
Journal of Clinical Dermatology & Therapy Category: Clinical
Type: Case Study
Video Dermatoscopy in Lymphedema An Additional Tool
*Corresponding Author(s):
Ravi Kumar ChittoriaDepartment Of Plastic Surgery, Jawaharlal Institute Of Postgraduate Medical Education And Research (JIPMER), Pondicherry, India
Tel:+91 9442285670,
Email:drchittoria@yahoo.com
Received Date: Oct 29, 2019
Accepted Date: Nov 11, 2019
Published Date: Nov 18, 2019
Abstract
Lymphedema is a major cause of morbidity which is associated with physical, psychological and social burdens. The affected limb has skin changes that range from pitting edema to fissures which are associated with infection. We would like to present our experience with the use of videodermatoscopy to identify the various skin changes at a magnification which might help us to prevent and treat infections more effectively.
Keywords
Dermatoscopy; Lymphedema; Videodermatoscopy
INTRODUCTION
Videodermatoscopy (VD) is a non-invasive technique in whichskin is observed in vivo by a video camera equipped with lenses that allow magnifications ranging from 4x to 1000x. The images obtained are visualized on a high definition monitor and may be stored on a personal computer, in order to identify and compare changes over time [1].
Lymphedema (primary & secondary) is associated with various secondary skin changes ranging from reversible pitting edema to mossy foot. These skin changes are classified by WHO into 7 stages [2].
According to the Fifth WHO Expert Committee on Filariasis, lymphoedema can be classified as follows:
Stage 1: The feature of stage 1 lymphoedema is:
The main difference between stage 2 lymphoedema and stage 1 is that the swelling does not disappear without lymphoedema management.
Stage 3: Swelling is not reversible overnight.The principal feature of stage 3 lymphoedema is the presence of one or more shallow skin folds
Stage 4: Swelling is not reversible overnight.
The main feature of stage 4 lymphoedema is the presence of knobs lumps, lumps, or protrusions on the skin
Stage 5: Swelling is not reversible overnight.
The presence of one or more deep skin folds is the main feature of stage 5 lymphoedema
Stage 6: Swelling is not reversible overnight. On the surface of the foot (especially the toes), very small elongated or rounded small knobs can be clustered together, giving rise to the peculiar appearance of “mossy foot”
Patients with stage 6 lymphoedema) have acute attacks. Almost all these patients have entry lesions between the toes and bad odour. Wounds in the skin are frequently present.
Stage 7: The features of stage 7 lymphoedema are:
Emphasis on management of lymphedema is in the treatment and prevention of infection of the limb, the main source of which is the fissures in the skin through which ascending lymphangitis is noticed.
Even though most of the skin changes are visible through the naked eye, videodermatoscopy may help for accurate assessment of the skin changes and possible sites of future infection may be identified earlier due to higher magnification, thus leading to better management of the patient.
Lymphedema (primary & secondary) is associated with various secondary skin changes ranging from reversible pitting edema to mossy foot. These skin changes are classified by WHO into 7 stages [2].
According to the Fifth WHO Expert Committee on Filariasis, lymphoedema can be classified as follows:
- Grade I lymphoedema: mostly pitting edema; spontaneously reversible on elevation
- Grade II lymphoedema: mostly non-pitting edema; not spontaneously reversible on elevation
- Grade III lymphoedema (elephantiasis): a gross increase in volume in a grade II lymphoedema, with dermatosclerosis and papillomatous lesions
Stage 1: The feature of stage 1 lymphoedema is:
- Swelling is reversible overnight
- In stage 1 lymphoedema, the swelling increases during the day and disappears overnight
The main difference between stage 2 lymphoedema and stage 1 is that the swelling does not disappear without lymphoedema management.
Stage 3: Swelling is not reversible overnight.The principal feature of stage 3 lymphoedema is the presence of one or more shallow skin folds
Stage 4: Swelling is not reversible overnight.
The main feature of stage 4 lymphoedema is the presence of knobs lumps, lumps, or protrusions on the skin
Stage 5: Swelling is not reversible overnight.
The presence of one or more deep skin folds is the main feature of stage 5 lymphoedema
Stage 6: Swelling is not reversible overnight. On the surface of the foot (especially the toes), very small elongated or rounded small knobs can be clustered together, giving rise to the peculiar appearance of “mossy foot”
Patients with stage 6 lymphoedema) have acute attacks. Almost all these patients have entry lesions between the toes and bad odour. Wounds in the skin are frequently present.
Stage 7: The features of stage 7 lymphoedema are:
- Swelling is not reversible overnight. The patient is unable to adequately or independently perform routine daily activities such as walking, bathing, cooking, etc.
Emphasis on management of lymphedema is in the treatment and prevention of infection of the limb, the main source of which is the fissures in the skin through which ascending lymphangitis is noticed.
Even though most of the skin changes are visible through the naked eye, videodermatoscopy may help for accurate assessment of the skin changes and possible sites of future infection may be identified earlier due to higher magnification, thus leading to better management of the patient.
MATERIALS AND METHODS
This is a case report of a 29 year female patient admitted in plastic surgery department in the month of August 2019, with h/o swelling of the left lower limb since 16 years. On assessment and thorough evaluation, the patient was diagnosed with chronic primary lymphedema of left lower limb with secondary grade 7 skin changes (WHO grading) with multiple fissures over the affected limb (Figure 1). She also had foul-smelling serous discharge from the limb.
 Figure 1: Left lower limb lymphedema.
Figure 1: Left lower limb lymphedema.Videodermatoscopy was done using Aram Huvis® videodermatoscope with 1x, 60x (Figure 2), 200x (Figure 3), 1000x (Figure 4) with Skin XP Pro software system.
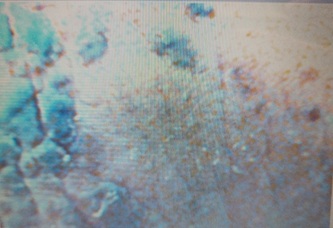 Figure 2: 60x magnification showing scales with pigmented skin.
Figure 2: 60x magnification showing scales with pigmented skin. Figure 3: 200x magnification with fissures and scales and pigmentation.
Figure 3: 200x magnification with fissures and scales and pigmentation. Figure 4: 1000x magnification showing deep fissures with dry scaly skin.
Figure 4: 1000x magnification showing deep fissures with dry scaly skin.RESULT
In our case, we have done serial videodermatoscopy. The changes noted included deep fissures in some areas with scaling of the skin. Large scabs over various areas. We noticed that our patient had dryness of the skin which was managed. Improvement was noticed by the healing of the fissures over the skin and was recorded using the videodermatoscope.
DISCUSSION
Videodermatoscopy is an evolved version of dermatoscopy. It is performed by a video camera equipped with opticfibers and lenses that allow magnifications rangingfrom 4x to 1000x. The images are visualizedon a monitor and stored using a specific software ona personal computer.This helps to identify and compare changes over time [3].Videodermatoscopy has great potential in differentiating various dermatological conditions and in the differential diagnosis of pigmented skin lesions, including some inflammatory diseases, cutaneous parasitoses like scabies, hair and nail abnormalities, various vascular lesions. In several disorders, it may be useful in differential diagnosis, prognostic evaluation, and in evaluating the response to treatment [3].
In lymphedema, the videodermatoscope not only helps in recording the progress of the skin changes with serial images, it also helps in identifying potential sites of entry of infection by accurately identifying the deep fissures [4], areas of dryness, or fungal infection which can then be treated appropriately. Also, it is valuable in identifying a possible source of infection which will help in preventing serious infections and the vicious cycle of skin thickening and more fissures leading to repeated infections.
It also helps in identifying and diagnosing the dreaded complication of lymphedema i.e., lymphangiosarcoma [5].
In lymphedema, the videodermatoscope not only helps in recording the progress of the skin changes with serial images, it also helps in identifying potential sites of entry of infection by accurately identifying the deep fissures [4], areas of dryness, or fungal infection which can then be treated appropriately. Also, it is valuable in identifying a possible source of infection which will help in preventing serious infections and the vicious cycle of skin thickening and more fissures leading to repeated infections.
It also helps in identifying and diagnosing the dreaded complication of lymphedema i.e., lymphangiosarcoma [5].
CONCLUSION
Our experience with videodermatoscope in lymphedema has shown that it can be used in the armamentarium of the investigation modalities to record and follow-up the skin changes during the course of the disease. Further regular evaluation may also lead to a classification system for skin changes may be formulated. However larger studies are required to emphasize the use of videodermatoscopy in all cases of lymphedema during evaluation.
REFERENCES
- Micali G, Lacarrubba F (2003) Possible applications of videodermatoscopy beyond pigmented lesions. International journal of dermatology. 42: 430-433.
- Dreyer G, Addiss D, Bettinger J, Dreyer P, Norões J, wt al. (2001) Lymphoedema staff manual: treatment and prevention of problems associated with lymphatic filariasis. In Lymphoedema staff manual: treatment and prevention of problems associated with lymphatic filariasis, WHO, Geneva, Switzerland.
- Micali G, Lacarrubba F (2010) Dermatoscopy in clinical practice: Beyond pigmented lesions. CRC Press, Florida, USA.
- Le Fourn E, Duhard E, Tauveron V, Maruani A, Samimi M, et al. (2011) Changes in the nail unit in patients with secondary lymphoedema identified using clinical, dermoscopic and ultrasound examination. Br J Dermatol 164: 765-770.
- Kelati A, Debagh F, Mernissi FZ (2018) Dermoscopy in a lymphangiosarcoma of Stewart–Treves syndrome. Breast Cancer Management 7: 12.
Citation: Reddy CL, Chittoria RK, Aggarwal A, Gupta S, Mohan PLBM (2019) Video dermatoscopy in Lymphedema - An Additional Tool. J Clin Dermatol Ther 5: 040.
Copyright: © 2019 Chirra Likhitha Reddy, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

Journal Highlights
© 2026, Copyrights Herald Scholarly Open Access. All Rights Reserved!
