
Hands Function and Rheumatoid Arthritis: Case Report and Rehabilitation Outcomes
*Corresponding Author(s):
Tarek M El-GoharyDepartment Of Physical Therapy, College Of Medical Rehabilitation Sciences, Taibah University, Medina, Saudi Arabia
Tel:+966 0545007025,
Email:dr.elgoharyt@yahoo.com
Abstract
Introduction
Rheumatoid arthritis is an autoimmune disorder which starts in the joints of the hands and feet with symptoms of warm, stiff and swollen joints. This case report purported to details the clinical presentation and rehabilitation outcomes of a case of Rheumatoid Arthritis causing severe functional disability of hands.
Case report
The study subject was 46-year-old Saudi male with 3 years history of Rheumatoid Arthritis. Patient received medical care and rehabilitation. Physical therapies to control symptoms, in addition to exercise therapy as tolerated, using the sponge ball, were the main interventions. The patient showed decrease in joints pain, synovitis and tenderness. Hand grip strength and Key pinch strength showed significant (p<0.05) improvement at 5 weeks of exercises. Patient has shown more independence with activities of daily living. Health assessment questionnaire disability index dropped from 1.7 to 0.9 which reflects improvements.
Discussion/Conclusion
The patient was slowly but fairly responding to physical& exercise therapy. Sponge soft ball is convenient tool to be used by patients with rheumatoid arthritis for improving hands functional capacity.
Keywords
INTRODUCTION
Rheumatoid Arthritis (RA) is an autoimmune disorder that produces persistent inflammatory joint symptoms throughout the body. RA is chronic non-curable systemic inflammatory disease with early symmetrical but unpredictable symptoms. RA has a rather rapid onset where early clinical manifestations most frequently located in the small joints of the hands [1]. RA is a complex systemic disease, if left untreated, can worsen in a matter of weeks. RA can progress differently in each patient. Therefore, rehabilitation should be tailored to suit every patient’s sufferance. RA has no specific etiology and it is not uncommon for patients to suffer a relapse while being under physical rehabilitation [2,3]. Patients with RA must be carefully monitored as they experience cycles of relapse [2,3]. The rheumatologist has to control symptoms using medications. Rehabilitation clinicians and physical therapists have to control symptoms and improve functional capacity using rehabilitation measures. Unfortunately, there is weak evidence and uncertainty to support using cold applications and hand exercises to control symptoms and improve functional ability of hands [4]. We hypothesize that early physical therapy intervention and participating in individualized hand exercise programme, within the limits of physical capacity, could slow down disease progression and improve functional ability of hands. Reviewing of related literature showed that there is no previously published case report discussing clinical presentation and rehabilitation progression of disabled hands in patient with RA. The present report describes an untraditional case presenting in a male patient formerly diagnosed with RA that developed flare up of symptoms along with muscular and osteoarticular complications of both hands.
CASE REPORT
A 46- year old, right hand dominant Saudi male patient with 3 years history of Rheumatoid Arthritis (RA) presented with a flare up of symptoms at both hands. Symptoms primarily were synovitis, swelling, pain, lack of power and increased heat at both hands. Patient was diagnosed with RA 3 years ago by rheumatologist. Patient started physical therapy rehabilitation program since he was diagnosed but he has been inconsistent with the rehabilitation particularly when he has symptoms under control. Patient indicated a past history of general body ache, low grade fever, deconditioning, fatigue, grossly restricted mobility in addition to lack of appetite for a two weeks before being diagnosed. Patient was first seen by internist who prescribed some analgesics and anti-inflammatory that did not help much. Morning stiffness and fatigue were his chief complaint. The rheumatologist requested all necessary investigations and confirmed the diagnosis of RA. Patient has positive family history given that his grandmother was diagnosed with RA. Patient presented, at this episode, with swelling of both knees and hands but for the purpose of discussion we will mainly focus on hands function and rehabilitation potential. The orthopedic clinical specialist who provides physical therapy and rehabilitation immediately referred the patient to the rheumatologist to monitor and control the flare up and exclude any new systemic diseases. The rheumatologist conducted all necessary investigations and adjusted the medications accordingly. Patient is currently taking disease-modifying anti-rheumatic drugs. The patient did not report any recent history of trauma. Patient reported that he has all over body ache, restricted mobility and poor functional capacity. Patient had poor posture in terms of mild stooping posture. Patient had pain severity of 3-4/10 at both hands which is getting worse. Pain is 2/10 at best and 8/10 at worst. Pain has a rather rapid onset in addition to a nature of wide range of characteristics like being constant or intermittent. The flare up and pain is slowing down the patient during most of activity of daily living and affects his quality of life. Patient had significant difficulties to button and unbuttons his shirt, use the keys or brush his teeth.
Objective physical examination revealed grossly restricted mobility of hands, Particularly Proximal Interphalangeal Joints (PIP) and Metacarpophalangeal Joints (MCP). The MCP joint of the index finger was the most affected. There was significant effusion of PIP and MCP joints in addition to swelling of periarticular structures particularly the extensors tendons as shown in figure 1. The patient had marked swelling and increased heat at swollen joints. Manual muscle test of fingers flexors and extensors was 4-/5 and 3/5 respectively. Right thumb extensors and abductors showed 3/5 and 3+/5 respectively. Left thumb extensors and abductors showed 3+/5 and 4-/5 respectively. Patient managed to oppose his thumb but with poor quality. Patient had difficulties to squeeze the hand grip dynamometer or pinch gauge. Patient reported difficulties with tip-to-tip, palmar and key pinch fingers strength. The study was single-blinded and of 6 weeks duration. Neuromuscular examination did not show any apparent deficits. Patient managed to finish 5x sit- to- stand in 18 seconds. Observational gait analysis revealed mild unsteadiness, slow gait and poor to fair feet clearance. Rehabilitation program was immediately restarted aiming to control symptoms, restore functional mobility, improve physical & functional capacity of both hands. This study was approved by the Ethics Committee of College of Medical Rehabilitation Sciences, Taibah University (Approval No. CMR-PT-2017-04). Informed consent was obtained from the patient to publish this case report. The results of the rehabilitation program showed fair results. Comparison of hand grip strength and key pinch measured at 2- and 5- week showed a significant improvement in strength parameters. PIP joints of both hands have shown fair improvement with grade 1+ to 2+ effusion (p<0.05). The health assessment questionnaire disability index was used to monitor functional progress. Patient showed 1.7 at the beginning but after receiving the rehabilitation program and at the fifth week he showed 0.9 score.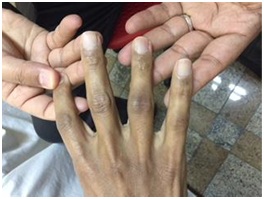 Figure 1: Swollen proximal interphalangeal joints and metacarpophalangeal joints.
Figure 1: Swollen proximal interphalangeal joints and metacarpophalangeal joints.
DISCUSSION
This case report presenting practical evidence-based advice on the best way to control symptoms associated with RA. The rationale of using the recommended interventions will be discussed along with the supporting evidence. The main purpose is to provide a framework for managing symptoms and improve the overall functional capacity. The primary target of this guidance is the physical therapists and rehabilitation team. Reviewing of related literature showed that this is the first case to describe clinical progression and physical rehabilitation outcomes of complex case of Rheumatoid Arthritis that disabled both hands. The patient had the typical picture of synovitis of the PIP and MCP joints but spared the distal interphalangeal joints of the hands. The PIP and the MCP joints of index and thumb, of both hands, had grade 3+ since the effusion was large enough not to respond to the milking manoeuver. The MCP joints of middle, ring, and little fingers had grade 2+ at both sides. Clinically, grade 3+ is more serious reaction to the disease. Moreover, effusion causes capsular distension, diminishes the hand grip efficiency and leads to pathomechanical consequences. Patient reported morning stiffness for almost one hour. Physical therapists should primarily emphasize on controlling the hands’ joints pain and swelling before proceeding with different rehabilitation techniques [4,5]. Patients with RA need multidisciplinary team approach for the best management [4,6]. Patients should be substantially involved in his rehabilitation programme. The therapist should establish active partnership with the patient [7]. Direct access to physiotherapy care is recommended. Rheumatologists are responsible to establish and monitor Disease-Modifying Anti-Rheumatic Drugs (DMARD) efficacy and seek alternatives when necessary [4]. Ongoing communication between different members of the multidisciplinary team is essential to avoid or minimize the deleterious consequences of RA. Ongoing educational programme is needed to guide the patient on the best way to control symptoms and combat the destructive disease effect [4]. Patient with RA has limitations with activities of daily living. Dominick, et al., stated that patients with RA need significant assist with personal care [8]. Patient was instructed to use cold packs to minimize the painful- swollen hands joints [4]. Patient was also instructed to squeeze soft sponge ball as tolerated. The ball was small enough to fit in one hand and allows fingers to contour around the ball. Patient reported no adverse events from using the sponge ball. Walsh encouraged clinicians to use interventions that have lower tendency for adverse events [5]. Hands exercises were essential to improve hands function and functional independence [4]. Moreover, regarding the training volume patient was instructed to pace activities according to his physical limits without exacerbating disease activity or harming his joints. Patient was given a handy sheet to illustrate the home exercise programme. A diary was given to monitor the adherence with the home exercise programme. Posture correction exercises in front of a mirror were used to correct the stooping posture. Board certified physical therapist consultant with 25 years of experience applied skilled physical therapy techniques. The therapist applied small amplitude oscillatory mobilization to restore hands functional mobility. Patient was demonstrated with gradual automobilization of both hands. After 6 weeks of physical therapy, patient has shown better posture, good/normal hand grip strength and better quality of hands’ mobility. Our findings correspond with Buljina, et al., who supported using exercise therapy to improve functional capacity of the rheumatoid hand [1]. The rehabilitation outcomes were in consensus with Knittle, et al., who encouraged therapists to set realistic and attainable exercise goals to achieve progress [9]. Squeezing the sponge ball was easy exercise plan that improved hands function. Patient started to have positive effect on quality of life through achieving more independence. While being under rehabilitation, the therapist was carefully monitoring symptoms and providing feedback on goal progress. Patient is still experiencing morning stiffness but less than before. Patient also managed to execute 5x sit-to- stand test in 12 seconds. Patient has shown satisfactory progress but still falls behind age matched community ambulant group who had 6.2±1.3 seconds [10].
In conclusion, comprehensive objective physical examination should be continuously conducted to differentiate the flare up of RA from the possibility being affected by any other systemic disease in addition to modify the rehabilitation program accordingly. Early diagnosis and management are essential to minimize the harmful effects of RA and its deleterious complications. The clinical and physical picture should be fully discussed with the treating physician. Physical therapists and rehabilitation clinicians need to encourage patients with RA to practice the types of strengthening exercises that have greater effects and lower propensity for adverse events.
ACKNOWLEDGMENTS
The authors would like to acknowledge the continuous support from Taibah University and deanship of scientific research for facilitating all steps of research work.
CONFLICT OF INTEREST
The authors declare that there is no conflict of interest.
AUTHORS’ CONTRIBUTION
TME and SMA conceived and designed the study, and conducted the data collection. TME and SMA analyzed and interpreted the data in addition to the final review of the results. TME and SMA wrote the initial and final draft of the report and send it for publication. All authors are responsible for the findings and have critically reviewed and approved the final draft.
REFERENCES
- Buljina AI, Taljanovic MS, Avdic DM, Hunter TB (2001) Physical and exercise therapy for treatment of the rheumatoid hand. Arthritis Rheum 45: 392-397.
- Brocq O, Millasseau E, Albert C, Grisot C, Flory P, et al. (2009) Effect of discontinuing TNFalpha antagonist therapy in patients with remission of rheumatoid arthritis. Joint Bone Spine 76: 350-355.
- Vincent Y, Leighton C, Carruthers KJ (2014) Incidence, prevalence, costs, and impact on disability of common conditions requiring rehabilitation in the United States: Stroke, spinal cord injury, traumatic brain injury, multiple sclerosis, osteoarthritis, rheumatoid arthritis, limb loss, and back pain. Arch Phys Med Rehabil 95: 986-995.
- Luqmani R, Hennell S, Estrach C, Birrell F, Bosworth A, et al. (2006) British society for rheumatology and British health professionals in rheumatology guideline for the management of rheumatoid arthritis (the first two years). Rheumatology (Oxford) 45: 1167-1169.
- Walsh DA, McWilliams DF (2014) Mechanisms, impact and management of pain in rheumatoid arthritis. Nat Rev Rheumatol 10: 581-592.
- Verhoef J, Toussaint PJ, Zwetsloot-Schonk JHM, Breedveld FC, Putter H, et al (2007) Effectiveness of the introduction of an International Classification of Functioning, Disability and Health-based rehabilitation tool in multidisciplinary team care in patients with rheumatoid arthritis. Arthritis Care and Research 57: 240-248.
- Vilet Vileland TPM (2003) Rehabilitation of people with rheumatoid arthritis. Best Pract Res Clin Rheumatol 17: 847-861.
- Dominick KL, Ahern FM, Gold CH, Heller DA (2004) Health-related quality of life among older adults with arthritis. Health Qual Life Outcomes 2: 5.
- Knittle KP, De Gucht V, Hurkmans EJ, Vliet Vlieland TPM, Peeters AJ, et al (2011) Effect of self-efficacy and physical activity goal achievement on arthritis pain and quality of life in patients with rheumatoid arthritis. Arthritis Care Res (Hoboken) 63: 1613-1619.
- Bohannon RW, Shove ME, Barreca SR, Masters LM, Sigouin C (2007) Five-repetition sit-to-stand test performance by community-dwelling adults: A preliminary investigation of times, determinants and relationship with self-reported physical performance. Isokinetics and Exercise Science 15: 77-81.
Citation: El-Gohary TM, Abd Elkade SM (2019) Hands Function and Rheumatoid Arthritis: Case Report and Rehabilitation Outcomes. J Clin Stud Med Case Rep 6: 063.
Copyright: © 2019 Tarek M El-Gohary, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

