
Management of a Female Patient with Fournier’s Gangrene Complicated by Hyperglycemic Hyperosmolar State and Multi-Organ Dysfunction: A Case Report
*Corresponding Author(s):
Tariq Abdul HamidDepartment Of Urology, Dubai Hospital, Dubai, United Arab Emirates
Tel:+971 552644224,
Email:drtariq_hamid@yahoo.com / taahamid@dha.gov.ae
Abstract
Background: Fournier's gangrene is a rare but deadly condition, with propensity for people with diabetes and long-term alcohol abuse, although it can also afflict patients with non-obvious immunological impairment. The nidus might be found in the genitourinary tract, lower gastrointestinal tract or the skin and is a mixed aerobic and anaerobic infection. The gangrene's development and spread is often fulminating resulting in multiple organ failure and death. Fournier’s gangrene in female patients has been reported to be associated with infection from episiotomy wounds and Bartholin’s abscess. But despite advanced management, mortality is still high and averages 20-30% .The current article discusses a case of Fournier’s gangrene in a female patient that was further complicated by a hyperglycemic hyperosmolar condition with approaching multi-organ dysfunction, as well as the successful medical and surgical therapy of the patient.
Case presentation: A 41 year old female presented to emergency with altered hemodynamic status, hyperosmolar hyperglycemia, hyponatremia and sepsis mandating optimization and immediate debridement of the perineal wound, followed by Intensive care and interval multiple debridement sessions and Negative pressure wound therapy, with multiple antibiotic therapies along the hospital course, eventually undergoing flap reconstruction of the wound.
Conclusion: Fourniers gangrene shows a higher male predilection with male: Female ratio of 10:1. However, the fact that women have a lower reported incidence of FG is no reason to dismiss the ailment as despite advanced therapeutic options available, mortality rate remains high ranging between 20-30%, mandating a thorough physical examination especially in diabetic patients with uncontrolled high blood glucose levels presenting with sepsis
Keywords
Case report; Diabetes mellitus; Fournier’s gangrene; Necrotising fasciitis; Wound debridement
Abbreviations
NF: Necrotizing Fasciitis
FG: Fournier’s Gangrene
IDU: Infectious Department Unit
NPWT: Negative Pressure Wound Therapy
NSTI: Necrotizing Soft Tissue Infections
GCS: Glascow Coma Scale
Background
Necrotizing Fasciitis (NF), a life-threatening infection of the soft tissues, is a medical and surgical emergency characterized by subtle, rapid onset of spreading inflammation and necrosis starting from the fascia, muscles and subcutaneous fat, leading to subsequent necrosis of the overlying skin. Once suspected, immediate and extensive radical debridement of necrotic tissues is mandatory. Appropriate antibiotics and intensive general support avoid massive systemic diffusion of the infective process and are the key for successful treatment. However, early diagnosis is missed or delayed in 85% to 100% of cases in large published series; because of the lack of specific clinical features in the initial stage of the disease, it is often underestimated or confused with cellulitis or abscess [1]. Mortality rates are still high as the infection itself can get complicated by other co-morbidities.
Fournier’s Gangrene (FG) is an infective NF that affects the external genitalia, perineal, and perianal regions. It is an acute, rapidly progressing, and possibly fatal NF. Men are often affected by Fourniers gangrene which was first recorded in 1883. Women and children, on the other hand are known to be affected. In the recent years, the incidence of this type of NF in both sexes has increased. However, despite advanced therapeutic options available, mortality rate remains high ranging between 20-30% [1].
The present case report describes a case of FG in a female patient that was complicated by hyperglycemic hyperosmolar state with impending multiorgan dysfunction and its successful management.
Case Presentation
A 41-year-old woman presented to the hospital with a two-day altered level of consciousness, Glascow Coma Scale (GCS) of 10/15, hypotension (77/64 mmHg), and tachycardia. This was also linked to septicemia and respiratory distress. Physical examination of the patient revealed that the lower abdomen was soft and non tender. During examination of the genitalia, erythema and induration were found in the perineal area, including the labia majora, as well as indurated necrotic spots on the right proximal medial thigh. Patient was resuscitated with fluids and vasopressors at the emergency room, and was electively intubated due to impaired consciousness.
After stabilization, the patient underwent IV contrast CT scan of the abdomen and pelvis, which revealed diffuse interstitial pancreatitis with peri-pancreatic inflammation and minor fluid collection (figure 1). In addition, diffuse inflammatory changes were noted in the skin and subcutaneous tissues of the pubic region and labia extending into the perineum, mainly on the right side.
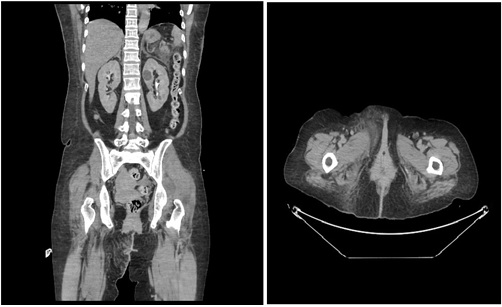 Figure 1: A) left B) right diffuse inflammatory changes in the skin and subcutaneous tissues of the pubic region and labia extending into the perineum.
Figure 1: A) left B) right diffuse inflammatory changes in the skin and subcutaneous tissues of the pubic region and labia extending into the perineum.
Lab parameters were significant for hyperglycemia (1223 mg/dl), blood glucose levels >600 mg/dl, HbA1c 17.6, Wbc 17.4, C-reactive protein 124, pro-calcitonin 0.84, and pH of 7.2. The patient also had elevated amylase, and lipase levels of 1070 U/L, and 4037 U/L, respectively. Her renal functions were also significantly impaired with a creatinine value of 5.3 mg/dl. The plasma osmolality of the patient was found to be 432 mOsm.
Based on the above-mentioned clinical, radiological and laboratory investigations, a diagnosis of Fournier’s gangrene was made. This diagnosis was further complicated by hyperosmolar hyperglycemic state and renal impairment with element of pancreatitis (multi organ dysfunction) with impaired GCS of 8. The patient was provided the medical care she needed to manage her diabetes and renal impairment. She was then given empirical antibiotics (meropenem) and an emergency wound debridement was planned, which included extensive debridement of the affected areas, including the labia majora, particularly on the right side (figure 2). The tissue sample from the debrided wound was sent for microbiological culture to identify the causative microorganism. The patient was then moved to Surgical Intensive Care Unit after surgery for additional round-the-clock care. The patient was also started on antifungals empirically and was overseen by the surgical team for wound care.
 Figure 2: A) Early operative debridement B) later operative debridement.
Figure 2: A) Early operative debridement B) later operative debridement.
Wound cultures taken during intraoperative debridement showed heavy mixed growth including coliform candida species and proteus species. She also had a positive blood culture for Lactobacillus jensenii. Culture directed antimicrobials such as meropenem and tigecycline were prescribed to the patient by the Infectious Department Unit (IDU). During the follow-up examination 2 weeks post 5th debridement, the IDU insinuated that there was a good source control (figure 3). Nevertheless, the specialists hinted regarding the possibility of osteomyelitis as the wound was quite deep seated. Therefore, it was decided to continue tigecycline for 3-4 weeks while awaiting another biopsy culture of the wound tissues.
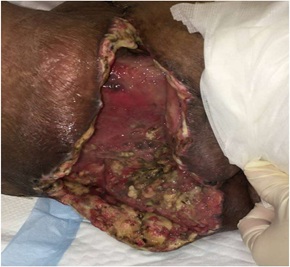 Figure 3: Post multiple debridements.
Figure 3: Post multiple debridements.
Biopsy culture initially showed no growth, however a repeat wound culture done 6 weeks later was positive for Enterococcus Raffinosus and Candida lusitaniae. Hence, the IDU decided to add combination of Linezolid, Tazocin, and Anidulafungin.
Patient was kept on Negative Pressure Wound Therapy (NPWT) with pressure varying between 125 to 150 mmHg, after the second session and she underwent a total of six debridement sessions. The wound was each time irrigated thoroughly with dermacyn and packed with dermacyn soaked gauze. During the third operating session, the patient had a diversion colostomy after debridement as a source control measure to prevent further stool contamination. It is of particular mention that after the second session, appropriate source control was achieved.
Patient’s condition gradually improved post diversion colostomy formation, and her GCS improved (15/15). During the follow-up, MRI pelvis with contrast was performed 4 weeks later that revealed no evidence of cortical erosion nor any destructive changes of the pubic bones and pubic rami on both sides. During post-operative follow-up period, the psychiatry team and medical team managed the patient’s gloominess and hyponatremia, respectively. The extensive wound closure was performed using 0/0 vicryl for subcutaneous layer and monocryl 2/0 for skin by the plastic surgery team. The closure was facilitated by performing a gluteal flap reconstruction making a small cut back incision along the lateral right gluteal area and drains were placed (figure 4).
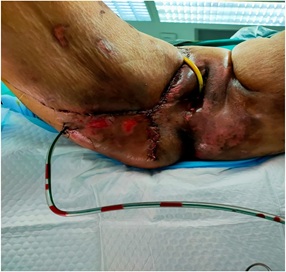 Figure 4: Gluteal flap reconstruction.
Figure 4: Gluteal flap reconstruction.
Patient was further followed by the team, and wounds were examined daily with regular dressings and she was maintained on a high protein diabetic diet to hasten the recovery. Further wound management also required Negative Pressure Wound Therapy (125-150 mmHg), which resulted in good wound healing (figure 5). Patient eventually underwent reversal of colostomy after complete wound healing 2 weeks later with complete wound healing (figure 6).
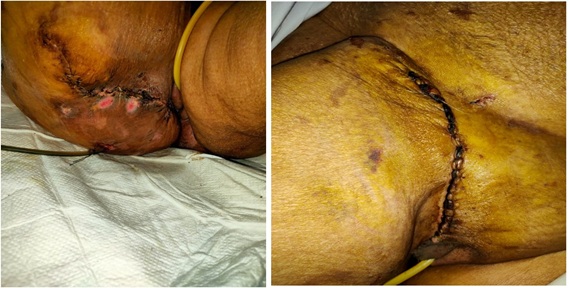 Figure 5: A) left B) right wound healing.
Figure 5: A) left B) right wound healing.
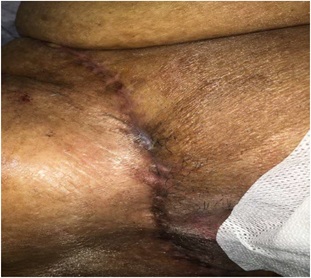 Figure 6: complete wound healing.
Figure 6: complete wound healing.
Discussion
Necrotizing Soft Tissue Infections (NSTIs) include necrotizing forms of fasciitis, myositis, and cellulitis. These infections are characterized clinically by fulminant tissue destruction, systemic signs of toxicity, and high mortality. Accurate diagnosis and appropriate treatment must include early surgical intervention and antibiotic therapy. NF shows a higher male predilection with male: female ratio of 10:1. FG severity index, length of hospital stays, number of debridement’s, and wound cultures of NF in females were comparable to that of males. Furthermore, the debridement of wounds in females is performed by a team of general surgeons, whereas the procedure is carried out by urologists in case of male patients. The mortality rate of this disease in females is comparable to that of men (6% versus 7% with p-value > 0.05) [2].
FG in female patients has been reported to be associated with infection from episiotomy wounds and Bartholin’s abscess. But despite advanced management, mortality is still high and averages 20-30% [3].
In terms of the predisposing diseases, diabetes mellitus (DM, n=8, 66.7%) ranking number one amongst the other factors. Perianal/scrotal discomfort and swelling were the most prevalent complaint at presentation (72.9%), followed by tachycardia (58.13%), purulent discharge from the perineum (55.81%), crepitus (51.16%), and fever (41.86%) [4]. Our patient, on the other hand, had an altered sensorium and sepsis, as well as an erythematous perineal area and necrotic patches over the right proximal medial thigh. Although thrombosis of penetrating arteries to the skin is the essential feature in the pathogenesis of NSTI, the initial clinical skin signs underestimate the tissue infection present. Before skin changes suggestive of necrosis appear, significant numbers of dermal capillary beds must thrombose [5]. Early operative debridement is a major determinant of outcome in NF. However, early recognition is difficult clinically. In a research by Ogilvie and Miclau, non-survivors had significantly lower mean serum sodium than survivors [6]. These findings could indicate that renal dysfunction occurs as a result of multiorgan damage induced by a more severe infection, as well as hyponatremia from fluid sequestration in severe soft tissue infections. A similar observation was made in our case, where the patient had chronic hyponatremia that was handled by the medical team throughout her hospital stay. Hyponatremia may thus be a valuable criterion for discriminating between life-threatening NF that may suggest more aggressive management in these groups of patients. In clinically indolent cases, radiological evaluation, such as CT and MRI, allows for early diagnosis. Surgical exploration and tissue biopsy are the gold standard. There is little resistance to blunt dissection of the normally attached superficial fascia, no bleeding, and foul-smelling 'dishwater' pus is characteristic.
The organisms that were prevalent in our case during the microbiological culture of the wound tissue samples were coliform candida species, proteus species, Lactobacillus jensenii, Enterococcus Raffinosus, and Candida lusitaniae. This is similar to the findings quoted by Oguz A in 2015 that showed higher prevalence of Escherichia coli (48.8%), Pseudomonas spp. (20.9%), Enterococcus spp. (18.6%), Staphylococcus spp. (13.9%), Streptococcus spp. (11.6%), Proteus spp. (11.6%), Acinetobacter spp. (9.3%), Bacteroides spp. (9.3%), and Klebsiellapneumoniae (4.6%) in patients with FG [4]. Fecal diversion is indicated when the anal sphincter is grossly contaminated or to facilitate wound management. The primary colostomy rate has been reported to be 16-17%, whereas the secondary colostomy rate has been reported to be 35-40%. A case series suggested that 3 patients received colostomy and 1 underwent cystostomy in order to counteract the fecal diversion [7]. Similar to the above-mentioned article, the patient in the present case report also underwent diversion colostomy..
A 52-year-old man with severe diabetic ketoacidosis who presented with fever and circulatory compromise had abnormal renal function, hypoalbuminemia, hyponatremia, abnormal liver function, metabolic acidosis, and high serum lactate concentrations, as seen in another case report by Jamieson A, et al. [8]. Despite rigorous treatment, the patient's delirium and high inflammatory markers persisted. Therefore, a CT scan was performed for the patient, which revealed gas within the perineum. As a result, the patient presented in this case report was diagnosed with FG and received surgical debridement and IV antibiotic therapy, which improved his overall condition. To summarise, occult perineal infection should always be suspected in diabetic ketoacidosis patients who have signs of sepsis but no apparent initial source of sepsis, as determined by a comprehensive history and physical examination (i.e., a likely undiagnosed scrotal abscess leading to skin sepsis and gas-gangrene of the subcutaneous tissues) [8-10].
Conclusion
The fact that women have a lower reported incidence of FG is no reason to dismiss the ailment. A fast diagnosis, early surgical intervention, precise antibiotic management, dressings and general care, as well as therapy of the patient's comorbidities, are all important factors in offering a better prognosis. As observed in this case, FG is a serious and life-threatening illness that can be detrimental and cause significant morbidity. Hyponatremia and hyperkalemia may be valuable markers for identifying life-threatening NF, suggesting more aggressive treatment in these patients who require immediate attention. Osteomyelitis should always be considered when deep wounds are present. With thorough wound inspections, adequate and careful glucose control becomes an important component in diabetic patients who present with hyperosmolar hyperglycemic state. The importance of early VAC therapy and diverting colostomy in instances involving the perineum and genitalia is critical for infection management. To avoid any healing complications, patients undergoing post flap reconstruction should have adequate wound care and comprehensive inspection
Authors Contribution
TH conceived and designed the manuscript. TH and AM drafted the manuscript. AK, MO and NM critically reviewed, revised and approved the manuscript. All authors have read and approved the manuscript and agreed to the submission.
References
- Aslanidis T, Myrou A, Giannakou-Peftoulidou M (2014) Management of a Young Female Patient with Fournier’s Gangrene and Lemierre’s Syndrome. Pan Afr Med J 18:
- Beecroft NJ, Jaeger CD, Rose JR, Becerra CMC, Shah NC, et al. (2021) Fournier’s Gangrene in Females: Presentation and Management at a Tertiary Center. Urology 151: 113-11
- Mallikarjuna MN, Vijayakumar A, Patil VS, Shivswamy BS (2012) Fournier’s Gangrene: Current Practices. ISRN Surg 2012: 942437.
- Oguz A, Gümü? M, Turkoglu A, Bozda? Z, Ülger BV, et al. (2015) Fournier’s Gangrene: A summary of 10 Years of Clinical Experience. Int Surg 100: 934-9
- Espandar R, Sibdari SY, Rafiee E, Yazdanian S (2011) Necrotizing Fasciitis of the Extremities: A Prospective Study. Strategies Trauma Limb Reconstr 6: 121-12
- Cabello RR, Gracida Mancilla N, Feregrino RR, Romero R, Ii F, et al. (2016) A Case Report of a Woman with Fournier’s Gangrene and Morbid Obesity. Medigraphic.com.
- Lancerotto L, Tocco I, Salmaso R, Vindigni V, Bassetto F (2012) Necrotizing Fasciitis: Classification, Diagnosis and Management. J Trauma Acute Care Surg 72: 560-566.
- Davoudian P, Flint NJ (2012) Necrotizing Fasciitis. Contin Educ Anaesth Crit Care Pain 12: 245-250.
- Zhang N, Yu X, Zhang K, Liu T (2020) A Retrospective Case Series of Fournier’s Gangrene: Necrotizing Fasciitis in Perineum and Perianal Region. BMC Surg 20:
- Eke N (2000) Fournier’s Gangrene: A Review of 1726 Cases. Br J Surg 87: 718-7
Citation: Hamid TA, Elmekresh A, Sidahmed MOA, Varghese SM, Sidou NMA, et al. (2023) Management of a Female Patient with Fournier’s Gangrene Complicated by Hyperglycemic Hyperosmolar State and Multi-Organ Dysfunction: A Case Report. Int J Case Rep Ther Stud 4: 023.
Copyright: © 2023 Tariq Abdul Hamid, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

