
Endovascular Management of Supra Hepatic IVC Budd-Chiari Syndrome in a 12 year old Boy: Case Report
*Corresponding Author(s):
Salah MDepartment Of Vascular Surgery, Saudi German Hospital, Jeddah, Saudi Arabia
Tel:+966 546028705,
Email:msalahvs@hotmail.com
Abstract
Primary Budd-Chiari Syndrome (BCS) is a rare condition affecting one in a million adults, even more rare in children. It is a rare form of hepatic venous outpatient obstruction at the supra hepatic Inferior Vena Cava (IVC), the hepatic veins or both. As this syndrome is uncommon, especially in paediatric age group, misdiagnosis and delay in diagnosis are frequent. A high index of clinical suspicion along the radiological and histological correlation can lead to early diagnosis and appropriate management. The most common BCS symptom is ascites. Our case was a 12 year old Sudanese boy, suffering of manifestations of portal hypertension, ascites, and hepatosplenomegaly. He was treated by Angioplasty and Stenting of the supra hepatic IVC, with good outcome and improvement of symptoms. Published literature on interventional procedure for Budd-Chiari Syndrome in children and adolescents is scare. The management of such cases was not unified in all the reports. Percutaneous endovascular angioplasty and stenting of the suprahepatic IVC was ideal for this patient.
CASE PRESENTATION
Our patient is a 12 years old Sudanese boy, referred to our Centre, suffering of hepatosplenomegaly, no jaundice, no history of hematemesis. His Laboratory tests, liver functions, CBC, Serum Creatinine were all within normal limits. Serology was negative. Hypercoagulability status and auto immune disorders were also tested and proved negative.
Abdominal ultrasound showed marked hepatosplenomegaly. Otherwise no significant abnormality. CT Venography was done, confirmed the diagnosis and showed non opacification of intra hepatic or suprahepatic IVC and the diagnosis was put as IVC web (Figure 1).
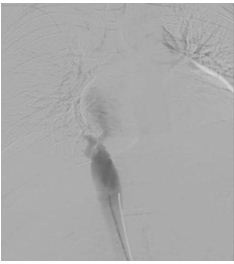 Figure 1: Direct Venography showing complete obstruction of intra or Suprahepatic IVC.
Figure 1: Direct Venography showing complete obstruction of intra or Suprahepatic IVC.
PATIENT MANAGEMENT
Plan of management was put to give the patient trial of Angioplasty and stenting of suprahepatic IVC. In the angio suite, under local anaesthesia, right femoral vein access and right internal jugular vein access were established. Although it was difficult crossing the IVC web from both sides, yet we managed to cross to cross the lesion. Ballooning of the lesion was done with recoil. Then a Venovo stent (Bard) 14 × 60 was inserted in the suprahepatic IVC landing at the junction of the right atrium with the IVC (Figure 2).
 Figure 2: Tight waist during Ballooning of the lesion IVC.
Figure 2: Tight waist during Ballooning of the lesion IVC.
Direct Venography post stenting of Patient passed smooth postoperative period. Postoperative CT and 3 months follow up CT showed patent retrohepatic IVC, patent IVC stent, also patent hepatic veins, patent portal vein and patent splenic web (Figure 3).
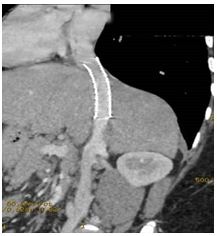 Figure 3: 3 months follow up CT Venography Showing patent IVC and patent stent.
Figure 3: 3 months follow up CT Venography Showing patent IVC and patent stent.
DISCUSSION
The Budd-Chiari Syndrome (BCS) is very rare in children compared to adults, and most authors mentioned an incident of about one case per million people per year in the general population of the world. Dulawri et al., [1], found that 177 cases of this syndrome, only 5% were found to be below 12 years of age. Hoffman HD et al., [2], reported the largest paediatric series of 9 cases with membranous obstruction of the IVC. The chronic changes after hepatic venous outflow obstruction includes centrilobular fibrosis within weeks, progressive fibrosis and cirrhosis may take months to appear. The classic triad of BCS is abdominal pain, ascites and hepatomegaly. Physical examination may show jaundice, ascites, hepatomegaly, splenomegaly and ankle edema. Harmanci et al., 2013 [3]. The most common cause in adults in thrombosis, secondary to an underlying hyperproliferative disease; and in children. The most common cause is a membranous obstruction of the inferior vena cava. Plassier et al., 2008 [4]. Liver function tests can be normal or increased. Ascitic fluid examination can provide useful clues to the diagnosis, including high protein concentration (> 3gm/dl) and serum ascites albumin concentration, gradient (> 1.1 gm/dl) are suggestive of BCS. Taksande et al., 2017 [5]. Doppler ultrasound, venography and liver biopsy have been very helpful in its diagnosis. CT venography shows the exact site of obstruction. Digital subtraction angiography is the gold standard for evaluation of the IVC and hepatic veins.
The classic management as reported by most authors, following the already established step wise strategy, medical therapy as the first step, angioplasty/stenting as the second step, Trans-Jugular Intrahepatic Portosystemic Shunt (TIPS) as the third step and the liver transplantation as the last step. Mancuso M. 2015 [6]. Recently, a new algorithm was suggested in which medical therapy is suggested only for patients without any sign of portal hypertension, while early interventional treatment (angioplasty/stenting) is suggested when either any symptom or sign of portal hypertension appears, with the aim of preventing liver impairment or failure. Mancuso M. 2015 [6].
CONCLUSION
Owing to the rarity of BCS in the Paediatric age group, a high index of clinical suspicion is required and the final diagnosis can be made by Liver Biopsy and CT Angiography. The flow chart management comes from expert opinion and is not evidence based. Angioplasty and stenting are recommended by most authors, which, we did for our case. Angioplasty and stenting was done successfully and safely for our patient, with good postoperative outcome and improvement as we felt it was the ideal way of management for such a case.
REFERENCES
- Dilarwari JB, Bambrey P. Chawla Y, Kaur U, Bhusnurmath SR, et al. (1994) The hepatic outflow obstruction (the Budd-Chiari syndrome). Medicine 43: 21-36.
- Hoffman HD, Stockland B, von der Heyden U (1987) Membranous obstruction of the inferior vena cava with Budd-Chiari syndrome in children: A report of nine cases. J Pediatr Gastroenterol Nutr 6: 878-884.
- Harmanci O, Kav T, Peynircioglu B, Buyukasik Y, Sokmensuer C, et al. (2013) Long-term follow-up study in Budd-Chiari syndrome: Single-center experience in 22 years. J Clin Gastroenterol 47: 706-712.
- Plessier A, Valla D (2008) Budd-Chiari syndrome. Semin Liver Dis 28: 250-269.
- Taksande A, Meshram R, Yadav P, Borkar S, Lokhare A, et al. (2017) A rare case of Budd-Chiari Syndrome in a Child. International Journal of Pediatrics 5: 5809-5812.
- Mancuso A (2015) An update on the management of Budd-Chiari syndrome: The issues of timing and choice of treatment. Eur J Gastroenterol Hepatol 27: 200-203.
Citation: Salah M, Hemeda S, Abogreda A, Sakr A, Elfarra Y (2019) Endovascular Management of Supra Hepatic IVC Budd-Chiari Syndrome in a 12 year old Boy: Case Report. J Surg Curr Trend Innov S1: 002.
Copyright: © 2019 Salah M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

