
Subclavian Steal Syndrome Due to a Subtotal-Occlusion of an Aberrant Right Subclavian (Lusorian) Artery-A Case Report
*Corresponding Author(s):
Ahmad Al HalabiDepartment Of Vascular Surgery And Endovascular Medicine, General Hospital Of Celle, Lower Saxony, Germany
Tel:+ 49 51417226029,
Email:ahmed.alhalabi@live.com
Abstract
Despite its rare incidence, an occlusion or near-occlusion of an aberrant right subclavian artery (lusorian artery) presents a challenging pathology to treat. While open surgical approaches have been regarded as first-line treatment for a long time, endovascular solutions have proven over the last years to be a less invasive yet effective alternative, like in many other vascular conditions.
We report on a 47-year-old female complaining of dizziness and vertigo, together with a weakness in the right arm aggravated by manual activities.
Other than obesity (BMI of 34 kg/m2) and smoking (45 Pack years), no other relevant history was present. A series of intensive neurological diagnostics revealed no pathological findings. However, duplex ultrasound of the neck vessels showed a retrograde flow in the right vertebral artery secondary to a subtotal occlusion of the right Subclavian Artery (SA). Complimentary CT-angiography additionally revealed an aberrant origin of the SA from the descending aorta.
Due to the location of the lesion and the expected technical difficulties in obese patients, we opted for an interventional endovascular angioplasty. Through this case report we aim to present the role of endovascular interventions in the treatment of occlusions and stenoses in the context of an abnormal anatomy.
Keywords
BACKGROUND
An aberrant origin with an atypical course of the right subclavian artery could result in many pathological conditions, which have been classified by Kieffer et al. into four major groups [4]:
• Group 1: Patients with dysphagia caused by non-aneurysmal aberrant RSA (dysphagia lusoria)
• Group 2: Patients with symptomatic occlusive disease of non-aneurysmal aberrant RSA
• Group 3: Patients with aneurysmal aberrant RSA without aortic lesions, with or without oesophageal compression or arterial thromboembolism
• Group 4: Patients with an aortic (usually aneurysmal) lesion involving the origin of the aberrant RSA, with or without aberrant RSA aneurysm
Owing to the general trend in modern vascular surgery, open treatment modalities of the above conditions are being increasingly replaced by novel endovascular solutions [5], unless other aortic arch deformations necessitate an open approach [6]. Surgical therapies themselves have been improved with hybrid-techniques [6], especially in case of dysphagia and aneurysms, resulting in low postoperative morbidity [7,8]. Nevertheless, no guidelines or systematic reviews addressing treatment regimens have been published so far.
CASE PRESENTATION
History
Other than Obesity (BMI of 34 kg/m2), smoking (45 Pack years) and a conservatively treated cervical disc protrusion (C5-C6), her previous medical history was unremarkable.
Examination and diagnostics
Clinically, the patient was in a good general condition. Brachial blood pressure was considerably lower on the right side and the radial pulse was relatively weaker (Δ 60 mmHg). The clinical neurological exam was normal and showed no focal or general pathologies (including normal reflexes and no nystagmus).
Blood tests revealed elevated cholesterine and LDL values. Taking the blood pressure difference and the existing cardiovascular risk factors into consideration, a duplex ultrasound of the supraaortic vessels was carried out. While both carotid arteries exhibited a regular flow, post-stenotic disturbances (peak systolic velocity of up to 270 m/s) were found in the right subclavian artery. In addition, the right vertebral artery showed a retrograde flow which decreased upon compression of the arm, suggesting a subclavian steal syndrome.
Further investigation with CT angiography showed an 8 mm long high-grade stenosis of the right subclavian artery, directly proximal to the origin of the vertebral artery (Figure 1), together with an aberrant origin directly from the descending aorta (Figure 2).
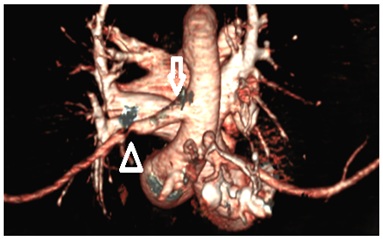 Figure 1: Computer assisted 3D reconstruction of the aortic arch showing the aberrant origin of the right subclavian artery directly from the descending aorta (arrow) and the stenosis (triangle).
Figure 1: Computer assisted 3D reconstruction of the aortic arch showing the aberrant origin of the right subclavian artery directly from the descending aorta (arrow) and the stenosis (triangle).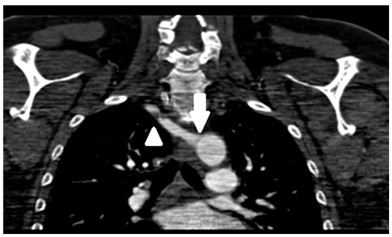 Figure 2: CT angiogram showing the aberrant origin of the right subclavian artery directly from the descending aorta (arrow) and the stenosis (triangle).
Figure 2: CT angiogram showing the aberrant origin of the right subclavian artery directly from the descending aorta (arrow) and the stenosis (triangle).How we did it
The guide wire was then withdrawn, and a direct injection of contrast medium was used to identify and locate the target vessel, opposite to which the tip of the Bernstein-catheter was placed. Using slight axial rotation and supporting the tip of the catheter again the ridge of the subclavian branch, the guide wire was eventually successfully inserted in the right subclavian artery after several attempts. The catheter was then placed proximally, and the stenosis was identified through an antegrade angiography of the right subclavian artery, where the ipsilateral vertebral flow was absent (Figure 3). The Bernstein catheter was then exchanged with a 7F, 90 cm long guiding sheath (Destination®, Terumo Interventional System) over the guide wire in Seldinger-technique. A balloon expandable Stent (8 mm diameter, 27 mm length, Express LD®, Boston Scientific Corporation) was the placed into the stenotic segment and successfully implanted. The final angiographic examination showed a successful dilatation of the stenosis with a regular antegrade flow through the vertebral artery (Figure 4). An incidentally-diagnosed high grade stenosis of the right common iliac artery was then managed with the implantation of a 9 mm x 25 mm balloon expandable Stent (Express LD®, Boston Scientific Corporation).
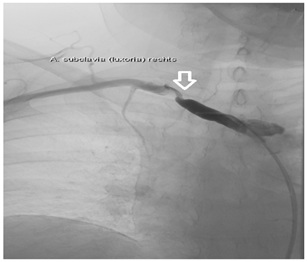 Figure 3: Antegrade angiography showing high grade stenosis of the lusorian artery (Arrow). Note the absence of the right subclavian artery.
Figure 3: Antegrade angiography showing high grade stenosis of the lusorian artery (Arrow). Note the absence of the right subclavian artery.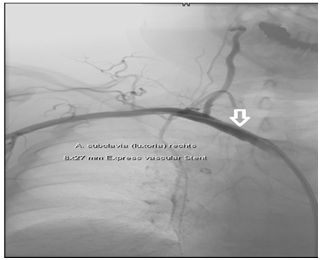 Figure 4: Result post-angioplasty showing successful dilatation of the subclavian stenosis with a regular antegrade flow in the right vertebral artery. The stent location is marked with an arrow.
Figure 4: Result post-angioplasty showing successful dilatation of the subclavian stenosis with a regular antegrade flow in the right vertebral artery. The stent location is marked with an arrow.RESULTS AND FOLLOW-UP
DISCUSSION
Through this case report we aim at drawing attention to the unique aspects of vascular anatomic variations such as the lusorian artery in the management, while praising the role of endovascular interventions in the treatment of occlusions and stenoses in such challenging anatomies. We also want to emphasize the importance of a global assessment of the cardiovascular patients and the key role played by interdisciplinary team work in contributing to correct diagnoses and effective treatment.
CONCLUSION
REFERENCES
- Polguj M, Chrzanowski L, Kasprzak JD, Stefa?czyk L, Topol M, et al. (2014) The aberrant right subclavian artery (arteria lusoria): the morphological and clinical aspects of one of the most important variations--a systematic study of 141 reports. ScientificWorldJournal 2014: 292734.
- Gul A, Corbacioglu A, Bakirci IT, Ceylan Y (2012) Associated anomalies and outcome of fetal aberrant right subclavian artery. Arch Gynecol Obstet 285: 27-30.
- Song MJ, Han BH, Kim YH, Yoon SY, Lee YM, et al. (2017) Prenatal diagnosis of aberrant right subclavian artery in an unselected population. Ultrasonography 36: 278-283.
- Kieffer E, Bahnini A, Koskas F (1994) Aberrant subclavian artery: surgical treatment in thirty-three adult patients. J Vasc Surg 19: 100-109.
- Jahangeer S, Bashir M, Harky A, Yap J (2018) Aberrant subclavian: new face of an old disease. J Vis Surg 4: 108.
- Atay Y, Engin C, Posacioglu H, Ozyurek R, Ozcan C, et al. (2006) Surgical approaches to the aberrant right subclavian artery. Tex Heart Inst J 33: 477-481.
- Wooster M, Back M, Sutzko D, Gaeto H, Armstrong P, et al. (2018) A 10-Year Experience Using a Hybrid Endovascular Approach to Treat Aberrant Subclavian Arterial Aneurysms. Ann Vasc Surg 46: 60-64.
- Debonnaire G, Verbist J, Peeters P (2012) Dysphagia lusoria. Indications and surgical approaches for non-aneurysmatic aberrant right subclavian artery. Acta Chir Belg 112: 237-239.
Citation: Al Halabi A, Baharmast K, Shirinova A (2019) Subclavian Steal Syndrome Due to a Subtotal-Occlusion of an Aberrant Right Subclavian (Lusorian) Artery-A Case Report. J Angiol Vasc Surg 4: 018.
Copyright: © 2019 Ahmad Al Halabi, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

