
Prevalence of Dermatoses on the Feet in Benghazi
*Corresponding Author(s):
Salwa A El-DibanyDermatology Department, Faculty Of Medicine, Omer Elmuktar University, Al Bayda, Libyan Arab Jamahiriya
Tel:+218 91379934,
Email:salwaeldibani@yahoo.com
Abstract
Introduction
Feet are organs carrying the weight of the body and are subject to various environmental factors. Almost 70% of adults have various foot problems.
Objective
To determine the skin disease seen on feet of patients attending dermatology clinic in Benghazi.
Methodology
Cross- sectional study, all patients attending dermatology clinic during 2 years period from 1st of January 2008 to 31st of December 2009, were included in the study.
Results
There were 1781 patients attending dermatology clinic during the study period, (8.7%) 155 of them had foot skin problems. Mean age was 30.5±16. 2 years, minimum age was 2 years and maximum age was 70 years, 26.5% was in age group 21-30 years. Male to female ratio was 1:1.6, were the female constitute to 61.3%. Majority from urban area 98.1%. Closed shoes used by 71.6% of the patients, 27% had aggravating factors as walking and contact to leather, 16% had positive family history of same disease. The most common foot disease were, foot callosities (14.8%), foot eczema (12.3%), common wart (11.6%) and tinea pedis (11.6%).
Conclusions
Female more affected than male, affecting all ages, majority using closed shoes.
Recommendation
Large-scale survey (community based) is suggested to know the prevalence of foot skin disease in Benghazi.
Keywords
INTRODUCTION
Foot diseases have been found to be common Worldwide despite their morbidity and the availability of more effective treatments However, foot health is affected by factors such as mechanical effects originating from the shoes, personal hygiene, seasonal, characteristics education, economics status as well as trauma [1-3]. Skin diseases seen on the feet are found, according to the order of their frequency, to be due to fungal infections, toe-nail pathology, bacterial infections, hyperkeratinization, and eczematous reactions [3,4]. Large epidemiological studies on foot diseases were conducted in Europe, East Asia and Hong Kong, to allow more accurate information on the scope of foot problems, fungal and non-fungal diseases [4-6]. The results of these studies revealed that skin diseases seen on the feet are found, according to the order of their frequency, to be due to fungal infections, toe-nail pathology, bacterial infections, hyperkeratinization, and eczematous reactions [3,4].
The aim of the present work was to evaluate the skin diseases that may affect the feet in patients attending outpatient dermatology.
CLINIC MATERIALS AND METHODS
This was a prospective study, in which consecutive patients who presented with any skin disease (not just foot disorder) were recruited from dermatology outpatient at Elkeesh clinic during a 2-year period from 1st of Jan. 2008 to 31st of Dec. 2009. A detailed medical history was obtained and thorough skin, nail, toea-webb examination was performed in all patients. KOH examinations for fungus and skin biopsies were done whenever needed. The type of used shows was reported.
RESULTS
One thousand eighty one consecutive patients were examined for foot skin diseases at the dermatology outpatient clinic one day per week over a period of 2 years. One hundred fifty five (14.3%) of the patients were found to have foot skin problems Mean age ± Standard Deviation was 30.5±16.2years, with minimum age was 2 years and maximum age was 70 years , and 26.5% of the patients were in the age group 21-30 years table 1. Females constituted 61.3% of the patients, with a female to male ratio of 1.6:1. The majority of patients (98.1%) were found to be from urban areas. Closed shoes were used by 71.6% of the patients. More than one third (34. 2%) of the patients were students and employee.
|
Age Group |
Gender Types |
||||
|
Age |
Males |
Females |
|||
|
<10 |
12.3% |
8 |
13.3% |
11 |
11.5% |
|
1-112 |
16% |
21 |
35% |
4 |
4.2% |
|
21-30 |
26.5% |
11 |
18.3% |
30 |
31.5% |
|
31-40 |
17.4 |
7 |
11.6% |
20 |
21% |
|
41-50 |
15.5 |
8 |
13.3% |
16 |
16.8% |
|
51-60 |
9.7 |
4 |
6.6% |
11 |
11.5% |
|
61-70 |
2.3 |
1 |
1.6% |
3 |
3.1% |
|
|
60 |
38.7% |
95 |
61.3% |
|
Table 1: Distribution of patients according to age & sex.
Females constituted 61.3% of the patients, with a female to male ratio of 1.6:1 table 1. The majority of patients (98.1%) were found to be from urban areas figure 1. Closed shoes were used by 71.6% of the patient’s. More than one third (34. 2%) of the patients were students and employee.
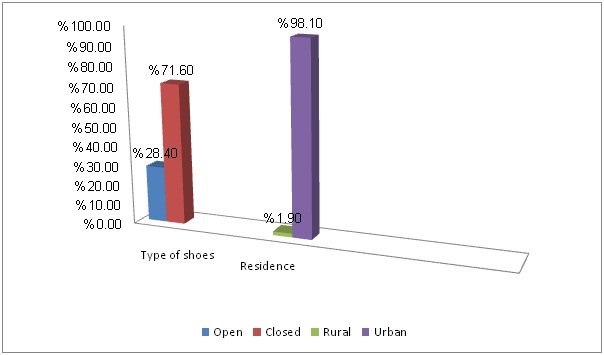
Figure 1: Distribution of patients according to residence & type of shoes.
Seventy three percent of the patients were aggravated by walking and 16% had positive family history of same diseases figure 2.
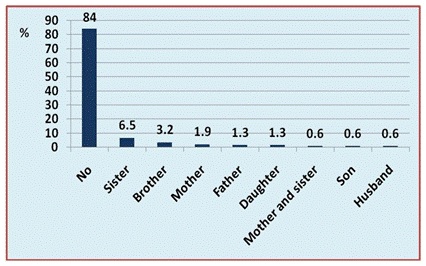 Figure 2: Distribution of patients according to family history of same disease.
Figure 2: Distribution of patients according to family history of same disease.
Table 2 the most common foot diseases were foot eczema (31.6%), foot callosities (14.8%), common warts (11.6%) tinea pedis (11.6%), and plantar warts (9.0%).
|
Type of Foot Skin Disease |
No. |
% |
|
Palmo planter-desquamation |
3 |
1.9 |
|
Juvenile planter dermatitis |
8 |
5.2 |
|
Foot-eczema |
19 |
12.3 |
|
Planter wart |
14 |
9 |
|
Friction dermatitis |
6 |
3.9 |
|
Insect bite |
4 |
2.6 |
|
Chill blain |
2 |
1.3 |
|
Planter psoriasis |
4 |
2.6 |
|
Vitiligo |
1 |
0.6 |
|
Callosities |
23 |
14.8 |
|
Tinea pedis |
18 |
11,6 |
|
Myxoid cyst |
1 |
o.6 |
|
Hand –foot eczema |
3 |
1.9 |
|
In growing nail toe |
1 |
0.6 |
|
Common wart |
18 |
11.6 |
|
Neurodermatitis |
2 |
1.3 |
|
Hyperhydrosis |
2 |
1.3 |
|
Hyperkeratosis &fissure heel |
4 |
2.6 |
|
Trauma |
1 |
0.6 |
|
Tinea corporis |
1 |
0.6 |
|
Dyshydrotic eczema |
1 |
0.6 |
|
Rhenyoid phenomena |
1 |
0.6 |
|
Contact eczema |
5 |
3.2 |
|
Planter hyperkeratosis |
1 |
1.9 |
|
Pyoderderma |
1 |
0.6 |
|
Planter dermatitis |
2 |
1.3 |
|
Scabies |
1 |
0.6 |
|
Foot dermatitis |
1 |
0.6 |
|
Palmo-planter keratoderma |
2 |
1.3 |
|
Planter eczema |
2 |
1.3 |
|
Diabetic ulcer |
1 |
0.6 |
|
Total |
155 |
100 |
Table 2: Distribution of patients according to type of foot skin disease (total no.= 155).
DISCUSSION
The occurrence of foot diseases in our patients visiting the dermatology outpatient clinic was less than what was reported in the earlier studies from Saudi Arabia, Europe and Hong Kong [5-7], in which males were more affected than females too. In the present study, 26.5% of our patients were in the age group 21-30 years, which is a finding similar to what was reported by Zimmo in Saudi Arabia [3]. Foot eczema, and students and employee were more commonly affected with foot diseases. The percentage of used closed shoes was more than that of open shoes, and this leads to an increased local temperature because of occlusion, and humidity because of perspiration, and hence, increased friction and enhancement of fungal growth. However, fungal infections were the most common clinically diagnosed foot diseases in Europe, Hong Kong and Saudi Arabia (2,4,8 ). The difference between studies may reflect the difference in patient’s habits, social behavior, environmental factors, occupational activities, health attitude, and footwear. The relationship between these factors and foot problems is a complex one that deserves considerably more research.
CONCLUSIONS
The feet of both sexes are subjected to several skin diseases such as induced by inflammatory skin diseases (eczema), chronic friction and pressure (callosities), and infections (viral warts and fungal infections). Alarge scale survey.
REFERENCES
- ?nan?r I, ?ahin MT, Gündüz K, Dinç G, Türel A, et al. (2002) Tinea pedis and onychomycosis in primary school children. Mycoses 45: 198-201.
- Zimmo SK (2008) Prevalence of dermatologic foot diseases in Saudi Arabia. 19: 23-26.
- Helfand AE (1998) Podiatric medicine and public health. Concepts and perspectives. Special Commission of the Podiatric Health Section of the American Public Health Association. J Am Podiatr Med Assoc 88: 353-359.
- Fung WK, Lo KK (2000) Prevalence of skin disease among school children and adolescents in a student health service center in Hong Kong. Pediatr Dermatol 17: 440-446.
- Roseeuw D (1999) Achilles foot screening project: Preliminary results of patients screened by dermatologists. J Eur Acad Dermatol Venereol 12: 6-9.
- Burzykowski T, Molenberghs G, Abeck D, Haneke E, Hay R, et al. (2003) High prevalence of foot diseases in Europe: results of the Achilles Project. Mycoses 46: 496-505.
- Haneke E, Roseeuw D (1999) The scope of onychomycosis: Epidemiology and clinical features. Int J Dermatol 38: 7-12.
- Cheng S, Chong L (2002) A prospective epidemiological study on Tinea pedis and onychomycosis in Hong Kong. Chin Med J (Engl) 115: 860-865.
Citation: El-Dibany SA, El-Sherif A, El-Sherif NA (2019) Prevalence of Dermatoses on the Feet in Benghazi. J Clin Dermatol Ther 5: 030.
Copyright: © 2019 Salwa A El-Dibany, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

