
Unilateral Parotitis in Neonatal and Young Children
*Corresponding Author(s):
Sofia Brandão MirandaPediatrics Department, Hospital De Braga, Braga, Portugal
Email:asofiabmiranda@gmail.com
Ana Ribeiro
Intensive Neonatal Care Unit, Hospital De Braga, Braga, Portugal
Email:anabarrosribeiro@gmail.com
Abstract
Introduction
Bacterial parotitis is a rare condition in newborns, typically occurring between the 7th and 14th days of life. The exact cause is not fully understood, but it has been linked to several risk factors such as prematurity, dehydration, low birth weight, orogastric tube feeding, immunodeficiency, oral trauma, ductal obstruction, and structural changes in the parotid gland. The diagnosis is based on clinical signs and symptoms and Staphylococcus Aureus is the most common cause, but other agents have also been identified. The prognosis is generally good with early diagnosis and appropriate treatment, although there is a risk of recurrence.
Case Reports
We present two cases of bacterial parotitis with different approaches. The first case is a 2-month-old female infant who developed a fever, swelling in the left angle of the jaw, and inflammatory signs 10 days after being born. The second case is a 13-day-old male newborn who was admitted to the Emergency Department with swelling and pain on the left side of his face. Both cases were diagnosed with bacterial parotitis, with the first case caused by Staphylococcus aureus, and the second case caused by Streptococcus pneumonia. Treatment in both cases involved intravenous antibiotics and surgical drainage may be necessary in cases where the infection is resistant to medical treatment or has caused complications such as abscesses. The infants were discharged after 6 days and 2 weeks respectively with no recurrences or complications.
Conclusion
Bacterial parotitis is a rare but potentially serious condition in newborns that should be considered in the differential diagnosis of infants with facial swelling. Early diagnosis and appropriate treatment can lead to good outcomes, but there is a risk of recurrence.
Keywords
Breast feeding; Lymph nodes; Saliva drainage; Trauma
Introduction
Bacterial parotitis is a rare condition in newborns and its incidence has been decreasing in recent years, with an estimated incidence of 13.8 cases per 10,000 admissions in newborns. It is more common in males and typically occurs between the 7th and 14th days of life. The exact cause of this condition is not fully understood, but it has been linked to several risk factors such as prematurity, dehydration, low birth weight, orogastric tube feeding, immunodeficiency, oral trauma, ductal obstruction, and structural changes in the parotid gland. The diagnosis is based on clinical signs and symptoms and Staphylococcus Aureus is the most common cause, but other agents have also been identified. Treatment typically involves intravenous antibiotics and surgical drainage may be necessary in cases where the infection is resistant to medical treatment or has caused complications such as abscesses. The prognosis is generally good with early diagnosis and appropriate treatment, although there is a risk of recurrence. We present two cases of bacterial parotitis with different approaches.
Cases Report 1
A 2-month-old female infant of Caucasian ethnicity with no history of consanguinity was born via a dystocic delivery with vacuum extraction at 40 weeks and 3 days. She had an Apgar score of 8/10/10 and required oxygen at birth. Fetal serologies and ultrasounds were normal. The results for Group B Streptococcus were negative in vaginal and rectal exudate oh her mother. The infant was considered at risk for infection due to the presence of maternal fever during labor and meconium in the amniotic fluid. She was discharged from the maternity ward 48 hours after birth while exclusively breastfeeding.
Ten days after birth, the infant was evaluated due to a 10% weight loss and feeding difficulties. Formula was introduced, resulting in good weight gain. Three months later, the infant developed a fever, swelling in the left angle of the jaw, and inflammatory signs. Examination of the parotid region revealed erythema, edema, and purulent drainage from the Sténon canal in the oropharynx (Figure 1). Ultrasonography revealed an increase in the volume of the left parotid gland with globally heterogeneous echostructure and wavy contours, consistent with probable parotitis. Laboratory analysis showed no leukocytosis, and C-reactive protein was 27.7 mg/L (reference range (RR) : < 20mg/L). Procalcitonin was 0.08 ng/ml (RR: < 2mg/mL) and renal function and ionogram were normal.
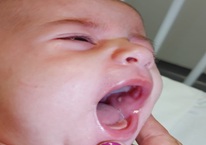 Figure 1: Purulent drainage from the Sténon canal.
Figure 1: Purulent drainage from the Sténon canal.
Blood culture and culture of the drained exudate were performed, and the infant was hospitalized for empirical intravenous antibiotic therapy with flucloxacillin (150 mg/kg/dose) administered every 8 hours, and cefotaxime (150 mg/kg/dose) administered every 8 hours. The blood culture was negative, and Staphylococcus aureus (SA) was isolated from the purulent exudate. The organism was sensitive to amoxicillin, oxacillin, and penicillin, and had intermediate sensitivity to levofloxacin, establishing the definitive diagnosis of bacterial parotitis. After three days, cefotaxime was discontinued and treatment with intravenous flucloxacillin was continued with a favorable clinical response. The infant was discharged on the sixth day of hospitalization with oral flucloxacillin (147 mg/kg/day) for 10 days. Three weeks later, an ultrasonography was performed, which showed slight heterogeneity on the left side with several intraparotid lymph nodes. After 1 year, the child has remained without any complications or recurrences.
Case Report 2
A 13-day-old male, Caucasian newborn with a normal prenatal history, no infectious risk, and a negative Streptococcus group B test at 36 weeks of pregnancy was admitted to the Emergency Department with swelling and pain on the left side of his face. These symptoms had started six hours prior to admission, and he did not have a fever or irritability. The newborn was breastfeeding with good weight gain. On examination, the newborn was uncomfortable and had a red, hot, and painful swelling on the left side of his face with purulent drainage from the Sténon canal. Blood analysis revealed a high white blood cell count, neutrophilia (25,000/uL, reference range: 5-20.2x10^9), and an elevated C-reactive protein level (5.8mg/L, reference range: <20mg/L). An ultrasound showed swelling of the left parotid gland, with slightly heterogeneous echostructure, and increased echogenicity of the periparotid subcutaneous tissue, findings consistent with parotitis. A blood culture and culture of the exudate were performed, and the newborn was hospitalized in the Neonatal Intensive Care Unit.
An empirical antibiotic therapy consisting of ampicillin at a dosage of 50 mg/kg/dose and cefotaxime at a dosage of 150 mg/kg/day administered every 8 hours was initiated. After two days, the newborn's condition deteriorated with the onset of fever and increased swelling of the face. Blood analysis revealed an increase in PCR to 89.8 mg/L. An immunological study was conducted, which revealed normal immunoglobulins and complement levels, and a negative HIV serology. The blood culture and exudate examination revealed the presence of Staphylococcus aureus (SA), which was resistant to amoxicillin. The antibiotic therapy was changed to flucloxacillin at a dosage of 200 mg/kg/day administered every 6 hours, while maintaining cefotaxime, resulting in clinical improvement. The newborn was discharged on the eighth day of hospitalization in good general condition, without fever or swelling. The patient was advised to continue breastfeeding exclusively and to continue taking flucloxacillin for 14 days as a precaution.
Discussion
Bacterial acute parotitis is a rare infectious pathology among newborns, with only a limited number of cases described in the literature. However, it should be considered in the differential diagnosis of facial swelling, particularly in the presence of risk factors, as early diagnosis and treatment are crucial in preventing complications. The parotid gland is the most commonly infected salivary gland due to the lack of bacteriostatic properties in the mucoid component of serous secretions. The infection is typically unilateral and is acquired through the oral cavity via the Sténon canal or by the hematogenous route, often in association with or preceded by sepsis. Contaminated maternal milk or formula milk can also contribute to the transmission of the infection via the ascending route. As reported in the literature, both cases presented here were unilateral. Several factors that predispose to its development have been identified, such as male sex with a ratio of 3:1, prematurity, and low birth weight.
Dehydration, including subclinical forms, plays a significant role in the pathogenesis of bacterial acute parotitis by increasing the viscosity of saliva and causing obstruction of the flow in the ducts. Prolonged feeding with an orogastric tube can decrease saliva drainage, resulting in functional ductal obstruction and local inflammation. Other potential risk factors for infection include the presence of lesions in the oral cavity, structural anomalies of the gland, and decreased salivary flow, which allows for the retrograde migration of bacteria. Staphylococcus aureus (SA) is the most commonly identified etiological agent in all age groups, including nosocomial infections. Other less common agents include 22% gram-positive cocci (Streptococcus pyogenes, Streptococcus viridans, Streptococcus pneumoniae), 16% gram-negative bacilli (Escherichia coli, Pseudomona aeruginosa, Klebsiella pneumoniae, Haemophilus influenzae), and 4% anaerobes (Bacteroides melaninogenicus and/or disiens, Fusobacterium nucleatum, Veillonella alkalescens, Peptostreptococcus spp., Prevotella spp.).
S. agalactiae is a rare cause of bacterial acute parotitis, with only a limited number of cases described in the literature, most of which occur in the context of late sepsis. In cases of parotitis, the main route of infection for SA is ascending through the Sténon canal after oral cavity colonization. This can explain the frequent occurrence of purulent drainage through the duct in cases of staphylococcal parotitis, as observed in the cases presented here [1-8]. In the first clinical report, no risk factors were identified for its occurrence. Bacteraemia with a focus on the parotid gland or a primary infection of this gland with subsequent hematogenic dissemination are suspected options. In the second clinical report, the only identified risk factor was male gender.
The diagnosis of bacterial acute parotitis is primarily based on clinical observation, specifically the presence of parotid swelling accompanied by inflammatory signs. This may be accompanied by systemic symptoms such as fever (occurring in approximately one-third of cases), irritability, refusal to eat, and clinical signs of sepsis. The discharge of purulent content through the duct is a pathognomonic sign of this pathology [1,2,4,5]. Analytically, leukocytosis with neutrophilia and an increase in acute phase reactants such as PCR and amylase may be present, although these laboratory tests are non-specific and may be normal [2,4,5].
To confirm the diagnosis and guide therapy, it is essential to collect exudate and blood cultures to identify the etiological agent [4]. Purulent exudate can be obtained through drainage of the duct, which is less invasive and less specific, or by direct needle aspiration of the parotid gland, which is more specific and avoids contamination by oral cavity flora [2,4]. In some cases, aseptic parotitis may be found [6]. In our first case, there was no leukocytosis, but an increased PCR. The second case presented with leukocytosis and neutrophilia, as well as an increased PCR and amylase [2]. Treatment consists of antibiotics and drainage of the purulent content [2,4,7]. In severe cases, hospitalization may be required [4]. The first case was treated with amoxicillin-clavulanate, and the second case was treated with clindamycin. Both cases showed improvement of clinical condition after treatment [2].
The initial empiric treatment for acute bacterial parotitis consists of intravenous broad-spectrum antibiotic therapy with coverage for the most frequently implicated agents, namely Streptococcus aureus, for example, a combination of a penicillin resistant to penicillinases and an aminoglycoside or third-generation cephalosporin. The treatment is modified according to the antibiogram [1,2,4,5,7]. An increase in methicillin-resistant SA may require the use of vancomycin; in the presence of an anaerobe, treatment may include a combination of metronidazole with a macrolide, or a penicillin associated with a β-lactamase inhibitor such as clavulanate. In addition to antimicrobial treatment, proper hydration and analgesia must also be provided [1,4,8].
In our first case, initial empirical therapy with flucloxacillin and cefotaxime was administered to cover the most prevalent agents of neonatal parotitis, including SA and gram-negative bacteria. Following the results of the cultures, directed antibiotic therapy was implemented targeting the specific agent. In the second case, initial treatment with ampicillin and cefotaxime aimed to cover gram-negative bacteria. However, due to clinical and analytical deterioration, the antibiotic therapy was optimized by expanding coverage to include gram-positive SA. Since the implicated agent was already known, cefotaxime was discontinued, and flucloxacillin monotherapy was maintained. Surgical drainage of the gland is rarely necessary, as supported by literature [2,4,5].
Although not consensual, it was decided to maintain treatment for 10 days in the two case reports, as most authors advise treatment for 7-10 days or until 3 to 5 days after the disappearance of swelling [1,7]. The early institution of targeted antibiotic therapy, as well as advances in antimicrobial therapy, have improved the prognosis of neonatal parotitis, making complications such as facial nerve paralysis, salivary fistula, extension of infection to the external auditory canal, sepsis and meningitis rare [1,4,5,6]. In most cases, there is an improvement within the first 24-48 hours of antimicrobial treatment, with a reduction in parotid swelling [4]. The prognosis for this pathology is favorable in most cases, without recurrence. If clinical improvement does not occur within the first few days, imaging should be repeated to exclude abscesses or complications [1,2,4].
Conclusion
Acute bacterial parotitis is a rare condition in newborns and infants and its initial symptoms are not specific. However, early diagnosis is crucial. Therefore, it should be considered when a child exhibits irritability with swelling of the parotid gland. Early diagnosis and appropriate antibiotic treatment can prevent acute suppurative parotitis and its complications.
References
- Pereira C, Prior AR, Abrantes M, de Azevedo AS (2017) Bilateral bacterial parotitis in a newborn: A case report. Nascer E Crescer: Birth and Growth Medical Journal 5: 3-6.
- Oliveira MJ, Guedes M, Costa FM, Almeida R (2007) Neonatal parotitis caused by Streptococcus group B: A case report. Nascer E Crescer: Revista Do Hospital De Crianças Maria Pia XVI 233-234.
- Özdemir H, Karbuz A, Ciftçi E, Fitöz S, Ince E, et al. (2011) A cute neonatal suppurative parotitis: A case report and review of the literature. International Journal of Infectious Diseases 15: e500-e502.
- Costa L, Leal LM, Vales F, Santos M (2016) Acute parotitis in a newborn: A case report and review of the literature. The Egyptian Journal Of Otolaryngology 32: 236-239.
- Soltani M, Javid A (2019) A cute bacterial parotitis in early infancy: A case report and review of the literature. Iranian Red Crescent Medical Journal 21: e91903.
- Curiela JA, Río GD, Val PD, Conde AAA, Lavín AC (2004) Parotiditis aguda supurativa neonatal. Anales de Pediatría 60: 274-277.
- Nso Roca AP, Baquero-Artigao F, García-Miguel MJ, del Castillo Martín F (2007) Parotiditis aguda neonatal por Streptococcus agalactiae. Anales de Pediatría 67: 65-67.
- Decembrino L, Ruffinazzi G, Russo F, Stronati M (2012) Monolateral suppurative parotitis in a neonate and review of literature. International Journal of Pediatric Otorhinolaryngology 76: 930-933
Citation: Miranda SB, Ribeiro A, Nogueira MV, Macedo J, Silva A (2023) Unilateral Parotitis in Neonatal and Young Children. J Med Stud Res 5: 022.
Copyright: © 2023 Sofia Brandão Miranda, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

