
Omental Infarction: Unusual Complication after Laparoscopic Proctocolectomy
*Corresponding Author(s):
Awni D ShahaitDepartment Of Surgery, Wayne State University School Of Medicine, Michigan, United States
Tel:+1 3137458778,
Email:Gmostafa@med.wayne.edu
Abstract
Omental Infarction is an under-explored origin of acute abdominal pain and has uncertain etiology. Because of its low incidence and nonspecific presentation, it can be difficult to diagnose. However, the increasing use of CT scans in patient evaluation has unveiled this phenomenon. We present the first case of postoperative omental infarction after laparoscopic proctocolectomy with end ileostomy in a 71-year-old male patient, who was successfully treated by removal of the infarct.
Keywords
Colectomy; Laparoscopy; Omental infarction; Secondary
BACKGROUND
Although the precise cause of omental infarction is not well defined, the proposed mechanism states that blood flow is interrupted and is followed by edema and venous stasis, culminating with hemorrhagic necrosis [1-3]. Omental Infarction which also called “The Great Impersonator” can mimic wide array of disease, which make it difficult to catch. Over all, it is uncommon entity and most reported cases are primary [4]. Omental infarction can be classified into primary or secondary based on its etiology. Primary omental infarction is not precipitated by a specific cause and may be linked to risk factors including obesity, vibration occupations, laxative use, and sudden changes in position [1,5]. Secondary omental infarction is caused by abdominal surgery (laparoscopic or open), trauma, malignancy, and intraabdominal masses. In this report, we present the first case of postoperative omental infarction following laparoscopic proctocolectomy for ulcerative colitis.
CASE PRESENTATION
A 71-year-old male patient, known to have a longstanding history of ulcerative colitis, was followed closely by colonoscopy every 3-5 years. The last colonoscopy was performed in 2014 and showed low-grade dysplasia in random biopsies from the rectum. Repeated colonoscopies with random biopsies did not show any dysplasia. After discussing the case with the gastroenterologist, surgeon, and the family, it was decided to proceed with prophylactic laparoscopic proctocolectomy with end ileostomy given that the patient has a ulcerative colitis for long time and that will increase risk of colon cancer. Moreover, the health status of patient is acceptable at this stage to undergo major procedure. On physical examination, the abdomen was soft, with no scars and no tenderness. Vital signs were within normal limits and his BMI was 30.9 Preoperative labs are listed in Table 1.
|
WBC |
7.0109/L |
|
Hemoglobin |
12.0 g/dL |
|
Platelets |
219 109/L |
|
Creatinine |
1 mg/dL |
|
Sodium |
138 mEq/L |
|
Potassium |
4.4 mEq/L |
|
Albumin |
4.4 U/L |
Table 1: Preoperative laboratory.
The procedure was performed without acute complications. The hospital course was uneventful, and the patient was discharged to the nursing facility after he tolerated diet and his ileostomy was functioning well.
Two weeks later, the patient visited the Emergency Department (ED) for left upper quadrant abdominal pain that was continuous, not radiating, and gradually increasing in severity. An appropriate workup was performed, including abdominal and pelvic CT scans with contrast, which showed an inflammatory mass in the left upper quadrant (Figure 1 and Figure 2). Suspicion for omental infarction was raised, and conservative management was initiated with NSAIDs. The patient improved and was discharged shortly. Thereafter, the patient visited the ED multiple times for the same complaint, with failure of medical management. After discussing the situation with the patient and his family, the decision was made to proceed with diagnostic laparoscopy, which revealed omental infarction. The omental infarction was evacuated, and the pathology report was consistent with our diagnosis.
 Figure 1: Axial cut showing large inflammatory mass in the left side (black hollow arrow).
Figure 1: Axial cut showing large inflammatory mass in the left side (black hollow arrow).
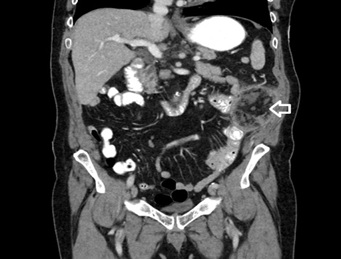 Figure 2: Coronal cut showing inflammatory mass in the left upper quadrant (white hollow arrow).
Figure 2: Coronal cut showing inflammatory mass in the left upper quadrant (white hollow arrow).
The hospital course was uneventful. The pain was alleviated, the patient tolerated his diet, and the ileostomy was functioning well. Subsequent follow up in the clinic showed that the patient was doing well, with a return to his baseline activity. Multiple phone calls with the patient to assess his status till 3 years out from surgery, he stated that he is doing well and abdominal pain again.
DISCUSSION
Acute abdominal pain due to omental infarction is becoming more commonly diagnosed with the implementation of CT scans in patient evaluations. The condition may present with a wide array of symptoms, though patients usually present with subacute pain and no accompanying fever or leukocytosis [6]. According to published data, omental infarctions tend to be right-sided, primarily due to a longer and more mobile omentum on the right side of the abdomen [1,2]. This poses a challenge to its diagnosis, which is mostly achieved intraoperatively. Though the true incidence has not been reported with roughly about 400 cases reported in general and few reported as postoperative cases, it is more common in adults and male patients. (Male: female ratio is 2-2.5:1) [1,3,6].
Regarding postoperative omental infarction, some have proposed that the interruption in blood flow to the greater omentum occurs during surgical manipulation or postoperative healing [5,7]. Kerr, et al. also stated that omental infarctions were found in both open and laparoscopic operations. However, it is unknown whether a laparoscopic approach leads to a lower incidence of omental infarction [6].
In a study by Kerr, et al. 15 patients had CT scan findings of omental infarctions after colonic resection. Most of the reported colonic surgeries were right hemicolectomy, and they reported only one case of open panproctocolectomy. For the last surgery, the CT scan was performed because of concerns due to rising serum tumor markers 6 months after the procedure, and it was managed conservatively [6]. Here we report the first case of left-sided omental infarction following laparoscopic proctocolectomy for ulcerative colitis, which was managed with surgical intervention after failure of conservative management.
No consensus exists with regard to the proper management for this disease entity [4,8,9]. Most published reports favor conservative management with anti-inflammatory drugs and serial follow-up with imaging. Others advocate for early surgical intervention (laparoscopic approach was preferred) to achieve an accurate diagnosis, rule out abscess formation, and relieve the patient’s pain [1,2].
REFERENCES
- Park TU, Oh JH, Chang IT, Lee SJ, Kim SE, et al. (2012) Omental infarction: case series and review of the literature. J Emerg Med 42: 149-54.
- Schwartzman GJ, Jacobs JE, Birnbaum BA (2001) Omental infarction as a delayed complication of abdominal surgery. Clinical Imaging. 25: 341-343.
- McCusker R, Goh DW (2018) Omental infarction: a case of a whole omental infarct. ANZ J Surg 88: 107-108.
- Buell KG, Burke-Smith A, Patel V, Watfah J (2017) Omental Infarction: The Great Impersonator. Cureus 9: 1940.
- Arigliani M, Dolcemascolo V, Nocerino A, Pasqual E, Avellini C, et al. (2016) A Rare Cause of Acute Abdomen: Omental Infarction. J Pediatr 176: 216.
- Kerr SF, Hyland R, Rowbotham E, Chalmers AG (2012) Postoperative omental infarction following colonic resection. Clinical Radiology 67: 134-139.
- Fuentes PAS, López VL, Febrero B, Ramírez P, Paricio PP (2015) Omental infarction: Surgical or conservative management? Cir Esp 93: 475-477.
- Lindley SI, Peyser PM (2018) Idiopathic omental infarction: One for conservative or surgical management? J Surg Case Rep 2018: 95.
- McMillen B, Hekman DP, Nguyen MTT, Grewal D (2019) Idiopathic omental infarction: managed conservatively. BMJ Case Rep 12.
Citation: Shahait AD, Alghanem L, Mostafa G (2019) Omental Infarction: Unusual Complication after Laparoscopic Proctocolectomy. J Clin Stud Med Case Rep 6: 076.
Copyright: © 2019 Awni D Shahait, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

