder floor imprint. The patient was finally launched in unblocking associated with endoscopic lithotripsy under spinal anesthesia, immediately grinding bladder stones (immediate expulsion) and treating kidney stone with lithotripsy later, to reduce its size, followed by endoscopic removal [7-10]. At two months, the absence of new episodes of hematuria (for which it decided the resumption of the ASA), good quality of life and social life (ADL and IADL ceilings; number rating scale - NRS 2/10), improvement in urinary symptoms (lingered some tenesmus bladder, so it was decided to introduce tamsulosin associated with dutasteride, after pressure monitoring and PSA) and improved mood (GDS 7), so we opted for "watchful waiting" before prescribing an SSRI and subsequent potential management of prostate disease.
DISCUSSION
For the study of stones we have used more than one imaging technique. In fact, the combined use of the abdomen and US direct radiography (below in the flow chart from the urological computerized tomography - uro-CT) [11] has an approximately 89-100% sensitivity/specificity of diagnosis. It allow to obtain information on the presence/nature of stones, as well as on the presence and extent of the obstruction, using techniques semi-invasive or non-invasive in over 90% of patients with lithiasis in place (due to the poor ability of spontaneous elimination of centimetric calculations, even more rare in the presence of BPH). Moreover, the centimetric calculations are distinguished, as is written in the literature by a lower efficacy of ESWL (Extracorporeal Shock Wave Lithotripsy) for kidney stones (which justified the use here, in two stages, the endoscopic-urethroscopy technique, URS) [12,13]. For the IPB was used the inhibitor combination of 5-alpha-reductase and alpha-blocker (tamsulosin and dutasteride is chosen in over 60% of cases), both to facilitate the leakage of the calculations which caused significant symptom improvement (trial CombAT) [14-16], following the Evidence Based-Medicine - EBM indications of scientific societies (Italian Society of Urology, SIU; Italian Association of Urologists, AURO) [13,17-19]. This also allowed not to put the luggage in the therapeutic SSRI, safeguarding the elderly patient from inherent dangers of polypharmacy but also by adverse effects of excessive decisiveness therapy (prostatectomy and its adverse iatrogenic events and postoperative complications). In conclusion, the management of our patients has allowed a minimum use of in-hospital treatment, an improvement in symptoms and a speedy return of the subject to his life, in his natural environment and his family. In this we have tried to follow the recommendations of both the nepho-urologic (Italian Society of Urology, SIU; Italian Society of Nephrology, SIN; Italian Association of Urologists, AURO) and geriatric (Italian geriatrics and gerontology society - SIGG; Italian Society of Hospital and Community Geriatrics - SIGOT) scientific societies that the geriatric methodology (the multidimensional assessment).
CONCLUSION
The presented case report reflects, in our view, a typical case of a patient with renal pathology who is taken in charge according to an eminently geriatric perspective. The success of the choices made and the good quality of life of the subject, combined with its independence in real life, are the objectives that have been pursued, geriatric perspective, to combine patient care according EBM, problem solving of lithiasis and safeguarding social and affective life, the mission Geriatrician in any medical field, including the nephro-urologic field.
REFERENCES
- Hicks D, Li CY (2007) Management of macroscopic haematuria in the emergency department. Emerg Med J 24: 385-390.
- Rodgers M, Nixon J, Hempel S, Aho T, Kelly J, et al. (2006) Diagnostic tests and algorithms used in the investigation of haematuria: Systematic reviews and economic evaluation. Health Technol Assess 10: iii-iv.
- Wiedemann A (2017) [Geriatric urology: Increasingly important in urological care]. Urologe A 56: 992-996.
- Jimbo M (2010) Evaluation and management of hematuria. Prim Care 37: 461-472.
- Müllhaupt G, Engeler DS, Schmid HP, Abt D (2015) How do stone attenuation and skin-to-stone distance in computed tomography influence the performance of shock wave lithotripsy in ureteral stone disease? BMC Urol 15: 72.
- Cakiroglu B, Eyyupoglu SE, Tas T, Balci MC, Hazar I,, et al. (2014) Are Hounsfield densities of ureteral stones a predictive factor for effectiveness of extracorporeal shock wave lithotripsy? Int J Clin Exp Med 7: 1276-1283.
- Philippou P, Lamrani D, Moraitis K, Wazait H, Masood J, et al. (2011) Shock-wave lithotripsy in the elderly: Safety, efficacy and special considerations. Arab J Urol 9: 29-33.
- Philippou P, Lamrani D, Moraitis K, Bach C, Masood J, et al. (2012) Is shock wave lithotripsy efficient for the elderly stone formers? Results of a matched-pair analysis. Urol Res 40: 299-304.
- Kramolowsky EV, Quinlan SM, Loening SA (1987) Extracorporeal shock wave lithotripsy for the treatment of urinary calculi in the elderly. J Am Geriatr Soc 35: 251-254.
- Knoll T, Buchholz N, Wendt-Nordahl G (2012) Extracorporeal shockwave lithotripsy vs. percutaneous nephrolithotomy vs. flexible ureterorenoscopy for lower-pole stones. Arab J Urol 10: 336-341.
- Borghi L, Caudarella R, Gambaro G (2000) Guidelines for nephrolithiasis. Italian Society of Nephrology (SIN). Giornale Italiano di Nefrologia 17: 59-64.
- Chaussy CG, Tiselius HG (2018) How can and should we optimize extracorporeal shockwave lithotripsy? Urolithiasis 46: 3-17.
- Association of Italian Urologists (AURO) (2007) Guideline on Urinary Stones. AURO, Palazzo Del Casinò, Lido, Italy.
- Oelke M, Roehrborn CG, D'Ancona C, Wilson TH, Castro R, et al. (2014) Nocturia improvement in the combination of Avodart(®) and tamsulosin (CombAT) study. World J Urol 32: 1133-1140.
- Roehrborn CG, Wilson TH, Black LK (2012) Quantifying the contribution of symptom improvement to satisfaction of men with moderate to severe benign prostatic hyperplasia: 4-year data from the CombAT trial. J Urol 187: 1732-1738.
- Walker A, Doyle S, Posnett J, Hunjan M (2013) Cost-effectiveness of single-dose tamsulosin and dutasteride combination therapy compared with tamsulosin monotherapy in patients with benign prostatic hyperplasia in the UK. BJU Int 112: 638-646.
- Baggio B (2000) Drawing up guidelines for the management of kidney stones in Italy. J Nephrol 3: 61-64.
- Pagliarulo A, Bertaccini A, Breda G, D'Elia G, Ferri C, et al. (2009) Content '2009 Guidelines''. Italian Society of Urology, Palazzo Del Casinò, Lido, Italy.
- Cupisti A, Vezzoli G, Croppi E, Lombardi M, Marangella M, et al. (2011) Diagnostic procedure and therapy of stones. Trace elements and mineral metabolism.
Citation: Magro VM, Caturano M, Coppola C, Verrusio W (2019) Elderly Patient with Hematuria and Lithiasis: The Point of View of the Geriatrician through the Analysis of a Case Report. J Gerontol Geriatr Med 5: 031.
Copyright: © 2019 Valerio Massimo Magro, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

Journal Highlights
© 2026, Copyrights Herald Scholarly Open Access. All Rights Reserved!
