
Top-Down Redistribution of Brain Circulation from Thalamus to Cerebellum in Response to Intravenous Laser Irradiation of Blood in Case of Chronic Cerebellar Stroke: Pilot Observation from Brain Images
*Corresponding Author(s):
Shin-Tsu ChangDepartment Of Physical Medicine And Rehabilitation, Taichung Veterans General Hospital, Taichung, Taiwan, Department Of Physical Medicine And Rehabilitation, Tri-Service General Hospital, School Of Medicine, National Defense Medical Center, Taipei, Taiwan
Tel:+886 935605578,
Email:ccdivlaser1959@gmail.com
Abstract
Background: The cerebellum is a part of the brain that plays a vital role in most physical movement. However, function of the cerebellum may be impaired when the blood vessel is blocked or bleeding, so called cerebellar stroke, causing complete interruption to a portion of the cerebellum. Even though the mortality rate has declined recently, many patients still suffer from limited motor function after years.
Case report: A 59-year-old woman experienced cerebellar stroke 2 years ago. Her motor function was obviously affected, corresponding to the decreased perfusion of the cerebellum observed from brain images. The Intravascular Laser Irradiation of Blood (ILIB) intervened later. After two ILIB courses, her legs weakness and unsteady gait, have been improving, along with increased perfusion in the bottom of cerebellum viewed from the second images. In addition, the perfusion in the thalamus decreased accidentally.
Conclusion: We deduce that the distribution of brain circulation was attributed to ILIB, which improve the motor function simultaneously in our case. This phenomenon had been investigated in previous studies. But no one described the redistribution in cerebral blood flow in the case after stroke. Thus, we present this case and state that ILIB has therapeutic effect on patient with chronic cerebellar stroke.
Keywords
Cerebellar stroke; Cerebral blood flow; Intravenous laser irradiation of blood; Redistribution; Single-photon emission computed tomography
INTRODUCTION
Cerebral circulation is the movement of blood through the vascular complex supplying the brain. The brain accounts for about 2% of body weight, but the rate of the Cerebral Blood Flow (CBF) is typically 750 milliliters per minute among adults, representing 15% of the resting cardiac output. Simultaneously, the brain highly depends on sustained delivery of oxygen and glucose from CBF [1].
Some studies used transcranial Doppler ultrasonography for evaluating CBF after the onset of stroke [2,3]. While other study accessed CBF with positron emission tomography [4] and laser Doppler flowmetry [5]. However, we adopted Single-Photon Emission Computed Tomography (SPECT), using radiotracer like Ethyl Cysteinate Dimer (ECD) to access CBF and cerebrovascular reserve. It is another CT technique for imaging the penumbra [6].
Cerebellar stroke accounts for approximately 2% to 3% of all ischemic strokes. The majority of the deficits seem to be asymptomatic, subtle, only minor symptoms of dizziness, nausea, vomiting, unsteady gait and headache, or mimicking labyrinthitis and visceral conditions such as viral gastroenteritis [7]. Of them, balance function is crucial for posture and gait, which is expected to recover by such patients like our case.
On last three decades, ILIB has demonstrated notable effectiveness in the treatment of cardiovascular and other systemic diseases. We will report a case with cerebellar stroke, who obtained symptom relief corresponding to the changes on brain image after the administration of ILIB.
CASE PRESENTATION
A 59-year-old woman was robust prior stroke attack. She suffered from blurred vision and syncope on 2018/05/20. The symptoms accompanied with persistent dizziness, bilateral legs weakness and unsteady gait. There was neither sensory loss nor diplopia. She was brought to local hospital immediately, where MRA showed small caliber in left VA/BA, fine right VA separated from BA. She was then admitted for intensive rehabilitation and evaluation.
However, her symptoms did not improve after a month, so she came to our NS OPD for help. Frequency of blurred vision with dizziness improved after medication. But, she still suffered from bilateral legs weakness, unsteady gait and paroxysmal dizziness. She was referred to our Rehabilitation Outpatient Clinic for better motor recovery. The Tc-99m ECD brain perfusion SPECT study was done on 2018/10/25, which disclosed relative hypoperfusion in the bottom of bilateral cerebellum, left temporal region, left inferior frontal region, and left caudate nucleus (Figure 1).
 Figure 1: Brain SPECT before and after ILIB. The white to red area indicated better perfusion than the blue and green area.
Figure 1: Brain SPECT before and after ILIB. The white to red area indicated better perfusion than the blue and green area.
(A): This brain SPECT (conducted before ILIB therapy) showed hypoperfusion in the bottom of bilateral cerebellum.
(B): The second brain SPECT (conducted after ILIB therapy) showed the increased perfusion in the bottom of cerebellum.
We arranged the first two ILIB therapies on 2018/11/12 and 2018/12/24. She mentioned that there was prominent improvement with better strength of legs, while symptom with paroxysmal dizziness was noted especially in the morning. After the third course of ILIB therapy on 2019/04/26, her walking balance also got better. Furthermore, we arranged SPECT study for follow-up, which showed theperfusion in the bottom of cerebellum enhanced while the perfusion in the thalamus decreased compared with last time (Figures 1 and 2).
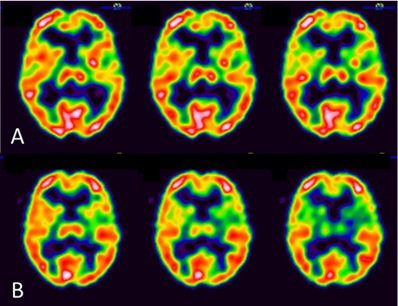 Figure 2: Brain SPECT before and after ILIB.
Figure 2: Brain SPECT before and after ILIB.
(A): This brain SPECT (conducted before ILIB therapy) showed the normal perfusion in the thalamus.
(B): The second brain SPECT (conducted after ILIB therapy) showed the perfusion in the thalamus decreased compared with last time.
Figure 3 showed the time interval of the whole clinical course, intervention, and associated evaluation. Table 1 summarized the changes in individual neural area observed from brain SPECTs.
 Figure 3: Time interval of the case and her self-feeling
Figure 3: Time interval of the case and her self-feeling
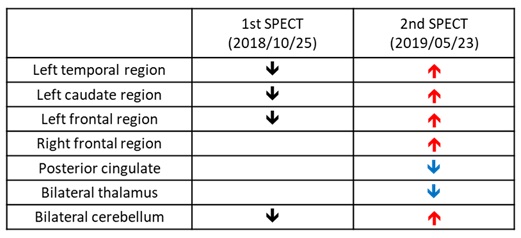 Table 1: Perfusion changes of varying brain areas in brain SPECTs.
Table 1: Perfusion changes of varying brain areas in brain SPECTs.
DISCUSSION
Based on clinical pictures and brain SPECT images, after administration of ILIB, prior hypoperfusion in the bottom of cerebellum improved from the first SPECT to the second SPECT. Unexpectedly, the normal perfusion in the thalamus in the first SPECT became decreased observed in the second SPECT. Therefore, a kind of redistribution in CBF occurred in our case after 3 courses of ILIB.
Jackman & Iadecola [8] stated that there are many safeguards to keep cerebral circulatory system from fluctuations in blood supply, which may be harmful and even contribute to stroke. One of safeguards is functional hyperemia, the increase in blood flow coupled to neuronal metabolic activity, can preserve brain perfusion even with varying supply or demand. Therefore, we may deduce that those safeguards are expected to be impaired in stroke patients [8]. However, in previous study, it has been concluded that functional hyperemia may be preserved in post-stroke lesion activated by the stimulus, such as motor activation task, cerebral vasodilating agent and visual stimulation, possibly by means of sacrifice surrounding tissues [9,10]. Interestingly, we also found the similar phenomenon, termed as redistribution in our case. After three courses of ILIB, perfusion in the bottom of cerebellum increased while relative hypoperfusion in the thalamus instead, noted by SPECT. The effects of increased perfusion in the cerebellum present as advancement of motor function and walking balance.
With respect to redistribution in our case, there are many examples to show such circumstance. Maršál, et al. [11] indicated preferential supply of blood to the brain, myocardium, and adrenal glands in hypoxic fetuses, evidenced by the increased cardiac output of left ventricle in the situation of rising proportion of blood from the umbilical vein to the foramen ovale and ductus venosus. Wiegers, et al. [12] also mentioned that hypoglycemia resulted in redistribution of CBF towards the thalamus, in accordance with activation of brain regions linked to the sympathetic response to hypoglycemia. Namely, those who lacks redistribution of CBF during hypoglycemia may be associated with impaired awareness of hypoglycemia [12]. Moreover, Zhuo and his colleagues found increased blood flow in the auditory and striatal areas, along with the reduction in the visual and parietal areas, result in auditory verbal hallucinations in patient with Schizophrenia, and conclude a phenomenon of redistribution in CBF [13].
There are several tools to evaluate CBF and thus providing information on the redistribution of the blood flow supply. Brain SPECT has proven to be a reliable imaging marker of regional CBF, even in cases of luxury perfusion [14]. Because brain activity is directly related to blood flow, SPECT effectively shows us the patterns of activity in the brain. Besides, it is less harmful that allows for repeated studies for follow-up [6].
ILIB has been used for the treatment of diverse illness since 1988. It has anti-inflammatory effects, positive impact on rheological properties of the blood, declining aggregation of thrombocytes, and a better deformability of the erythrocytes, thus contributing a better supply of oxygen [15]. It can not only improve the function of the cardiovascular system, but also be applied to various disease, such as arthritis, fibromyalgia, hepatic disease, postpartum mastitis and diabetes mellitus, as its influence on amplifying oxygen supply and hence to improving microcirculation [16,17].
CONCLUSION
Based on our clinical pictures of our case, we considered ILIB has therapeutic effect on patient with chronic cerebellar stroke, resulting in redistribution of brain circulation concurrently, which enhanced perfusion over vital lesion at the expense of surrounding tissue.
CONFLICT OF INTEREST
Authors state no conflicts of interest.
REFERENCES
- Shah RS, Jeyaretna DS (2018) Cerebral vascular anatomy and physiology. Surgery (Oxford) 36: 606-612.
- Bonnin P, Leger PL, Deroide N, Fau S, Baud O, et al. (2011) Impact of intracranial blood-flow redistribution on stroke size during ischemia-reperfusion in 7-day-old rats. J Neurosci Methods 198: 103-109.
- Li L, Ke Z, Tong KY, Ying M (2010) Evaluation of cerebral blood flow changes in focal cerebral ischemia rats by using transcranial Doppler ultrasonography. Ultrasound Med Biol 36: 595-603.
- Szilágyi G, Nagy Z, Balkay L, Boros I, Emri M, et al. (2005) Effects of vinpocetine on the redistribution of cerebral blood flow and glucose metabolism in chronic ischemic stroke patients: a PET study. J Neurol Sci. 230: 275-284.
- Schiffner R, Bischoff SJ, Lehmann T, Rakers F, Rupprecht S, et al. (2017) Redistribution of cerebral blood flow during severe hypovolemia and reperfusion in a sheep model: critical role of α1-adrenergic signaling. Int J Mol Sci 18: 1031.
- Wey HY, Desai VR, Duong TQ (2013) A review of current imaging methods used in stroke research. Neurol Res 35: 1092-1102.
- De Cocker LJ, Geerlings MI, Hartkamp NS, Grool AM, Mali WP, et al. (2015) Cerebellar infarct patterns: The SMART-medea study. Neuroimage Clin 8: 314-321.
- Jackman K, Iadecola C (2015) Neurovascular regulation in the ischemic brain. Antioxid Redox Signal. 22: 149-160.
- Inao S, Tadokoro M, Nishino M, Mizutani N, Terada K, et al. (1998) Neural activation of the brain with hemodynamic insufficiency. J Cereb Blood Flow Metab 18: 960-967.
- Yamauchi H, Kudoh T, Sugimoto K, Takahashi M, Kishibe Y, et al. (2005) Altered patterns of blood flow response during visual stimulation in carotid artery occlusive disease. Neuroimage 25: 554-560.
- Maršál K (2018) Physiological adaptation of the growth-restricted fetus. Best Pract Res Clin Obstet Gynaecol 49: 37-52.
- Wiegers EC, Becker KM, Rooijackers HM, von Samson-Himmelstjerna FC, Tack CJ, et al. (2017) Cerebral blood flow response to hypoglycemia is altered in patients with type 1 diabetes and impaired awareness of hypoglycemia. J Cereb Blood Flow Metab 37: 1994-2001.
- Zhuo C, Zhu J, Qin W, Qu H, Ma X, et al. (2017) Cerebral blood flow alterations specific to auditory verbal hallucinations in schizophrenia. Br J Psychiatry 210: 209-215.
- Kim HS, Kim DI, Lee JD, Jeong EK, Chung TS, et al. (2002) Significance of 99mTc-ECD SPECT in acute and subacute ischemic stroke: comparison with MR images including diffusion and perfusion weighted images. Yonsei Med J 43: 211-222.
- Weber MH (2007) The intravenous laser blood irradiation - introduction of a new therapy. German Journal of Acupuncture and related Techniques 50: 12-23.
- Mikhaylov VA (2015) The use of Intravenous Laser Blood Irradiation (ILBI) at 630-640 nm to prevent vascular diseases and to increase life expectancy. Laser Ther 24: 15-26.
- Liu EY, Chang ST (2019) Benefits of intravascular laser irradiation of blood on motor and sensory recovery viewing from brain function images: portrait of a case with chronic Sjögren’s syndrome, transverse myelitis, and Guillain-Barré syndrome. Biomed J Sci& Tech Res 14: 10738-10741.
Citation: Tai CT, Cheng YY, Chang ST (2020) Top-Down Redistribution of Brain Circulation from Thalamus to Cerebellum in Response to Intravenous Laser Irradiation of Blood in Case of Chronic Cerebellar Stroke: Pilot Observation from Brain Images. J Phys Med Rehabil Disabil 6: 054.
Copyright: © 2020 Cheng-Ting Tai, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

