
Neuroenergy Mapping Diagnostic Capabilities in Hypoxic Brain Lesions
*Corresponding Author(s):
Alexandra Alexandrovna MaximovaMiraculum Medical Center, Tbilisi, Georgia
Tel:+995 595283313,
Email:aleksandra-krasn@mail.ru ; am@maximov.com
Abstract
Neuroenergy Mapping (NEM) is the topographic mapping of the brain’s energy metabolism by Direct Current Potentials (DCP). It allows an independent cohort of patients (18 children from 3 to 14 years old) with sharply reduced DCP in one or more areas of the cerebral cortex to be identified among children with diagnoses of ASD and other developmental disorders. Considering the experience of working with NEM and general clinical indications for children, there appeared to be a possibility of central circulatory disorders, and patients were referred for additional examinations. These included a Doppler ultrasonography of the brain and neck vessels and X-rays of the cervical spine in three projections. Results confirmed a diagnosis of dyscirculatory encephalopathy (I67.8) for 15 of the 18 patients. For 9 of these, blood circulation disorders were aggravated by identified disorders of the cervical spine. For 3 patients, the decrease in DCP was due to physiological vasospasm.
Successful correction of Central Nervous System (CNS) blood flow disorders led to an improvement in the general condition of patients. This included an abatement or disappearance of gross behavioral and sleep disorders and improvement of cognitive abilities and concentration.
The NEM study allowed patients to be quickly divided into cohorts. Each of these, in accordance with DCP indicators, was prescribed certain additional, traditional examinations. NEM therefore saved time and resources for both doctors and patients. For patients with severe negative behavior, NEM was particularly important, as traditional brain studies (EEG, MRI, and others) are difficult to process for this type of patient. Thus, sharply reduced DCP can become a biomarker for hypoxic brain lesions, and the NEM study wasa convenient tool for preliminary diagnosis.
Confirmed diagnoses of Autism Spectrum Disorder (ASD) and other developmental disorders should not discourage doctors and parents from considering that possible underlying pathological conditions may warrant a new diagnosis and treatment for the child patient. Health professionals should consider that parental complaints about their child’s condition may also have a basis other than ASD or other developmental disorders.
Keywords
ASD; Autism; Brain hypoxia; Cervical spine; Concentration; Ischemia; Negative behavior; Neuroenergy mapping; Sleep disorders
PURPOSE OF THE STUDY
To investigate Neuroenergy Mapping (NEM) as a possible non-invasive, diagnostic tool for revealing the state of blood flow in the central nervous system.
RESEARCH OBJECTIVES
1. Investigate the use of Neuroenergy Mapping (NEM)
- • To identify a cohort of patients with a sharply reduced DCP (direct current potentials) level,
- • To indicate that such deviations from the norm (standard) are possible violations in the central circulatory system
- • To recommend the traditional studies (ultrasound of the vessels of the brain/neck and X-rays of the cervical spine)that can confirm the NEM-indicated preliminary diagnosis.
2. Investigate the relationship between:
- • A sharply reduced level of DCP and the state of skeletal muscles of the cervical spine
- • A sharply reduced level of DCP and pathological changes in the blood vessels of the brain
RESEARCH MATERIALS
This study was conducted at the Center for Integrative Medicine, Miraculum (Integrative Medicine Center Miraculum LLC, State Registry Identification Number #405298244; www.facebook.com/autism.ge); Tbilisi, Georgia; as part of general research on the dependence of negative behavior and emotional disorders in children and adolescents on various pathological conditions [1-3]. A total of 135 patients, aged 3 to 19 years, took part in the study. Diagnoses included childhood autism (F. 84) and atypical autism (F. 84.1); anxiety personality disorders (F. 41); hyperkinetic disorders (F. 90); and dissocial personality disorder (F. 60.2). For this article, the considered sample was limited to patients in whom the initial NEM study recorded sharply reduced DCP in one or more lobes of the cerebral cortex. This was 14% of the entire sample or 18 children.
RESEARCH METHODS
-
Study of the disease’s history and patient’s life
-
Assessment of physical development
-
Examination by a pediatrician, neurologist, neurophysiologist, and psychologist
-
Instrumental diagnostics:
- • Neuroenergy Mapping(NEM) of the brain: study of the intensity of the cerebral energy exchange in the brain through analysis of Direct Current (DC) potentials as determined by changes in the acid-base balance of brain tissues,
- • Doppler Ultrasound (DUS) of the brain and neck blood vessels (intra/extracranial),
- • Radiography of the cervical spine in three projections.
INTRODUCTION
Currently, due attention is not given to studying the relationship of blood flow disorders of the central nervous system to behavioral and cognitive problems of children with diagnoses of autism and hyperkinetic and dissocial personality disorders. The high level of anxiety, hyperactivity, and negative behavior characteristic of such patients are considered disorders to be corrected by using certain classes of drugs without first searching for a root cause. An increasing number of studies in recent years have focused on:
- • the side effects of using neuroleptics, especially in children;
- • the legality of prescribing them; and
- • the validity of diagnostic criteria on which prescriptions are based.
Attention Deficit Hyperactivity Disorder (ADHD) is not associated with possible central circulation disorders, nor is a high level of anxiety associated with the possibility of benign intracranial hypertension. Studies in the field of high intracranial pressure and increased anxiety underlying a headache are few, and they focus mainly on children with hydrocephalus [4]. Based on the current study, however, it appears that children with ASD may have persistent cerebrospinal fluid disorders, although, at first glance, they may not be obvious, and that it is reasonable to pursue the possibility of such a diagnosis.
Although there is a study showing that ADHD patients are highly likely to have cerebral blood flow disorders [5], these conclusions have not been widely disseminated within clinical practice. There is a need to diagnose vascular pathologies and microcirculation disorders in ADHD, as well as investigate the feasibility of using vascular drugs for such patients.
In terms of reducing negative behavior in children with ASD, a recent study was conducted on the use of baclofen in combination with a neuroleptic [6]. The study concluded that baclofen has a beneficial effect, but its mechanism is described through its effect on the Gamma-Aminobutyric Acid (GABA) system. In the opinion of the author, there is another reason for this effect. Baclofen is seen as a central muscle relaxant that leads to improved behavior in children with ASD because it stabilizes he central circulatory system, including the circulation of the cervical-collar zone.
Neuroenergy mapping
NEM evaluates the intensity of cerebral energy metabolism by analyzing the Direct Current (DC) potentials associated with the acid-base balance of brain tissues. DC potentials refer to a stable difference in the millivolt (mV) range potentials recorded between the brain (or extra cerebral structures) and reference areas using direct current amplifiers. In a stable functioning state, this difference of potentials is stable within 1 mV for tens of seconds. The NEM registers slow brain activity. The DC potentials level correlates with a variety of biochemical parameters of the brain and main bodily systems, allowing resulting data to be used for diagnosing various pathophysiological conditions.
NEM shows the patient's DC potentials in 5 brain zones:
- • frontal zone
- • central zone
- • occipital zone
- • right temporal zone
- • left temporal zone
NEM results are compared to the standards for brain activity in these areas. The comparison is based on actual physical indicators, which deviate from the norm in one direction or another and is visualized by the software in a particular color scheme.
The interpretation of NEM data for patients with autism and other developmental disorders, with subsequent follow-up researches and pharmacological therapy choices, used methods developed directly by the author when working with patients at Miraculum. The original methodology was developed by a doctor of biological sciences, Professor V. F. Fokin, in the Neurophysiology Laboratory of the Scientific Center of Neurology of the Soviet, and later Russian, Academy of Medical Sciences [7].
RESEARCH RESULTS
A total of 18 patients, aged 3 to 14 years, participated in the study. They showed a wide variety of Direct Current Potentials (DCP) deviations from the standard/norm, both in the degree of deviation and the location (by the lobes of the cerebral cortex). However, despite the diversity, the overall indicator for patients was a sharp decrease in the DCP compared to the standard.
It should also be noted that all 18 patients in this article’s cohort had tonic disorders, increased reflexes, dysarthria, sleep-wake rhythm disorders, significant emotional lability, and cognitive disorders. When diagnosing these patients originally, these conditions were primarily ignored as symptoms of negative behavior. The results of the NEM study gave reason to investigatea new diagnosis of dyscirculatory encephalopathy (I67.8), which needed to be confirmed by a scientifically proven diagnostic method, a Doppler Ultrasound (DUS) of the brain and neck blood vessels.
For 15 patients (84% of the sample), the preliminary diagnosis was confirmed by the DUS. For 3 patients, the sharp decrease in DCP was explained by the existence of physiological vasospasm, which was confirmed by repeated NEM.
For 18 patients, the DCP decrease was:
Occipital lobe of the brain cortex (norm is 10.20 mV):
- • (-) 12.10 mV to (-) 1. 24 mV-7 patients,
- • 66 mV to 4.50 mV-8 patients.
Right temporal lobeof the brain cortex (norm is 9.80 mV):
- • (-) 37.40 mV to (-) 2.80 mV-10 patients,
- • 40 mV to 4.56 mV- 4 patients.
Left temporal lobeof the brain cortex (norm is 9.80 mV):
- • (-) 15.43 mV to (-) 0.28 mV- 8 patients,
- • 29mV to 3.50 mV- 5 patients.
Frontal lobeof the brain cortex (norm is 8,60 mV):
- • (-) 19.93 mV- only 1 patient,
- • 58 mVto 3.97mV- 9 patients.
Parietal lobeof the brain cortex (norm is 13,10 mV):
- • (-) 2.73 mVto (-) 1.23 mV- 2 patients,
- • 01 mVto 6.70 mV- 9 patients.
A sharp decrease in DCP in all lobes of the cerebral cortex precipitated an investigation into the likelihood of central circulatory disorders, while also allowing for a general clinical picture that accounted for past clinical experience with such children. All patients were, therefore, referred for additional studies that included the following:
- • For 15 patients, changes in blood flow in the vascular pools of the corresponding areas of the brain were detected during an ultrasound of the brain vessels and neck. These included deformity of the carotid arteries, moderate or severe extra vascular compression of the vertebral arteries during rotation, and moderate asymmetry of the vertebral arteries. In addition, notice the dysplasia of the vertebral arteries: Its diameter in patients ranges from 2.5-3.6 mm with a norm of 3.6-3.8 mm. Also, notice the decrease in the speed of linear blood flow through the vertebral arteries: Along the right vertebral artery, it ranges from 8-11 cm/s (with a norm of 10.7-18.5 cm/s), and the left vertebral artery ranges from 9.6-12 cm/s (with a norm of 12-19.5 cm/s).
- • In 9 patients out of the 15, the results of X-rays of the cervical spine in three projections revealed significant deviations from the norm, including the presence of abnormal kyphosis / lordosis in the cervical spine and instability of one or more vertebrae of the cervical spine
- • In the 3 remaining patients (out of the sample cohort of 18), the preliminary diagnosis of dyscirculatory encephalopathy was not confirmed, and the sharp DCP decrease was explained by physiological vasospasm during the first study, later confirmed by repeated NEM
- • For Miraculum patients without a pronounced DCP decrease, the DUS and radiography did not detect any of the above-mentioned violations
In this study, correlations between (1) a decrease in the diameter of the vertebral arteries and/or a decrease in the level of linear blood flow in the vertebral arteries and (2) a decrease in the DCP level in the occipital lobe of the cerebral cortex and the left/right temporal lobes of the cerebral cortex were evaluated. In general, the DCP decrease in the right and left temporal lobes was recorded for the most part in the area of the occipital lobe of the cerebral cortex.
To study the correlations, the Statistica 10 program was used to calculate the following Spearman correlation coefficients:
- • The Spearman correlation coefficient between the diameter of the vertebral arteries and the DCP decrease made up 0.96%. Such a high positive correlation confirms our hypothesis that low DCP levels are indicators of brain cell hypoxia against the background of central vascular disorders. Vertebral artery dysplasia, as a rule, is associated with the features of the vascular bed in these patients, as well as vertebral pathologies recorded during radiography of the cervical spine with functional tests
- • The Spearman correlation coefficient between the decrease in the level of linear blood flow in the right vertebral artery and the DCP decrease in the right temporal lobe made up 0.76% (a high positive correlation).
- • The Spearman correlation coefficient between the decrease in the level of linear blood flow of the left vertebral artery and the DCP decrease in the left temporal lobe made up 0.87% (a high positive correlation).
Thus, it can be argued that the study of DCP levels during NEM can indicate a new direction in diagnosing the state of blood flow in the central nervous system.
In accordance with confirmed diagnoses and based on all studies, a treatment protocol was developed for 15 patients. First, central circulatory disorders were addressed by:
- • improving the microcirculation of brain vessels (Vinpocetine, Nicergoline)
- • enhancing antioxidant activity (Ethylmethylhydroxypyridine succinate)
- • restoring venous outflow (Thiamine+Aescine, Diosmin+Flavonoids expressed as Hesperidin)
Second, 9 patients were treated with the following to correct musculotonic disorders due to problems of the cervical spine:
- • central-action muscle relaxants (Tolperisone)
- • a Shants neck collar,
- • electrophoresis and osteopathy sessions,
- • therapeutic medical massaging of the neck and collar area,
- • therapeutic gymnastics.
The course of treatment was followed from 1 to 3 months, depending on apatient's condition. After treatment, a second NEM brain study was performed. These recorded a positive trend in the DCP indications forall parts of the cerebral cortex (Table 1).
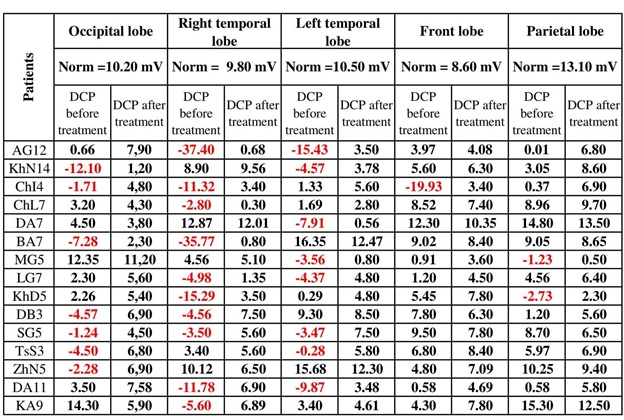 Table 1: Results of the NEM study before and after treatment of 15 patients with a confirmed diagnosis of dyscirculatory encephalopathy (I67.8.).
Table 1: Results of the NEM study before and after treatment of 15 patients with a confirmed diagnosis of dyscirculatory encephalopathy (I67.8.).
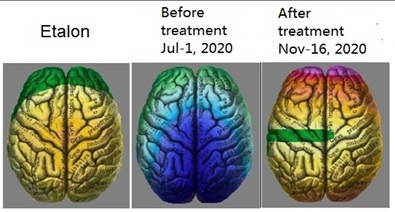 Figure 1: Visual representation of brain function before and after treatment (NEM studies).
Figure 1: Visual representation of brain function before and after treatment (NEM studies).
Figure 1 shows brain functioning improvement for one patient from July 1, 2020 (the first NEM study), to November 16, 2020 (the NEM study after treatment). The child’s brain is compared to the etalon on the left. The blue color in the central image is evidence of a profound brain hypoxia. The image on the right clearly shows that problems in the brain remain, but they are of a different scale. There are no signs of hypoxia, and the image is significantly closer to the reference.
Before the start of treatment, a parental survey documented the problems each child was experiencing. After treatment, a second survey recorded the following:
- • Behavior improved, and negative behavior diminished or abated;
- • Sleeping and waking patterns stabilized, and hyperactivity was reduced;
- • Emotional states stabilized;
- • Cognitive and motor functioning improved;
- • Concentration improved;
- • Speech apparatus functioning and small/large motor skills improved.
CONCLUSION
- A sharp decrease in DCP compared to the norm indicated pathological changes in vascular circulation, which were subsequently recorded and confirmed by an ultrasound of the brain/neck vessels and a radiography of the cervical spine.
- An analysis of deviations registered in the DCP allows clinicians to estimate the effectiveness of prescribed pharmacology for correcting disorders of the blood flow in the central nervous system, including:
- • drugs that improve blood circulation and metabolism in the brain - Vinpocetine, Nicergoline
- • diuretic drugs - Acetazolamide
- • venotonic medications - Thiamine+aescine, Diosmin+Flavonoids expressed as Hesperidin
- • antioxidants - Ethylmethylhydroxypyridine succinate
- • centrally acting muscle relaxants - Tolperisone
- Stabilization and improvements in the central circulatory system appear to be the result of correctly choosing pharmacological interventions and rehabilitation therapies that were appropriate for new diagnoses. These choices appear to lead directly to a subsequent improvement in the patients’ conditions and to a decrease in negative behavior in the entire sample of patients.
NEM allows the ability to quickly and easily organize patients with developmental disorders into separate cohorts based on various gross deviations from the reference indicators of brain function. This allows a clinician to outline the main directions for a search of existing neurological disorders and to determine the optimal list of additional examinations that needs to occur. Within the framework of this article, a sharply reduced DCP indicates possible hypoxic lesions in the brain and indicates, as a top priority among additional studies, a need for a DUS of the vessels of the brain and neck and X-rays of the cervical spine in three projections. In the cohort of patients for this article, the preliminary diagnosis of dyscirculatory encephalopathy (I67.8), based on NEM data, was later confirmed by traditional studies in 84% of cases. Thus, NEM can act as a convenient and useful tool for preliminary diagnosis, and sharply reduced DCP may be considered as one of the biomarkers of hypoxic brain lesions.
These conclusions are especially relevant for children with official diagnoses of ASD and other developmental disorders. The vast majority of official international (DSM-5, ICD-10/11) and national diagnostic manuals and guidelines classify developmental disorders as mental illnesses. Because of this, many doctors, in full compliance with the guidelines, ignore medical problems in such children, do not conduct necessary research, and ignore parents' complaints about the manifestations of various pathological conditions in the child, then attributed to autism. As a result, this category of young patients around the world remains deeply under-researched and deprived of full-fledged medical care. Under these conditions, the NEM could provide invaluable assistance in conducting a comprehensive preliminary diagnosis of gross neurological disorders.
REFERENCES
- Maximova AA (2020) The relationship of somatic pathological changes with negative behavior of asd children. Digital Scientific Journal 7: 1-9.
- Maximova AA (2020) The influence of pathological changes in the intestinal microbiocenosis on the appearance or intensification of negative behavior in children with ASD. International Research Journal.
- Maximova AA (2020) Effects of thyroid dysfunction and cortisol imbalance on the cognitive and mental development of children with autism spectrum disorder. International Research Journal.
- Tellman-Ward GR, Bannister CM, Lewis MA, Shaw J (1997) The incidence of chronic headache in children with shunted hydrocephalus. Eur J Pediatr Surg. 1997 Dec 1: 12-14.
- Di Tommaso MC (2012) A comparative study of bipolar disorder and attention deficit hyperactivity disorder through the measurement of regional cerebral blood flow. J Biol Regul Homeost Agents 26: 1-6.
- Mahdavinasab SM, Saghazadeh A, Motamed-Gorji N, Vaseghi S, Mohammadi M-R et al. (2019) Baclofen as an adjuvant therapy for autism: a randomized, double-blind, placebo-controlled trial. Eur Child Adolesc Psychiatry 28: 1619-1628.
- Fokin VF (2003) Ponomareva N.V. Energetic physiology of the brain. M. Antidor Publishing House Page no: 288.
Citation: Maximova AA (2021) Neuroenergy Mapping Diagnostic Capabilities in Hypoxic Brain Lesions. J Angiol Vasc Surg 6: 057.
Copyright: © 2021 Alexandra Alexandrovna Maximova, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

