
Vitiligo Development after COVID-19 Vaccination
*Corresponding Author(s):
Ashley A BarrasDepartment Of Internal Medicine, Section Of Dermatology, Louisiana State University Health Shreveport, United States
Email:aab001@lsuhs.edu
In this study, we present a 64-year-old African American woman with hypopigmented macular areas on her face, hands, and trunk. The lesions first appeared on her hands in early summer of 2021, three months after receiving the first dose of the Moderna COVID-19 vaccine, eventually spreading to her face, abdomen, and back. The patient has a history of Systemic Erythematous Lupus (SLE), currently on Plaquenil, with autoimmune testing positive for ANA and anti-SSB. She reported no personal or family history of vitiligo. She was first examined by Rheumatology and was prescribed a trial of CellCept but discontinued using it due to blistering on her face. She was then referred to a Dermatology clinic. On examination, there were depigmented white macules and patches consistent with vitiligo. The diagnosis was confirmed upon dermatological and woods lamp examination. She was prescribed a topical calcineurin inhibitor and was instructed to return to the clinic for follow-up.
Vitiligo has a complex autoimmune etiology, which stems from melanocyte loss or dysfunction. Studies have shown the importance of a specific neoantigen of melanocytes, HSP70i, which is a heat shock protein eventually presented to T lymphocytes, causing the destruction of melanocytes. Overexpression of this neoantigen leads to more dendritic cell activation and lymphocyte infiltration into depigmented areas [5,6].
Multiple mechanisms have been presented to address the reasoning behind autoimmune phenomena linked with COVID-19. The most accepted theory is one consisting of molecular mimicry occurring between the antigenic epitopes of the virus and heat shock proteins7. While this is a promising hypothesis because these proteins have been associated with several other autoimmune diseases triggered by COVID-19 infections, there is still room for questioning on the exact mechanism because IgG antibodies generated against SARS-CoV-2 have not been shown to recognize and react to these specific proteins. One other hypothesis of note is that COVID-19 infections may stimulate significant IFN-I production from dendritic cells, which is a key pathogenic mechanism of vitiligo [7].
At baseline, other autoimmune diseases are more likely to develop in patients with a history of autoimmune disease, such as our patient with SLE [8]. However, it is also important to note that vaccines can trigger autoimmune diseases in patients with genetic predispositions to these diseases as well. For example, autoimmune diseases such as immune thrombocytopenic purpura, systemic lupus erythematosus, and multiple sclerosis have already been linked to various vaccines such as influenza, hepatitis B, and the MMR vaccines [8]. As it is not clear if the vitiligo presented in this case was caused by vaccination, genetic predisposition, or a combination of both, the temporal relation of the development is of note. Further studies are needed to determine a causal relationship between the COVID-19 vaccination, vitiligo, and autoimmune predisposition (Figure 1).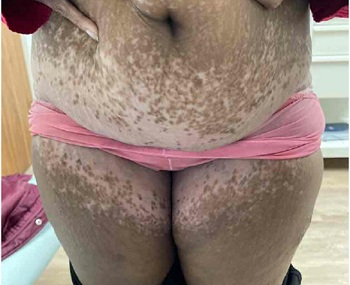
Figure 1: Depigmented areas on lower abdomen and upper thighs.
Consent
The patient provided written informed consent for use of images and publication of their case details. Data sharing not applicable to this article as no datasets were generated or analyzed during the current study.
References
- McMahon DE, Amerson E, Rosenbach M, Lipoff JB, Moustafa D, et al. (2021) “Cutaneous Reactions Reported after Moderna and Pfizer COVID-19 Vaccination: A Registry-Based Study of 414 Cases. J Am Acad Dermatol 85: 46-55.
- Ciccarese G, Drago F, Boldrin S, Pattaro M, Parodi A Sudden Onset of Vitiligo after COVID-19 Vaccine. Dermatol Ther 35: 15196.
- Kaminetsky J, Rudikoff D (2021) New?onset Vitiligo Following MRNA?1273 (Moderna) COVID?19 Vaccination. Clin Case Rep 9: 04865.
- Okan G, Vural P (2022) Worsening of the Vitiligo Following the Second Dose of the BNT162B2 mRNA COVID?19 Vaccine. Dermatol Ther 35: 15280.
- Mosenson JA, Eby JM, Hernandez C, Le Poole IC (2013) A Central Role for Inducible Heat-Shock Protein 70 in Autoimmune Vitiligo. Experimental Dermatology 22: 566-569.
- Mosenson JA, Zloza A, Klarquist J, Barfuss AJ, Guevara-Patino JA, et al. (2012) HSP70i is a critical component of the immune response leading to vitiligo. Pigment Cell Melanoma Res 25: 88-98.
- Riquelme IL, Ballesteros MDF, Ordoñez AS, Díaz DJG (2022) COVID ?19 and Autoimmune Phenomena: Vitiligo after Astrazeneca Vaccine. Dermatol Ther 35: 15502.
- Vadalà M, Poddighe M, Laurino C, Palmieri B (2017) Vaccination and Autoimmune Diseases: Is Prevention of Adverse Health Effects on the Horizon? EPMA J 8: 295-311.
Citation: Barras AA, Dautel AD, Haas C (2022) Vitiligo Development after COVID-19 Vaccination. J Clin Dermatol Ther 8: 0107.
Copyright: © 2022 Ashley A Barras, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

