Occupational Radiation Dose for Medical Workers at Al-Ahli Hospital in West Bank- Palestine
*Corresponding Author(s):
Muntaser S AhmadNuclear Medicine Department, Al-Ahli Hospital, Farsh Al Hawa, Hebron, Palestine
Tel:+970595107857,
Email:wmuaser@gmail.com
Abstract
Introduction: The radionuclides have been used in diagnosis and treatment to improve health services. The aim of current study was established to determine the occupational dose of nuclear medicine staff at Al-Ahli Hospital in west bank.
Materials and Methods: The data analysis of occupational medical workers exposure in nuclear medicine (NM) at the nuclear medicine department (N.M.D) at Al-Ahli hospital, Palestine is presented for the time interval three months between 15/9/2018 to 15/12/2018.The whole- body exposure doses of the workers were measured by using the thermoluminescent dosimetry (TLD) technique. The data analysis demonstrates that all values of the occupational dose were below the relevant dose limits.
Results: The Medical physicist have the highest radiation exposure 4.4 mSv where the technician has moderate dose 1.352 mSv, and the nurse has the lowest dose 1.154 mSv. The quarter annual average effective doses in NM has been found well below the maximum permissible dose (MPD) with no over-exposure detected. This dropped of effective dose is outcome of radiation protection improvement during the recent year.
Conclusion: The results of the measured annual dose were well below the international recommended dose limit.
Keywords
Effective dose; NM; MPD; TLD
INTRODUCTION
Newly, the source of radioactive material have been applied in various applications such as research, education, agriculture, industries, and medicine. The radionuclides have been used in diagnosis and treatment to improve health services [1]. The occupational and medical exposure are considered as the main types of the radiation exposure in ionizing radiation section [2]. The severity of cancer risk is directly dependent on the absorbed dose. Therefore, it is essential to establish a model to define the effects of low radiation dose onto carcino-genic effects [3].
The main objective for radiation protection which improved by the International Commission on Radiological Protection (ICRP) is to develop a standard projection system which can be used in medical, occupational, environmental, and exposure controls against radiological accidents. Through this system, the radiation exposure limitation were involved for different practices [4]. The occupational exposures can define as the exposure for the workers through dealing with the ionizing radiation whenever on the work time [5]. The using of radioactive material in the medical application involves using machine, preparing radioactive material, and handling with unsealed radioactive, and dealing with the radioactive waste [6].
The radiation dose estimate for the workers considered an essential factor for the organizations to assess the radiation risks and establish protective measures [7,8]. The staff in Nuclear Medicine (N.M) department receive a high radiation doses comparing with other medical applications. Moreover, the staff in NM involving the nuclear medicine specialist, medical physics, nuclear medicine technologist (NMT), nurses, and others are received the exposure dose from man-made radiation sources. Hence, the routine monitoring for radiation exposures should be followed [9,10].
In the report of ICRP the occupational radiation is expressed the terms of effective dose and equivalent dose for extremities and eye lens [11]. The personal equivalent dose (H10) is the essential operational quantity in the radiation protection field and it can define as the effective dose (received dose) by the tissue at depth 10 mm from the skin surface, it is represented as the whole-body dose.
As the following of the basic safety standards (BSS) recommendations, the H should apply to both extremities through operational quantity Hp (0.07) and for whole body through operational quantity Hp (10). Usually, the whole-body dose scale is used for individual monitoring of external radiation, and it reported in terms of equivalent personal dose Hp (10). Hp (10) gives a conservative measure for effective dose of radiation events at the front of the body [12]. Following the ICRP roles, the annual effective dose for occupational exposure should not excess than 20 mSv through the averaging of 5 years, while the maximum permissible dose in an individual year should not excess than 50 mSv [13].
There are various devices used to estimate the staff dose, thermo-luminescent dosimetry (TLD) is considered as the most suitable method to measure the personal dosimeters [14]. In most conventional diagnostic nuclear medicine departments (NMD), the procedures using Tc-99m for diagnostic scintigraphy are predominate. The current study objective was shared between investigation of the occupational radiation dose history among the workers in NMD at Al-Ahli hospital, and to compare these values with standard personal doses which recommended by the ICRP.
MATERIALS AND METHODS
NMD at Al-Ahli hospital consists of several rooms and can be distributed into three parts. The first part contains the following rooms; the first room is located at the beginning of the department; it contains the Gamma- Camera machine. In the same room, it contains the machine operating control; the second room locates in front of the first room, it containing the hot-lab room which used to prepare the radiopharmaceutical materials; the third room it located in front of the hot-lab room, this room using for the patients injection (injection room).
The second part consist of the department entrance, the reception section, the rest room for the patient’s companions, and the patient’s toilet. The third part consists of four isolated rooms which used for patient’s treatment, through using Iodine -131. Room 1 and room 2 were located beside each other, and room 3 and room 4 were located beside each other in the opposite of the first two rooms.
One medical physicist has more than 15 years of experience or technical staff (preparation) who is preparing the radio-pharmaceutical material through elution of Tc-99m from molybdenum/technetium generators. One nuclear medicine technologist (NMT) with 4 years’ experience or technical staff (operators), and two nurses with more than 10 years of experience for each one, were monitored during the tasks of preparation and injection of the radiopharmaceuticals into patients undergoing diagnostic examination.
The study was used TLD device. The TLDs contains a card with holders including a detector crystal of LiF:Mg:Ti Card (TLD-100), which use to determine the deep doses and skin measurements.
The TLDs were distributed in different areas includes seven areas; Area 1 were put in the hot lab (radiopharmaceuticals preparing room); Area 2 were put in the front of the technologist who using the operating Gamma-Camera machine; Area 3 was located in the front of patient in the injection room; Area 4 were located in the front of two isolated rooms (room 1 and room 2) which used for patient treatment using Iodine-131; Area 5 was located in front of the second two isolated rooms ( room 3 and room 4); Area 6 was located on the front of the reception room; and Area 7 was located in the patients toilet. All TLDs were placed on the high one meter above the ground and one meter far from the interest areas as mentioned above.
The TLDs calibration process was totally automated in the reader which represented by the Palestinian health ministry to significantly reduce time and costs and then all TLDs were taken back to the N.M.D for using. A Model 6600 TLD Reader with suitable computer program were used to estimate the TLDs reading. The Area monitoring, or workplace monitoring were taken from N.M.D at Al-Ahli hospital for the period from 15/09/2018 to 15/12/2018. One non-irradiated TLD of the same type was used to measure the area monitoring doses for estimating the background radiation dose was all of the other measurements were subtracted from this measure.
The TLDs cards were read out on a Harshaw 6600 automated TLD reader. The TLD card labels were included a bar-coded with the area number. The calibration of the TLDs was performed in the health physics division (HPD) in Ramallah-West Bank. The doses of the received TLDs are measured in the TLD Reader by using hot nitrogen gas flow.
RESULTS AND DISCUSSION
Occupational doses at N.M.D
The results for the equivalent doses for nuclear medicine workers were determined and presented in Table 1.
|
Area’s |
Background |
Results |
|
Area 1 |
182.95 E-3 |
4643.4 E-3= 4.4 mSv |
|
Area 2 |
182.95 E-3 |
381.39 E-3=0.198 mSv |
|
Area 3 |
182.95 E-3 |
691.03 E-3=0.508 mSv |
|
Area 4 |
182.95 E-3 |
604.68 E-3=0.421 mSv |
|
Area 5 |
182.95 E-3 |
408.04 E-3=0.225 mSv |
|
Area 6 |
182.95 E-3 |
197.93 E-3=0.014 mSv |
|
Area 7 |
182.95 E-3 |
243.08 E-3=0.06 mSv |
Table 1: Distribution of the TLDs dose (mSv) by medical staff in N.M.D.
Table 1 shows that the effective dose during the study period for the nuclear medicine workers who works in area 1,2, and 3 ranged from 0.198 to 4.4 mSv at Hp(10). The physists worked in area 1 alone and there are no other works inter this area. The NMT worked in area 2 alone, while the area 3 sharing between the nursing and the NMT for preparing and injecting the dose to the patients, respectively.
It can consummated that all of measurement were below the dose limitation general, it was noted that the medical physicist who work in the area 1 received comparatively higher rate (>3 mSv) than the other nuclear medicine workers due to their main job and responsibilities to prepare the radioactive materials in the hot-lab area which consist of radioactive generators and other radioactive materials, and give it to the NMT to inject the patients.
In the same table, it shows that the effective dose during the study period for the nuclear medicine workers in area 4 and 5 ranged from 0.225 to 0.421 mSv. The NMT and the nurses sharing these two-area’s due to give the ablation dose for the patient and follow up the patient during stay in the isolation room, respectively. The dose in the fifth area is about twice as high as the fourth area, and that is because the load for both room 1 and room 2 which have been received 19 isolated patients while room3 and room 4 have been received 11 isolated patients in the same period. The reception dose reached to 0.014 mSv, while the patients’ toilet doses reached to 0.06 mSv.
The results for the total dose for the nuclear medicine workers were determined and presented in Table 2, and Figure 1.
|
Total number of workers |
Working group |
Hp (10) |
|
1 |
physicist |
4.4 |
|
1 |
technician |
1.352 |
|
2 |
nurse |
1.154 |
|
1 |
reception |
0.06 |
Table 2: Distribution of the dose (mSv) by medical staff in the N.M.D.
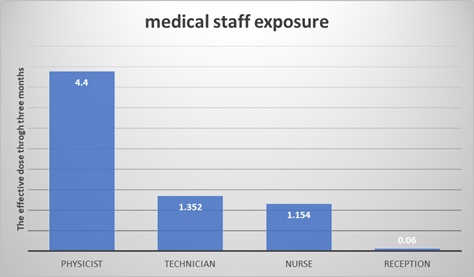
Figure 1: The medical staff exposure doses distribution.
Annual the system used in the HPD for the minimum detection level (MDL) is 0.05 mSv for a three months monitoring after deducting the background radiation. If the Hp(10) which represented the effective dose for occupational exposure less than the MDL thus the area considered un-exposed. In this study, all the nuclear medicine workers are exposed at a various ratio related the place and the responsibilities for each worker. However, the nuclear medicine workers had a relatively higher occupational dose, but their dose was still below the recommended dose limit (20 mSv/year).
The available worldwide annual effective dose for occupational exposure in nuclear medicine department during a block of four years is given in Table 3.
|
Annual average effective dose (mSv) |
||||
|
Country |
Period |
Monitored |
Exposure worker |
Reference |
|
Worker |
||||
|
Poland |
1991-2009 |
0.7 |
2.2 |
Piwowarska-Bilska et al [15] |
|
Ghana |
2000-2009 |
- |
0.72 |
Hasford et al [16] |
|
France |
2005-2011 |
0.31 |
0.83 |
Feuardent et al [17] |
|
Bangladesh |
2010-2014 |
0.22 |
0.55 |
Rahman et al [13] |
|
Kuwait |
2008-2009 |
1.03 |
1.06 |
Brindhaban et al [9] |
|
Iran |
2009-2011 |
1.4 |
1.94 |
Motevalli et al [6] |
|
Pakistan |
2007-2011 |
- |
1.12 |
Masood et al [18] |
|
Kingdom of Saudi Arabia |
2009-2010 |
- |
1.56 |
Nassef et al [19] |
Table 3: Comparison of annual average effective dose of monitored and exposed workers with other countries.
CONCLUSION
The presented data analysis concerning the occupationally exposed medical staff suggests that all the occupationally exposed workers has received radiation doses well below the permissible limits. This notice could be used to improve the radiation protection in the N.M.D and is indicative of the possibility of further reductions in subsequent years with the implementation of changes in regulatory standards, new technologies, changes in work practices and other radiation protection programs. Efforts are being concerted regarding the optimization of protection procedures and schemes to circumvent further any unnecessary radiation exposures. The limitations of this study are represented in the short duration of data collection, also there have not measurement of the hand dose by using the ring detectors.
CONTRIBUTORS
All authors contributed to the conception or design of the work, the acquisition, analysis, or interpretation of the data. All authors were involved in drafting and commenting on the paper and have approved the final version.
FUNDING
This study did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
CONFLICT OF INTEREST
The author have no conflict of interest.
DISCLOSURE
The author did not receive any type of commercial support in forms of either compensation or financial support for this study.
ETHICAL APPROVAL
Informed consent was obtained from all participants.
REFERENCES
- Jalilian AR, Beiki D, Hassanzadeh-Rad A, Eftekhari A, Geramifar P, et al. (2016) Production and Clinical Applications of Radiopharmaceuticals and Medical Radioisotopes in Iran. Semin Nucl Med 46: 340-358.
- Morgan WF, Bair WJ (2013) Issues in low dose radiation biology: the controversy continues. A perspective. Radiat Res 179: 501-510.
- Wakeford R (2015) From Hiroshima and Nagasaki to Fukushima 1 Long-term eff ects of radiation exposure on health. Lancet 386: 469-478.
- Cousins C, Miller DL, Bernardi G, Rehani MM, Schofield P, et al. (2011) International commission on radiological protection. ICRP publication 120: 1-125.
- Gadhi MA, Fatmi Sh, Gadhi M Sh, Mahmood U, Shakil M, et al. (2016) Variation of annual effective dose from external ionizing radiation among Variation of annual effective dose from external ionizing radiation among radiation workers of Bahawalpur Institute of Nuclear Medicine and Oncology ( BINO ), Pakistan. Int J Radiat Res 14: 229-235.
- Motevalli SM, Borhanazad AM (2015) Assessment of occupational exposure in medical practice in tehran , iran. Rom Rep Phys 67: 431-438, 2015.
- Villoing D, Yoder RC, Passmore C, Bernier MO, Kitahara CM. (2018) A US multicenter study of recorded occupational radiation badge doses in nuclear medicine. Radiology 287: 676-682.
- Bernier MO, Doody MM, Van Dyke ME, Villoing D, Alexander BH, et al. (2018) Work history and radioprotection practices in relation to cancer incidence and mortality in US radiologic technologists performing nuclear medicine procedures. Occup Environ Med 75: 533-561.
- Al-Abdulsalam A, Brindhaban A (2014) Occupational radiation exposure among the staff of departments of nuclear medicine and diagnostic radiology in Kuwait. Med Princ Pract 23: 129-133.
- Sabol J, Hudzietzová J, Fülöp M (2015) Imaging in nuclear medicine: Monitoring of skin doses of workers. EHB pp. 1-4.
- Shore RE (2016) Radiation and cataract risk: Impact of recent epidemiologic studies on ICRP judgments. Mutat Res 770: 231-237.
- Kopec R, Budzanowski M, Budzy?ska A, Czepczynski R, Dziuk M, et al. (2011) On the relationship between whole body, extremity and eye lens doses for medical staff in the preparation and application of radiopharmaceuticals in nuclear medicine. Radiat Meas 46: 1295-1298.
- Rahman MS, Begum A, Hoque A, Khan RK, Siraz MMM (2015) Assessment of whole-body occupational radiation exposures in nuclear medicine practices of Bangladesh during 2010-2014. Iran J Nucl Med 24: 51-58.
- Carinou E, Ferrari P, Bjelac OC, Gingaume M, Merce MS, et al. (2015) Eye lens monitoring for interventional radiology personnel: dosemeters, calibration and practical aspects of H p (3) monitoring. A 2015 review. J Radiol Prot 35: 17-34.
- Piwowarska-Bilska H, Birkenfeld B, Gwardy? A, Supi?ska A, Listewnik MH, et al. (2011) Occupational exposure at the Department of Nuclear Medicine as a work environment: A 19-year follow-up. Pol J Radiol 76: 18–21.
- Hasford F, Owusu-Banahene J, Amoako JK, Otoo F, Darko EO, et al. (2012) Assessment of annual whole-body occupational radiation exposure in medical practice in Ghana (2000–09). Radiat Prot Dosimetry 149: 431-437.
- Feuardent J, Scanff P, Crescini D, Rannou A (2013) Occupational external exposure to ionising radiation in France (2005–2011). Radiat Prot Dosimetry 157: 610-618.
- Masood K, Ahmad M, Zafar J, ul Haq M, Ashfaq A, et al. (2012) Assessment of occupational exposure among Pakistani medical staff during 2007–2011. Australas Phys Eng Sci Med 35: 297-300.
- Nassef MH, Kinsara AA (2017) Occupational radiation dose for medical workers at a university hospital. J Taibah Univ Sci 11: 1259-1266.
Citation: Ahmad MS, Zeyadeh SL, Odah R, Oglat AA (2020) Occupational Radiation Dose for Medical Workers at Al-Ahli Hospital in West Bank- Palestine. J Nucl Med Radiol Radiat Ther 5: 017.
Copyright: © 2020 Muntaser S Ahmad, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.