
Phlegmasia Cerulea Dolens Report of a Case with Unusual Presentation
*Corresponding Author(s):
Álvaro Sánchez GalánAngiology And Vascular Surgery Service Of The University Hospital Of Sanchinarro, HM Hospitals, Calle De Oña 10 C.P 28050 Madrid, Spain
Tel:+34 917567800,
Email:alvarosanchez1306@gmail.com
Abstract
Phlegmasia cerulea dolens is a rare entity secondary to severe Deep Vein Thrombosis (DVT), usually in the lower extremities, and associated with rapidly progressive pain and marked swelling that may compromise the perfusion of the limb. This situation may lead to venous gangrene and the limb’s amputation secondary to a compartment syndrome.
We present the case of a patient with a surgical history of lumbar spine surgery three months before the start of de described symptoms. She refered a clinical description of rapidly progressive edema and the appearance of cerulean colour in her left lower limb.
With diagnostic aids, acute DVT was confirmed caused by extrinsic compression of the left iliofemoral axis secondary to chronic retroperitoneal hematoma.
Keywords
INTRODUCTION
It can occur at any age, although its peak incidence is set between the 5th and 6th decade of life. Its classical clinical presentation has been described as a sudden onset of pain in about 75% of cases, followed by edema and a violaceous skin discoloration. The physical examination shows painful edema of the limb and a bluish colour. In addition, the patient may present some degree of shock, absence of pulse in the lower extremity and coldness of the limb. If the condition is allowed to evolve, bullae, paresthesias, motor paralysis, renal failure, venous gangrene and even death may occur.
This disease has a risk of amputation between 12 and 25% of described cases, and a mortality rate close to 25%, where about 30% is due to a pulmonary thromboembolism. The diagnosis is fundamentally clinical and requires only confirmation with an ultrasound study [3].
PRESENTATION OF THE CASE
Since the patient was not improving with conservative treatment, she underwent surgery, performing a L5-S1 left hemilaminectomy, facetectomy, foraminotomy and discectomy with hard-root decompression. Transpedicular arthrodesis L5-S1 with distraction maneuvers - reduction with titanium system (compatible resonant) Romeo by Spineart and arthrodesis on transverse processes with autologous bone graft and B Gel. The patient recovery is satisfactory after a prophylactic doses treatment with LMWH until full mobility is recovered (three weeks).
During the third postoperative month and while walking, she suddenly notices progressive edema of the entire left lower limb, initially painlessly, but rapidly progressive. Given these symptoms, she decides to turn to the emergency room at the "Gómez Ulla" Military Hospital in Madrid, Spain. She had a marked swelling of the lower limb which obliged the medical personnel to remove her clothes with scissors before attending her. During the physical examination, the patient is found with stable vital signs, without cardiac arrhythmia, no dyspnea nor chest pain. Arterial pulses were present and symmetric in both lower extremities, there was lower limb edema with an important difference in diameter compared to the contralateral limb and a cerulean discoloration of the entire limb (Figure 1). With a diagnosis of severe Deep Vein Thrombosis (DVT) associated to phlegmasia, anticoagulation with LMWH and complete rest in the Trendelenburg position were indicated.
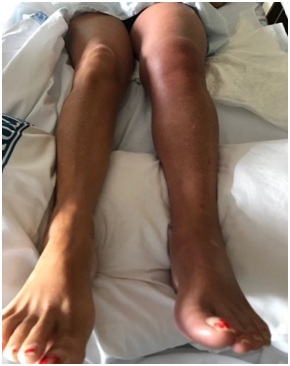
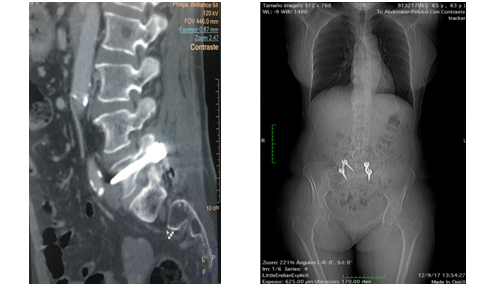 Figure 2: Angio-CT. Notice the presence of the tip of the osteosynthesis screw protruding into the retroperitoneal space.
Figure 2: Angio-CT. Notice the presence of the tip of the osteosynthesis screw protruding into the retroperitoneal space.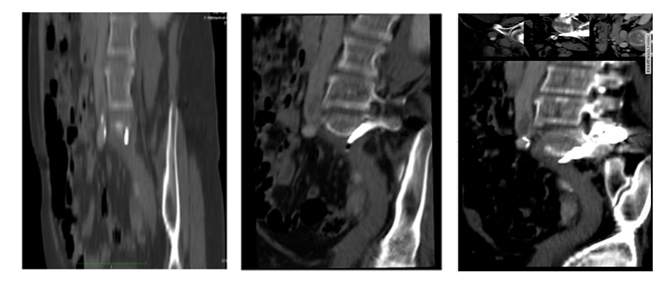 Figure 3: Reconstruction of the Angio-CT. Notice the presence of compressive hematoma on the left iliac venous axis and associated venous thrombosis.
Figure 3: Reconstruction of the Angio-CT. Notice the presence of compressive hematoma on the left iliac venous axis and associated venous thrombosis.After three months of anticoagulation, a vascular venous echodoppler was performed, finding repermeabilization of the left iliac venous axis and minimal post-thrombotic changes (thickening of the wall and discrete reduction of its caliber when compared to the right iliac venous axis). The total anticoagulation time was six months.
DISCUSSION
The case presented was medically managed with good results, but we are aware that a kind of severity score should be established, because undoubtedly, in cases of greater complexity and aggressiveness than we have described, more daring actions such as mechanical thromboaspiration will be required. , with or without the implantation of a cava tempor filter, the use of fasciotomies, venous stenting, etc.
CONFLICT OF INTERESTS
REFERENCES
- Trousseau A (1865) Phlegmasia alba dolens. Clinique Médicale de l’Hôtel-Dieu de Paris 654-712.
- Perkins JM, Magee TR, Galland RB (1996) Phlegmasia caerulea dolens and venous gangrene. Br J Surg 83: 19-23.
- Falcón FB, Pereda RML, Maripangui DM, Campos AG, Sarmiento CM (2010) Flegmasía cerulea dolens. Rev Hosp Clín Univ Chile 21: 124-127.
- Sharafuddin MJ, Sun S, Hoballah JJ, Youness FM, Sharp WJ, et al. (2003) Endovascular Management of venous thrombotic and occlusive diseases of the lower extremities. J Vasc Interv Radiol 14: 405-423.
- Izquierdo-Lamoca LM (2014) Tratamiento recanalizador de las trombosis venosas del sector iliofemoral. Angiología 66: 326-330.
- Goldenberg NA, Branchford B, Wang M, Ray C Jr, Durham JD, et al. (2011) Percutaneous mechanical and pharmacomechanical thrombolysis for occlusive deep vein thrombosis of the proximal limb in adolescent subjects: findings from an institution-based prospective inception cohort study of pediatric venous thromboembolism. J Vasc Interv Radiol 22: 121-132.
- Lessne ML, Bajwa J, Hong K (2012) Fatal reperfusion injury after thrombolysis for phlegmasia cerulea dolens. J Vasc Interv Radiol 23: 681-686.
- Patel KR, Paidas CN (1993) Phlegmasia cerulea dolens: the role of non-operative therapy. Cardiovasc Surg 1: 518-523.
- Eklof B, Arfvidsson B, Kistner R, Masuda EM (2000) Indications for surgical treatment of iliofemoral vein thrombosis. Hematol Oncol Clin North Am 14: 471-482.
Citation: González FS, Galán AS, Guerrero AS, Dominguez MF, Izquierdo AM, et al. (2019) Phlegmasia Cerulea Dolens Report of a Case with Unusual Presentation. J Angiol Vasc Surg 4: 019.
Copyright: © 2019 Felipe Sainz González, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

