
Endoscopic Diagnosis of Mixed Parasitic Infestation as an Uncommon Cause of Iron Deficiency Anaemia
*Corresponding Author(s):
Ehab AbdelmalekThe Princess Alexandra Hospital, Harlow, England, United Kingdom
Tel:+447480637779,
Email:ehabadib@yahoo.com
Abstract
Iron deficiency anaemia (IDA) is confirmed by a low level of haemoglobin (Hb), low ferritin or iron level in addition to hypochromic microcytic blood picture. It is ideal to get a coeliac screen with either anti-tissue transglutaminase (Anti-tTG) or anti-endomysial antibodies along with serum immunoglobulin IgA.
Gastroscopy and colonoscopy are essential to investigate the upper and lower gastrointestinal tract. When colonoscopy is contraindicated, CT colonography is a sufficient alternative. However, CT colonography lacks the advantage of the detection of vascular malformations like angiodysplasia.
Direct visualization of the small bowel with either small bowel video capsule endoscopy or double-balloon endoscopy, is not necessary unless there is an inadequate response to iron therapy, or the patient becomes transfusion dependent.
Despite the aim of the endoscopic examination is to diagnose mucosal pathology, on rare occasions, it can detect an unexpected cause of GI blood loss like luminal parasites.
Keywords
Anaemia; Iron deficiency; Taenia species worm; Trichuris trichiura
INTRODUCTION
Anaemia affects 24.8% of the population worldwide, and roughly half of them have IDA [1] which is a common cause for referral to the gastroenterology clinic [2].
The main causes of iron deficiency are deficient dietary intake, iron malabsorption, and chronic blood loss that could be gastrointestinal (GI) or non-gastrointestinal.
CASE PRESENTATION
Subjective data
30-year-old young Ethiopian lady who works as a housemaid was referred from her GP because of iron deficiency anaemia with haemoglobin level 74g/L. There was a history of mild abdominal discomfort, otherwise, the patient denied a history of overt GI bleeding, dysphagia, recent change in bowel habit or weight loss. There was no record of bleeding from different body orifices such as epistaxis, haemoptysis, haematuria, menorrhagia or metrorrhagia. The patient did not report the use of non-steroidal anti-inflammatory medications (NSAIDs) or anticoagulants. The patient mentioned that she had been consuming red meat in her diet. Following a retrospective enquiry about her dietary habits, the patient was unable to give a clear history about the ingestion of raw or undercooked meat.
There was no past medical history of GI disorders, surgery or anaemia. No family history of coeliac disease, inflammatory bowel disease, polyposis syndromes, GI cancer, IDA or bleeding disorders were reported. She neither smokes nor drinks alcohol.
Objective data
The patient was pale, otherwise, a thorough physical examination was unremarkable.
Laboratory investigations
• Hypochromic microcytic anaemia, Hb 74g/L (normal value 115-165), MCV 68fl (normal value 76 – 96), MCH 20.8pg (normal value 27.0 - 32.0), Ferritin 17mcg/L (normal value 20 – 275), Iron 3.8umol/L (normal value 7.0 - 29.0), Transferrin saturation 6% (normal value 15-55).
• Vitamin B12 and folate were normal.
• Na+, K+, urea and creatinine were normal.
• Anti-tTG was negative and IgA was normal.
Endoscopic examination
Gastroscopy (Figure 1) was reported normal and CLO test was negative. Duodenal biopsies came back normal.
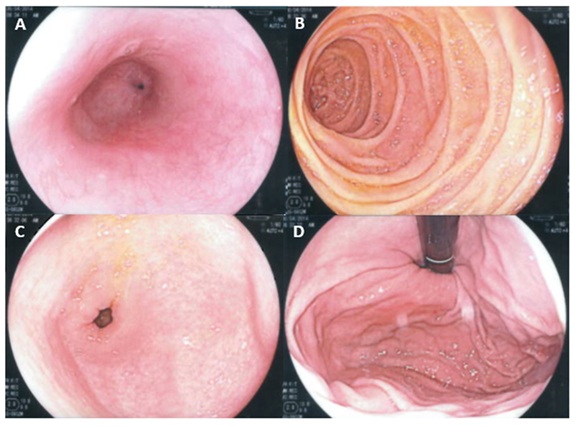 Figure 1: Gastroscopy images; A) Oesophagus, B) Gastric antrum, C) Duodenum second part, D) Gastric fundus.
Figure 1: Gastroscopy images; A) Oesophagus, B) Gastric antrum, C) Duodenum second part, D) Gastric fundus.
Colonoscopy (Figure 2) showed heavy parasitic infestation with two different types of worms, one of them looked like a flat ribbon and the other one was thin whip-like. With the use of the suction trap, a sample of the worms was collected and sent to the parasitology laboratory. The result came back as Taenia species (Figure 2A, 2B red arrow & 2C) worm and Trichuris trichiura (female worm) (Figure 2B blue arrow & 2D).
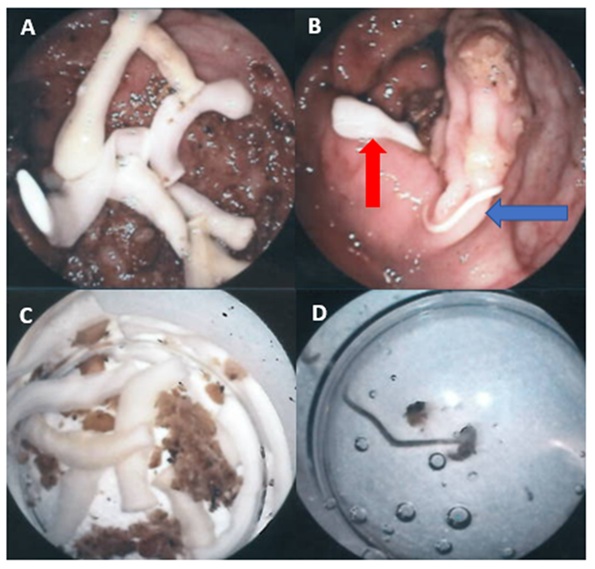 Figure 2: Colonoscopy images; A) Taenia worms, B) Taenia worms after sampling, C) Taenia worm (red arrow), Trichuris worm (blue arrow), D) Trichuris trichiura after sampling.
Figure 2: Colonoscopy images; A) Taenia worms, B) Taenia worms after sampling, C) Taenia worm (red arrow), Trichuris worm (blue arrow), D) Trichuris trichiura after sampling.
The patient was treated with a combination of praziquantel and ivermectin as advised by the tropical medicine consultant in addition to oral iron replacement. She was advised to avoid eating raw or undercooked meat in addition to maintain good personal hygiene and careful handwashing.
The patient was followed up in the clinic three months later, where she advised being generally well and did not report any complications or treatment side effects. Stool examination using concentration techniques did not reveal ova of parasites or proglottids of Taenia worm species.
A more recent blood test showed resolution of anaemia with Hb level 115g/L and Ferritin 24mcg/L. The patient was advised to continue oral iron for another three months.
CONCLUSION
Parasitic infestations are still an important cause of IDA particularly in people of low socioeconomic status, where faecal examination for parasites can be considered in the initial investigations of IDA.
Patients with IDA should have a serological screening for coeliac disease. In absence of an obvious cause for IDA (after excluding gynaecological causes in pre-menstrual women), all patients should have a gastroscopy with either colonoscopy or radiological imaging.
In some cases, the endoscopic examination can help to reveal rare causes of IDA like mixed parasitic infestation and allow sampling of the adult worms as in this patient.
REFERENCES
- World Health Organization (2008) Worldwide Prevalence of Anaemia 1993-2005. WHO.
- Goddard AF, James MW, McIntyre AS, Scott BB (2011) Guidelines for the management of iron deficiency anaemia. Gut 60: 1309-1316.
- Bouri S, Martin J (2018) Investigation of iron deficiency anaemia. Clin Med (Lond) 18: 242-244.
- Short MW, Domagalski JE (2013) Iron deficiency anemia: evaluation and management. Am Fam Physician 87: 98-104.
- Holmes G, Ciacci C (2018) The serological diagnosis of coeliac disease-a step forward. Gastroenterol Hepatol Bed Bench 11: 209-215.
- Stein J, Connor S, Virgin G, Ong DE, Pereyra L (2016) Anemia and iron deficiency in gastrointestinal and liver conditions. World J Gastroenterol 22: 7908-7925.
- A Gunn, S Pitt (2012) Parasitology: an Integrated Approach, Wiley-Blackwell, UK, pp. 105-108.
- Cooper E. Trichuriasis (2011) In: Tropical Infectious Diseases: Principles, Pathogens and Practice, 3rd edn, Guerrant R, Walker DH, Weller PF (Eds), Saunders Elsevier, Philadelphia, pp.791.
- Pezzoli A, Fusetti N, Pizzo E (2016) Capsule endoscopy diagnosis of intestinal Taenia. Gastrointest Endosc 83: 261.
Citation: Abdelmalek E (2020) Endoscopic Diagnosis of Mixed Parasitic Infestation as an Uncommon Cause of Iron Deficiency Anaemia. J Gastroenterol Hepatology Res 5: 028.
Copyright: © 2020 Ehab Abdelmalek, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

