
Journal of Medicine Study & Research Category: Medical
Type: Review Article
Role of IDD Therapy in the Back and Neck Pain
*Corresponding Author(s):
Gourishankar PatnaikDepartment Of Orthopedics And Spine Surgery, American Spine Center, Muscat, Sultanate Of Oman, Oman
Tel:+91 9853674074,
Email:drgspatnaik@gmail.com
Received Date: Dec 12, 2017
Accepted Date: Jun 08, 2018
Published Date: Jun 22, 2018
Abstract
Intervertebral Differential Dynamics (IDD) Therapy treatment is a non-surgical spinal decompression programme for low back pain, neck pain and some related conditions. It was developed in the late 1990’s to address the failings of traditional traction and the natural limitations of what can be achieved with the hands alone. IDD Therapy can isolate each lumbar vertebra (L1, L2, L3, L4 or L5) and distract the vertebrae surrounding an injured disc 5 to 7 millimeters. The 25 to 30 minute treatment provides static, intermittent, and cycling forces on structures that may be causing low back pain. Negative pressure promotes the diffusion of water, oxygen, and nutrients into the vertebral disc area, thereby re-hydrating the degenerated disc. Repeated pressure differential promotes retraction of a herniated nucleus pulposus (the elastic core of the intervertebral disc). The IDD Therapy treatment can reduce pressure on the vertebral joints, promote retraction of herniated discs, and promote self-healing and rehabilitation of damaged discs, thereby relieving low back pain.
This article highlights the biomechanics, indications and treatment protocol of this important non-surgical treatment regimen of back and neck pain.
This article highlights the biomechanics, indications and treatment protocol of this important non-surgical treatment regimen of back and neck pain.
Keywords
IDD; Intermittent distraction; Intervertebral disc; Spine
INTRODUCTION
Back pain affects nearly everyone at some point during their life. Whilst most back pain resolves itself or with a short course of treatment, for some people back pain can become an unwelcome companion. Neck pain affects thousands of people every year and yet treatment options for neck pain are somewhat limited in comparison to back pain. Traction therapy has been utilized in the treatment of low back pain for decades. The most recent incarnation of traction therapy is non-surgical spinal decompression therapy which can cost over $100,000. This form of therapy has been heavily marketed to manual therapy professions and subsequently to the consumer. The purpose of this paper is to initiate a debate pertaining to the relationship between marketing claims and the scientific literature on non-surgical spinal decompression. Traction as a therapeutic intervention in the treatment of low back pain has existed for many years. Its use has progressed from simple static traction to intermittent motorized traction. A recent systematic review found only seven randomized controlled trials for intermittent motorized traction and six reported no difference in outcomes between the traction groups and the control groups. The most recent incarnation of traction has been a form of intermittent motorized traction commonly referred to as spinal decompression therapy. Developers and manufacturers of the equipment along with clinicians often consider it to be a unique form of traction.
Intervertebral Disc Decompression (IDD) is a modern non-surgical technology providing decompression therapy to the spine. It comprises of a series of treatment sessions that are specifically designed for each patient. The Accu SPINA and SDS SPINA are CE and FDA cleared Class II medical devices, licenced to deliver IDD Therapy spinal decompression (Figure 1).
Intervertebral Disc Decompression (IDD) is a modern non-surgical technology providing decompression therapy to the spine. It comprises of a series of treatment sessions that are specifically designed for each patient. The Accu SPINA and SDS SPINA are CE and FDA cleared Class II medical devices, licenced to deliver IDD Therapy spinal decompression (Figure 1).
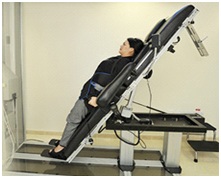
Figure 1: IDD machine by AcuSpina.
Manual therapists use a variety of techniques to treat neck pain but when these standard treatments fail to produce adequate results, the treatment options are very limited. IDD Therapy is the non-surgical spinal decompression treatment for people suffering with chronic back pain and neck pain. Treatment works by gently distracting and mobilizing targeted spinal segments using a series of carefully controlled pulling forces which we call distraction forces. The goal of treatment is to address the causes of pain.
Every aspect of the treatment is recorded and this enables clinicians to accurately monitor progress and adjust treatment appropriately, as (part of a commitment to evidence-based medicine. The distraction helps to improve mobility in the painful area and this is important for healing. It also helps relieve pressure on structures such as the intervertebral disc, spinal nerves and the joints of the vertebrae themselves, which can be causing pain.
A key benefit of IDD Therapy is the ability to adjust and focus distraction forces to a targeted level of the spine. This is achieved using precisely measured angles, which are adjusted deepening on the level of the spine being treated.
Features
• Computerized & personalized program based on the patient’s pathology
• Mobilize and manipulate specific spinal segments to induce negative intradiscal pressure
• Designed to provide static, intermittent and cyclic oscillation forces
• Forces applied to a specific disc in variable direction, frequency and amplitude
• Mobilize and manipulate specific spinal segments to induce negative intradiscal pressure
• Designed to provide static, intermittent and cyclic oscillation forces
• Forces applied to a specific disc in variable direction, frequency and amplitude
How does IDD work?
An intervertebral disc (or intervertebral fibrocartilage) lies between adjacent vertebrae in the vertebral column. Each disc forms a fibro cartilaginous joint (a symphysis), to allow slight movement of the vertebrae, and acts as a ligament to hold the vertebrae together. Intervertebral discs rely on movement and pressure differentials for hydration and nutritional pathways (Figure 2). Compression is the number one enemy of the intervertebral disc and that is why “decompression” has always been appealing and why releasing pain to allow movement in the vertebral joints is a key objective of any spinal treatment. Traction in one form or another has been around for centuries but the technology and knowledge of the spine has only taken off in the last 20 years to enable the treatment to evolve.
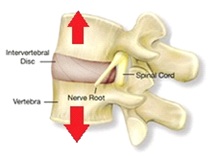
Figure 2: Disc with nerve roots.
Opening targeted spinal segments to create negative pressure is what separates IDD Therapy spinal decompression from traditional traction. IDD Therapy is not a cure-all, but it is a highly-effective treatment tool which when used as part of a complete program of care, offers clinicians the opportunity to tackle back pain, neck pain and in particular disc-related conditions in a manner previously not possible [1].
This technology is designed to provide non-surgical treatment utilizing differential dynamics. This relieves pressure on the spinal nerves involved, especially those associated with herniated discs, degenerative disc disease, posterior facet syndrome, and alleviates sciatica. With intermittent distraction, technique of IDD the spinal decompression has a maximum high tension and a low tension and the low force does not go to zero thereby maintaining the tension throughout the treatment (Figure 3).

Figure 3: Chart showing Intermittent Distraction.
The treatment protocol achieves these effects through decompression of intervertebral discs, unloading through distraction and positioning. Each treatment session is designed according to the level of problem. During the session, the patient is closely monitored and after 10 treatments, the patient is reviewed for progress, which can be in terms of pain, motor activity, sensation, function and ROM.
PARAMETERS
Patient specific information is entered into the computer and the computer analyzes the data and creates a specific protocol.
• Progression Time
• Decompression Weight
• Regression Time
• High Hold
• High Tension
• Low Hold
• Oscillation Parameters
• Transition Time
• Frequency
• Target Level L4, L5, S1
• Amplitude
• Angulation
• Progression Time
• Decompression Weight
• Regression Time
• High Hold
• High Tension
• Low Hold
• Oscillation Parameters
• Transition Time
• Frequency
• Target Level L4, L5, S1
• Amplitude
• Angulation
ANGULATION SYSTEM
The IDD system can isolate each vertebra (L1, L2, L3, L4, L5 etc.,) depends on the angulation in the set up.
TREATMENT PROTOCOL
25 session, 20 sessions over 10 weeks and 5-maintenance session over 5 months. This will insure long-term success. Patient starts to feel better after the 5th-7th session. IDD is a highly integrated software program allowed to keep real time tracking of the force applied to the specific segment of the spine that is injured The IDD program gives real time patient response, to the specific program applied during therapy session to ensure suitability of the forces applied.
The first graph illustrates the patient is lagging on the IDD Graph (Figure 4). The graphs below then detail specifically how we can cater to each patient depending on their specific need (Figure 5). Whether they need low, medium, or high level oscillation. We also have low and high amplitude.
The first graph illustrates the patient is lagging on the IDD Graph (Figure 4). The graphs below then detail specifically how we can cater to each patient depending on their specific need (Figure 5). Whether they need low, medium, or high level oscillation. We also have low and high amplitude.
Figure 4: Graph illustrating the patient is lagging on the IDD Graph.
Figure 5: The graphs below then detail specifically how we can cater to each patient depending on their specific need. Whether they need low, medium, or high level oscillation.
Once set, the patient relaxes and is ready for treatment. As with all treatments, patient safety is paramount and IDD treatment has many safety features for complete peace of mind. Treatment on the SPINA machine lasts for approximately 25 minutes, during which time there are 13 minutes when the joint is fully distracted. Unique to IDD Therapy is a patented oscillation capability, which gently mobilizes the joint at the point of maximum joint distraction [2]. As well as comfort, the oscillation enables patients to adapt to higher pulling forces whilst remaining completely relaxed for the duration of treatment. (Some patients actually go to sleep during treatment). Different oscillation waveforms gives the clinicians idea about the effectiveness of the pulling forces (Figure 6).
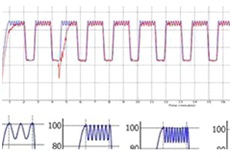
Figure 6: Different Oscillation Waveforms.
IDD Therapy is a tool used as part of a complete programme of care. As treatments progress and pain is relieved, patients are shown simple exercises to help condition the body and are advised on lifestyle changes to help get the most from the treatment and achieve lasting pain relief. The number of treatments a patient requires will vary depending on the nature of your condition. Some patients can experience relief within a few treatments, whilst other patients require a course of treatments to give the body time to adapt to changes, heal and strengthen.
IDD Therapy spinal decompression vs traction
IDD Therapy Spinal Decompression is able to distract and mobilize specific segments of the spine and thus decompress a targeted intervertebral disc. Traditional traction has been outmoded for a number of years and one of the shortcomings of traction was the inability to focus and control forces at specific spinal levels at the origin of the problem.
The four goals of IDD Therapy spinal decompression are to:
• Release pressure on nerves
• Improve Disc Health
• Re-educate soft tissues
• Re-align spinal structures
IDD Therapy treatment is applied by distracting and mobilizing targeted spinal segments at precisely measured angles, using high distraction forces which incorporate joint mobilization in a longitudinal plane [3]. Controlled forces are high enough to comfortably stretch the paraspinal tissues, open and create pressure differentials in disc space and are applied for sufficient time to have a therapeutic effect.
Ergonomic pelvic and thoracic harnesses secure the patient to the bed and a computer controlled cyclic distraction force is applied. Treatment is delivered by CE& FDA cleared Class II SPINA devices. All aspects of treatment and outcomes are recorded as part of a commitment to evidence-based medicine. Spinal decompression therapy resolves problems with the disc and removes the pressure applied to the disc by supplying nutrients and oxygen to the disc. This creates a state of non-gravitation or negative pressure within the spinal canal and reduces pressure inside the intervertebral disc by softly increasing a specific part of the disc through the decompression of a precise part of the lesion. Lee et al., reported that a group that received spinal decompression therapy and manual therapy showed a larger degree of pain reduction and a higher increase in the range of motion (ROM) of the hip joint than a group that received spinal decompression therapy and general physical therapy [4].
The four goals of IDD Therapy spinal decompression are to:
• Release pressure on nerves
• Improve Disc Health
• Re-educate soft tissues
• Re-align spinal structures
IDD Therapy treatment is applied by distracting and mobilizing targeted spinal segments at precisely measured angles, using high distraction forces which incorporate joint mobilization in a longitudinal plane [3]. Controlled forces are high enough to comfortably stretch the paraspinal tissues, open and create pressure differentials in disc space and are applied for sufficient time to have a therapeutic effect.
Ergonomic pelvic and thoracic harnesses secure the patient to the bed and a computer controlled cyclic distraction force is applied. Treatment is delivered by CE& FDA cleared Class II SPINA devices. All aspects of treatment and outcomes are recorded as part of a commitment to evidence-based medicine. Spinal decompression therapy resolves problems with the disc and removes the pressure applied to the disc by supplying nutrients and oxygen to the disc. This creates a state of non-gravitation or negative pressure within the spinal canal and reduces pressure inside the intervertebral disc by softly increasing a specific part of the disc through the decompression of a precise part of the lesion. Lee et al., reported that a group that received spinal decompression therapy and manual therapy showed a larger degree of pain reduction and a higher increase in the range of motion (ROM) of the hip joint than a group that received spinal decompression therapy and general physical therapy [4].
Decompression of a targeted spinal segment
In order to decompress a targeted level, engineers applied the principles of vector forces from physics to the spine. They observed that by focusing a controlled distraction force at a specific angle, they could open targeted spinal segments by between 5mm -7mm [1]. As the angle, which a pulling force makes with the horizontal increases, the component of force in the horizontal direction (Fx) decreases and the vertical component of force (Fy) increases (Figure 7). This causes the relative direction of the pulling force to change and therefore the focus point of application of the pulling force to move progressively along the x-axis
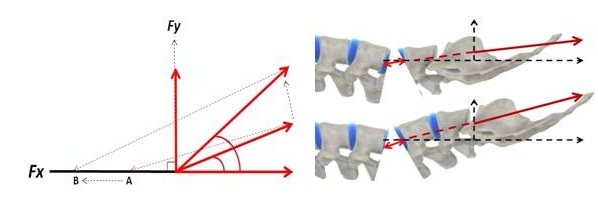
Figure 7: Measured changes in the angle of applied pulling force enable clinicians to focus and direct distraction forces accurately to injured spinal segments.
Measured changes in the angle of applied pulling force enable clinicians to focus and direct distraction forces accurately to injured spinal segments. A difference of just 5 degrees can have a bearing on the patient experience. Traditional traction was applied without thought to measuring angles to treat targeted segments. Without this knowledge, practitioners were in effect treating blindly [5].
Sinusoidal distraction force: This patented waveform replaces linear pulling forces allowing greater comfort and application of higher distraction forces of up to half body weight plus 5-10kgs (Figure 8). Patient comfort was a shortcoming for some traction machines and the risk of applying adequate force to distract the spine was that the patient could go into spasm, causing an actual increase in intradiscal pressure and pain [2].Longer treatment duration: Twenty-five minute treatment during which time joints are distracted for 13 times to a high tension, whilst soft tissues are worked and remain under constant tension. With traditional traction, not only was it uncomfortable for patients to tolerate higher distraction forces for adequate time (necessary to open the disc space), traction was applied for shorter periods to accommodate other treatment techniques within a standard 30-minute treatment slot.Thus whilst some patients might feel some comfort during traction, traction was applied for insufficient time to have an adequate therapeutic effect. A case of fitting the treatment to the needs of the clinic timetable rather than to the therapeutic objectives of treatment, which require a longer treatment time. After completion of 25 minute of treatment on the IDD machine the distraction and oscillation graph is studied (Figure 9).
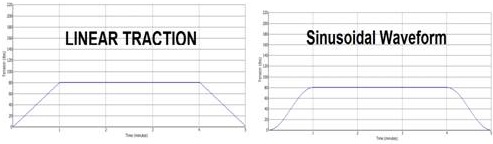
Figure 8: Linear Traction vs Sinusoidal waveform.
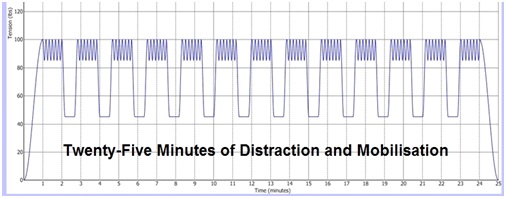
Figure 9: Graph showing 25 minutes of distraction and oscillation.
JOINT MOBILIZATION
The sinusoidal waveform allows for the application of oscillatory forces to mobilize the joint in a longitudinal, rather than anterior-posterior plane at the point when the joint is distracted. When mobilizing any other joint in the body, clinicians open the joint and then apply mobilization to so not to rub the joint surfaces and to create a synovial pumping mechanism. The challenge with the spine is to not only distract the vertebrae longitudinally to decompress the disc, but also to apply adequate force, hold it and then mobilize at the point of maximum distraction (Figure 10).
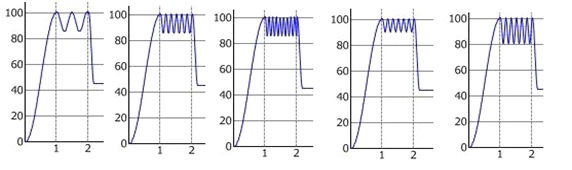
Figure 10: Patterns of graph after IDD treatment.
McClure et al., show that 92% of 129 patients considered surgical candidates had a greater than 50% reduction in pain with IDD Therapy [6].
Schimmel et al., show IDD Therapy to be no different from sham treatment whilst Shealy et al., show pain relief at the end of treatment and continuous pain reduction one year after completion of treatment [7,8].
SCANNING
MR Scanning is much more widely available now. IDD Therapy providers use an MRI scan to rule out contraindications and to assist in both the diagnosis and setting of the treatment plan. Whilst a disc prolapse may be asymptomatic, many are not (Figure 11).
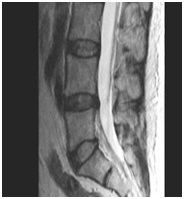
Figure 11: MRI scan of LS Spine.
Traditional traction was applied in most cases with a try it and see approach without the benefit of a scan. IDD Therapy providers know that a patient with a severely degenerated disc will take longer to notice changes than a patient with a large disc prolapsed. With traction, not only did the clinician have an inadequate tool to treat targeted segments, they didn’t have the benefit of seeing the underlying pathology. Thus if a patient did not respond to treatment after a few sessions, that may not have implied that the treatment was ineffective, rather than the treatment plan had not taken account of the condition and likely response time! Negative pressure promotes the diffusion of water, oxygen, and nutrients into the vertebral disc area, thereby re-hydrating the degenerated disc. Repeated pressure differential promotes retraction of a herniated nucleus pulposus (the elastic core of the intervertebral disc) [9].
CONCLUSION
In order to decompress (take pressure off) a joint, it is necessary to distract it in the opposite direction to the compressive force. Where a joint has become stiff and immobile, gentle mobilization at the point of distraction helps to improve mobility in the joint and allow the natural mechanisms, which keep joints healthy to operate freely. Following salient features of IDD therapy enable patient for an optimal relief.
• Improved harnessing secures the pelvis
• Measured angle of distraction
• Computer controlled sinusoidal waveform
• Cyclical distraction, higher distraction forces
• Ergonomic harnesses
• Patient completely relaxed for 25 minutes, plus
• Benefit of a scan to determine the treatment plan enable the patient to get optimal benefit from back and neck pain
IDD Therapy Spinal Decompression applies new technology to physical laws to enable clinicians to distract and mobilize targeted spinal segments as part of a complete programme of care, including manual therapy and exercise rehabilitation. Hence rather than a brand new revolution, IDD Therapy treatment is a true paradigm shift in non-invasive spinal care. We hope that in these pages you will get a good understanding of how IDD Therapy can help your patients. There is very limited evidence in the scientific literature to support the effectiveness of non-surgical spinal decompression therapy. This intervention has never been compared to exercise, spinal manipulation, standard medical care or other less expensive conservative treatment options which have an ample body of research demonstrating efficacy. Considering the cost-benefit relationship, many better researched and less expensive treatment options are available to the clinician. This study examined the clinical effects of conducting spinal decompression therapy and general traction therapy, which are non-surgical treatment methods, for patients with intervertebral disc herniation. In conclusion, physical therapists may be required to select an appropriate treatment method considering the condition of a patient, cost, and time. Follow up studies should be conducted on the long-term effects of these therapies, increasing the treatment period and the number of treatments.
In the future, we see the IDD Therapy spinal treatment programme as a key cost-effective resource to tackle both back pain itself and the ever-increasing costs of chronic back pain to society and health care.
• Improved harnessing secures the pelvis
• Measured angle of distraction
• Computer controlled sinusoidal waveform
• Cyclical distraction, higher distraction forces
• Ergonomic harnesses
• Patient completely relaxed for 25 minutes, plus
• Benefit of a scan to determine the treatment plan enable the patient to get optimal benefit from back and neck pain
IDD Therapy Spinal Decompression applies new technology to physical laws to enable clinicians to distract and mobilize targeted spinal segments as part of a complete programme of care, including manual therapy and exercise rehabilitation. Hence rather than a brand new revolution, IDD Therapy treatment is a true paradigm shift in non-invasive spinal care. We hope that in these pages you will get a good understanding of how IDD Therapy can help your patients. There is very limited evidence in the scientific literature to support the effectiveness of non-surgical spinal decompression therapy. This intervention has never been compared to exercise, spinal manipulation, standard medical care or other less expensive conservative treatment options which have an ample body of research demonstrating efficacy. Considering the cost-benefit relationship, many better researched and less expensive treatment options are available to the clinician. This study examined the clinical effects of conducting spinal decompression therapy and general traction therapy, which are non-surgical treatment methods, for patients with intervertebral disc herniation. In conclusion, physical therapists may be required to select an appropriate treatment method considering the condition of a patient, cost, and time. Follow up studies should be conducted on the long-term effects of these therapies, increasing the treatment period and the number of treatments.
In the future, we see the IDD Therapy spinal treatment programme as a key cost-effective resource to tackle both back pain itself and the ever-increasing costs of chronic back pain to society and health care.
REFERENCES
- Shealy N, Leroy P (1998) New Concepts in Back Pain Management. AJPM 1: 239241.
- Shealy CN, Koladia N, Wesemann MM (2005) Long-term effect analysis of IDD therapy in low back pain: a retrospective clinical pilot study. Am J Pain Manage 15: 93-97.
- Schaufele MK, Newsome M (2011) Intervertebral Diff erential Dynamics (IDD) Therapy vs. Exercise Based Physical Therapy -Results from a Randomized Controlled Trial. Phys Med Rehab Kuror 21: 34-40.
- Lee Y, Lee CR, Cho M (2012) Effect of decompression therapy combined with joint mobilization on patients with lumbar herniated nucleus pulposus. J Phys Ther Sci 24: 829-832.
- Eyerman EL (1998) Simple Pelvic Traction Gives Inconsistent Relief to Herniated Lumbar Disc Sufferers. Journal of Neuroimaging, Orlando, Florida, USA.
- McClure D, Farris B (2006) Intervertebral Differential Dynamics Therapy - A New Direction for the Initial Treatment of Low Back Pain. European Musculoskeletal Review: 45-48.
- Shealy CN, Borgmeyer V (1997) Decompression, Reduction, and Stabilization of the Lumbar Spine: A Cost- Effective Treatment for Lumbosacral Pain. American Journal of Pain Management 7: 63-65.
- Schimmel JJ, de Kleuver M, Horsting PP, Spruit M, Jacobs WC, et al. (2009) No effect of traction in patients with low back pain: a single centre, single blind, randomized controlled trial of Intervertebral Differential Dynamics Therapy. Eur Spine J 18: 1843-1850.
- Cholewicki J, Lee AS, Reeves NP, Calle EA (2009) Trunk muscle response to various protocols of lumbar traction. Man Ther 14: 562-566.
Citation: Patnaik G (2018) Role of IDD Therapy in the Back and Neck Pain. J Med Stud Res 1: 002.
Copyright: © 2018 Gourishankar Patnaik, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
© 2026, Copyrights Herald Scholarly Open Access. All Rights Reserved!

