
Treatment of Acute Mediastinitis Secondary Traumatic Esophageal Perforation by Naso-Mediastinal Drainage
*Corresponding Author(s):
Jessica L BuickoDepartment Of Surgery, Weill-Cornell Medicine, New York, NY, United States
Tel:+1 518 2297711,
Email:JBuicko@med.miami.edu
Abstract
Mediastinitis secondary to esophageal perforation is a serious condition with potentially grave complications. Traditional treatment regimens involve open trans-thoracic mediastinal drainage procedures which have a high morbidity and mortality rate [1].
Surgical drainage options primarily include a trans-cervical or trans-thoracic approach. The decision of which approach to use is typically dependent on the extent of the disease process. If the disease process extends below the fourth thoracic vertebra, trans-cervical drainage is usually inadequate, and a trans-thoracic approach should be considered, or a combination of the two techniques [2].
In regard to the mortality of this condition, Corsten et al., showed a high mortality rate of patients undergoing trans-cervical drainage alone (47% mortality) versus a combined trans-cervical and trans-thoracic mediastinal approach (19% mortality, p<0.05) [3].
A thoracic approach allows for great exposure of the entire mediastinum and permits more aggressive drainage and debridement. However, entering the chest is more invasive and could potentially lead to contamination of the pleural space. Contrary to Corsten et al., and Inoue et al., demonstrated that trans-cervical drainage for patients with localized necrotizing mediastinal infections was adequate with minimal morbidity and mortality [2]. Patients with extensive necrotizing infections were more likely to develop empyema and therefore require trans-thoracic drainage, but still had favorable outcomes with a mortality rate of 13% [2].
We present the unique case of acute mediastinitis secondary to traumatic esophageal perforation treated by naso-mediastinal drainage.
Keywords
Esophageal Perforation; Mediastinitis; Thoracic Surgery; Trauma
CASE PRESENTATION
Plain chest radiography and CT scanning revealed the knife to be lodged in the mediastinum posterior to the esophagus (Figures 1A and 1B). Oral examination and flexible laryngoscopy confirmed that no part of the knife was present in the oropharynx or esophagus.
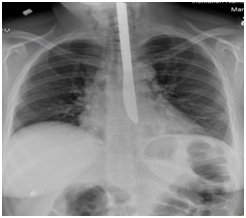
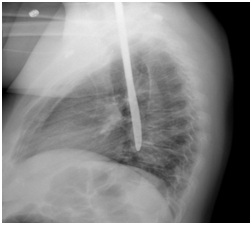
In the operating room the patient underwent trans-oral extraction of the knife under fluoroscopic guidance though a posterior esophagotomy. Upon removal of the knife, purulent drainage was observed from the extraction site.
The mediastinum was then drained with a 10 mm Jackson Pratt Drain that was secured to the patients left nares. A nasogastric tube was inserted through the patients left nares under direct visualization (Figure 2). The patient was treated with a course of piperacillin-tazobactam and vancomycinfor seven days. Cultures eventually returned positive for Streptococcus viridans and the patient recovered uneventfully.
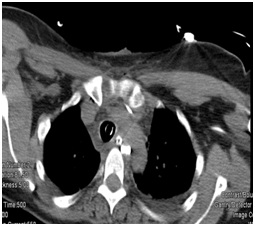 Figure 2: CT scan showing a 10mm Jackson Pratt drain secured in the posterior mediastinum.
Figure 2: CT scan showing a 10mm Jackson Pratt drain secured in the posterior mediastinum.DISCUSSION
Posterior cervical perforations are most common because of the thin posterior wall of the esophagus. Dissection of the retroesophageal space allows for bacterial spread through the mediastinum [5].
In a ten-year, multi-center study evaluating patients presenting to trauma centers with penetrating esophageal injuries, Asensio et al., found that of the 405 patients enrolled, the majority were male (88%) with an average age of 29. Furthermore, on presentation, 24% of patients were hypotensive with a systolic blood pressure less than 90 mmHg, 19% had subcutaneous emphysema and 7% had dysphagia [6]. Most patients presented with very minimal or no symptoms. This study also found the injuries were primarily to the cervical esophagus (56%) and that complications associated with esophageal injuries with or without surgical intervention were not uncommon. Of the 41% of patients in the study that developed complications, a majority were either abscess, mediastinitis or empyema [6]. Although uncommon, some patients developed esophageal leaks or tracheoesophageal fistulas. Timing of intervention appeared to be directly related to morbidity and mortality [6]. Early diagnosis and management are necessary to avoid these potential complications.
The diagnosis can be made using many different modalities. According to the Western Trauma Association’s esophageal perforation guidelines, stable patients who have sustained a penetrating injury with a suspected trans-mediastinal trajectory should have a CT scan performed first rather than esophagography [7]. Esophagography using a water-soluble contrast can diagnose small esophageal perforations, however is underutilized because CT scanning can demonstrate air in the soft tissues of the mediastinum indicating perforation and can most times be performed more expediently [1].
Currently there have been many treatment options discussed in current literature, including both operative and non-operative modalities. Operative management includes primary closure, resection, T-tube drainage, exclusion and diversion, and intraluminal stenting [8]. All of these modalities require an incision in the lateral neck or through a thoracotomy.
Non-operative management includes the use of antibiotics, but still runs a high risk of pneumothorax, pneumomediastinum, septic shock and respiratory failure. Other minimally invasive modalities for treatment include percutaneous drainage via CT guided drain placement, but this technique has proved to be very difficult due to the surrounding anatomy.
CONCLUSION
If this can be accomplished without a major operative intervention the patient’s recovery and overall management should be greatly improved.
REFERENCES
- Jones WG 2nd, Ginsberg RJ (1992) Esophageal perforation: a continuing challenge. Ann Thorac Surg 53: 534-543.
- Inoue Y, Gika M, Nozawa K, Ikeda Y, Takanami I (2005) Optimum drainage method in descending necrotizing mediastinitis. Interact Cardiovasc Thorac Surg 4: 189-192.
- Corsten MJ, Shamji FM, Odell PF, Frederico JA, Laframboise GG, et al. (1997) Optimal treatment of descending necrotizing mediastinitis. Thorax 52: 702-708.
- Pearse HE (1938) Mediastinitis following cervical suppuration. Ann Surg 108: 588-611.
- Wheatley MJ, Stirling MC, Kirsh MM, Gago O, Orringer MB (1990) Descending necrotizing mediastinitis: transcervical drainage is not enough. Ann Thorac Surg 49: 780-784.
- Asensio JA, Chahwan S, Forno W, MacKersie R, Wall M, et al. (2001) Penetrating esophageal injuries: multicenter study of the American Association for the Surgery of Trauma. J Trauma 50: 289-296.
- Biffl WL, Moore EE, Feliciano DV, Albrecht RA, Croce M, et al. (2015) Western Trauma Association Critical Decisions in Trauma: Diagnosis and management of esophageal injuries. J Trauma Acute Care Surg 79: 1089-1095.
- Urschel HC Jr, Razzuk MA, Wood RE, Galbraith N, Pockey M, et al. (1974) Improved management of esophageal perforation: exclusion and diversion in continuity. Ann Surg179: 587-590.
Citation: Lopez MA, Buicko JL, Lopez-Viego MA (2019) Treatment of Acute Mediastinitis Secondary Traumatic Esophageal Perforation by Naso-Mediastinal Drainage. Archiv Surg S Educ 1: 004.
Copyright: © 2019 Michael A Lopez, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

