
Haemolacria Associated with Severe Attacks of Migraine with Visual Aura and Hypertension
*Corresponding Author(s):
Reid JMDepartment Of Neurology, University Of Aberdeen, Scotland, United Kingdom
Tel:+44 1224554922,
Fax:+44 1224551188
Email:john.reid.2@nhs.sco
Abstract
Background: Haemolacria is a rare condition not previously associated with migraine with aura. We report the first such case and speculate as to a possible cause.
Case: A 47 year old lady presented with repeated attacks of migraine with visual aura, ipsilateral sensory symptoms, and at times associated with ipsilateral haemolacria and significantly raised blood pressure. Neurological, ENT and ophthalmological assessments were unremarkable. MRI brain scan and laboratory investigations were normal. The haemolacria episodes recurredon removal of prophylaxis.
Conclusion: This is the first reported case of haemolacria associated with migraine with aura. We speculate it has an autonomic basis and is also linked to hypertension.
Keywords
Autonomic features; Haemolacria; Migraine
INTRODUCTION
Haemolacria, meaning bloody tears, is a rare phenomenon of varied aetiology. It can be unilateral or bilateral and has been linked to conditions including bacterial conjunctivitis, lacrimal sac tumours and retrograde epistaxis [1,2]. It can be idiopathic or be present as part of a dissociative disorder [3].
We report an unusual case of a lady with migraine with visual aura who developed haemolacria ipsilateral to the most severe attacks of headache, often with elevated blood pressure. To our knowledge this has not been previously reported in migraineurs with aura. We speculate that this may be linked to cranial autonomic symptoms present in 46-56% of patients with migraine [4].
CASE PRESENTATION
A 47-year-old lady first presented to local Emergency department 9 years ago with left sided haemolacria on a background of a severe migraine attack (Figure 1a). Since then the patient experienced 8 further episodes of haemolacria always associated with a severe attack of migraine with visual aura.
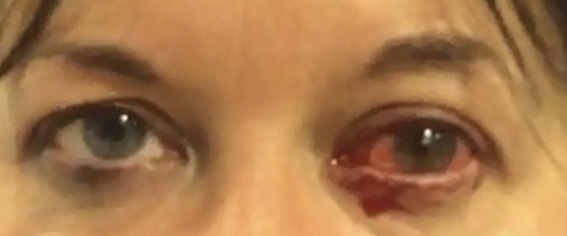 Figure 1: Photograph taken during acute attacks demonstrating left 1(a) and right sided haemolacria
Figure 1: Photograph taken during acute attacks demonstrating left 1(a) and right sided haemolacria
The patient’s migraine attack typically starts with a prodrome of feeling tired with a cold sensation on left side of the head prior to developing thumping headache. She can develop nausea and prefers to lie in a dark room. She can develop purple or green flashing lights in her vision for 5 min. Her left eye can swell up, injected, with no rhinorrhoea. She can develop associated weakness and tingling in the left arm and leg. The headache lasts 1-3 days followed bycognitiveblunting. Triggers for attacks include stress, flashing or bright lights, and missing meals. The most severe migraine attacks with visual aura and left sided tingling were associated with ipsilateral haemolacria. The patient describes “a pop”sensation in her eye beforehand and produces about a teaspoonful of blood during eachepisode. Each of these episodes occurred during an extremely stressful time in her life during, and her blood pressure could be significantly elevated, occasionally as high as 230/130mm Hg, as recorded by a wrist monitor at home.The patient experienced eight attacks of left sided of haemolacria to date. Seven years after the first episode, she developed an attack with right sided haemolacria (Figure 1b). Initially she found the bleeding quite distressing but now just sleeps it off.
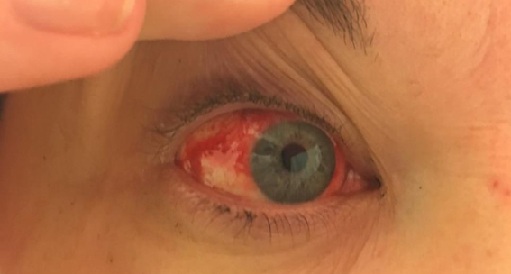 Figure 1(b): Occurring 7 years after first presentation.
Figure 1(b): Occurring 7 years after first presentation.
Past medical history includes hypertension, reactive depression and endometrial ablation. She has never smoked and drinks minimal alcohol.
For acute migraine the patient takes Migraleve and Naratriptan with a partial response. Prophylactics tried included Propranolol 40 mg twice daily and Pizotifen 1.5 mg at night, which was stopped due to weight gain. A switch to Topiramate increased to 75 mg twice daily reduced migraine frequency and caused some weight loss. A left greater occipital nerve blockade had partial success to reduce attack frequency. Following a period of remission she tried reducing Topiramate, which resulted in an exacerbation of her headaches and led to further episodes of haemolacria associated with significantly elevated blood pressure. Consequently, Topiramate was restarted. Atenolol 25 mg was added but caused lethargy and was stopped. Candesartan was initiated for blood pressure and migraine prophylaxis. Currently her migraines are well controlled whilst taking Candesartan 16mg once daily, Indapamide 2.5mg once daily and Naratriptan 2.5mg as required.
CLINICAL EXAMINATION AND INVESTIGATIONS
The neurological examination was unremarkable. A medical Ophthalmologist found no significant Ophthalmological problem to cause haemolacria, including no eyelid or conjunctival abnormality. The patient did not consent to ‘lacrimal probing’. Nasendoscospy by an Ear, Nose and Throat specialist found no abnormality.
CT scan of the paranasal sinuses was normal. The nasal septum was in the mid-line with normal calibre inferior turbinates. MRI brain scan was normal. Blood tests (thyroid function tests, prolactin, glucose, full blood count, clotting profile) and 24-hour urinary catecholamines were normal. Following a hypertension clinic appointment, a 24-hour ambulatory blood pressure monitor revealed daytime average blood pressure of 138/96mmHg and 126/81mmHg overnight, and antihypertensive medications were adjusted.
DISCUSSION
Haemolacria is a rare condition perplexing many clinicians due to its varied and often unknown aetiology. Haemolacria (literally bloody tears) can present as an isolated focal symptom or a part of a more generalized condition. A study from China found that the majority of cases were uniocular and occurred in females over 18 years old, with local lesions being the most common cause [5]. In contrast, four cases of children with unilateral haemolacria were documented to be idiopathic and self-limiting [6].
Causes of haemolacria include trauma, tumours of the lacrimal sac or paranasal sinuses, hereditary haemorrhagic telangiectasia, Henoch-Schonlein Purpura, epistaxis with retrograde flow, vascular malformations, inherited or acquired bleeding disorders and dissociative disorders [1,3]. One study found evidence of haemolacria being more common in women during the first week of menstruation, suggesting a hormonal link [7]. Epistaxis secondary to uncontrolled hypertension was linked to haemolacria in a different case thought to be due to retrograde flow through the nasolacrimal duct [2]. Finally, vertebral artery dissection associated with bilateral haemolacria and migraine was reported in a 12-year-old girl but no suggestion of a cause was ascertained [8].
To our knowledge, this is the first reported case of unilateral haemolacria in a patient with migraine with aura. The fact it can side shift, together with normal examination and investigations, suggests it is not caused by a structural abnormality. Furthermore, the lack of menstruation in our patient makes a hormonal link unlikely and a bleeding disorder has been ruled out by normal blood tests. Similarly, the lack of epistaxis in general nor during the nine episodes makes epistaxis with retrograde flow unlikely. Undoubtedly the significant hypertension that is documented with the haemolacria may be a contributing factor. We think it is unlikely these episodes are dissociative given she presented in straightforward way and the episodes can be controlled by migraine prophylactic medications. Since haemolacria was ipsilateral to the migraine headache with associated conjunctival injection, we propose this may occur, partly due to autonomic involvement of the conjunctiva, although the exact mechanism remains unknown.
CONCLUSION
This case highlights a rare presentation of haemolacria ipsilateral to migraine with visual aura and associated with hypertension. We propose this is caused partly by an autonomic phenomena. In any case of haemolocaria it is important to exclude an underlying structural lesion, and also consider a dissociative or haematological cause.
CONSENT
Informed consent was obtained from the patient to utilize her anonymized medical record, photograph and case for this report.
REFERENCES
- Murube J (2011) Bloody tears: historical review and report of a new case. Ocular Surface 9: 117-125.
- Seethapathy G and Jethani J (2020) Uncontrolled systemic hypertension and haemolacria. Indian Journal of Ophthalmology 68: 638-639.
- Rahman MS, Karim MR, Islam MM, Karim MdR (2007) Dissociative disorders with haemolacria: Series of case reports. Journal of Bangladesh College of Physicians and Surgeons 35: 36-42.
- Barbanti P, Fabbrini G, Pesare M, Vanacore N, Cerbo R (2002) Unilateral cranial autonomic symptoms in migraine. Cephalalgia 22: 256-259.
- Bai F, Zhou XB, Wang P, Wang LH, Wang F, et al. (2020) Retrospective investigation of spontaneous bloody tears: a report of 27 cases. Zhonghua Yan Ke Za Zhi 56: 53-58.
- Ho VH, Wilson MW, Linder JS, Fleming JC, Haik BG (2004) Bloody tears of unknown cause: case series and review of the literature. Ophthalmic Plast Reconstr Surg 20: 442-447.
- Ottovay E and Norn M (1991) Occult haemolacria in females. Acta ophthalmologica 69: 544-546.
- Ullah A, Badshah M, Jamil U (2015) An unusual case of bloody tears. Ann Indian Acad Neurol 18: 351.
Citation: Barakova L, Reid JM (2020) Haemolacria Associated with Severe Attacks of Migraine with Visual Aura and Hypertension. J Clin Stud Med Case Rep 7: 0102.
Copyright: © 2020 Barakova L, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

