
Staphylococcal Scarlet Fever in a Child
*Corresponding Author(s):
Cristina F RodriguesDepartment Of Pediatrics, Hospital De Braga, Sete Fontes - São Victor, Braga, Portugal
Tel:+351 913154545,
Email:cristinaafrodrigues@hotmail.com
Abstract
Staphylococcal scarlet fever is a rare infectious skin disease, with few cases reported in literature. The etiology is related to the staphylococcal epidermolytic toxin. It manifests itself as a mild form of staphylococcal scalded skin syndrome, being characterized by a scarlet fever exanthema (without blistering), fever and affection of the general condition, with progression to desquamation in large flaps. Systemic antibiotic treatment should be initiated. The authors describe a case of this pathology in a child.
Keywords
Exanthema; Exfoliatins; Staphylococcal scalded skin syndrome
Introduction
Staphylococcus aureus is a constant member of microbial flora in 10-20% of the population [1] and is responsible for several types of skin and soft tissue infections, often toxin-mediated [2,3]. Staphylococcal Scarlet Fever (SSF) is a rare infectious skin disease, epidermolytic toxin-mediated, described as a mild manifestation of staphylococcal Scalded Skin Syndrome (SSSS) [1,3,4-7]. As a mild form of SSSS, the differential diagnosis of SSF includes other infections, inflammatory conditions and toxicities: SSSS, epidermolytic hyperkeratosis, drug eruption, drug induced toxic epidermal necrolysis, scarlet fever and streptococcal scarlet fever [5,8-9]. SSF is characterized by fever, affection of general condition and a scarlatiniform exanthema, accentuated in the flexural areas, but no enanthem or bullae, no strawberry tongue or palatal petechiae [1,7,9-10]. Evolves into desquamation in large flaps, but does not progress to blister formation [7,9].
Case Report
A previously healthy three-year-old girl developed a progressive erythematous exanthema, beginning in the chest and extending to axillary and cubital folds after sun exposure with her usual sunscreen. Since four days before, she was under treatment with topical mupirocin and an antiseptic bath product due to impetigo in nasal and mentonian regions. The next day she was observed by her medical provider, diagnosed with tonsillitis and medicated with oral amoxicillin. Two days later she came to our medical department for worsening of the exanthema and pruritus, facial and limb edema, poor oral intake and fever in the last 24 hours. On physical examination, she presented a generalized erythematous exanthema (including face and scalp), mainly in the upper anteroposterior thoracic region (Figure 1), marked xerosis, edema and heat in the limbs and face (mainly perioral), with cheilitis (Figure 2), a skin detachment area of approximately 4% of the body surface (Figure 3) with negative Nicolsky sign and a bilateral punctiform oropharyngeal exudate. The analytical study had no significant alterations, infectious serologies were unremarkable and group A Streptococcus antigen test was negative.Given the suspicion of a staphylococcal scarlet fever, she started intravenous flucloxacillin and clindamycin (150 and 35 mg/kg/day, respectively). A methicillin-sensitive Staphylococcus aureus was isolated in bilateral axillary swab. She was discharged after three days with symptomatic improvement, completing ten days of oral antibiotic.
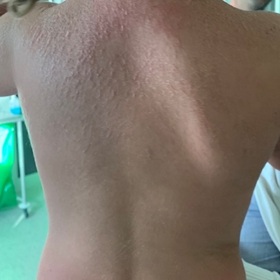 Figure 1: Erythematous exanthema on the upper posterior thoracic region.
Figure 1: Erythematous exanthema on the upper posterior thoracic region.
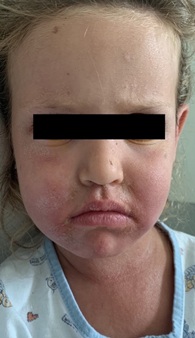 Figure 2: Xerosis and edema of the face, mainly perioral, with cheilitis.
Figure 2: Xerosis and edema of the face, mainly perioral, with cheilitis.
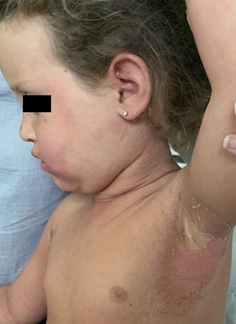 Figure 3: Skin detachment.
Figure 3: Skin detachment.
Discussion
In this case, the topical antiseptic, amoxicillin and sun exposure became confounders responsible for different diagnostic hypothesis. We considered SSF, SSSS and drug induced toxic epidermal necrolysis. Failure to treatment with mupirocin is an important variable to take in account. The diagnosis was established based on clinic and laboratory results. Antibiotic treatment targeting toxin production should be initiated in suspected forms of toxin-mediated infections [3,5]. In mild forms of SSSS the lesions should be cleaned and dried with compresses [5]. Topical antibiotics are not effective and should not be used due to unpredictable absorption [5]. The risk of sepsis or septic shock is low and skin injury should be avoided to limit the risk of skin blistering [3]. The authors pretend to alert to the occurrence of this rare pathology little described on literature, requiring a high level of suspicion for a correct diagnosis and treatment.
Declaration of Interest
The authors declare that there were no conflicts of interest in conducting this work.
Funding Sources
There were no external funding sources for the realization of this paper.
References
- Josa PL, Rubio CG, Rebollo JC, Mendizábal BL (2013) Escarlatina estafilocócica como manifestación atenuada del síndrome de escaldadura estafilocócica. RevPediatr Aten Primaria 15: 65-67.
- Lowy FD (1998) Staphylococcus aureus infections. N Engl J Med 339: 520-532.
- Courjon J, Hubiche T, Phan A, Tristan A, Bès M, et al. (2013) Skin findings of staphylococcus aureus toxin-mediated infection in relation to toxin encoding gene. Pediatr Infect Dis J 32: 727-730.
- Weisse ME (2001) The fourth disease, 1900-2000. Lancet 357: 299-301.
- Ladhani S, Joannou CL, Lochrie DP, Evans RW, Poston SM (1999) Clinical, microbial, and biochemical aspects of the exfoliative toxins causing staphylococcal Scalded-skin syndrome. Clin Microbiol Rev 12: 224-242.
- Feldman CA (1962) Staphylococcal scarlet fever. N Engl J Med 267: 877-878.
- Carvalho L, Leça A (2008) Infecções da pele e dos tecidos moles. In: Amaral JV. Tratado de Clínica Pediátrica, (2nd edn). Abbott Laboratórios, Lda, Amadora, Portugal. Pg no: 1416-1429.
- McMahon P (2019) Staphylococcal scalded skin syndrome. UpToDate, Massachusetts, United States.
- Diiorio DA, Humphrey SR (2019) Staphylococcal scalded skin syndrome (Ritter disease). In: Kliegman RM, ST Geme JW (eds.). Nelson textbook of pediatrics, (21st edn). Elsevier, Philadelphia, Pennsylvania. Pg no: 13710-13713.
- Wang CC, Lo WT, Hsu CF, Chu ML (2004) Enterotoxin B is the predominant toxin involved in staphylococcal scarlet fever in Taiwan. Clin Infect Dis 38: 1498-1502.
Citation: Rodrigues CF, Ribeiro A, Faria C, Ferreira C, Silva H, et al. (2021) Staphylococcal Scarlet Fever in a Child. J Neonatol Clin Pediatr 8: 071.
Copyright: © 2021 Cristina F Rodrigues, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

