
Propeller Flap: Surgical Option after Resection of Lower Limb Melanoma
*Corresponding Author(s):
Roney Gonçalves Fechine FeitosaDivision Of Plastic Surgery, Department Of Surgery, Escola Paulista De Medicina, Universidade Federal De São Paulo, São Paulo, Brazil
Tel:+55 1155764848,
Email:dr.an@bol.com.br
Abstract
Objective: To describe a series of cases of lower limb reconstruction using an axial reverse flow flap (propeller flap) after melanoma excision.
Patients and methods: From August 2014 to December 2016, at the Plastic Surgery Service at UNIFESP, five patients with defects in the lower limbs after melanoma resection were reconstructed using propeller flap. In all cases, the perforating vessels were previously mapped using Doppler ultrasound.
Results: The size of the defect ranged from 4 cm × 3 cm to 8 cm × 4.5 cm. One case had a 180º rotation. In all the others, a 90° rotation was sufficient. All patients had good aesthetic results.
Conclusion: The propeller flap is a simple and low cost technique. It is indicated for reconstruction of the distal third of small and/or medium-sized lower limb. The aesthetic result is satisfactory with the thickness and color of the flap very similar to the excised area.
Keywords
Lower limbs; Melanoma; Perforator flap
Introduction
Restoration of skin coverage is an indispensable step in the treatment of tumors, carcinomas or melanomas, that evolve with a solution of continuity of the integument. Limited mobility and lack of skin make reconstruction of the lower limb a challenge. Random flaps (such as the keystone area flap) have reduced mobility and poor vascularization. Muscle flaps are used today with great discretion, given the enormous morbidity in the donor area. Axial fasciocutaneous flaps are very versatile, but usually require treatment of the donor area. Microsurgical flaps are time and support structure demanding, and are reserved for large defects.
The propeller flap is a type of local flap based on perforating vessels, defined by the Tokyo Consensus (2011) as “a perforating flap with a skin island composed of two parts, one larger and one smaller, separated by a nutrient perforating vessel that corresponds to its axis of rotation” [1].
It was first described in 1991 by Hyakusoku, et al. who used an island flap, vascularized by perforating vessels, with an axis of rotation in the pedicle, for the treatment of burn sequelae [2].
This was only possible due to a better knowledge of the anatomy and importance of the myocutaneous or septocutaneous perforators. Authors such as Donski and Fogdestam described that fasciocutaneous flaps that maintained vascularization through perforators could be larger than the local flaps previously used [3]. Over time, flaps began to be made with increasingly smaller skin bridges (also known as keystone flaps), until some surgeons chose to perform island flaps, without the skin pedicle, and with increasingly larger rotation arcs [4].
Since then, propeller flaps have become increasingly popular, as they have several advantages. They reconstruct with tissues similar to the original, because they use tissues neighboring the defect. In general, they present less donor area morbidity, often allowing primary closure of the donor area. They also allow a great rotation arc (up to 180º) [5,6]. Another advantage is that, especially in the reconstruction of defects in the distal third of the leg, they can be alternatives to microsurgical flaps, with lower cost, shorter surgical time, and no need for vascular anastomosis [7]. Despite these advantages, there are still no large clinical trials comparing the two techniques.
Propeller flaps are also subject to complications, the most worrisome of which is partial or total necrosis of the flap. Other complications described are epidermolysis, transient venous congestion, infection, hematoma, and dehiscence. Risk factors for complications are not yet fully defined [5,6,8].
Objective
To describe five clinical cases in which the helix flap was used for treatment of lower limb reconstruction after melanoma resection.
Methodology
This is a retrospective and descriptive study of five patients submitted to the propeller flap - consisting of two “blades” of a propeller, with the perforating vessels located in the center, so that the larger “blade” is rotated in order to close the defect - in the distal third of the lower limbs after resection of primary or metastatic melanoma. Preoperative Doppler ultrasound was used to map the perforating vessels. The procedures were performed between November 2012 and January 2014 at Hospital São Paulo, and were subsequently followed up by the Plastic Surgery Discipline of Escola Paulista de Medicina. Approval was issued by the Research Ethics Committee of the Universidade Federal de São Paulo under number 0675/2019 and written consent was obtained from all patients.
Results
The defect size ranged from 4 × 3 cm to 8 × 4.5 cm, and the flap size ranged from 7 × 3 cm to 12 × 5 cm. One case had a 180° rotation. In all the others, a 90-degree rotation was sufficient. One patient had partial wound dehiscence. All patients had good esthetic results and the donor area closed primarily (Table 1).
|
Gender/age |
Locationleg |
Sizedefect |
Size flap |
Rotation |
Complication |
|
M / 54 yrsold |
Rightlower 1/3 thigh |
8x3 cm |
9x3,5 cm |
90° |
- |
|
W / 58 yrsold |
Leftmiddle 1/3 leg L |
4x3 cm |
9x3,5 cm |
90° |
- |
|
M /59 yrsold |
Right1/3 lowerleg |
5x4,5 cm |
12x5 cm |
180° |
- |
|
M / 60 yrsold |
Leftmiddle 1/3 leg |
7x3,5 cm |
9x4,5 cm |
180° |
Partialepidermolysis flap |
|
W / 62 yrsold |
Rightlower 1/3 thigh |
8x4,5 cm |
11 x 5cm |
60° |
Seroma in the donor area |
Table 1: Data, dimensions, and specificities about the five patients and the procedures they underwent.
Helix flaps are a good option for covering defects after resection of lower limb melanoma. In the cases described here, all presented good postoperative results, without serious complications (Figure 1-3).
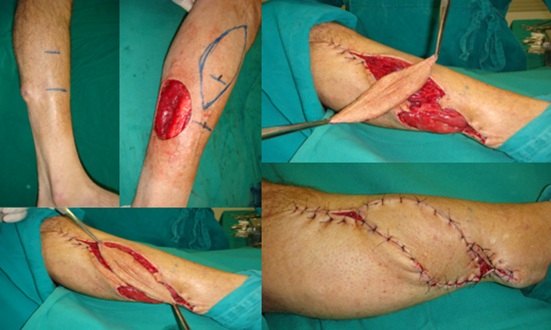 Figure 1: 59-year-old male with 1.5x.1.2cm ameloblastic melanoma, performed resection of lesion with margins resulting in a 5x4.5cm defect. Scheduled helix flap with 12x5cm dimension, 180 degree rotation based on anterior tibial vessel perforator.
Figure 1: 59-year-old male with 1.5x.1.2cm ameloblastic melanoma, performed resection of lesion with margins resulting in a 5x4.5cm defect. Scheduled helix flap with 12x5cm dimension, 180 degree rotation based on anterior tibial vessel perforator.
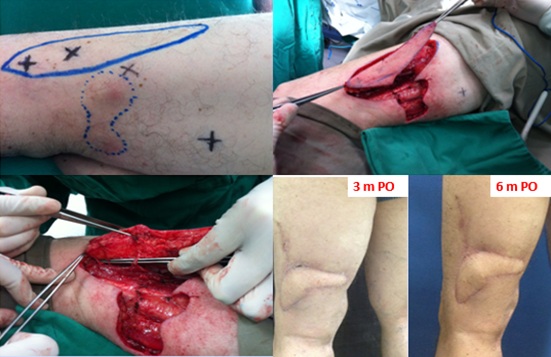 Figure 2: Male, 54 years old, diagnosed with two melanoma in situ lesions on the left thigh, resulting in a 6x2cm defect. Programmed 9x3cm helix flap and 90-degree rotation for synthesis of the defect.
Figure 2: Male, 54 years old, diagnosed with two melanoma in situ lesions on the left thigh, resulting in a 6x2cm defect. Programmed 9x3cm helix flap and 90-degree rotation for synthesis of the defect.
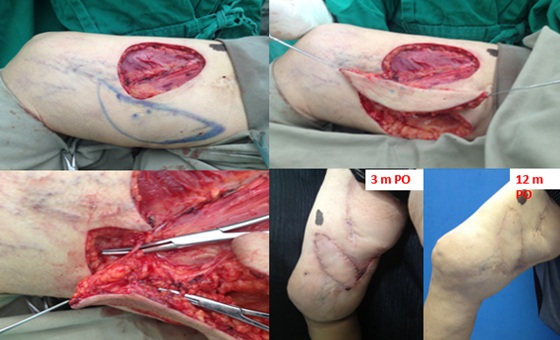 Figure 3: 62-year-old woman with 2mm breslow melanoma, disease-free sentinel lymph node, resulting in a defect of 8x4.5cm, decided to perform a helix flap of 11x5cm and rotation of 60 degrees. Evolving with seroma in the donor area, treated with puncture in the postoperative period and with good evolution in the late postoperative period.
Figure 3: 62-year-old woman with 2mm breslow melanoma, disease-free sentinel lymph node, resulting in a defect of 8x4.5cm, decided to perform a helix flap of 11x5cm and rotation of 60 degrees. Evolving with seroma in the donor area, treated with puncture in the postoperative period and with good evolution in the late postoperative period.
Discussion
The middle and proximal thirds of the leg have a good area of skin coverage and muscle mass, which is a valuable donor area for pedicled tissues.
In the distal third of the leg there is no interposition of muscle tissues between the noble structures and the integument, and the integument has limited distensibility and mobility. Such characteristics make the use of skin grafts and random rotation flaps inadequate for injuries that reach the entire skin thickness. Therefore, it is necessary to resort to more complex procedures such as microsurgical flaps or pedicled flaps in reverse flow islands.
Helix flaps are a relatively new and very promising concept, especially in challenging areas such as lower limb reconstruction, as demonstrated in the cases described here. In theory, they are flaps capable of reconstructing defects with similar tissues, with little donor area morbidity, preserving the main vessels of the region, reducing surgical time and hospitalization.
Despite these advantages, they are not free of complications, many of them significant. In a literature review carried out by Gir, et al. the occurrence of partial necrosis was 11% and total necrosis was 1% [5]. Nelson, et al. found 11% of partial necrosis and 5% of total necrosis. In this same study, 82.9% of flaps had no complications [6]. In the recent meta-analysis and systematic review, published in 2016 by Bekara, et al. also arrived at similar results: 10.5% for partial necrosis and 3.5% for total necrosis. Other complications described were epidermolysis (3.5%) and transient venous congestion (3%) [8]. In these cited works the flap rotation arc and the dissection plane (sub or suprafascial) were not associated with the occurrence of complications. In the cases reported here, there was no partial or total necrosis of the flaps, but one of the cases evolved with surgical wound dehiscence. Even though only resuture was needed, it was a complication that delayed the patient's full recovery.
Classically, lower limb defects, especially in the distal third, are indicated for reconstruction with microsurgical flaps. Propeller flaps may be a simpler alternative in these cases, especially in small and moderate defects. There are still no studies directly comparing these two techniques, but some important information is already available. Wu et al reported a 2019 case series on free flaps, with an occurrence of 3.8% of total necrosis and 10% of cases requiring revision procedure or major surgery. These rates are quite similar to those found in the large studies on helix flaps described to date [9].
One of the main pillars of this surgical technique is the fact that a rotation of the pedicle by up to 180 degrees does not compromise its patency. Some experimental studies have been performed to investigate this fact, with contradictory results. Wong and co-workers studied in a virtual model the factors affecting vessel patency [10]. They observed that the angle of rotation should be no more than 180º, the arterial pressure should be kept constant during surgery, the pedicle diameter should be approximately 1mm and its length should be greater than 30mm [10]. Damir, et al. and Izquierdo, et al. also reported that the torsion of up to 180º in the pedicle does not affect its patency [11,12]. On the other hand, Salgarello, et al. in an experimental study demonstrated that rotations of up to 90º may compromise the flow of vessels with microsurgical anastomoses [13].
Another point not yet fully defined is the maximum flap size. Saint-Cyr, et al. described the “perforasome” theory, which suggests that perforator flaps can have their area of vascularization increased by opening communicating vessels with the territories of adjacent ligated perforators [14]. According to this theory, it is difficult to study and define the safe size for a flap in cadaveric studies, because this compensatory mechanism would occur only in vivo [14]. In the meta-analysis and systematic review published by Bekara et al, flap size > 100 cm was not a risk factor for complications. Innocenti, et al analyzed 74 cases and also found no difference in the number of complications between flaps of 5-14cm and 15-25cm [15].
As a diagnostic method, most studies use portable acoustic Doppler to map perforators [8]. This method is successful in identifying vessels in up to 80% of cases [16]. It’s main advantages are its practicality, low cost and the possibility of intraoperative use. Another imaging exam that can be used is the color Doppler ultrasound, which has as its main convenience the ability to obtain information related to the diameter and flow of the vessels. The problem is that it depends on an experienced examiner and is more time consuming than the other alternatives. CT angiography is a method that has advanced greatly in recent years and can identify perforators as small as 0.3 to 0.5mm, and assess their size, location, and three-dimensional path with high sensitivity and specificity. The main disadvantages are the use of contrast, ionizing radiation, and higher cost. Magnetic resonance imaging can also be used, although some studies point to a reduced accuracy in the diagnosis of perforators with diameter smaller than 1 mm [17]. In this study, only portable acoustic Doppler was used, without major difficulties in the identification of perforators.
Besides factors related to technique and surgical planning, clinical factors of the patient can influence the final result. In the study published by Bekara, et al. age over 60 years (RR=1.61; p=0.03), arteriopathy (RR=3.12; p=0.01) and diabetes (RR=2.0; p=0.02) were factors associated with higher risk of adverse events [8]. Smoking was not statistically significant as a risk factor, with a relative risk of 1.96 (0.99 to 3.90 in the 95% confidence interval) and p=0.06 [8]. The patients in this study were not smokers and only one had comorbidities (hypothyroidism).
The distal regions of the lower limb, including the lower third of the leg and the feet, are areas that are very prone to soft tissue loss from trauma and trophic injury. The anterior position of the tibia, with its thin and vulnerable covering, and the large number of tendons that cannot remain exposed, require rapid yet complex skin coverage. The situation regarding the direction of blood flow, the scarcity of muscle bellies for flaps, and inelastic skin for viable randomized flaps complicate this situation. In the past, flaps with intermediate transfer were used, as well as cross leg flaps still are, with important disadvantages: they depend on more than one surgical time, generate a lot of discomfort to the patient, and are not always effective. Microsurgery has become an option that contributes a lot to the coverage of lesions in this aspect, but it depends on a team with training and specialized material. The donor areas are larger, can cause relative functional deficit and use larger vascular trunks.
Conclusion
Reverse flow fasciocutaneous flaps can contribute to the coverage of small and medium lesions in this location, with less functional and aesthetic sequelae, and shorter surgical time. It constitutes an efficient surgical option for its safety, versatility, and lower hospitalization cost.
Financial Disclosure Statement
The authors have nothing to disclose. No funding was received for this article.
Statement of Institutional Review Board Approval
This study was conducted at Plastic Surgery Department at Paulista School of Medicine - Federal University of São Paulo. The research protocol was approved by the institution’s Research Ethics Committee (registration number: 0675/2019), in compliance with the ethical principles of the Declaration of Helsinki and with the requirements of Brazilian National Health Council (Resolutions 466/12 and 510/16).
Conflict of Interest Statement
Conflict of Interest None.
References
- Pignatti M, Ogawa R, Hallock GG, Mateev M, Georgescu AV, et al. (2011) The “Tokyo” consensus on propeller flaps. Plast Reconstr Surg 127: 716-722.
- Hyakusoku H, Yamamoto T, Fumiiri M (1991) The propeller flap method. Br J Plast Surg 44: 53-54.
- Donski PK, Fogdestam I (1983) Distally based fasciocutaneous flap from the sural region. A preliminary report. Scand J PlastReconstr Surg 17: 191-196.
- El-Saadi MM, Khashaba AA (1990) Three anteromedial fasciocutaneous leg island flaps for covering defects of the lower two-thirds of the leg. Br J Plast Surg 43: 536-540.
- Gir P, Cheng A, Oni G, Mojallal A, Saint-Cyr M (2012) Pedicled perforator (propeller) flaps in lower extremity defects: A systematic review. J Reconstr Microsurg 28: 595-601.
- Nelson JA, Fischer JP, Brazio PS, Kovach SJ, Rosson GD, Rad AN (2013) A review of propeller flaps for distal lower extremity soft tissue reconstruction: Is flap loss too high? Microsurgery 33: 578-586.
- Rad AN, Singh NK, Rosson GD (2008) Peroneal artery perforator-based propeller flap reconstruction of the lateral distal lower extremity after tumor extirpation: Case report and literature review. Microsurgery 28: 663-670.
- Bekara F, Herlin C, Mojallal A, Sinna R, Ayestaray B, et al. (2016) A Systematic Review and Meta-Analysis of Perforator-Pedicled Propeller Flaps in Lower Extremity Defects: Identification of Risk Factors for Complications. Plast Reconstr Surg 137: 314-331.
- Wu CC, Lin PY, Chew KY, Kuo YR (2014) Free tissue transfers in head and neck reconstruction: complications, outcomes and strategies for management of flap failure: analysis of 2019 flaps in single institute. Microsurgery 34: 339-344.
- Wong CH, Cui F, Tan BK, Liu Z, Lee HP, et al. (2007) Nonlinear finite element simulations to elucidate the determinants of perforator patency in propeller flaps. Ann Plast Surg 59: 672-678.
- Demir A, Acar M, Yldz L, Karacalar A (2006) The effect of twisting on perforator flap viability: An experimental study in rats. Ann Plast Surg 56: 186-189.
- Izquierdo R, Dobrin PB, Fu K, Park F, Galante G (1998) The effect of twist on microvascular anastomotic patency and angiographic luminal dimensions. J Surg Res 78: 60-63.
- Tos P, Innocenti M, Artiaco S, Antonini A, Delcroix L, et al. (2011) Perforator-based propeller flaps treating loss of substance in the lower limb. J OrthopTraumatol 12: 93-99.
- Saint-Cyr M, Schaverien M, Arbique G, Hatef D, Brown SA, et al. (2008) Three- and four-dimensional computed tomographic angiography and venography for the investigation of the vascular anatomy and perfusion of perforator flaps. Plast Reconstr Surg121: 772-780.
- Innocenti M, Menichini G, Baldrighi C, Delcroix L, Vignini L, et al. (2014) Are There Risk Factors for Complications of Perforator-based Propeller Flaps for Lower-extremity Reconstruction? Clin OrthopRelat Res 472: 2276-2286
- Rand RP, Cramer MM, Strandness DE Jr (1994) Color-flow duplex scanning in the preoperative assessment of TRAM flap perforators: A report of 32 consecutive patients. Plast Reconstr Surg. 93: 453-459.
- Ono S, Hayashi H, Ohi H, Ogawa R (2017) Imaging Studies for Preoperative Planning of Perforator Flaps: An Overview. Clin Plast Surg 44: 21-30.
Citation: Feitosa RGF, de Oliveira GAF, Filho IDdeAOSF, Gomes HC, Ferreira LM (2021) Propeller Flap: Surgical Option after Resection of Lower Limb Melanoma. J Clin Dermatol Ther 7: 093.
Copyright: © 2021 Roney Gonçalves Fechine Feitosa, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

