
Giant Mediastinal Schwannoma: Is a Hybrid Approach the New Mandatory Checkpoint?
*Corresponding Author(s):
Christina PopovicDepartment Of Cardiothoracic Surgery, Princess Alexandra Hospital, Brisbane, Queensland, Australia
Tel:+61 7 3176 2111,
Email:popovicchristina@gmail.com
Abstract
We present the case of a 53 year-old female with a giant mediastinal schwannoma and neovascularisation from the aorta and intercostal arteries. Given her risk of intraoperative bleeding complications, elective preoperative angiography and embolization was performed in order to minimise intraoperative blood loss from the mass and associated vasculature. This resulted in improved operative visibility, as well as faster recovery and freedom from blood transfusion post-operatively. To our knowledge this is the first reported patient with a Schwannoma to undergo pre-operative angiography and planned embolization for the purpose of minimising intraoperative blood loss.
Keywords
Angiography; Embolization; Mediastinum; Schwannoma
INTRODUCTION
Schwannomas are the most common neurogenic tumour of the posterior mediastinum. Although usually benign and incidentally diagnosed, increasing size can cause physiologic compromise. Thus, complete surgical resection is recommended.
It has been well-described in the medical literature, that patients with giant mediastinal schwannomas often present with well-circumscribed, neovascularised masses. Severe bleeding has been reported on presentation as well as intra-operatively [1,2], leading to hypovolemia, cardiac arrest, abandoned procedures, blood transfusions and increased morbidity [3]. With the increasing use of percutaneous angioembolisation interventions, a hybrid approach to haemostasis was planned to minimise complications and improve outcomes.
CASE REPORT
A 53-year-old female presented with new dyspnoea, orthopnoea, increasing peripheral oedema and hypoxia leading to type 2 respiratory failure. This was on a background of progressive dyspnoea for one month. On further history, new mid-thoracic ‘electric’ pains were reported along with small volume rusty haemoptysis noted the preceding week. She had a known left thoracic Schwannoma diagnosed sixteen years prior on core biopsy. Last surveillance CT three years prior was reported as stable. She was never referred for surgical resection. She had no clinical signs of neurofibromatosis.
A CT Pulmonary Angiogram demonstrated a 100x88x69 millimeter soft tissue mass in the left hemithorax with associated atelectasis and a large pleural effusion. An intercostal catheter subsequently drained over a liter of haemorrhagic fluid, which was negative for malignancy and infection on cytology and microscopy (Figure 1).
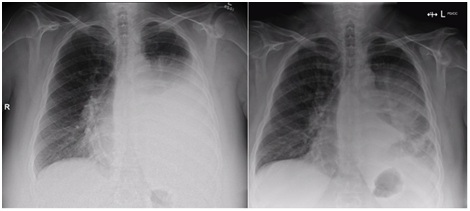 Figure 1: Presentation chest X-ray (left) demonstrating large pleural effusion prior to drainage and subsequent chest X-ray following intercostal catheter insertion.
Figure 1: Presentation chest X-ray (left) demonstrating large pleural effusion prior to drainage and subsequent chest X-ray following intercostal catheter insertion.
An MRI Chest demonstrated a heterogenous appearance most likely consistent with ancient change, although malignant transformation was not excluded. Multiple new enhancing mediastinal and retrocrural foci were indicative of further slowly progressive nerve sheath lesions. A repeat biopsy confirmed benign schwannoma.
A dedicated CT angiogram demonstrated multi-level intercostal arterial vascular supply. The mass displaced the left hilar vessels anteriorly with compressive atelectasis of the posterior left upper and lower lobes, and there was concern for inadequate surgical access for haemostasis (Figure 2).
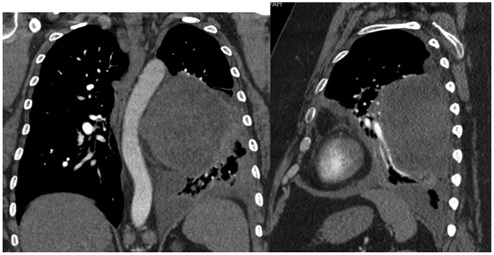 Figure 2: Coronal and sagittal sections of the posterior mediastinal mass, with adjacent atelectasis. CT Angiogram demonstrating mass with deviation of aorta, and vascular supply.
Figure 2: Coronal and sagittal sections of the posterior mediastinal mass, with adjacent atelectasis. CT Angiogram demonstrating mass with deviation of aorta, and vascular supply.
Due to the risk of haemorrhage and difficulty mobilising such a large fixed mass, formal angiography and embolization was requested to coil feeding vessels. This demonstrated arterial supply to the Schwannoma from the left T6 and T7 intercostal arteries, which were then selectively embolised without complication (Figure 3).
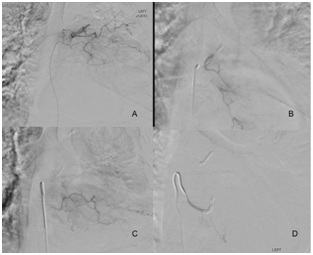 Figure 3: (A) Angiography demonstrating intercostal arterial supply to Schwannoma at level T6, (B) Subsequent angiogram following the interval embolisation coil placed in T6 intercostal artery, (C) Angiography of T7 intercostal artery with feeding vessels to Schwannoma, (D) Angiography following angioembolisation of T7 intercostal artery with no demonstrated vascular supply to Schwannoma.
Figure 3: (A) Angiography demonstrating intercostal arterial supply to Schwannoma at level T6, (B) Subsequent angiogram following the interval embolisation coil placed in T6 intercostal artery, (C) Angiography of T7 intercostal artery with feeding vessels to Schwannoma, (D) Angiography following angioembolisation of T7 intercostal artery with no demonstrated vascular supply to Schwannoma.
The patient then underwent a left posterolateral thoracotomy and resection. Findings included a large solid, grey, well-encapsulated mass with further nutrient vessels from intercostal arteries and the aorta. Due to the bulky nature of the tumour and adherence to surrounding structures, surrounding vessel ligation and mobilisation was eventually achieved with great difficulty, including tumour debulking and posterior rib dislocation. Two smaller masses were also resected. Exhaustive decortication was then performed for long-term haemorrhagic lung consolidation and compression, with excellent lung re-inflation.
Histopathology confirmed benign Schwannoma. The patient had no post-operative complications and did not require a blood transfusion. She was discharged home after eleven days. Her symptoms resolved and she was recurrence-free on CT surveillance at 12 month follow-up.
DISCUSSION
Mediastinal tumors are the most common cause of a posterior mediastinal mass [4]. They develop from mediastinal peripheral nerves, sympathetic and parasympathetic ganglia, and embryonic neural tube remnants [5].
Only recently has the use of elective pre-operative angiography and embolization been increasingly reported with the more routine use of interventional angiography. Historically, most of these procedures have been to delineate spinal vascular supply by identifying the artery of Adamkiewicz or to investigate potential neuroforaminal involvement, often in conjunction with a neurosurgical consultation and combined approach. It has become common practice to consider spinal angiography if the tumor is located near the site of the Adamkiewicz artery [3].
Bleeding complications have been well-described for giant schwannomas, as incidental findings leading to diagnosis as well as intra-operative complications [1,2]. This has lead to VATS conversion to thoracotomy, increased morbidity or abandoned procedures due to blood loss [3,6]. Others also report debulking without complete resection due to poor exposure from ongoing nutrient vessel bleeding [7].
There has been increasing suggestion that a certain subset of patients would benefit from elective pre-operative angioembolization of large mediastinal tumors, however no indications or guidelines are defined. Surgical excision usually confers excellent survival and recurrence is uncommon, however without complete resection of the tumour, risk of recurrence is increased [8]. Therefore, all attempts should be made to achieve complete excision, including hybrid haemostasis.
CONCLUSION
We present the case of successful elective preoperative angioembolization and subsequent uncomplicated resection of a giant posterior mediastinal mass. We suggest that pre-operative angiography +/- embolization should be considered in patients with a large mediastinal mass where concerns arise for major intraoperative blood loss due to vascular anatomy, difficulties with thoracic access and where completeness of tumour excision may be compromised by these factors.
FUNDING/CONFLICTS OF INTEREST
None.
REFERENCES
- Jang, JY, Kim JS, Choe JW, Kim MK, Jung JW, et al. (2013) A Case of Giant, Benign Schwannoma Associated with Total Lung Collapse by Bloody Effusion. Tuberc Respir Dis (Seoul)75: 71-74.
- Kato M, Shiota S, Shiga K, Takagi H, Mori H, et al. (2011) Benign giant mediastinal schwannoma presenting as cardiac tamponade in a woman: a case report. J Med Case Rep 5: 61.
- Madariaga ML, Borges LF, Rabinov JD, Chang DC, Lanuti M, et al. (2018) Angiography Before Posterior Mediastinal Tumor Resection: Selection Criteria and Patient Outcomes. Ann Thorac Surg 105: 1000-1007.
- Strollo DC, Rosado-de-Christenson ML, Jett JR (1997) Primary mediastinal tumors: Part II. Tumors of the middle and posterior mediastinum. Chest 112: 1344-1357.
- Marchevsky AM (1999) Mediastinal tumors of peripheral nervous system origin. Semin Diagn Pathol 16: 65-78
- Ciriaco P, Negri G, Bandiera A, Casiraghi M, Ferla L, et al. (2006) Videothoracoscopic Resection of Benign Neurogenic Tumors of the Posterior Mediastinum. Innovations (Phila) 1: 332-334.
- Wu Y, Zhang J, Chai Y (2016) Giant mediastinal schwannoma located in the lower right side of the chest. Nigerian Journal of Clinical Practice 19: 678-680.
- Quarteya B, Lenertb J, Deb SJ, Henrye LR (2011) Giant posterior mediastinal ancient schwannoma requiring thoracoabdominal resection: A case report and literature review. World J Oncol 2: 181-184.
Citation: Popovic C, Ura M (2019) Giant Mediastinal Schwannoma: Is a Hybrid Approach the New Mandatory Checkpoint? Archiv Surg S Educ 1: 003.
Copyright: © 2019 Christina Popovic, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

