
Primary Squamous Cell Carcinoma of the Endometrium in a Postmenopausal Woman: Case Report
*Corresponding Author(s):
Kumkum VadehraDepartment Of Pathology And Laboratory Medicine, Harbor-University Of California At Los Angeles Medical Center, Torrance, California, United States
Tel:+1 424306646,
Email:kumkum125@yahoo.com
Abstract
Primary squamous cell carcinoma of the endometrium is an extremely rare tumor with poorly understood pathogenesis. The first case of Primary Endometrial Squamous Cell Carcinoma (PSCCE) was reported in 1892. Since then only sporadic cases have been reported in the literature. There is limited data available about epidemiology, clinical progression and different therapeutic options for the disease. This report describes a case of a postmenopausal woman with Primary Squamous Cell Carcinoma of the Endometrium (PSCCE).
Keywords
Endometrium; Human papilloma virus; Postmenopausal bleeding; p16; Squamous cell carcinoma
INTRODUCTION
Primary squamous cell carcinoma of the endometrium is an extremely rare tumor with poorly understood pathogenesis. The first case of primary endometrial squamous cell carcinoma (PSCCE) was reported in 1892.[1] Since then only sporadic cases have been reported in the literature. There is limited data available about epidemiology, clinical progression and different therapeutic options for the disease. This report describes a case of a postmenopausal woman with Primary Squamous Cell Carcinoma of the Endometrium (PSCCE).
CASE PRESENTATION
A 72-year-old Gravida 3 Para3 African-American woman with no significant past medical history presented to gynecology department at Harbor-UCLA Medical Center with postmenopausal vaginal bleeding and pelvic pain for one month. The patient also reported severe constipation necessitating regular laxative use and unintentional weight loss of 35 pounds over last three months. The general appearance was cachectic. Gynecologic examination revealed unremarkable soft cervix and normal size, mobile uterus. There was no abnormal discharge or foul smell. The abdomen was soft without tenderness or masses and no other special positive signs. Pap smear by Thin prep method showed High Grade Squamous Intraepithelial Lesion (HSIL). HPV results for the cervical smear showed HPVmRNA E6/E7 detected. Pelvic ultrasound revealed 8.2 x 6.3 x 5.8 cm heterogeneous uterus. A 2.6 x 3 x 2.4 cm sub mucosal anterior body fibroid was seen. The endometrial echo complex measured 5mm. Subsequently, endometrial biopsy was performed. Histopathological examination with Hematoxylin and Eosin (H&E) staining showed neoplastic squamous cells, occasionally found singly and arranged in variably sized nests, solid cohesive groups, coalescing trabecular aggregates and ribbons, irregularly infiltrate the desmoplastic, variably acutely and chronically inflamed fibrocollagenous stroma. These cells display moderate to marked nuclear pleomorphism with some bizarre enlarged forms, nuclear hyperchromasia, occasional multinucleation, coarse chromatin clumping, some nucleolar prominence, recognizable intercellular bridges, increased and abnormal mitoses, focal spindled configuration, rare individual cell keratinization and confluent tumoral necrosis. Benign endometrial tissue or glandular formation is not seen. The tumor cells show positive IHC staining for p40, CK20, ER and negative for CK7, HPV, p16. The proliferation index with Ki67 is high (70%). The histological pattern and immunophenotype shows “invasive moderately differentiated squamous cell carcinoma consistent with endometrial primary (Figures 1-8).
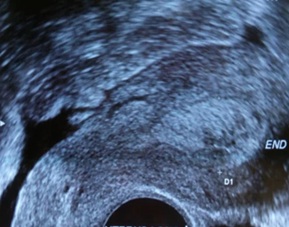 Figure 1: Transvaginal ultrasound showing longitudinal section of the uterus showing 2.6 cm anterior fundal heterogeneous mass
Figure 1: Transvaginal ultrasound showing longitudinal section of the uterus showing 2.6 cm anterior fundal heterogeneous mass
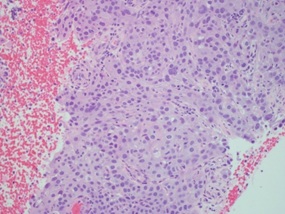 Figure 2: Medium power view of endometrial biopsy showing moderately differentiated squamous cell carcinoma cells and absence of endometrial glands (H&E ×100).
Figure 2: Medium power view of endometrial biopsy showing moderately differentiated squamous cell carcinoma cells and absence of endometrial glands (H&E ×100).
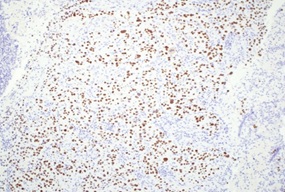 Figure 3: Endometrial biopsy showing diffuse positivity for p40 in the tumor cells as seen by immunohistochemistry (magnification ×100).
Figure 3: Endometrial biopsy showing diffuse positivity for p40 in the tumor cells as seen by immunohistochemistry (magnification ×100).
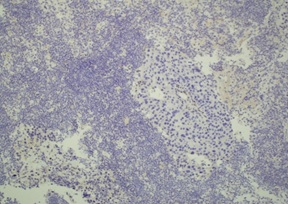 Figure 4: Endometrial biopsy showing patchy positivity for ER in the tumor cells as seen by immunohistochemistry (magnification ×100).
Figure 4: Endometrial biopsy showing patchy positivity for ER in the tumor cells as seen by immunohistochemistry (magnification ×100).
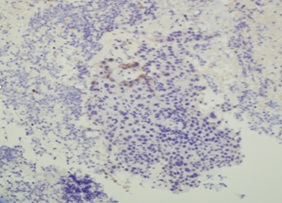 Figure 5: Endometrial biopsy showing patchy positivity for CK20 in the tumor cells as seen by immunohistochemistry (magnification ×100).
Figure 5: Endometrial biopsy showing patchy positivity for CK20 in the tumor cells as seen by immunohistochemistry (magnification ×100).
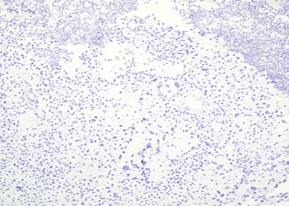 Figure 6: Absence of immunohistochemical staining for CK7 in the tumor.
Figure 6: Absence of immunohistochemical staining for CK7 in the tumor.
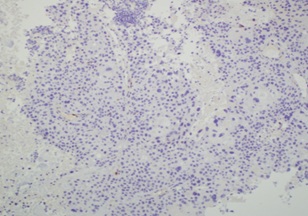 Figure 7: Absence of immunohistochemical staining for p16 in the tumor.
Figure 7: Absence of immunohistochemical staining for p16 in the tumor.
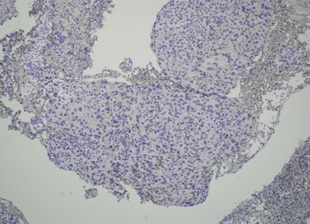 Figure 8: Absence of immunohistochemical staining for HPV in the tumor.
Figure 8: Absence of immunohistochemical staining for HPV in the tumor.
The prognostic grade was classified as FIGO (International Federation of Gynecology and Obstetrics) stage IIa. The patient was planned for concurrent weekly cisplatin (40 mg/m2) and radiotherapy. However, within two months of diagnosis and having received two cycles of chemotherapy and one external beam radiation she developed bilateral severe hydronephrosis requiring percutaneous nephrostomy tube placement. Based on new MRI findings of hydronephrosis and as cities, the cancer was restaged and upgraded to IIIa. Furthermore, the clinical course was complicated by acute renal failure, hypokalemic metabolic disturbance, anemia, ascites, cachexia of malignancy. After five months of initial diagnosis, the patient succumbed to the co-morbid medical complications.
DISCUSSION
The first case of primary endometrial squamous cell carcinoma (PSCCE) was reported in 1892. Early in 1928, Fluhmann established the strict pathologic and clinical criteria for PSCCE: exclusion of endometrioid adenocarcinoma component (coexistence with endometrial adenocarcinoma) [1,2]; absence of connection between the endometrial tumor and cervical squamous epithelium; and absence of primary invasive squamous cell carcinoma from other sites (e.g., cervical and colorectal lesions).Histologically almost all types of endometrial cancer are adenocarcinoma [3]. On the other hand, most of the endometrial squamous carcinomas originate from the squamous cell carcinoma of the cervix that extend into the endometrial cavity or from the endometrial pleuripotent stem cell [4], and squamous metaplasia of the normal endometrium [5]. Primary endometrial SCC is a rare entity. However, this type of endometrial cancer has a high degree of malignancy and poor prognosis, and the 5-year survival rate was very low except for individual cases [6,7]. The common treatment methods include combined surgical approach (radicle hysterectomy with adnexa removal)and radiotherapy [8]. According to Goodrich et al. report, after the radical surgery their two patients received external beam radiation with cisplatin chemo-sensitization [9], followed by vaginal brachytherapy and have obtained good clinical result. Since our case was not a surgical candidate, cisplatin-based chemo-sensitization with external beam radiotherapy was attempted. The efficacy of treatment further could not be determined due to mortality associated with rapid evolution of advanced stage disease.
The pathogenesis and etiology of PSCCE are poorly investigated and incompletely understood. Various scholars have speculated that the etiology could be related to bi-directional differentiation of pluripotent endometrial precursor cells [10], heterotopic cervical tissue [11], chronic pelvic inflammatory, radiation therapy [12], or HPV infection [13]. Generally high-risk HPV subtypes are the major cause of cervical SCC [14]. Some scholars have tried to explain the relationship between HPV infection and PSCCE, but it still remains controversial. A study conducted by Bures, et al. suggested that the pathogenesis of PSCCE involves overexpression of p19 .[15], pRb, CDK6, and Cyclin D1, but no expression of p16, p18, CDK4, and HPV E7, thereby excluding the association of HPV and PSCCE. Similar result has been demonstrated in the present case where the squamous cancerous cells in the endometrium showed negative staining with p16 and HPV, thereby failing to establish the role of HPV in pathogenesis of PSCCE in contrast to the high grade squamous intraepithelial lesion of the cervix in which HPV mRNA E6/E7 was detected.
CONCLUSION
Primary squamous cell carcinoma of the endometrium is rare and aggressive cancer, characteristic of elderly patients. In conclusion, we believe that our case fulfils the strict criteria for the diagnosis of PSCCE as defined by Fluhmann, et al. which is further confirmed by immunohistochemical stains for an endometrium primary [2]. The presence of atypical squamous cells without endometrial glands in an endometrial biopsy should alert the clinician to investigate the source of the lesion. Early diagnosis followed by prompt surgical operation remains the best treatment for patients with PSSCE at present. Currently there is no consensus for a universally accepted optimal treatment method among various modalities that would improve the prognosis. Hence such case reports of disseminated cancer and death attributed to PSCCE emphasize the importance of timely diagnosis and adequate treatment of this aggressive cancer.
ACKNOWLEDGEMENT
Thank you to the Obstetrics- Gynecology Team at Harbor-UCLA Medical Center, Torrance CA for the case specimen and the Histology Lab at Harbor-UCLA Medical Center, Torrance CA for preparing the slides and perform immunohistochemical studies for this case.
REFERENCES
- Gebhard C (1982) About the carcinoma forms of the uterine body emanating from the surface epithelium and about horn cancer of the cavum uteri. Z Geburtshilfe Gynakol 24: 1-21.
- Fluhmann CF (1928) Squamous epithelium in the endometrium in benign and malignant conditions. Surg Gynecol Obstet 46: 309-316.
- Houissa-Vuong S, Catanzano-Laroudie M, Baviera E, A Balaton, B Galet, et al.(2002) Primary squamous cell carcinoma of the endometrium: case history, pathologic findings, and discussion. Diagn Cytopathol 27: 291-293.
- Thomakos N, Galaal K, Godfrey KA, et al. (2008) Primary endometrial squamous cell carcinoma. Arch GynecolObstet 278: 177-180.
- Lee SJ, Choi HJ (2012) Primary endometrial squamous cell carcinoma: a case report and review of relevant literature on Korean women. Korean J Pathol 46: 395-398.
- Simon A, Kopolovic J, Beyth Y (1988) Primary squamous cell carcinoma of the endometrium. Gynecol Oncol 31: 454-461.
- Terada T, Tateoka K (2013) Primary pure squamous cell carcinoma of the endometrium: A case report. Int J Clin Exp Pathol 6: 990-993.
- Bagga PK, Jaswal TS, Datta U, Mahajan NC (2008) Primary endometrial squamous cell carcinoma with extensive squamous metaplasia and dysplasia. Indian J Pathol Microbiol 51: 267-268.
- Goodrich S, Kebria-Moslemi M, Broshears J, Sutton GP, Rose P (2013) Primary squamous cell carcinoma of the endometrium: two cases and a review of the literature. Diagn Cytopathol 41: 817-820.
- Horn LC, Bilek K (1993) Primary squamous cell carcinoma of the endometrium. Clinicopathologic data and histogenetic classification. Zentralbl Pathol 139: 355-360.
- Yamamoto Y, Izumi K, Otsuka H, Kishi Y, Mimura T, et al. (1995) Primary squamous cell carcinoma of the endometrium: A case report and a suggestion of new histogenesis. Int J Gynecol Pathol 14: 75-80.
- Goodman A, Zukerberg LR, Rice LW, Fuller AF, Young RH, et al. (1996) Squamous cell carcinoma of the endometrium: a report of eight cases and a review of the literature. Gynecol Oncol 61: 54-60.
- Im DD, Shah KV, Rosenshein NB (1995) Report of three new cases of squamous carcinoma of the endometrium with emphasis in the HPV status. Gynecol Oncol 56:464-469.
- Schiffmann Castle PE, Jeronimo J, Rodriguez AC, et al. ( 2007) Human papillomavirus and cervical cancer. Lancet 370: 890-907.
- Bures N, Nelson G, Duan Q, Magliocco A, Demetrick D, et al. (2013) Primary squamous cell carcinoma of the endometrium: clinicopathologic and molecular characteristics. Int J Gynecol Pathol 32:566-575.
Citation: Vadehra K, Bhuyan RR, McPhaul L (2020) Primary Squamous Cell Carcinoma of the Endometrium in a Postmenopausal Woman: Case Report. J Clin Stud Med Case Rep 7: 094.
Copyright: © 2020 Kumkum Vadehra, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

