
Lichen Striatus versus Linear Lichen Planus
*Corresponding Author(s):
Piotr BrzezinskiDepartment Of Dermatology, 6th Military Support Unit, Ustka, Poland
Tel:+48 692121516,
Fax:+48 598151829
Email:brzezoo77@yahoo.com
LETTER
Sir,
We present a case of adult lichen striatus in an atopic patient first diagnosed as lichen planus.
A 34 year-old patient, known with atopic dermatitis since childhood, managed well with emollients, in good medical status, no drug intake, no background of allergy, was seen in consultations for a lichenoid unilateral linear eruption over the right superior limb. He declared no symptoms, the sudden onset of the skin lesions, and no recent medical events in his life.
Close examination revealed lichenoid papules distributed in a linear mode, over the antero-lateral aspect of the right superior limb, no surrounding erythema, no scaling, and no scratching marks. Discrete xerosis over the body was also noticed.
Presumptive clinical diagnosis was linear lichen planus and a punch-biopsy was done, describing: hyperkeratosis, necrotic keratinocytes in the epidermis, mild spongiosis with exocytosis of lymphocytes, and focal lymphocytic infiltrate at the dermal-epidermal junction. The pathologist’s opinion was against lichen planus with concordance of clinical second opinion of lichen striatus.
During the following 7 months different therapies have been tried with no improvement of the skin lesions: topical class II steroids, phototherapy, systemic corticosteroids, antihistamines, emollients, tacrolimus, even homeopathy.
In favor of clinical diagnosis of lichen striatus were: the unilateral distribution of the lesions, over limbs, following Blaschko lines, with no other cutaneous signs; the absence of pruritus; abrupt onset and long evolution despite any attempt of treatment; papules were not so intense violaceous; polygonal appearance and Wickham’s striae were absent. The linearity of the lesions corresponded to Blaschko’s lines (Figure 1).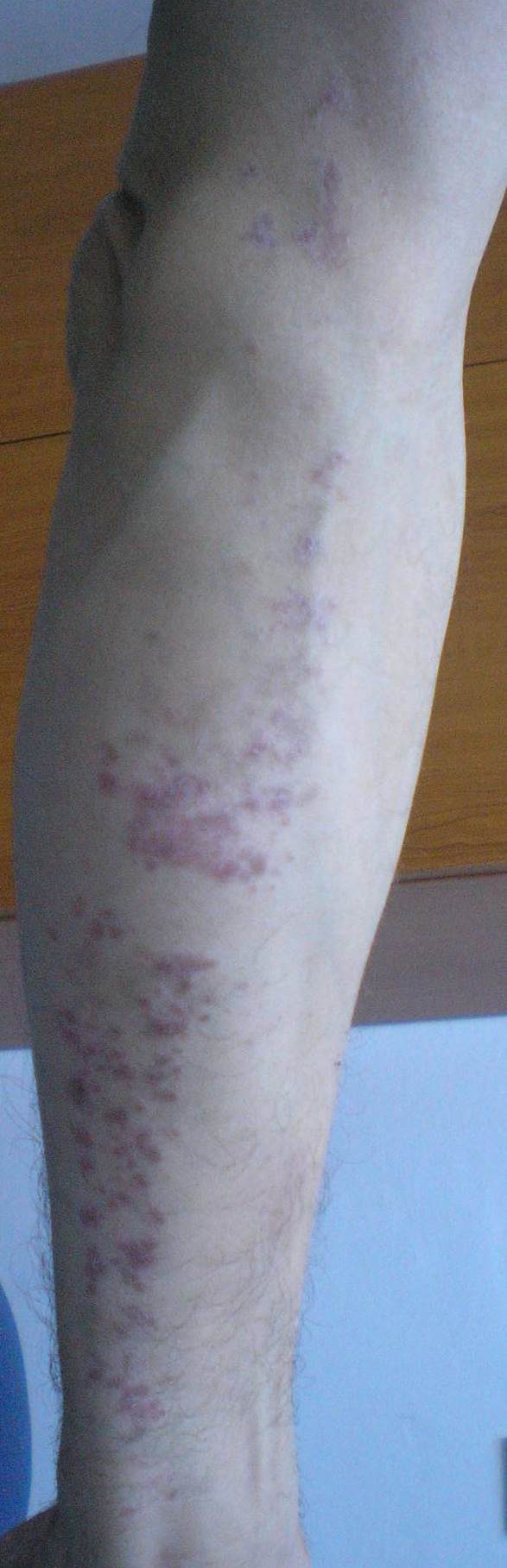
Figure 1: Lichenoid unilateral linear eruption over the right superior limb and lines of Blaschko.
The patient was followed for 7 months, trying different therapeutic modalities; afterwards he was not seen in consultation.
DISCUSSION
Lichen striatus is a rarely reported dermatosis with a peculiar linear distribution that establishes the diagnosis. It is well known in children, seldom described in adults. Clinical picture is quite specific: erythematous- hyperchromic lichenoid papules developed along the lines of Blaschko [1].
The etiology remains obscure, although different theories have been proposed: environmental factors, viral infections, cutaneous injury, and hypersensitivity acting on a genetic predisposition. There is an association between Lichen striatus and atopy (as present case) which may contribute to its pathogenesis; multiple studies report an increased incidence of lichen striatus in those with atopic family histories (asthma, allergic rhinitis, atopic dermatitis [2]. The appearance of lichen striatus that follows the lines of Blaschko suggests a postzygotic somatic mutation. It is more often described in children (especially 5-15 years old), both sexes being equally afflicted, although some studies favor the females. Lichen striatus is a clinical diagnosis; in a doubtful situation skin biopsy is needed o rule out other lichenoid dermatoses (especially lichen planus). In most cases it is a self limiting disease or with a good response to topical treatments [3].
Focal pattern of lymphocytic infiltrate is a pathological hint supporting lichen striatus [4].
Although lichen striatus is a clinical diagnosis, in doubtful situations, skin biopsy, thoroughly examination, medical history and long follow-up are needed o rule out other lichenoid dermatoses (especially lichen planus) [5].
REFERENCES
- Karempelis PS, Cely SJ, Davis LS (2014) Lichen striatus in a mother and son. Int J Dermatol 53: 366.
- Patrizi A, Neri I, Fiorentini C, Bonci A, Ricci G (2004) Lichen striatus: clinical and laboratory features of 115 children. Pediatr Dermatol 21: 197-204.
- Güngör ?, Topal IO, Erdogan S, Erdogan S, Özcan D (2014) Classical lichen planus and lichen planus pigmentosus inversus overlap with dermoscopic features. Our Dermatol Online 5: 42-44.
- Santos BS, Guedes Vilar EA, Freitas PM, Barbosa Durães SM, Estrella E. (2013) Multiple cutaneous reticulohistiocytomas along the lines of Blaschko associated with lichen striatus. Indian J Dermatol Venereol Leprol 79: 251-252.
- Chiriac A, Foia L, Chiriac AE, Birsan C, Solovan C, et al. (2013) Lichen striatus - case reports. Our Dermatol Online 4: 330-332.
Citation: Brzezinski P, Chiriac A, Birsan C (2015) Lichen Striatus versus Linear Lichen Planus. J Clin Dermatol Ther 2: 008.
Copyright: © 2015 Piotr Brzezinski, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

