
Olfactory Stimulation Improves Geriatric Cognitive Function through Evaluation of Auditory Perception
*Corresponding Author(s):
Yea-Jyh ChenSchool Of Nursing, College Of Health & Human Services, University Of North Carolina Wilmington, 601 S College Road, Wilmington, NC 28403, United States
Tel:+1 9109620584,
Fax:+1 9109624921
Email:chenyj@uncw.edu
Abstract
This secondary data analysis aimed to understand auditory perception and determine the efficacy of using Olfactory Stimulation (OS) to improve perceptual cognition in older people. We abstracted the data from available healthy older Taiwanese adults (24 OS and 20 control). The OS group received neutral nasal inhalation before each meal for 12 days. All participants completed the Assessment of Auditory Perception for Conceptual Recognition short form (AAPCR-S) twice, at pre-test and post-test, reflecting their cognitive function. The OS participants had enhanced auditory conceptual ability compared to pre-test (p< 0.001), but the control did not. The interaction effect on auditory perception significantly differed by time with a large effect size (p= 0.004, ηp2 = 0.18). No difference was found between groups. The results illustrated that OS using odor and flavor inhalation was effective to improve auditory conceptual ability for healthy older adults over time. We suggest that, with a normal olfactory sensation, older adults will integrate physical mechanisms into an effective network of auditory and cognitive processing along with improving swallowing function. It is imperative to include systematic sensation protocol with comprehensive tests for auditory and cognitive processing while evaluating changes on age-related cognitive function.
Keywords
Cognitive function; Geriatric auditory perception; Olfactory stimulation; Taiwanese
Introduction
Olfactory Stimulation (OS) has been suggested to have promising effects in improving cognitive function in people with cognitive decline or dysfunction [1,2] and swallowing in healthy older adults [3]. Geriatric olfactory sense fades gradually and imperceptibly [4,5] as a natural course cycle that may frequently co-occur with dementia and age-related hearing loss. Our prior laboratory evidence demonstrated that volatile molecules via olfaction were able to activate the neuronal reactivities in the brainstem in relation to swallowing [6], and it could potentially also be co-activated in cognitive areas around the orbitofrontal and limbic lobes. The auditory conceptual assessment measures the effects on the central processing system to determine whether maximum outcomes enhance the associated domains, i.e., cognition. Therefore, changes in auditory perception, in particular, were examined in our study to measure cognitive function after olfactory stimulation.
The Assessment of Auditory Perception for Conceptual Recognition (AAPCR) was a cognitive test used to determine conceptual knowledge of semantic memory in people with neurophysiological damage [7]. This computer-based instrument is culturally sensitive and requires participants to identify non-speech environmental sounds in given situations. It was designed as a standardized means to benefit individuals with some degrees of auditory processing difficulty in communication, which is commonly seen in the older population [8,9]. The psychometrics of the AAPCR were established, including high criterion-related validity with the Montreal Cognitive Assessment-Taiwanese version [8-10]. A higher AAPCR score indicates better auditory conceptual ability. This report presents auditory perception ability in healthy older adults and tests the hypothesis using OS yields improved perceptual cognition.
Materials and Methods
This secondary data analysis was part of the geriatric swallowing projects [3]. Healthy older Taiwanese adults (24 in the experimental [OS] group and 20 in the control group) were included without baseline differences in demographic characteristics (i.e., age, gender, education). The OS group received neutral nasal inhalation before each meal for 12 days. All participants were evaluated by their conceptual ability in cognition using the AAPCR-S at baseline (pre-test) and at the end of the study (post-test). Considering the limited attention on aging, the AAPCR-S, which contains a total of 36 items including the simple (Test 1; 12 items) and complex (Test 2; 24 items) environmental sound identification tests, was adequately applied [11]. Likewise, using the study sample, the AAPCR-S was shown to be reliable and competitive with the AAPCR (test-retest reliability r= 0.75, p < 0.001). It indicates the status of any impaired auditory perception among healthy older adults in this study, reflecting a poor cognitive conceptualizing ability. During the assessment, the examinee was asked to point to the expected picture from four displayed pictures after the target sound was heard. The potential score of the AAPCR-S ranges from 0-36. Within and between group differences in auditory perception were compared by two-sample independent t-test and paired t-test. A mixed-design, two-way 2 x 2 repeated measures analysis of variance (ANOVA) further evaluated the combined effects to expand our understanding of how effective the intervention was, associated with geriatric auditory recognition over time. The significance level was set at < 0.05.
Results
For the OS participants, the post-test AAPCR-S score increased, indicating enhanced auditory conceptual ability compared to pre-test (M= pre-test 30.29 vs. post-test 32.63, t= -4.12, p < 0.001), but was not significant in the control group (M= pre-test 32.05 vs. post-test 31.65, p> 0.05). The group x time interaction effect significantly differed on auditory perception by time with large effect size [F (1,42) = 9.25, p=0.004, ηp2 = 0.18]. Figure 1 displays the crossover interaction effects with the opposite direction in the AAPCR-S scores. The OS group had the higher mean score at post-test compared to the decreased mean score shown in the control group. There were no significant differences between groups on AAPCR-S in pre- and post-tests (p> 0.05).
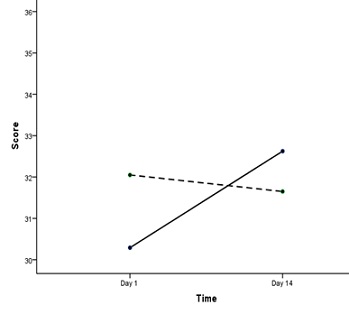 Figure 1: Auditory conceptual ability had a significant interaction effect from olfactory stimulation (yes/no) and time (day 1 vs. day 14). [Note. Solid line: Older adults with OS; Dashed line: Older adults without OS (control). Day 1: pre-test; Day 14: post-test.]
Figure 1: Auditory conceptual ability had a significant interaction effect from olfactory stimulation (yes/no) and time (day 1 vs. day 14). [Note. Solid line: Older adults with OS; Dashed line: Older adults without OS (control). Day 1: pre-test; Day 14: post-test.]
Discussion
This study analysis aimed to identify the effects of olfactory stimulation on cognitive changes according to enhanced auditory perception ability among community-dwelling older adults in Taiwan. The results represent a high likelihood of acquiring cortical changes in general older adults. The experiment participants demonstrated a great improvement in auditory conceptual performance after the olfactory intervention, whereas control individuals had negative responses (reduced scores) on cognitive assessment at post-test. This result illustrates that using olfactory stimulation improves and/or delays physical degeneration in age-related cognitive performance.
In our findings, the OS older individuals with increased auditory perception had gained the benefit of enhancing their factual knowledge and remembering events by odor and flavor smelling, which was consistent with previous evidence [7,12]. The improved auditory conceptual ability in the OS group was determined by the performance of declarative memory in the AAPCR-S; however, the older adults in the control group did not show improvements. This implies that the OS older adults might have better sensory and perceptual integration, leading to neural network dynamics, than the control adults [13,14]. That said, the between-group difference was not statistically significant.
Cognition decline has been positively linked to age-related physical changes that reinforce the development of unpleasant mild cognitive impairment or age-related auditory processing disorders. From this standpoint, our attempt to use auditory conceptual performance as cognitive function to determine the effects of olfactory stimulation was innovative and subtle. According to Fitten [15], a parallel relationship was suggested between cognitive decline and physical frailty. Frailty among older people predisposes psychological deficits relevant to predicting cognitive impairment. Similar results in studies by Yang et al. [16] and LaGorio et al. [17] confirmed that cognitive impairment in aging was associated with dysphagia. It shows that these sensory dysfunctions are interrelated, and also that body systems benefit from reciprocal interactions among good sensation functioning [4,13,14].
Declined functional capacity varies by individual among healthy older people. Also, the significant interaction effect between time and group, given personal variations on aging frailty, may affect the study control participants being desensitized with unchanged and/or negative cognitive performance. This explains and reflects the incompatible slopes on post-test (Figure 1). Our finding is limited by the secondary data analysis. Future studies with a larger sample size should consider individual variations and include comprehensive tests for auditory and cognitive processing. Together with our previous study findings [3], this analysis reveals that healthy older people with olfactory stimulation prior to each meal could benefit not only their swallowing function but also their cognition-related abilities.
Conclusion
Olfactory stimulation using odor and flavor inhalation was effective in improving auditory conceptual ability for healthy older adults. Our study employed the auditory perception measure to determine cognitive function with regards to OS. It is imperative to consider using a systematic sensation protocol (e.g., olfaction, audition, perception etc.) while evaluating changes to age-related cognitive function. Overall, OS may have the potential to modulate geriatric cognitive functional decline in addition to swallowing function. We conclude that, with a normal olfactory sensation, older adults’ physical mechanisms will integrate into an effective network of auditory and cognitive processing and will improve swallowing function.
Conflict of Interest
There is no known financial or other conflict of interest to disclose by authors.
Acknowledgement
The authors would like to first thank all study participants and research assistant, LC Lin, who assisted during data collection.
References
- Agatonovic-Kustrin S, Kustrin E, Morton DW (2019) Essential oils and functional herbs for healthy aging. Neural Regen Res 14: 441-445.
- D'Andrea F, Tischler V, Dening T, Churchill A (2022) Olfactory stimulation for people with dementia: A rapid review. Dementia (London) 21: 1800-1824.
- Chen YJ, Chen YT, Lin LC, Chen SC, Wang CT, et al. (2021) Effects of olfactory stimulation on swallowing function in Taiwanese older adults. Gerontol Geriatr Med 7: 23337214211015449.
- Boesveldt S, Postma EM, Boak D, Welge-Luessen A, Schöpf V, et al. (2017) Anosmia-A clinical review. Chem Senses 42: 513-523.
- Jang SS, Choi JS, Kim JH, Kim N, Ference EH (2022) Discordance between subjective and objective measures of smell and taste in US adults. Otolaryngol Head Neck Surg 166: 572-579.
- Chen YT, Chen LY, Renn TY, Cheng MS, Wang CT, et al. (2022) Olfactory stimulation successfully improves swallowing function of aged rats through activating central neuronal networks and downstream DHPR-RyR-mediated neuromuscular activities. J Gerontol A Biol Sci Med Sci 77: 235-242.
- Chen WJ (2018) The reliability and validity of the assessment of auditory perception for conceptual recognition (AAPCR). Unpublished master’s thesis, National Taipei University of Nursing and Health Sciences, Taipei, Taiwan.
- Chen YC, Chen YT, Chang LC, Chen YJ (2022) Evaluating conception by the Assessment of Auditory Perception for Conceptual Recognition (AAPCR). Poster presented at the Sigma’s 33rd International Nursing Research Congress, Edinburgh, Scotland.
- Bayles K, McCullough K, Tomoeda CK (2020) Cognitive-Communication Disorders of MCI and Dementia: Definition, Assessment, and Clinical Management (3rdedn.). Plural Publishing, California, USA.
- Tsai CF, Lee WJ, Wang SJ, Shia BC, Nasreddine Z, et al. (2012) Psychometrics of the Montreal Cognitive Assessment (MoCA) and its subscales: Validation of the Taiwanese version of the MoCA and an item response theory analysis. Int Psychogeriatr 24: 651-658.
- Chen YT, Lai YC, Chen WJ, Lin HT, Chang CF (2022) Clinical application of the Assessment of Auditory Perception for Conceptual Recognition (AAPCR) and its psychometrics. Poster presented at Annual conference of Taiwan Speech-Language-Hearing Association, Taipei, Taiwan.
- Ayaz M, Sadiq A, Junaid M, Ullah F, Subhan F, et al. (2017) Neuroprotective and anti-aging potentials of essential oils from aromatic and medicinal plants. Front Aging Neurosci 9: 168.
- Brooks CJ, Chan YM, Anderson AJ, McKendrick AM (2018) Audiovisual temporal perception in aging: The role of multisensory integration and age-related sensory loss. Front Hum Neurosci 12: 192.
- Rutherford BR, Brewster K, Golub JS, Kim AH, Roose SP (2018) Sensation and psychiatry: Linking age-related hearing loss to late-life depression and cognitive decline. Am J Psychiatry 175: 215-224.
- Fitten LJ (2015) Psychological frailty in the aging patient. Nestle Nutr Inst Workshop Ser 83: 45-53.
- Yang EJ, Kim KW, Lim JY, Paik NJ (2014) Relationship between dysphagia and mild cognitive impairment in a community-based elderly cohort: The Korean longitudinal study on health and aging. J Am Geriatr Soc 62: 40-46.
- LaGorio LA, Shah R, Buchman A, Leurgans SE, Bennett DA (2017) Association between impaired swallowing and cognition in healthy older adults. Innov Aging 1: 154.
Citation: Chen YT, Chen YJ, Lai YC, Chang HM (2023) Olfactory Stimulation Improves Geriatric Cognitive Function through Evaluation of Auditory Perception. J Gerontol Geriatr Med 9: 164.
Copyright: © 2023 Yea-Tzy Chen, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

