
Journal of Alternative Complementary & Integrative Medicine Category: Medicine
Type: Research Article
Panax notoginseng Enhances Wound Healing Efficiency and Quality on Diabetic Rats
*Corresponding Author(s):
Kevin Kin Man YueSchool Of Chinese Medicine, Hong Kong Baptist University, Hong Kong, China
Tel: +852 34112468,
Email:kkmyue@hkbu.edu.hk
Received Date: Mar 20, 2019
Accepted Date: Apr 09, 2019
Published Date: Apr 16, 2019
Abstract
Diabetic patients are known to have impaired wound healing and a higher risk of diabetic foot ulcer, which may result in amputation. However, drug dressing for promoting wound healing is rarely found. Most commercial dressings can only address the basic needs for diabetes and usually requires a much longer healing time than for non-diabetes. Sanqi, Notoginseng Radix et Rhizoma, is traditional Chinese medicine that shown the effect on treating hemorrhage can be a solution for diabetic wound.
In the in vivo experiment, the alginate dressing with Sanqi can heal the wound 1.5 times faster than the one without it. In this study, the effect of Sanqi on diabetic wound healing in animal model was investigated. In the animal model, SD rats (male: 200g, 2-3 months old) were induced diabetes by intraperitoneal injection, Streptozotocin (STZ) (50mg/kg/day) or sham control (0.1M sodium citrate, pH 4.5), for 2 continuous days. By excising the dorsal skin portion (2cmx2cm), full thickness wounds were created in rats. In each rat, the wound was treated with (a) alginate dressing, and (b) Sanqi alginate dressing. Digital images of the wound site were made twice a week for 3 weeks. The wounds were found 9% faster in terms of wound area percentage decrease than general alginate dressing.
Our results, therefore, suggested Sanqi might contribute in promoting diabetic wound healing efficiency suggesting a new dressing solution to better address chronic wound in a cost-effective manner.
Aims/hypothesis: Sanqi, Latin Pharmaceutical Name is Notoginseng Radix et Rhizoma, a traditional Chinese medicine that shown the effect on treating hemorrhage, may play a role in efficient wound healing in diabetic subjects. We tested whether Sanqi contribute to the healing effect of diabetic wound healing.
Methods: In this study, the effects of Sanqi on wound healing in both diabetic and non-diabetic animals were investigated. In the animal model, SD rats (male: 200g, 2-3 months old) were induced diabetes by intraperitoneal injection, Streptozotocin (STZ) (50mg/kg/day) or sham control (0.1M sodium citrate, pH 4.5) for 2 continuous days. By excising the dorsal skin portion (2cmx2cm), full thickness wounds were created in rats. In each rat, the wound was treated with (a) alginate dressing, and (b) Sanqi alginate dressing. Following the treatment, digital images of the wound site were made twice a week for 3 weeks. HPLC was conducted to indicate the majority active components present in Sanqi, which may participate in the wound-healing event. And the antimicrobial ability of Sanqi in alginate dressing was evaluated.
Results: In both diabetic and non-diabetic animals, higher wound healing rate was found under the treatment of Panax notoginseng when comparing with both positive and negative controls.
Conclusion/interpretation: Our results, therefore, suggested Panax notoginseng might contribute in promoting diabetic wound healing efficiency.
In the in vivo experiment, the alginate dressing with Sanqi can heal the wound 1.5 times faster than the one without it. In this study, the effect of Sanqi on diabetic wound healing in animal model was investigated. In the animal model, SD rats (male: 200g, 2-3 months old) were induced diabetes by intraperitoneal injection, Streptozotocin (STZ) (50mg/kg/day) or sham control (0.1M sodium citrate, pH 4.5), for 2 continuous days. By excising the dorsal skin portion (2cmx2cm), full thickness wounds were created in rats. In each rat, the wound was treated with (a) alginate dressing, and (b) Sanqi alginate dressing. Digital images of the wound site were made twice a week for 3 weeks. The wounds were found 9% faster in terms of wound area percentage decrease than general alginate dressing.
Our results, therefore, suggested Sanqi might contribute in promoting diabetic wound healing efficiency suggesting a new dressing solution to better address chronic wound in a cost-effective manner.
Aims/hypothesis: Sanqi, Latin Pharmaceutical Name is Notoginseng Radix et Rhizoma, a traditional Chinese medicine that shown the effect on treating hemorrhage, may play a role in efficient wound healing in diabetic subjects. We tested whether Sanqi contribute to the healing effect of diabetic wound healing.
Methods: In this study, the effects of Sanqi on wound healing in both diabetic and non-diabetic animals were investigated. In the animal model, SD rats (male: 200g, 2-3 months old) were induced diabetes by intraperitoneal injection, Streptozotocin (STZ) (50mg/kg/day) or sham control (0.1M sodium citrate, pH 4.5) for 2 continuous days. By excising the dorsal skin portion (2cmx2cm), full thickness wounds were created in rats. In each rat, the wound was treated with (a) alginate dressing, and (b) Sanqi alginate dressing. Following the treatment, digital images of the wound site were made twice a week for 3 weeks. HPLC was conducted to indicate the majority active components present in Sanqi, which may participate in the wound-healing event. And the antimicrobial ability of Sanqi in alginate dressing was evaluated.
Results: In both diabetic and non-diabetic animals, higher wound healing rate was found under the treatment of Panax notoginseng when comparing with both positive and negative controls.
Conclusion/interpretation: Our results, therefore, suggested Panax notoginseng might contribute in promoting diabetic wound healing efficiency.
Keywords
Diabetes; Herbal therapy; Notoginseng Radix et Rhizoma; Sanqi; Wound Healing
INTRODUCTION
Diabetes Mellitus (DM) is a chronic metabolic disease that could be characterized by uncontrollable high blood glucose (hyperglycemia). According to the statistics of the International Diabetes Federation, there are currently about 700,000 people suffering from diabetes in Hong Kong, in another word, one in every ten people in Hong Kong suffers from this disease [1]. By 2023, the number of people with diabetes in Hong Kong is expected to increase to 920,000. Approximately 25% of these diabetic patients will develop foot ulcers. More than 6.5 million chronic skin ulcers caused by pressure, venous stasis, or diabetes mellitus in the Unites States annually [2]. Chronic wounds account for an estimated $6-$15 billion annually in US health care costs. There is tremendous pressure on the medical system to develop cost-effective therapies.
Clinically, the aim of the diabetic ulcers management is to provide a moist and clean environment that favors the wound healing [3,4]. It requires offloading the wound by using daily saline or similar dressings to provide a moist wound environment. However, most clinical dressings can only address the basic needs for wound healing while diabetic wounds usually require a longer healing time than for non-diabetes. The healing of wounds in diabetic subject is generally delayed due to peripheral arterial insufficiency, high blood glucose and continuous inflammatory response [5]. Prolonged wound healing causes higher risk of presenting osteomyelitis or cellulitis that may result in amputation.
Sanqi, Notoginseng Radix et Rhizoma, is traditional Chinese medicine that shown the effect on treating hemorrhage. It officially joined the Chinese materia medica during the 16th century [6,7]. Due to its ability to treat all blood disorders, it is the main ingredient of the well-known patent medicine Yunnan Baiyao, which was first marketed in 1902 and remains a favorite emergency remedy for acute bleeding disorders [8]. Increasing experimental and clinical research is being conducted on the medicinal effects of Sanqi in recent years, confirming the wide variety of actions ascribed to the plant in traditional herb primers [9]. The antimicrobial ability based on the Standard Plate Count (SPC) shown that that alginate demonstrated excellent antimicrobial ability and Sanqi had the best antimicrobial ability among all herbs tested. Alginate was able to release Sanqi sustainably which was proved by Colorimetry.
In this report, we hypothesize that Sanqi could promote diabetic wound healing efficiency. Using animal models treated with (a) alginate dressing, and (b) Sanqi alginate dressing, the rate of wound healing was investigated. Using HPLC, the majority active components present in Sanqi was revealed. Our results demonstrated that Sanqi contribute in promoting wound healing efficiency in both diabetic and non-diabetic subjects.
Clinically, the aim of the diabetic ulcers management is to provide a moist and clean environment that favors the wound healing [3,4]. It requires offloading the wound by using daily saline or similar dressings to provide a moist wound environment. However, most clinical dressings can only address the basic needs for wound healing while diabetic wounds usually require a longer healing time than for non-diabetes. The healing of wounds in diabetic subject is generally delayed due to peripheral arterial insufficiency, high blood glucose and continuous inflammatory response [5]. Prolonged wound healing causes higher risk of presenting osteomyelitis or cellulitis that may result in amputation.
Sanqi, Notoginseng Radix et Rhizoma, is traditional Chinese medicine that shown the effect on treating hemorrhage. It officially joined the Chinese materia medica during the 16th century [6,7]. Due to its ability to treat all blood disorders, it is the main ingredient of the well-known patent medicine Yunnan Baiyao, which was first marketed in 1902 and remains a favorite emergency remedy for acute bleeding disorders [8]. Increasing experimental and clinical research is being conducted on the medicinal effects of Sanqi in recent years, confirming the wide variety of actions ascribed to the plant in traditional herb primers [9]. The antimicrobial ability based on the Standard Plate Count (SPC) shown that that alginate demonstrated excellent antimicrobial ability and Sanqi had the best antimicrobial ability among all herbs tested. Alginate was able to release Sanqi sustainably which was proved by Colorimetry.
In this report, we hypothesize that Sanqi could promote diabetic wound healing efficiency. Using animal models treated with (a) alginate dressing, and (b) Sanqi alginate dressing, the rate of wound healing was investigated. Using HPLC, the majority active components present in Sanqi was revealed. Our results demonstrated that Sanqi contribute in promoting wound healing efficiency in both diabetic and non-diabetic subjects.
MATERIALS AND METHODOLOGY
Antimicrobial ability assay
The alginate dressing was prepared by mixing 1g Sodium Alginate powder in 20mL of distilled water. Then 0.5g of herb was mixed in. By Anti-drop method, Calcium Chloride solution was added into Sodium Alginate solution [10]. Petri dishes were filled half full with the sodium alginate & herb mixture. Calcium chloride solution was added onto the Petri dish until the gel completely formed. Milk was dropped on the Petri dish and spreaded. All sampled Petri dishes were covered and kept in room temperature allowing microbial to grow. After 12 days, inspection was performed. To quantify the percentage of visible infected area of each sample dish, a piece of infected area measurement instrument (small square: 50mmx50mm) was used to count the infected area. For each Petri dish, the total of small square was 256, making the total surface area of 640,000 mm2 (=256x50x50). For accuracy, microscope was used to confirm the existence of bacteria in the visible infected area % of Visible Infected Area = No. of small square of infected area x 100/256.
Alginate dressing production
Calcium Chloride solution was prepared by adding Calcium Chloride powder into deionized water until it is saturated; Sodium Alginate solution was prepared by adding 0.5g Sodium Alginate powder in a beaker then combined with 10mL of deionized water (ratio of 1g: 20 ml). Control Alginate dressing was formed by combining Calcium Chloride solution and Sodium Alginate solution in 3:1 ratio. For the Sanqi alginate dressing, 11g of Sanqi was combined with 1.68g CaCl2, 1g Sodium Alginate, and 20mLof distilled water.
Animals keeping
SD rats (200+/- 50g) were obtained from the Chinese University of Hong Kong. The handling of animal and all procedures were in accordance with National Institutes of Health guide for the care and use of Laboratory animals and Animals (Control of Experiments) Ordinance, Hong Kong, China. The approval of using animals was obtained by the Hong Kong Department of Health, and the Hong Kong Baptist University committee on the Use of Human and Animal Subjects in Teaching and Research. The animals were divided into each treatment group randomly. All efforts were made to minimize animal number and suffering.
Chemicals
Unless otherwise stated, all chemicals of reagent-grade quality were obtained from Sigma (St. Louis, MO, USA). Sanqi origin:YuenNan (GMP no: YN20150054).
Intraperitoneal injection of streptozotocin
To set up type 1 diabetic model, rats were kept in the animal room with a 12h of the light and dark cycle. After arrival, the rats were again kept for 1 week prior to experimentation. Streptozotocin (STZ) (50mg/kg/day) or sham control (0.1M sodium citrate, pH 4.5) was administrated in the rats by intraperitoneal injection for 2 continuous days.
Animal surgical procedures
In the animal model, by excising the dorsal skin portion (1.5cmx1.5cm), two full thickness wounds were created in each rat. In each rat, the wounds were treated with (a) alginate dressing and (b) Sanqi Alginate dressing. Following the treatment, digital images of the wound site were made every two days for 2weeks.
Statistical test
Results were presented as means ± standard deviation (SD). The data were analyzed by Student’s t-test and one-way Analysis Of Variance (ANOVA) followed by Tukey’s range test. P < 0.05 was considered statistically significant (*p<0.05 in comparison to the control. **p<0.01 in comparison to the control).
RESULTS
Sanqi with the least infection area on Alginate after 12 days
Herbal powder was mixed with alginate on petri dish and kept in room temperature for 12 days. The percentage of visible infected area on dish were inspected and quantified with a piece of infected area measurement instrument. Microscopic observation was applied to confirm the existence of bacteria on alginate dish. A few types of herbs, which are traditionally suggested, to apply for enhancing wound healing were analysed in this experiment. However, Sanqi demonstrated the best antimicrobial ability indicating that is suitable for external application.
Delayed healing was found on DM rats comparing with controls
In type 1 diabetic model, SD rats were injected with STZ for 2 continuous days. After 1 week, animals underwent surgical operation and each beared two regular-shape (1.5X1.5cm) wounds on the back. In each rat, the wound was treated with (a) alginate dressing and (b) Sanqi alginate dressing. Digital images of the wound site were made twice a week for 3 weeks. The wounds were found 9% faster in terms of wound area percentage decrease than Alginate dressing.
Non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 245% in terms of wound area change. For Sanqi in Alginate, non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 104% in terms of wound area change (Figure 1).
Non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 245% in terms of wound area change. For Sanqi in Alginate, non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 104% in terms of wound area change (Figure 1).
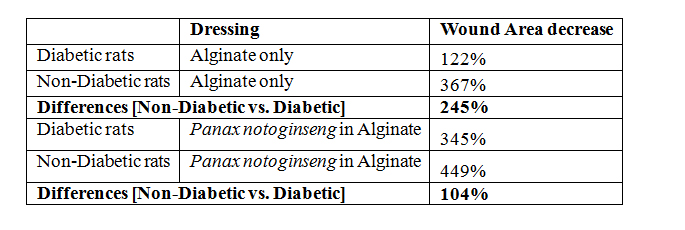 Figure 1: Weeks after injection of STZ, without Panax notoginseng in Alginate, resulted in non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 245% in terms of wound area change. With Panax notoginseng in Alginate, non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 104% in terms of wound area change.
Figure 1: Weeks after injection of STZ, without Panax notoginseng in Alginate, resulted in non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 245% in terms of wound area change. With Panax notoginseng in Alginate, non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 104% in terms of wound area change.Sanqi speeded up wound healing rate on both DM rats and controls
For non-diabetic rats, the presence of Sanqi in alginate dressing heals better by 82% in terms of wound area change and 9% in terms of wound quality assessment. For diabetic rats, the presence of Sanqi in alginate dressing heals better by 223% in terms of wound area change and 7% in terms of wound quality assessment (Figure 2a-c).These results imply that external application of Sanqi on wounds of type 1 diabetes condition in rats could result in increased healing rate.
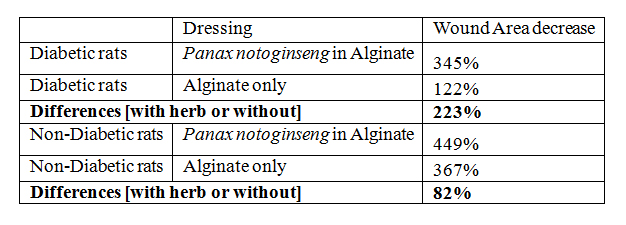 Figure 2a: Weeks after injection of STZ, without Panax notoginseng in Alginate, resulted in non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 245% in terms of wound area change. With Panax notoginseng in Alginate, non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 104% in terms of wound area change.
Figure 2a: Weeks after injection of STZ, without Panax notoginseng in Alginate, resulted in non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 245% in terms of wound area change. With Panax notoginseng in Alginate, non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 104% in terms of wound area change.
 Figure 2a: Weeks after injection of STZ, without Panax notoginseng in Alginate, resulted in non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 245% in terms of wound area change. With Panax notoginseng in Alginate, non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 104% in terms of wound area change.
Figure 2a: Weeks after injection of STZ, without Panax notoginseng in Alginate, resulted in non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 245% in terms of wound area change. With Panax notoginseng in Alginate, non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 104% in terms of wound area change.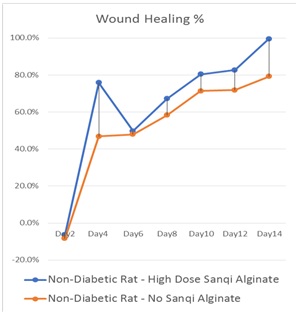 Figure 2b: In non-diabetic rats, with or without Panax notoginseng in Alginate dressing, the graph presents the changes of wound healing areas were measured every two days.
Figure 2b: In non-diabetic rats, with or without Panax notoginseng in Alginate dressing, the graph presents the changes of wound healing areas were measured every two days.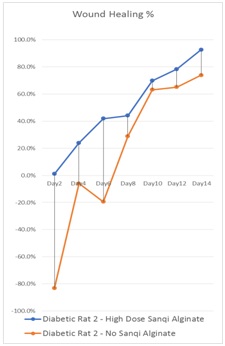
Figure 2c: 2 weeks after injection of STZ, with or without Panax notoginseng in Alginate dressing, the graph presents the changes of wound healing areas in diabetic rats were measured every two days.
With external application of Sanqi, as we can see, the rate of wound area decrease in DM rats (345%) is similar to the rate of wound area decrease in non-DM rat without external application of Sanqi (367%). We suggest that, with external application of Sanqi, the wound-healing rate in DM rats could be redeemed (Figure 2a).
Sanqi promoted higher quality of wound healing on DM rats
Observation of the quality of wound healing promoted by different treatment on both DM rats and controls. Re-epithelialization was observed. Absence of epidermal & dermal organization was found in DM rats with Sanqi external application. Whether there was presence of tissue granulation was also evaluated. Both Inflammatory tissue and granular layer were not found on rats.
Non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 7% in terms of wound quality assessment. For high Sanqi dosage in Alginate, non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 13% in terms of wound quality assessment (Figure 3a-b).
Non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 7% in terms of wound quality assessment. For high Sanqi dosage in Alginate, non-diabetic rats’ wounds recover better than diabetic rats’ wounds by 13% in terms of wound quality assessment (Figure 3a-b).
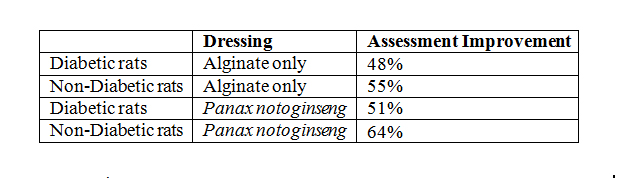
Figure 3a: 2 weeks after injection of STZ, the improvement of wound healing quality was under assessment. Base on the presence of tissue granulation, both inflammatory tissue and granular layer were evaluated.
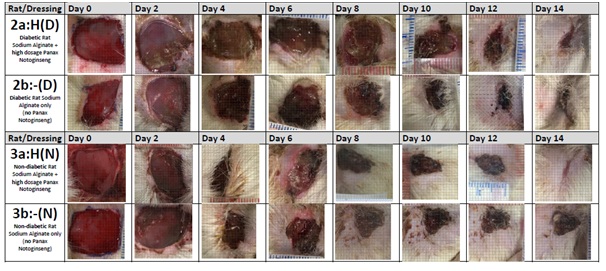 Figure 3b: 2 weeks after injection of STZ, the changes of wound healing areas in both non-diabetic and diabetic rats were measured every two days.
Figure 3b: 2 weeks after injection of STZ, the changes of wound healing areas in both non-diabetic and diabetic rats were measured every two days.These results imply that external application of Sanqi on wounds of type 1 diabetes condition in rats could result in good healing quality (Figure 3). The wound healing quality enhancement induced by external application of Sanqi is more significant in non-DM rats.
DISCUSSION
Foot ulcers are commonly found on DM patients. Diabetes was the 10th cause of death & accounted for 0.9% of all deaths in Hong Kong in 2014 and it was the 7th cause of death and impacted 9.3% of population in US in 2012. By 2030, it is estimated that more than 550 million people around the world will have diabetes. Approximately 25% of these diabetic patients will develop foot ulcers. DM patients with foot ulcers generally suffer from delayed wound healing due to poor blood circulation and infections. However, wound dressings for effective healing were rarely available in market.
There are increasing research reports on traditional Chinese medicines according to their active components and chemical structures. Sanqi is the main ingredient of the well-known patent medicine Yunnan Baiyao, which was first marketed in 1902 and remains a favorite emergency remedy for acute bleeding disorders [6]. Increasing experimental and clinical research is being conducted on the medicinal effects of Sanqi in recent years, confirming the wide variety of actions ascribed to the plant in traditional herb primers [7]. However, past work focusing on the search and separating the active molecules in herbs and the effect in vitro [11]. The effect of Sanqi on wound healing in vivo is still remained unknown [12]. Our current animal study demonstrated that after two weeks of Sanqi external application, higher speed and better quality of wound healing occurred on both DM rats and non-DM rats (Figures 2&3). Wounds of DM rats with Sanqi external application, healed in similar rate of non-DM rats with Alginate (Figure 1). Evidences were provided that Sanqi ability to treat the issue of poor blood circulation.
Besides, suggesting Sanqi for external application, the anti-microbial ability of the herbal dressing is concerned. Since moist and clean environment is essential for wound healing. The antimicrobial ability based on the Standard Plate Count (SPC) shown that that alginate demonstrated excellent antimicrobial ability and Sanqi had high antimicrobial ability among all herbs tested.
In summary, our findings suggested that external application of Sanqi, might enhance the efficiency of wound healing on DM patients and improve the wound healing quality in non-DM patients. These results warrant further investigations on the major active components responsible for the healing effects so as to develop effective therapeutic treatment on wound healing especially in diabetic patients.
There are increasing research reports on traditional Chinese medicines according to their active components and chemical structures. Sanqi is the main ingredient of the well-known patent medicine Yunnan Baiyao, which was first marketed in 1902 and remains a favorite emergency remedy for acute bleeding disorders [6]. Increasing experimental and clinical research is being conducted on the medicinal effects of Sanqi in recent years, confirming the wide variety of actions ascribed to the plant in traditional herb primers [7]. However, past work focusing on the search and separating the active molecules in herbs and the effect in vitro [11]. The effect of Sanqi on wound healing in vivo is still remained unknown [12]. Our current animal study demonstrated that after two weeks of Sanqi external application, higher speed and better quality of wound healing occurred on both DM rats and non-DM rats (Figures 2&3). Wounds of DM rats with Sanqi external application, healed in similar rate of non-DM rats with Alginate (Figure 1). Evidences were provided that Sanqi ability to treat the issue of poor blood circulation.
Besides, suggesting Sanqi for external application, the anti-microbial ability of the herbal dressing is concerned. Since moist and clean environment is essential for wound healing. The antimicrobial ability based on the Standard Plate Count (SPC) shown that that alginate demonstrated excellent antimicrobial ability and Sanqi had high antimicrobial ability among all herbs tested.
In summary, our findings suggested that external application of Sanqi, might enhance the efficiency of wound healing on DM patients and improve the wound healing quality in non-DM patients. These results warrant further investigations on the major active components responsible for the healing effects so as to develop effective therapeutic treatment on wound healing especially in diabetic patients.
ACKNOWLEDGMENT
The authors thank the staff at the Hong Kong Baptist University for helpful technical assistance.
FUNDING
This work was supported by Hong Kong Baptist University. KL and CL are supported by a studentship from the University Grant.
DUALITY OF INTEREST
The authors declare that there is no duality of interest associated with this manuscript.
CONTRIBUTION STATEMENTS
KY, GZ and AL designed the research. KL and CL performed the research, analyzed data and wrote the manuscript. KY is the guarantor of this work and, as such, had full access to all data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
REFERENCES
- Statistics from the Department of Health (2006) Department of Health. Statistics from the Department of Health, Hong Kong.
- World Health Organization (2016) World Health Statistics 2016: Monitoring health for the SDGs. World Health Organization, Geneva, Switzerland.
- National Institute for Health and Care Excellence (2016) Chronic wounds: advanced wound dressings and antimicrobial dressings. National Institute for Health and Care Excellence, London, UK.
- Sood A, Granick MS, Tomaselli NL (2014) Wound Dressings and Comparative Effectiveness Data. Adv Wound Care (New Rochelle) 3: 511-529.
- Advanced Tissue (2016) 6 Key Factors in Treating a Diabetic Wound. Advanced Tissue, Arkansas, USA.
- Dong J (2013) The Relationship between Traditional Chinese Medicine and Modern Medicine. Evid Based Complement Alternat Med 2013: 153148.
- Majewska I, Gendaszewska-Darmach E (2011) Proangiogenic activity of plant extracts in accelerating wound healing - a new face of old phytomedicines. Acta Biochim Pol 58: 449-460.
- Yang B, Xu ZQ, Zhang H, Xu FY, Shi XY, et al. (2014) The efficacy of Yunnan Baiyao on haemostasis and antiulcer: a systematic review and meta-analysis of randomized controlled trials. Int J Clin Exp Med 7: 461-482.
- Zhi-gang Y, A-qin C, Song-dong Y (2005) Research Progress of Pharmacological Actions of Panax notoginseng, Shanghai Journal of Traditional Chinese Medicine 39: 59-62.
- Varaprasad K, Raghavendra GM, Jayaramudu T, Seo J (2016) Nano zinc oxide-sodium alginate antibacterial cellulose fibres. Carbohydr Polym 135: 349-355.
- Prabu D, Majdalawieh AF, Abu-Yousef IA, Inbasekaran K, Balasubramaniam T, et al. (2016) Preparation and characterization of gatifloxacin-loaded sodium alginate hydrogel membranes supplemented with hydroxypropyl methylcellulose and hydroxypropyl cellulose polymers for wound dressing, Int J Pharm Investig 6: 86-95.
- Wang T, Guo R, Zhou G, Zhou X, Kou Z, et al. (2016) Traditional uses, botany, phytochemistry, pharmacology and toxicology of Panax notoginseng (Burk.) F.H. Chen: A review. J Ethnopharmacol 188: 234-258.
Citation: Cho N, Lee CY, Lee KM, Li WY, Yue KKM (2019) Panax notoginseng Enhances Wound Healing Efficiency and Quality on Diabetic Rats. J Altern Complement Integr Med 5: 066.
Copyright: © 2019 Natelie Cho, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
© 2026, Copyrights Herald Scholarly Open Access. All Rights Reserved!

