
Inadvertent Arterial Catheterization during Central Venous Catheter Insertion Same Problem with Different Management Modalities
*Corresponding Author(s):
Amr Awad AlbayomyDepartment Of Surgery, Vascular Surgery Unit, King Fahad Hospital Of University, Al Khobar, Saudi Arabia
Tel:+966 567326212; +20 1006278058,
Email:amvascular@gmail.com
Abstract
Most common complications of Central Venous Catheter (CVC) insertion are around vascular injury, misplacement and infection. Early complications regarding vascular trauma and catheter malposition need early management to avoid high morbidity and mortality sequels. Proper investigation and surgical planning should be a corner stone in successful management.
We present a series of 3 cases of inadvertent arterial catheterization during central venous catheter insertion despite using US guided puncture techniques and being patient in ICU or operative room. Although similar skin puncture area (supraclavicular between heads of sternocleidomastoid muscle), there are different arterial anatomical sites of penetration with different management plans.
Keywords
Catheter malposition; Central lines; Double layer stent; Inadvertent catheter; Ultrasound guided
ABBREVIATIONS
IJV: Internal Jugular Vein
USG: Ultrasound Guided
CVP: Central Venous Pressure
CXR: Chest X-Ray
CVC: Central Venous Catheter
CTA: Computerized Tomography Angiography
CCA: Common Carotid Artery
CCU: Coronary Care Unit
CVC: Central Venous Catheter
SCM: Sternocleidomastoid Muscle
CVP: Central Venous Pressure
SCV: Superior Vena Cava
Rt: Right
Lt: Left
INTRODUCTION
Steps of CVC insertion have its guarding check points to assure right puncture site, being in the right vein and avoidance of arterial or other structures malposition. Prophylactic measures avoiding inadvertent arterial puncture are crucial, also post insertion confirmation of catheter position is mandatory to decrease the unfavorable sequels that may even risk the patient life.
Case 1 presentation
Blood sample from the line was taken to check blood gases which then confirmed being arterial one.
|
PH |
pCo2 |
PO2 |
O2Sat |
|
7.4 |
44.3 |
83.8 |
98.8 |

Bedside neck color Doppler evaluation in longitudinal plan revealed passage of the catheter into the common *carotid artery (Figure 3).
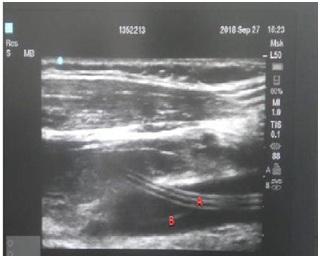
A CTA was then done for the neck and upper chest great vessels detecting precisely the puncture, course and tip positions of the catheter. It showed that the right central venous line had transfixed the right IJV then passed into the mid aspect of the right CCA, passing to the brachiocephalic artery with the tip protrudes into the aortic arch. As the catheter was 7fr. Size in a reachable anatomical site we decided to explore the jugular and carotid vessels to remove the malpositioned catheter with vessels repair. In operative room under local anesthesia and the patient in supine position with neck slight extension with left sided rotation and through an anterior neck longitudinal incision along anterior border of SCM, the IJV and CCA were exposed and controlled with vessel loops. Transfix punctures through the vein were found and a puncture of CCA. The catheter was pulled with artery control by a satinsky clamp then repair of the arterial puncture with proline 5/0 continuous sutures then repair of the vein punctures sites by couple of the same sutures.
Post-operative the patient was vitally stable with no signs of bleeding or hematoma collections. Patient blood exchange transfusion was then resumed using a Peripheral Inserted Central Catheter (PICC line).
Case 2 presentation
As the patient was already anesthetized and the surgical operation was started we decided to complete the surgical operation after insertion of other peripheral lines then after the neurosurgery operation finished and while the patient was still intubated, he was taken to have a CTA for neck and upper chest great vessels investigating the state of this central catheter.
CTA revealed puncture of the first part of Rt. Subclavian artery between the origins of right vertebral artery and right thyrocervical trunk then through the brachiocephalic artery with the tip in the ascending thoracic aorta (Figure 4).
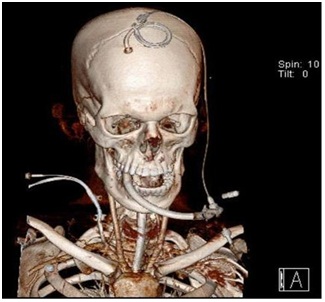
We decided to take the patient back to operative room and through a medial supraclavicular incision towards the punctured subclavian artery the procedure was done with control of main branches of first part of the artery and protecting the right phrenic nerve on the anterior aspect of the scalene anterior muscle (Figure 5). After artery control with clamps, catheter was removed with repair of puncture site with running proline 5/0 sutures. Suction drain was inserted and wound was closed in layers (Figure 6). Two days later the drain was removed with no significant collection with intact upper limb vascularity and no development of new neurological deficit clinically and he was vitally stable.
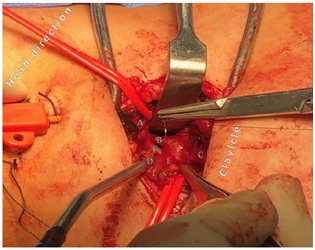 Figure 5: Supraclavicular exposure of first part of subclavian artery.
Figure 5: Supraclavicular exposure of first part of subclavian artery.A) Rt. phrenic nerve B) Rt. vertebral artery C) Rt. internal mammary artery D) Rt. thyrocervical trunk E) Rt. subclavian artery F) Cathet
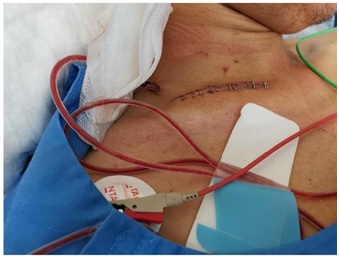 Figure 6: Post operative supraclavicular incision approximated by stapler.
Figure 6: Post operative supraclavicular incision approximated by stapler.Case 3 presentation
During current admission in CCU a CVC (7fr.) was planned to be inserted in Rt. IJV. After insertion for about 10 days giving fluids and medications and while connecting the central line to a pressure transducer to measure the central venous pressure it was surprisingly noticed that the pressure and the wave forms are arterial in nature.
Blood gases also confirmed being arterial blood samples.
Plain CXR was done which gave a high suspicion of being arterial catheter by the straight course of the catheter and direction towards the ascending aorta rather than the Superior Vena Cava (SVC) (Figure 7).

A triphasic CTA was performed showing that the catheter penetrated the proximal common carotid artery with its tip in ascending aorta (Figures 8 and 9).
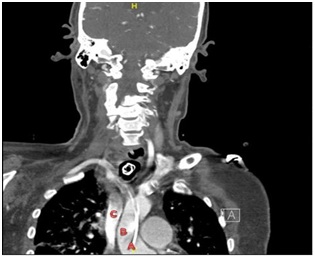
A) Tip of the catheter B) Ascending aorta C) Superior vena cava
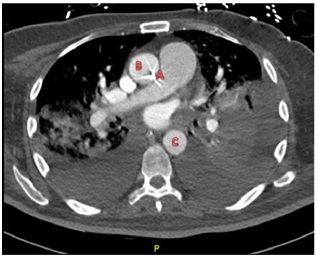 Figure 9: Axial section of CTA chest (venous phase) Showing the passage of catheter into ascending aorta.
Figure 9: Axial section of CTA chest (venous phase) Showing the passage of catheter into ascending aorta.A) The catheter B) Ascending aorta C) Descending thoracic aorta
The patient condition was a challenging one for open surgical removal of the central catheter as he had recent MI, multiple comorbidities, on dual antiplatelet and the low anatomical site of CCA penetration which could need median sternotomy to guarantee the proper control of CCA. For these reasons we preferred managing the case through minimal invasive procedures by pulling the catheter with securing the puncture hole by stent placement. With co-operation with neuro-intervention under local anesthesia through right femoral artery access and selective Rt. CCA angiogram detecting precisely the site of arterial puncture, securing the passage with a stiff wire, deployment of a double layer stent at the site of arterial puncture (Figure 10) then pulling the catheter out. We were standby to do balloon dilatation of the stent if leakage detected but fortunately no leak detected post catheter removal from the puncture site (Figure 11).
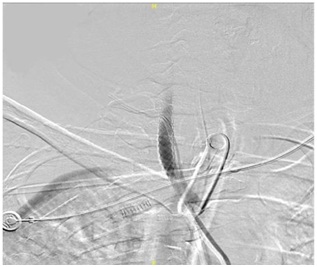
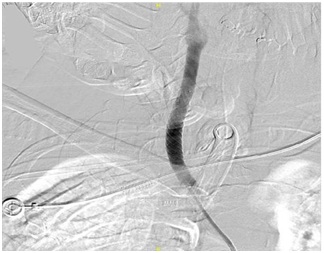
Post-operative the patent was vitally stable with no clinical signs of bleeding, hematoma formation or any new neurological events. Follow-up X-ray showed no hemothorax.
DISCUSSION
CVC complications included failure to place the catheter (22%), arterial puncture (5%), catheter malposition (4%), pneumothorax (1%), subcutaneous hematoma (1%), hemothorax (less than 1%), and asystolic cardiac arrest (<1%) [2]. Arterial puncture was noted in 3 to 15 % of central venous access procedures [1].
Unrecognized arterial cannulation with subsequent dilation and catheter placement is associated with life-threatening hemorrhage and neurologic complications [3].
Prolonged arterial catheterization can result in thrombus, neurologic deficits, and stroke. Immediate removal of an accidental arterial catheter can result in uncontrolled hemorrhage, pseudoaneurysm, and Arteriovenous (AV) fistula formation; especially in patients who are treated with anticoagulants or antiplatelet agents [4].
Late recognition of arterial cannulation increases the risk of hemorrhagic complications that may require surgical intervention [4] as one of our cases which was detected 10 days post insertion.
If inadvertent arterial insertion fails to be recognized, further complications can arise from infusion through malpositioned catheters. Rare cases of cerebrovascular events and neurologic deficits have been reported in the literature as a result of infusion through an accidental arterial lines [5,6].
Various risk factors have been identified for CVC misplacements like obesity, short neck, lack of USG, coagulopathy, intubated patient, hypovolemic, hypotensive patient (less pulsatile backflow), congenital malformations, edematous patient etc. inexperience of the clinician inserting the line has a consistent relationship to complication rate [7].
Inadvertent arterial cannulation can be detected by brightness of the blood color and the projectile flow. This is not always a reliable confirmation when a patient is hemodynamically unstable, therefore the central catheter remains in an artery.
Inadvertent arterial cannulation is a known complication during CVC placement, the combined use of ultrasound measurement and arterial blood gas analysis helps in picking up the arterial puncture at the earliest. The management is based on the site of arterial puncture and patient factors.
Various means have been suggested to prevent the misplacements of IJV catheters like use of USG and fluoroscopic guidance. Early detection of misplaced catheters can be done by using CXR, arterial blood gas analysis and central venous pressure monitoring.
Arterial blood gas analysis seems to be an easy, effective and definitive way of confirming the placement of IJV catheter. A chest X-ray is recommended after inserting IJV catheter to check whether the placement in central vein is consistent with the pathway of SVC.
Ultrasound can significantly decrease the negative impact of clinician inexperience [7]. While Multiple studies have demonstrated the benefit of using ultrasound to reduce vascular complications [8,9], Using the ultrasound does not eliminate the risk of arterial puncture, and catheters can still be inadvertently placed into the arterial system [10,11] As occurred in all of our patients who received central catheters USG.
Pressure waveform monitoring is another technology used to guide central line insertion. It can be used by itself or in tandem with ultrasound. Like ultrasound, however, it does not entirely prevent inadvertent arterial cannulation even though it is undeniably helpful [4].
We noticed in our cases that the precise evaluation of catheter anatomical puncture site, course and position of the tip was by CT angiogram within the venous phase in triphasic CTA as the catheter opacity is masked in arterial phase by the arterial opacity itself and become more obvious in venous phase.
The measures to manage inadvertent arterial trauma are catheter removal and external compression, endovascular intervention in the form of stents, closure devices, or direct surgical arterial repair.
For considering removal of a catheter and external compression the artery should be easily accessible and compressible, e.g. femoral artery. Recent studies have demonstrated that leaving the arterial catheter in place with prompt repair carries less morbidity and mortality than catheter removal with pressure [12,13].
Carotid artery compression involves risk of cerebral ischaemia, dislodgement of embolus. Guilbert et al. [12] concluded that pull and pressure method involves highest number of complications and recommended surgical arterial repair. They also proposed a Guilbert management algorithm [12] suggesting that if the site of repair is easily accessible like carotid artery surgical repair should be done and if not like in subclavian artery, an endovascular repair should be done [12].
The choice and use of endovascular techniques varies as per the patient factors, coagulation status and site of vessel punctured. Two types of endovascular devices are available, stent grafts or percutaneous vascular closure devices.
CONCLUSION
CONFLICTS OF INTEREST
REFERENCES
- McGee DC, Gould MK (2003) Preventing complications of central venous catheterization. N Engl J Med 348: 1123-1133.
- Eisen LA, Narasimhan M, Berger JS, Mayo PH, Rosen MJ, et al. (2006) Mechanical complications of central venous catheters. J Intensive Care Med 21: 40-46.
- Oliver WC Jr, Nuttall GA, Beynen FM, Raimundo HS, Abenstein JP, et al. (1997) The incidence of artery puncture with central venous cannulation using a modified technique for detection and prevention of arterial cannulation. J Cardiothoracic Vasc Anesth 11: 851-855.
- Bowdle A (2014) Vascular complications of central venous catheter placement: Evidence-based methods for prevention and treatment. J Cardiothoracic Vasc Anesth 28: 358-368.
- Khouzam RN, Soufi MK, Weatherly M (2013) Heparin Infusion through through a central line misplaced in the carotid artery leading to hemorrhagic stroke. J Emerg Med 45: 87-89.
- Wang RC, Katz SE, Lubow M (2000) Visual loss and central venous catheterization: Cortical blindness and hemianopsia after inadvertent subclavian artery entry. J Neuroophthalmol 20: 32-34.
- Blaivias M (2009) Video analysis of accidental arterial cannulation with dynamic ultrasound guidance for central venous access. J Ultrasound Med 28: 1239-1244.
- Troianos CA, Jobes DR, Ellison N (1991) Ultrasound-guided cannulation of the internal jugular vein. A prospective, randomized study. Anesth Analg 72: 823-826.
- Randolph AG, Cook DJ, Gonzales CA, Pribble CG (1996) Ultrasound guidance for placement of central venous catheters: A meta-analysis of the literature. Crit Care Med 24: 2053-2058.
- Pillai L, Zimmerman PM, d’Audiffret AC (2011) PS170. Inadvertent great vessel arterial catheterization during ultrasound-guided central venous line placement: A potentially fatal event. J Vasc Surg. 53: 74.
- Parsons AJ, Alfa J (2009) Carotid dissection: A complication of internal jugular vein cannulation with the use of ultrasound. Anesth Analg 109: 135-136.
- Guilbert MC, Elkouri S, Bracco D, Corriveau MM, Beaudoin N, et al. (2008) Arterial trauma during central venous catheter insertion: Case series, review and proposed algorithm. J Vasc Surg 48: 918-925.
- Shah PM, Babu SC, Goyal A, Mateo RB, Madden RE (2004) Arterial misplacement of large-caliber cannulas during jugular vein catheterization: Case for surgical management. J Am Coll Surg 198: 939-944.
Citation: Albayomy AA, Saleh MS, Elsaid AS, Nasr MA, Mohamed AA, et al. (2019) Inadvertent Arterial Catheterization during Central Venous Catheter Insertion Same Problem with Different Management Modalities. J Surg Curr Trend Innov: S1004.
Copyright: © 2019 Amr Awad Albayomy, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

