
Fillers and Vessels: The Story of Arterial Obstruction after Cosmetic Treatment
*Corresponding Author(s):
Velthuis PJSection Of Cosmetic Dermatology, Department Of Dermatology, Erasmus University Medical Center, Rotterdam, Netherlands
Tel:+31 104070110,
Email:peter@drvelthuis.nl; p.velthuis@erasmusmc.nl
Abstract
Most popular fillers in cosmetic medicine are hyaluronic acid based. These comprise over 90% of the market and come with the advantage to be soluble in case of complications. Other fillers are contained in the group of bio-stimulatory fillers. They exert a secondary volumizing effect by provoking a low-grade inflammatory response that produces extra collagen. Examples are calcium-hydroxyapatite and L-poly-lactid acid. Finally autologous fat is being used as a filling substance (lipofilling).
The gravest complications with fillers are intravascular injections. In particular when injected in arteries fillers can block blood flow and lead to skin necrosis or vison loss in case the material occludes the Central Retinal Artery (CRAO). Two opposing theories about the nature of arterial occlusion exist. One based on Ian Taylor idea of choke anastomoses assume vasoconstriction induced by the filler, both of the primary offended artery and its anastomosing vasosomes. In this case resolving the hyaluronic acid filler with the enzyme hyaluronidase at the primary occluding location would suffice. This is done under ultrasound guidance. The other theory assumes displacement of parts of the filler to end arterioles. Then, the whole affected area has to be flooded with large dosages of hyaluronidase. Obstructions with fillers based on other materials cannot be resolved.
It seems logical to prevent intra-arterial filler injection by duplex sonography detection of the course of arteries prior to injection. Ultrasound has additional advantages for cosmetic doctors such as recognizing remains of previously injected filler. It also can give feedback on a physician’s ability to inject filler in the correct subdermal location.
Fillers
Facial cosmetic treatments with subcutaneous fillers are increasingly popular. One of the most feared complications is vascular occlusion. This may lead to skin necrosis or permanent vision loss. The most important tool to detect an obstructed artery is duplex ultrasound. This imaging method may also aid in dissolving the causative filler material. Vascular ultrasound mapping prior to injection treatment may help prevent complications.
Together with botulinum toxin, filler injections have become the most frequently performed cosmetic medical treatments [1]. In numbers these have surpassed cosmetic surgery by far. With little or no downtime and smaller risks of complications they offer obvious advantages over surgery. In western countries two type of filling substance can be distinguished. Most popular are the hyaluronic acid fillers with a 90% market share. These exert a direct volumizing effect. Hyaluronic acid is a natural substance that occurs in many human tissues and organs. It has an important water-binding capacity and regulatory functions. It has a life span of hours to several days and is continuously synthesized by a various cell types [2]. The Hyaluronic Acid (HA) used in fillers is synthesized by genetically modified bacteria. It is a copy of the human material. To overcome the short life span of the molecules, these are chemically modified by means of internal cross-linking. This technology makes it also possible to renders fillers with different chemico-physical properties in term of rheology, cohesiveness and elasticity. This gives manufacturers the opportunity to deliver different HA filler types for each indications, being either superficial lines, rhytids or sunken cheeks [3]. HA fillers have the enormous advantage of a dissolving substance, the enzyme hyaluronidase.
Bio-stimulatory fillers pose the other group of fillers. These are intended to stimulate the body to form collagen. This process is part of a low grade inflammatory response. These filler are insoluble and need a carrier to deliver them from the syringe, through a needle into the tissue. Once inside the tissue these substances are broken down in several months [3]. Non-resorbable fillers consisting of moldable plastics form a third group of fillers. They stay permanently inside the tissue. The use of these has been banned in many countries. Another substance implicated in vascular occlusion is autologous fat. Fat transfer (also named lipofilling) is used for many kinds of bodily defect. The main cosmetic indications are facial defects in volume, small breast and buttocks. In particular the latter one has been implicated in a number of fatal embolisms [4].
In two surveys regarding vision loss after filler injection Beleznay, et al. noted that all types of fillers were implicated [5,6]. It is plausible that this group of materials is identical to the causative agents in occlusion of major facial arteries.
Vessels
Arteries in the face primarily stem from the External Carotid Artery (ECA). In the lower and middle part of the face it is the facial artery branching from the ECA in the neck that crosses the mandibular bone ventrally and delivers branches to lower and upper lip before its course cranially alongside the nose to the forehead, with a name-change to angular artery. In the lateral middle part of the face the transverse facial artery branches from the ECA just caudal to the zygomatic bone and courses medially. Arterial supply for the lateral upper face stems from the superficial temporal artery, that in the parietal region bifurcates medially becoming the frontal branch that runs medially to the forehead. A large part of the mid-forehead receives its blood supply from branches of the ophthalmic artery, in particular the supra-orbital and supratrochlear artery.
Some of the arterial supply in the lower and midface may stems from the maxillary artery who gives off branches named the mental artery (entering the chin area through mental foramen) and the infraorbital artery(entering the midface area through the infraorbital foramen). These arteries anastomose with branches of the facial artery. The most important and most dangerous anastomoses with regard of vision loss are those between facial (angular) and ophthalmic artery. There are also small interconnection between the intra-orbital / infra-trochlear arteries and the facial (angular) artery. These have proven to be the major sources of the central retinal artery occlusion.
Arterial Occlusion
Vascular occlusion in the face after filler injection leads to the so-called Nicolau syndrome. By and large it is a clinical diagnosis consisting of skin blanching, reticular bluish erythema, and slow capillary refill as immediate symptoms, followed a few days later by pustules and finally crusts with subsequent atrophic scars. Complete skin necrosis may appear in severe cases. The initial symptoms are immediate and accompanied by pain and edema [7].
In the first 1-2 days after occlusion an artery with increased lumen is seen on duplex ultrasound. At days 2 and later, rays of collateral arteries surrounding the obstructed vessel become visible. This is a very specific pattern that we tentatively named Medusa Head. On sonography hyaluronic acid filler is depicted as an anechoic pocket. It is impossible to determine whether the filler is actually inside a vessel. Since there are usually more than one filler deposits, we customary inject all HA filler deposits around the occluded artery with hyaluronidase (usually 50-100 units in total). This is best done under ultrasound guidance. In most cases we observe restore of blood flow within minutes (Figure 1). It is important to realize that the occluded arteries are found at the borders or sometimes even outside the clinically affected area [8]. 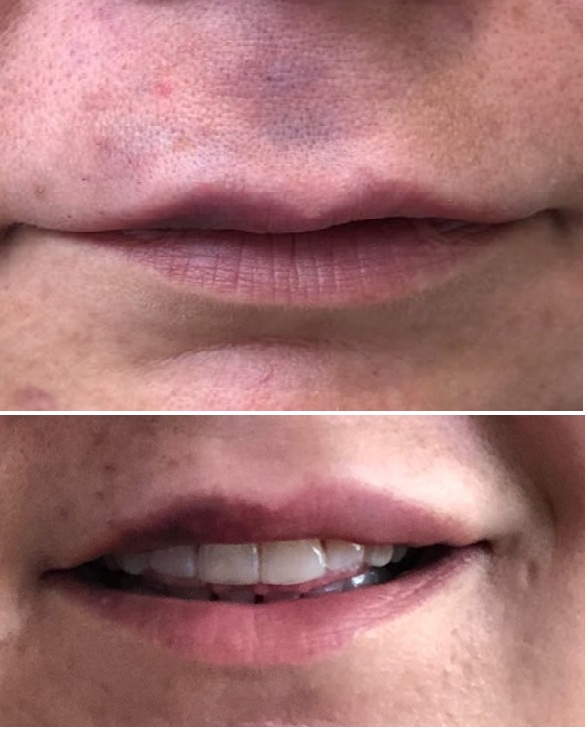
Figure 1: A case of obstruction of superior labial and columellar artery. Above 1 day after hyaluronic filler injection. Below 1 day after hyaluronidase injection in the filler pockets under ultrasound guidance.
There is some discussion about this approach. Many scholars do not accept that large facial arteries can be occluded. Should that be the case, anastomoses and collateral vessels will take over the blood supply in their opinion. They feel that the clinical picture is provoked by smaller elements of the filler substance coming loose, traveling to end-arterioles of the skin and eventually blocking oxygen transfer in capillaries. Alternative to our approach they flood the clinically affected area superficially and deep with large doses of hyaluronidase (usually 1500-3000 units) [9].
In our clinic, however, we follow the hypothesis of Ian Taylor’s group, that after contact with the filler vasoconstriction of the artery occurs. Concurrently choke anastomoses will prevent arterial blood to flow from bordering vasosomes into to (Remove to) the affected skin. Indeed HA filler has proved to be an irritant for the endothelium and may induce vasoconstriction [10]. Also it seems improbable that part of the filler substance will come loose, since the filler itself is designed to be very cohesive.
Recently we published 42 cases of Vascular Adverse Events (VAE) in the face referred to us in 22 months [8]. The locations and arteries implicated are given in table 1. In another study we calculated the incidence of these vascular adverse events to be 1:6600 [11]. Thus, a regular cosmetic doctor performing 1500-2000 treatment/year, will meet a VAE every 3-4 years. Restore of blood flow within two days is generally thought to be sufficient to prevent tissue from becoming necrotic.
|
Arteryinvolved |
N. of Cases |
|
Submental |
7 |
|
Inferiorlabial |
7 |
|
Facial + Superior Labial |
1 |
|
Superior Labial + Columellar |
6 |
|
Superior Labial |
3 |
|
Columellar |
2 |
|
Angular |
5 |
|
Dorsalnasal |
3 |
|
Transverse Facial |
1 |
|
Infraorbital |
1 |
|
Frontal Branch External Carotid |
3 |
|
Zygomatico-Orbital |
1 |
|
Supratrochlear |
2 |
|
Supraorbital |
2 |
|
Total |
44 |
Table 1: occluded arteries by fillers in 44 consecutive cases 2018-2020 [11].
It is questionable whether fillers can block arterial blood flow by compression. The general opinion is that this may only happen in the tight skin on the tip of the nose. However we have recently seen a case of temporary hair loss after filler injections that we believe resulted from filler placement between fascial sheets in the temple (van der Elzen et al. submitted). Some doctors hold the opinion that obstruction of venous vessels can cause a delayed blockage of the vascular system. This may account for cases sometimes seen where the symptoms do not appear ‘on the needle’, but several hours later. We fail to see the mechanism of this.
Vision loss is a very grave and feared complication in facial filler treatments. This is caused by fillers injected in arteries that anastomose with branches of the ophthalmic arteries [12]. In particular the nose and glabella regions are implicated. In those cases the filler supposedly travels in the direction opposing the blood flow. The extrusion force of the filling substance must be high enough to counteract the pressure of the blood flow in the ophthalmic artery. Another hypothesis may of course be the Taylor notion of provoked vasoconstriction [13]. Occlusion of the CRA leads to intense pain in the eye and immediate loss of vision. There is debate about how much time there is before vision loss is irreversible. Since retinal tissue must be regarded as an extension of the brain with its susceptibility for anoxia, it is generally believed there is very limited time for action, perhaps 30-90 minutes. Only in case of CRA occlusion by hyaluronic acid filler there is a potential way to dissolve the filler. For other filler types there is no antidote. Unfortunately, the best way to act is unclear. Retrobulbar injections of large and repeated dosages of hyaluronidase (H-ase) have long been the standard of care. However, the initial idea that H-ase was able to diffuse through the CRA arterial wall and dissolve the filler, has recently been doubted. Alternatively, canulation of the supratrochlear of supraorbital artery and direct intravascular infusion of the H-ase, can be tried [14].
Clearly more work has to be done to elucidate the pathophysiology of vascular adverse events and the best forms of action.
Prevention
Several experiments have made clear that simple aspiration before injecting fillers is not enough to prevent intra-arterial injection [15]. Therefore, it seems logical to perform prior ultrasound scanning of an area to identify vascular anomalies, in particular in case of nasal or glabellar injections. After nasal surgery arteries (Remove arteries) the main arterial blood supply of upper lip and adjacent areas may run an alternative course. Given the low incidence of VAE it will be very difficult to prove the beneficial effects of such an approach. Yet, duplex sonography is a very simple, non-invasive method that is completed in a few minutes [16]. As doctors, we owe it to our patients to do the utmost to prevent any harm being done.
Conflicts of Interests
Drs. Velthuis and Schelke are trainers in Cutaneous.
References
- ISAPS (2019) Isaps International Survey On. ISAPS.
- Abatangelo G, Vindigni V, Avruscio G, Pandis L, Brun P (2020) Hyaluronic Acid: Redefining Its Role. Cells 9: 1743.
- Herrmann JL, Hoffmann RK, Ward CE, Schulman JM, Grekin RC (2018) Biochemistry, Physiology, and Tissue Interactions of Contemporary Biodegradable Injectable Dermal Fillers. Dermatol Surg 1: 19-31.
- Oranges CM, Tremp M, di Summa PG, Haug M, Kalbermatten DF, et al. (2017) Gluteal Augmentation Techniques: A Comprehensive Literature Review. Aesthet Surg J 37: 560-569.
- Beleznay K, Carruthers JD, Humphrey S, Jones D (2015) Avoiding and Treating Blindness From Fillers: A Review of the World Literature. Dermatol Surg 41: 1097-117.
- Beleznay K, Carruthers JDA, Humphrey S, Carruthers A, Jones D (2019) Update on Avoiding and Treating Blindness From Fillers: A Recent Review of the World Literature. Aesthet Surg J 39: 662-674.
- Sito G, Manzoni V, Sommariva R (2019) Vascular Complications after Facial Filler Injection: A Literature Review and Meta-analysis. J Clin Aesthet Dermatol 12: 65-72.
- Schelke LW, Velthuis P, Kadouch J, Swift A (2019) Early ultrasound for diagnosis and treatment of vascular adverse events with hyaluronic acid fillers. J Am Acad Dermatol 0190-9622: 32392-32398.
- DeLorenzi C (2017) New High Dose Pulsed Hyaluronidase Protocol for Hyaluronic Acid Filler Vascular Adverse Events. Aesthet Surg J 37: 814-825.
- Ashton MW, Taylor GI, Corlett RJ (2018) The Role of Anastomotic Vessels in Controlling Tissue Viability and Defining Tissue Necrosis with Special Reference to Complications following Injection of Hyaluronic Acid Fillers. Plast Reconstr Surg 141: 818-830.
- Schelke L, Decates T, Kadouch J, Velthuis P (2020) Incidence of Vascular Obstruction After Filler Injections. Aesthet Surg J 40: 457-460.
- Kapoor KM, Kapoor P, Heydenrych I, Bertossi D (2020) Vision Loss Associated with Hyaluronic Acid Fillers: A Systematic Review of Literature. Aesthetic Plast Surg. 44: 929-944
- Taylor GI, Shoukath S, Gascoigne A, Corlett RJ, Ashton MW (2020) The Functional Anatomy of the Ophthalmic Angiosome and Its Implications in Blindness as a Complication of Cosmetic Facial Filler Procedures. Plast Reconstr Surg 146: 745.
- Zhu GZ, Sun ZS, Liao WX, Cai B, Chen CL, et al. (2017) Efficacy of Retrobulbar Hyaluronidase Injection for Vision Loss Resulting from Hyaluronic Acid Filler Embolization. Aesthet Surg J 38: 12-22.
- Kapoor KM, Murthy R, Hart SLA, Cattin TA, Nola PF, et a. (2021) Factors influencing pre-injection aspiration for hyaluronic acid fillers: A systematic literature review and meta-analysis. Dermatol Ther. 34: 14360.
- Velthuis PJ, Jansen O, Schelke LW, Moon HJ, Kadouch J, et al. (2021) A Guide to Doppler Ultrasound Analysis of the Face in Cosmetic Medicine. Part 2: Vascular Mapping. Aesthet Surg J.
Citation: Velthuis PJ, Schelke LW (2021) Fillers and Vessels: The Story of Arterial Obstruction after Cosmetic Treatment. J Angiol Vasc Surg 6: 069.
Copyright: © 2021 Velthuis PJ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

