
General Teaching Hospital “Enrique Cabrera”. Teaching Department of Surgery
*Corresponding Author(s):
Pedro López RodríguezHospital General Docente Enrique Cabrera, University Of Medical Sciences Of Havana, Cuba
Tel:+53 76413062,
Email:lopezp@infomed.sld.cu, pedro.rolando.lopez42@gmail.com
Abstract
Summary
Various techniques have been developed for the repair of femoral hernia. The technique with the Lichtenstein Plug since 1989 has allowed to obtain a lower rate of complications and recurrences, as well as an early recovery of the patients usual activities. Its application, widely spread in elective surgery, can also be performed in emergency surgery. The aim of this work is to review the experience of our basic group of work in the surgical treatment of femoral hernia using this technique.
Methods
A retrospective descriptive observational study was conducted in our basic work group from the surgery service of the General Teaching Hospital “Enrique Cabrera” between 2009 and 2018, to which this surgical technique was applied. We study the anatomical variants of hernias as well as post-operative complications and clinical evolution.
Results
The mean age of the patients was 58.7 years (19-92 years), being the female with the highest incidence 78%, as well as, the most frequent location the right, 67.5%. The prosthesis used in the hernioplasty was that of polypropylene. Local anesthesia was applied to 29 patients (63%) of them. The average surgical time was 25 minutes, (15-65 minutes). Ambulation was early and the average hospital stay was lessthan 24 hours, in most patients. Only one infection of the wound and one hernia recurrence in one patient was confirmed.
Conclusion
Therefore, we believe that the Lichtenstein Plug technique should be considered among the techniques of choice in the treatment of femoral hernia.
Keywords
INTRODUCTION
METHODS
RESULTS
|
|
Number of Patients |
Percentage % |
|
Men |
10 |
22, 0 |
|
Women |
16 |
78, 0 |
|
Right |
31 |
67, 5 |
|
Left |
15 |
32, 5 |
|
Recidiva |
1 |
2, 2 |
|
Primary |
45 |
97, 8 |
|
Middle Ages |
58,7 Years |
( Range 19-92 ) |
|
Type of Anesthesia |
Number of Patients |
Percentage % |
|
Local |
29 |
63,0 |
|
Regional |
12 |
26,2 |
|
General |
5 |
10,8 |
|
Average Duration |
25 Minutes |
(Range 15-65) |
|
Hospital Media Stay |
8 |
(Range 6-48) |
The only recurrences observed in our series were in a patient who was operated on because of a relapsed, incarcerated hernia. In the surgical act a wide femoral orifice was observed that was occluded with a cylinder of polypropylene mesh like all the other patients. In the postoperative period he presented wound infection and recurrence at four months. In the reoperation, it was found that the cylindrical prosthesis was of insufficient size to occlude the femoral orifice. This patient underwent a pre-peritoneal repair with a wide patch of polypropylene mesh.
DISCUSSION
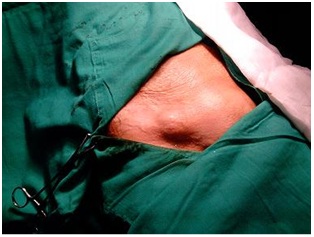
Figure 1: Patients with right femoral hernia.
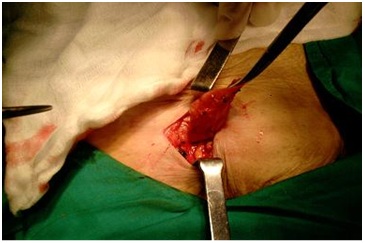
Figure 2: Hernia sac dissected through the dilated femoral orifice.
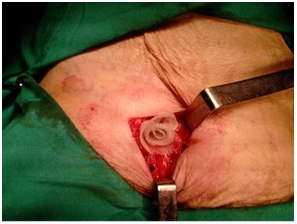
Figure 3: Occlusion of the femoral ring with a polypropylene cylindrical prosthesis.
CONCLUSION
REFERENCES
- Lichtenstein IL, Shore JM (1974) Simplified repair of femoral and recurrent inguinal hernias by a “plug” technic. Am J Surg 128: 439-444.
- Nicholson S, Keane TE, Devlin HB (1990) Femoral hernia: an avoidable source of surgical mortality. Br J Surg 77: 307-308.
- Bendavid R (1989) New techniques in hernia repair. World J Surg 13: 522-531.
- Lichtenstein IL (1987) Herniorrhaphy. A personal experience with 6,321 cases. Am J Surg 153: 553-559.
- Gilbert AI (1992) Sutureless repair of inguinal hernia. Am J Surg 163: 331-334.
- Robbins AW, Rutkow IM (1998) Mesh plug repair and groin hernia surgery. Surg Clin North Am 78: 1007-1023.
- Lichtenstein IL, Shulman AG, Amid PK (1990) Use of mesh to prevent recurrence of hernias. Postgrad Med 87: 155-158.
- Mansilla Molina D, Perez Folques JE, Civera Muñoz J, Vazquez Ruiz J, Polo Perez MI, et al. (1999) Hernioplasty without tension in crural hernias. Cir Esp 65: 176-178.
- Cobaleda FSB, Muñoz-Najar AG, Trujillo BM, Borajo MC, Matas FA, et al. (2000) Recurrent inguinal hernia: treatment using a preperitoneal approach and a wide polypropylene mesh prosthesis. Cir Esp 67: 354-357.
- Porrero JL, Ten M, Martín D, Lomar M (1993) Experience with the LUG tenstein PLUG technique in the treatment of Crural Hernia. Cir Esp 53: 97-99.
- Chamary VL (1993) Femoral hernia: intestinal obstruction is an unrecognized source of morbidity and mortality. Br J Sur 80: 230-232.
- Porrero JL, Sánchez-Cabezudo C, Bonachía O, López-Buenadicha A, Sanjuánbenito A, et al. (2005) [Inguinofemoral hernia: multicenter study of surgical techniques]. Cir Esp 78: 45-49.
- Rafael RF, Fernandez EIM, Rabassa PPC, Curbelo ONM, Weinman ESE (2003) Uso de Bioprótesis en las hernias inguinocrurales complicadas. Rev Cubana Cir 42: 1-7.
- de Juan A, Mena A, Die J, Rodríguez G, Sanjuanbenito A, et al. (2003) Is the Lichtenstein Plug technique suitable for the treatment of complicated crural hernia? Spanish Surgery 74: 104-107.
- Acevedo A, Reyes E, Herrera JC (2005) Femoral hernia: study of the posterior wall of the Inguinal Canal. Reuchi Cir 57: 495-499.
- Townsend CM, Beauchamp RD, Evers BM, Mattox KL, et al. (2007) Sabiston text Book of Surgery. 18th ed. Saunders Elservier, USA.
- Lòpez Rodriguez PR, Leòn Gonzàlez OC, Satorre Rocha J, Pol Herrera P, Garcia Castillo E (2012) Femoral Hernia. Ten years of experience in using the Lichtenstein Plug Technique. Rev Cuban Cir 51: 211-216.
- Townsend CM, Beanchamp RD, Evers BM, Mattox KL (2017) Sabiston Texbook of Surgery. 20th ed. Elsevier Saunders, USA.
- 19. Lockhart K, Dunn D, Teo S, Ng Jy, Dhillon M, et al (2018) Mesh versus non-mesh for inguinal and femoral hernia repair. Cochrane Database Syst Rev 9: CD 011517.
Citation: Rodríguez PL, Herrera PGP, Rocha JS, González OL, Fundora LMD, et al. (2019) General Teaching Hospital “Enrique Cabrera”. Teaching Department of Surgery. J Med Stud Res 2: 009.
Copyright: © 2019 Pedro López Rodríguez, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

