Introduction
Advances in clinical as well as psychosocial management of patients with HIV/AIDS have dramatically changed since the early stages of the pandemic, where treatment strategies did not appear to have had a positive influence on patients’ lives. The field of HIV/AIDS has advanced to such an extent that it has become acceptable and expected to focus energies on the quality of life issues surrounding HIV/AIDS and its treatments, rather than the sole focus on saving and sustaining life. It is within this context that research into sensory disabilities associated with HIV/AIDS is receiving more attention by academics as well as the medical fraternity. Within the head and neck, audiological manifestations including hearing loss and vestibular symptoms require attention to achieve clearer categorization of the symptomatology as well as sequellae of treatment options. Hence, the current researcher’s support of Friedman and Noffsinger’s [1] belief that as primary professionals in hearing health care, audiologists have a duty to inform not only themselves; but also other relevant health-care professionals about this issue, hence the current study.
Due to the fact that patients with HIV/AIDS are living longer because of the positive effects of HAART, it has become crucial that effects of HIV/AIDS and its treatments on the auditory system are better understood. It is well understood that the face of the HIV/AIDS pandemic has and continues to change internationally due to the discovery of antiretroviral drugs [2]. These advancements in treatment have also led to improvements in the medical field with people who have HIV/AIDS surviving for extended periods of time experiencing toxic-related morbidity that has influences on quality of life indicators [2]. There has always been a concern, nonetheless, that HIV-associated auditory disorders may be well under-reported; and this is thought to have possibly been due to the fact that even though hearing loss and dizziness are often the initial symptoms of underlying auditory system disease, these may not have been reported by patients prior to HAART because many patients focused on the life-threatening complications of the HIV disease rather than on quality of life issues [3]. In South Africa, where roll-out of HAART only occurred as recently as 2004, and where currently universal HAART coverage has still not been achieved, this under-reporting of auditory symptoms may still be highly prevalent. It is likely that reporting of quality of life complications will only be evidenced once universal coverage is attained for the population infected.
According to the research literature, auditory abnormalities associated with HIV/AIDS and its treatments have been reported in persons with varying degrees of HIV infection, as well as in treatment naïve as well as patients on antiretroviral treatment [4-8]. Causes of these abnormalities can be direct [4-7] as well as indirect [6-8]; although this distinction is not always clear and consistent. The direct or primary effects are reportedly due to the fact that the virus is neurotropic in nature and commonly manifests itself neurologically [4-7]. The indirect and/or iatrogenic causes are linked to opportunistic infections which require suppressive therapy, thereby leading to ototoxicity [6-8]. This evidence is based on numerous clinical, and mostly medically oriented studies that have demonstrated the occurrence of hearing loss and other auditory manifestations in HIV/AIDS. This evidence demonstrates that auditory manifestations may be one of the challenges that the population will have to deal with; therefore over and above management of the known side effects of ARVs, research into the identification and monitoring of all other manifestations of the disease is required. It is important to state that a majority of these findings are mainly from developed countries where the presentation and management of HIV/AIDS varies to that in developing countries, suggesting a need for more research into this area particularly since the numbers of adults living with HIV/AIDS in developing countries such as South Africa continues to remain high, and also because the context is different. With regard to auditory manifestations, both identification and monitoring of ototoxicity require rigorous research to enhance the patients’ quality of life, particularly since internationally; a link has been established between ARVs and ototoxicity [6-10].
Due to the fact that opportunistic infections are common in HIV/AIDS, use of a drug regimen that often involves potentially ototoxic medications [9,10] is not unusual. This therefore increases the likelihood of ototoxicity in this population; with particular contribution of the use of experimental antiretroviral drugs with undocumented or unknown side effects [8]. In South Africa, ototoxic drugs that are often used in the treatment of tuberculosis as an opportunistic infection increase the potential for a drug-induced hearing loss in this population [10]. Although the side-effects of many antiretroviral drugs are yet to be determined, HIV-infected individuals are often prescribed medications as a prophylaxis or treatment of opportunistic infections that have been long associated with the development of audiological and vestibular changes [8,11-14]. Antineoplastic medications such as vincristine, antifungal agents including amphotericin B, flucytosine and ketoconazole, immune modulators, aminoglycoside antibiotics, erythromycin, and Azidothymidine (AZT) are all widely prescribed in the management of HIV and are all reported to be associated with significant ototoxicity [7,8,11-14]. These medications are associated with hearing loss, tinnitus and vertigo. Frequently administered medications for PCP (Pentamidine, TMP/SMX, Primaquine) may cause tinnitus, vertigo, dizziness, auditory disturbances, deafness, decreased hearing, hearing loss, and otalgia [8]. Moreover, the use of experimental medications with relatively unknown toxicity as well as the use of ototoxic drugs, such as anti-Tuberculosis (TB) medications, in combination adds to the overall effect on hearing [15].
As mentioned earlier, in South Africa, one of the most frequently administered treatments to the HIV/AIDS population is that of TB treatment, where TB cases have dramatically increased over the past decade [16,17]. This upsurge in TB cases seems to continue, largely due to co-infection with the HIV, and with the emergence of drug resistant TB [17]. This co-occurrence of HIV/AIDS and TB has important clinical implications for the audiologist with regard to the possible association between TB treatment [18,19] and HAART. This implication is even more pronounced where the TB and HIV infected patient also happens to be under chronic noise exposure; which can act synergistically to exacerbate auditory symptoms. The concern with TB treatment is because some of the drugs used in the treatment of TB fall under the umbrella term ‘aminoglycosides’, which are known to be ototoxic in nature. Examples of these aminoglycosides include amikacin, gentamicin, kanamycin, netimicin, paromomycin, streptomycin, tobramycin, and apramycin [19].
As far as HIV/AIDS treatment is concerned; the impact of medications on hearing function have been reported, although not extensively, with Nucleoside analogue Reverse Transcriptase Inhibitors (NRTIs). Although a variety of adverse effects have been attributed to NRTIs, only a small number of cases of ototoxicity have been reported in the literature; particularly from developing country contexts. Case studies [20] have been reported where ototoxicity has been noted; although with a number of confounding variables including advanced age, occupational noise exposure, and prior hearing loss. One should note that not all of the currently reviewed studies utilized sensitive ototoxicity monitoring protocols such as extended high-frequency audiometry and/or otoacoustic emissions. Furthermore, some of these studies also did not follow longitudinal research designs that could have allowed the researchers to investigate within-subject changes, but they rather followed cross sectional methodology designs. In addition, the reports that other factors such as age, drug interactions, concomitant noise exposure, and so on may have an influence on the ototoxicity of HAART should be taken into consideration when reviewing the effects of HAART on hearing. Several other international cases of ototoxicity have been reported in HIV-infected patients who had been treated with zalcitabine [21-23], didanosine [24], zidovudine [20], and combinations of zidovudine and didanosine [25], stavudine and lamivudine [15], stavudine, lamivudine, didanosine, and hydroxyurea [15], and post exposure prophylaxis with stavudine, lamivudine, and nevirapine [26]. Furthermore, a study of 99 HIV-infected individuals on HAART revealed that hearing loss was common in their sample. This hearing loss was mostly associated with being 35 or older and with a history of ear infection, and there was a trend toward an association with documented receipt of therapy with antiretroviral drugs in the preceding 6 months [27]. Moreover, previous cross-sectional studies and case reports have shown an association between hearing loss and NRTI therapy [15,27,28]. There have been two case reports of hearing loss in persons receiving HAART regimens that included NRTIs and a second class of antiretroviral drugs; one with a NNRTI (Nevirapine) and one with a Protease Inhibitor (PI) (lopinavir/ritonavir) each combined with NRTIs, (both these subjects were also receiving stavudine and lamivudine) [20,26,29].
As earlier mentioned, while ototoxic hearing loss has been described in HIV-infected people, there have been extremely limited prospective studies [30]. Hence there still needs to be extensive investigations to clearly establish and confirm this relationship. The study by Schouten et al., [30] investigated hearing changes longitudinally in treatment-naïve HIV-infected patients following initiation of regimens containing NRTIs; and the results revealed changes in hearing levels at all frequencies at 32 weeks following commencement of HAART. The changes were however not attributed to treatment with ZVD and ddI; even after taking into account noise exposure, immune status and age. The results of this prospective pilot study did not support the view that treatment with nucleoside antiretroviral drugs damages hearing. These results were consistent with the report from the Adult/Adolescent Spectrum of HIV Disease Project Group that demonstrated no association between hearing loss and drugs used in the treatment of HIV; but were contrary to findings from other cross-sectional studies and case reports that indicated ototoxicity to be common in this population [27,31,32].
Reviewed studies have several criticisms that can be levelled against them when it comes to their methodological designs. Firstly, most studies did not incorporate Otoacoustic Emissions (OAEs) as part of their monitoring battery, and this could have had a significant impact on their results since OAEs have been shown to be sensitive to cochlear damage in ototoxicity monitoring. Secondly, most included small sample sizes; mostly case reports, and small sample sizes significantly reduces the strength of the study in terms of the ability to generalize the findings. Additionally, small sample sizes limit the power of the studies in detecting a difference and also limit their ability to accurately interpret results. Thirdly, and understandably; there were no control groups. Finally, extended high-frequency audiometry did not form part of the test battery in most. Extended high-frequencies have been reported to be finely tuned to the effect of damaging environmental factors such as noise and ototoxic drugs [12].
It is for the aforementioned reasons that the current study was conceptualised. It was deemed important to conduct longitudinal studies in developing countries such as South Africa; although challenges are anticipated in such contexts. These challenges include firstly, the fact that the nature of the HIV/AIDS disease and the population being studied may preclude complete control over confounding variables; and secondly, securing decent sized comparison groups may be difficult, thereby preventing randomized matching of participants; and thirdly, extended high-frequency audiometry which does not form part of the routine audiological test battery may influence the type of results found; and this influence could reflect in clinical changes in the extended high-frequencies depicted on the audiogram being entirely missed. Lastly, the length of time for which the audiologic monitoring can occur due to attrition may be too short to allow for clinical hearing loss possibly caused by HAART to manifest and therefore be detected on the audiogram; because of the migrating nature of patients in the public health care sector. Nonetheless, such longitudinal studies of patients on various regimens of HAART need to be performed. These need to be conducted in order to determine if any hearing changes occur during the period when the patients are receiving HAART; hence the current study. It is also important that assessment measures such as DPOAEs and extended high frequency audiometry, which are sensitive to cochlear changes, form part of the methodologies employed [33]. The current study therefore aimed to monitor the auditory status in two groups of adults with AIDS receiving HAART–two different regimens (Group A: nevirapine, 3TC-lamivudine, and D4T-stavudine; and Group B: AZT-azidothymidine, 3TC, and Efavirenz) in hospital outpatient clinics in Johannesburg, Gauteng, South Africa. The anticipated significance of the study besides adding to the published evidence on ototoxicity from developing countries; was to aid in guiding audiological clinical management of patients with HIV/AIDS in order to enhance their quality of life.
Material and Methods
Research aims and objectives
Primary aim: To monitor the auditory status in two groups of adults with AIDS receiving two HAART regimens (Group A: nevirapine, 3TC-lamivudine, and D4T-stavudine; and Group B: AZT-azidothymidine, 3TC, and efavirenz) in a hospital outpatient clinic in Johannesburg, Gauteng.
Specific objective: To longitudinally assess hearing function in AIDS infected adults on HAARTThe null hypothesis was that the participants’ hearing function before and after antiretroviral drug-use would remain the same. The alternative hypothesis was that it would not remain the same, that is, participants would present with changes in their auditory function [34-36].
Design of the study: The design adopted in the current study was a repeated measures, quasi-experimental design with pre- and post-treatment testing [37]. The advantage of the chosen design was the fact that it is purported to be the best design where there are practical and ethical barriers to conducting randomized controlled trials [38]. The aim was to assess and monitor the hearing function before and during antiretroviral treatment-with measures taken before commencement of ARVs, and at every three months interval; with the last analysed measures taken at 15 months following initiation of treatment. The antiretroviral medications and other therapies were the independent variables, with the audiological measures (otoscopy, impedance audiometry, pure tone audiometry, otoacoustic emissions) being dependent variables.
Participants: A total sample of 41 in Group A (mean age=34.6yrs; median=33yrs) and 33 in Group B (mean age=33.6yrs; median=33yrs) participated in the current study. The patients selected for this study were recruited from the hospital’s Adult HIV/AIDS clinics. Patients attending these Johannesburg based clinics have already been diagnosed with HIV/AIDS and are seen there for general medical management as well as antiretroviral treatment and monitoring. At the time of the study all patients with CD4+ counts below 250 cells/mm3 had access to ARV treatment, at these clinics-and this is the group that was targeted for the current study. Because the sample was restricted to a part of the population that was readily available, a nonprobability convenience sampling technique was adopted [37,39].
For participant selection criteria; although the researcher strongly believed that having strict inclusion criteria would create an artificial environment; not authentically representative of the adult HIV population in the context of the study; the researcher still believed that it was crucial to have some degree of control over variables which are known to have potential confounding effects on the results of the study (e.g. advancing age, noise exposure, history of TB treatment, syphilis, and so forth) [37,39,40]. These participant inclusion and exclusion criteria that were adopted following baseline testing are depicted in Table 1.
Research Procedures and Materials
Collection materials and test procedures used in the current study, with the exception of the inclusion of extended high-frequency audiometry; are replicated from Khoza-Shangase [40]. All participants underwent case history interviews and medical record reviews, otoscopy and tympanometry, with conventional and extended high-frequency pure tone audiometry, as well as distortion product otoacoustic emission testing. Baseline data were collected from assessing participants’ dependant variables before administration of ARV therapy. Although data were collected at three monthly intervals, for ease of current research data management, hearing function was examined at baseline (before initiation of ARVs) and with repeated measures only at 3, 9 and 15 months into treatment. Only participants who attended all 4 sessions were included in the study; hence the exclusion of some of the test sessions for all participants.
Following infection control measures proposed by Kemp and Roeser [41], all testing was conducted in a sound-proof booth. Pure tone audiometry testing followed by Distortion Product Otoacoustic Emission (DPOAE) measurements for all participants was undertaken and systematically recorded.
Case history and otoscopy
A case history form that targeted the signs and symptoms of auditory manifestations was utilized in order to gather all the important case history information, audiological data and some medical variables that could have exerted an impact on the results of the study [40]. This was followed by an otoscopic examination where the researcher evaluated the participants’ ears for the presence of impacted wax; otitis externa; possible otitis media; perforated tympanic membranes; collapsed ear canals; presence of any growths and any other ear disorders [42].
Impedance audiometry
Through the use of the Inter-Acoustic AZ26 audiotympanometer, the researcher performed impedance audiometry in the form of tympanometry on all participants. This was aimed at assessing the status and integrity of each participant’s middle ear. Standard single frequency tympanometry using an 85dB SPL tone set at 226Hz was performed. Only participants with normal (type Atympanogram) tympanometry results were included as abnormal results preclude DPOAE testing [40].
Pure tone audiometry
Conventional (250Hz-8000Hz) and extended high-frequency (10, 12 and 16 kHz) pure tone audiometry was performed on all participants through the use of Inter-Acoustic AC 40 diagnostic audiometer. The criteria used to define normal hearing, was that of pure tone thresholds of 25dBHL or lower across all frequencies, with the absence of an air-bone gap [43]. Participants presenting with normal pure tone audiometry at baseline were advanced to sessions two, three and four of the study where ototoxicity monitoring was conducted. Using pure tone data, a change in the hearing level of 10 dB at one or more frequencies is commonly taken to be indicative of some significant change [40,44], hence this protocol was followed in the current study.
Distortion product otoacoustic emissions
All participants with normal middle ear functioning underwent DPOAE measurements, as the crucial aspect of ototoxicity monitoring, through the use of a Biologic Scout Otoacoustic emissions meter. OAE testing is often used as a screening tool to determine the presence or absence of cochlear function, and analysis can be performed for individual cochlear frequency regions, therefore they are regarded an excellent tool for early detection of cochlea damage due to ototoxicity [12,33]. OAEs can detect cochlear dysfunction before it is evident on pure tone audiometry, and in ototoxicity monitoring this factor is critical since the main aim of monitoring is early detection of adverse effects of the drug before it causes clinical damage [12,33,45]. One significant methodological improvements of the current study to that by Khoza-Shangase [40] was that extended high-frequency audiometry formed part of the ototoxicity monitoring protocol, so the hailed sensitivity of this measure in ototoxicity monitoring could be assessed in the current study–while at the same time improving the clinical significance of the study. The following DPOAE test protocol was employed:
Test parameters: Diagnostic/High frequencyStimuli:Intensity level L1-L2=10dB (e.g. L1=65dB, L2=55dB)Ratio f2/f1=1.22Frequency range 750 to 8000 Hz
The presence of the DPOAE was determined by comparing the amplitude of the DPOAE to that of the noise floor to calculate the size of the emission. A Distortion Product (DP)-amplitude that exceeded the noise floor by at least 7dB across all frequencies measured was regarded as indicative of a normally functioning cochlea [33,40]. The size of the emission at the different frequencies measured was then monitored over the four testing sessions.
Validity and Reliability
To maintain a high level of test reliability, standardizing test administration, ensuring proper equipment calibration, and controlling participant variables were done. All standard precautionary measures advocated by Bess and Humes [46] and Hall [33] were followed during all audiological assessments. These measures included proper maintenance and calibration of the equipment, optimization of the testing environment, correct earphone and bone vibrator placement, as well as proper probe placement for DPOAE testing [40]. All data collection was performed in a soundproof booth. All participants were tested by the same researcher using the same test procedure at all 4 sessions. Furthermore, all patients were tested in the mornings to reduce the effect that fatigue can have on patients’ responses to behavioural audiometry testing [40].
Data Analysis and Statistical Procedures
Both descriptive and inferential statistics were used to analyze data from the study. Inferential statistics in the form of repeated measures ANOVA, MANOVA, and Tukey-Kramer post-test were used to establish statistical significance levels, and to determine when the statistically significant changes occurred within the longitudinal design of the study. Furthermore, clinical significance of the findings was also analysed [40].
Firstly, statistical comparison was done basing the results on the average change from baseline. Each frequency’s mean change from baseline for the ears individually was computed and then combined for both pure tone audiometry and distortion product otoacoustic emissions. Repeated-measures analysis of variance [34] was used to compare the mean change from baseline from session to session. In the analysis of the DPOAE data, the baseline DPOAE levels in decibels SPL for each f2 value tested were compared with the corresponding session 2, 3 and 4 measurements. The signal-to-noise difference was used as the measure of DPOAE amplitudes. For pure tone audiometry data, the baseline thresholds in decibels HL for each frequency were compared with the corresponding session 2, 3 and 4 results as well. To statistically test the hypothesis, a threshold P value (alpha) of 0, 05 was selected, [47]. Lastly, as part of statistical analysis of the data, a post-test in the form of the Tukey-Kramer multiple-comparison post-test was conducted. This test was conducted to compare pairs of group means so as to identify where, precisely, statistically significant changes occurred along the time continuum [40] (baseline to 15 months)-if they did.
Secondly, for the purposes of the current study, clinical significance (changes that are deemed significant enough to indicate structural and functional changes on the ear–as observed on the audiogram) over and above statistical significance was examined. The current researcher supports the school of thought that maintains that assessing an intervention’s effect should not only focus on the statistical significance of the findings, but should also focus at the clinical relevance or importance of these outcomes [40,48]. For pure tone testing, most often a change of 10dB at one or more frequencies is commonly taken to be indicative of some significant change [44]; andthis was the protocol followed in the current study [40]. As far as DPOAEs are concerned, change is only regarded as significant in DPOAE measures if there is a change of at least more than 6dB in DPOAE level between consecutive measures [49,50]. Absence of clinically significant changes in DPOAEs confirm intact cochlear functioning and the absence of evidence of cochlea damage, even microcochlear pathology–which is often evident on OAEs long before being depicted on the pure tone audiogram [33,40].
Table 2 provides a summary of all collection material and test procedures used in this study.
Ethical Consideration
Permission to conduct the research project was secured from the University’s Human Research Ethics Committee (Medical) prior to commencement of the study. Further permission from all relevant authorities such as hospital management and heads of departments was obtained. Informed consent to participate in the study was obtained from all participants before the study was conducted with an assurance that confidentiality would be maintained. Furthermore, to ensure anonymity, the researcher ensured that no personal or identifying information was included in the research project and research coding numbers instead of identifying information were used. The current study also reduced risks to the participants to a minimum by conforming to the ethical principles [51] and observing provisions of the Nuremberg Code of ethics [34] during the study.
Results
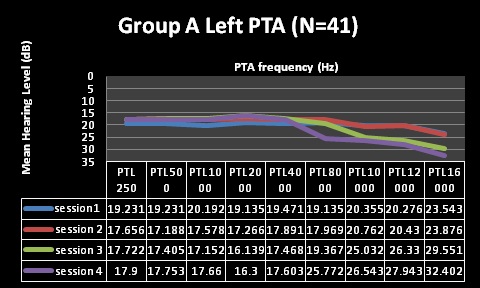
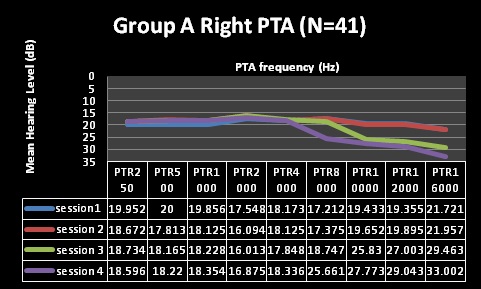
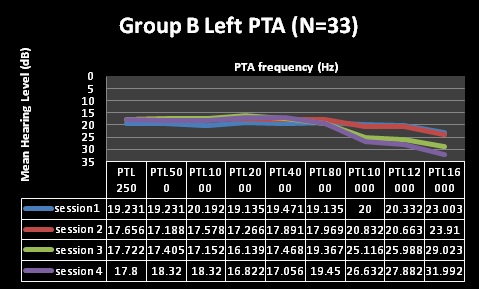
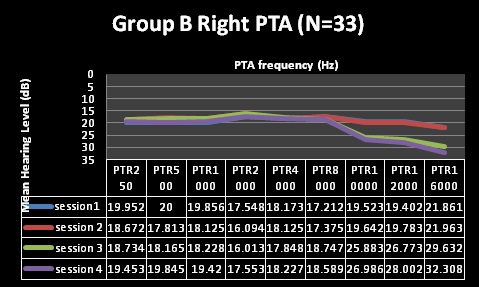
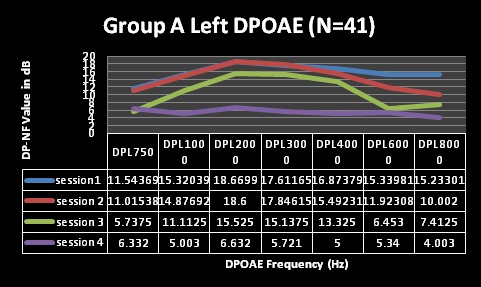
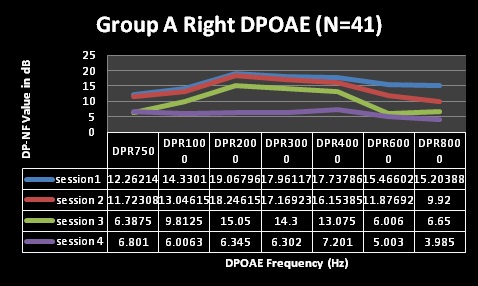
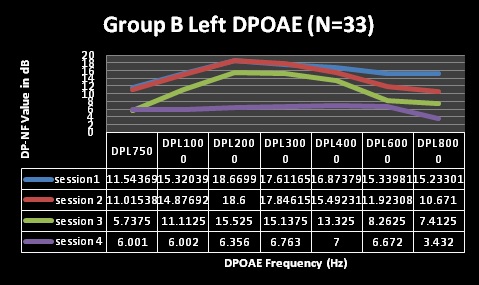
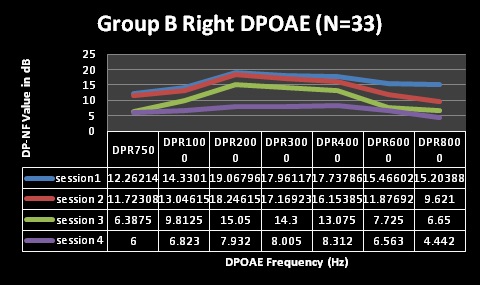
Findings depicted in Table 3 (session 1 and 2) indicate that pure tone audiometry results in both groups A and B revealed hearing within normal limits with average PTAs being above the level regarded as indicative of normal hearing across all frequencies evaluated; with session 2 representing three months following HAART commencement. These findings are depicted in Figures 1-4 for pure tone audiometry in left and right ears below.
Mean results for basic audiometry (250-8000Hz) were normal for all four testing sessions in both groups, with clinically and statistically significant changes at the extended high-frequencies (10, 12, and 16 kHz) from session 3 (at 9 months following HAART commencement). Group A also had changes at 8 kHz at session 4 (15 months), but this change was not statistically significant. Statistical significance was established through the use of MANOVA tables, where all changes in both groups were found to be statistically significant over the 4 testing sessions. MANOVA tables for repeated measures analysis of variance revealed statistically significant changes (alpha was less than 0.05), with the exception of significant changes at 8000Hz [group A at session 4 (p>0.05)]. Moreover, these changes were also audiologically clinically significant changes. Most often a change of 10dB at one or more frequencies is commonly taken to be indicative of clinically significant change [44]. All, but one (8 kHz in group A) of the mean changes in pure tone results of both groups in the current study were greater than 10dB, suggesting that they were clinically significant changes.
Furthermore, DPOAE measures for both groups A and B (Table 3 and Figures 5-8) revealed commencement of decreasing cochlea functioning (as indicated by reduced DPOAE amplitudes); although still within normal limits with average DPOAE emission size being above the level regarded as indicative of normally functioning cochlea across all frequencies evaluated for sessions one and two. MANOVA tables indicated that these changes were not statistically significant (p>0.05). Furthermore, these changes were also not clinically significant. Change is only regarded as clinically significant in DPOAE measures if there is a change of at least 6dB in DPOAE level between consecutive measures [49,50]. At sessions 1 and 2 in both groups; none of the mean changes in DPOAE results were greater than 6dB–indicating that no clinical changes occurred in the cochlear function.
Despite the essentially normal hearing function in high frequencies at sessions 1 and 2, results of the DPOAE analysis in both groups revealed cochlea function to be abnormal from session 2 at 8 kHz in both groups with changes indicating declining DPOAE values at repeated measures. These changes were found to occur at all frequencies evaluated but were more clinically significant at the high frequencies (and 6 and 8 kHz in group A) at session 3 and 4. The DPOAE results at these two frequencies at session 3 were in fact below the norm in that the DPOAE value did not exceed the noise floor by at least 7 dB as expected in a normally functioning cochlea. Statistically, MANOVA [within group (time)] results indicated extremely significant (p<0.001) for all frequencies assessed–implying that cochlear function changed after HAART initiation.
For the statistically significant results for DPOAEs in the ‘within group’ analysis, the Tukey-Kramer test indicated that, generally, the significant changes occurred between baseline measures and session 2 (at 3 months) for the lower frequencies, with the higher frequencies being significantly affected throughout the 4 sessions of testing.
Discussion
The absence of clinically significant changes in pure tone audiometry and DPOAEs in the first 2 sessions (over a period of 6 months post HAART commencement) confirmed intact hearing functioning and the absence of evidence of cochlea damage, even microcochlear pathology – which is often evident in OAEs long before being depicted on the pure tone audiogram [33]. It should be noted that the DPOAE measure used only assesses frequencies until 8000Hz, and does not include extended high-frequencies like the pure tome audiometry measure used. The fact that clinically significant changes were identified at session 3 and 4 (9 and 15 months post HAART initiation) highlights the importance of including extended high-frequencies in monitoring as they would allow for early detection of ototoxicity and afford the attending audiologist and attending physician an opportunity to consider alternative preventative measures significantly before the hearing changes affect frequencies important for speech perception.
These preventative measures would include the use of oto-protective agents as well as dose and medications considerations. When life-threatening illness necessitates treatment with ototoxic drugs, preserving the quality of the patients’ remaining life is customarily a treatment goal. Early detection of ototoxic hearing loss provides physicians with the critical information and opportunity necessary to minimize further impairment and, in some cases, prevent hearing loss from progressing to the point where permanent damage occurs. Although hearing loss is not regarded as a life-threatening condition, it does become a severe threat to essential quality of life indicators unless intervention occurs early during treatment. The adverse effects of a hearing loss on cognitive-linguistic skills and psychosocial behaviour are well documented, as well as the serious vocational, social, and interpersonal consequences for the patient [40]. One might argue that HAART plays a critical role in the treatment of a serious or life-threatening disease, that it offers such important therapeutic effects compared to the ototoxic side effects, that the ototoxicity risk can be considered to be of minor importance. However, the problem of ototoxic side effects is reported to be critical in developing countries, where highly effective and low-cost drugs are more easily prescribed without adequate monitoring [40].
This problem in compounded by the fact that patients on potentially ototoxic medication, without being audiologically monitored, may be exposed to other toxins such as noise exposure following treatment with ototoxic drugs which can act synergistically with the drugs that have not been fully cleared from the inner ear [40]. Increased susceptibility to hearing loss can continue for several months after completion of treatment or therapy with ototoxic drugs, and this might have a different meaning in the case of ARVs where the treatment is for life. Because of this concern, it becomes crucial that hearing conservation in the form of advising patients to avoid excessive noise exposure for at least six months following treatment is instituted. Additionally, provision of hearing aids to this population may require closer monitoring and detailed patient counselling with regards to careful monitoring and control of the hearing aid maximum output during HAART use [40].
The presence of significant changes on DPOAEs in the longitudinal follow up sessions in both groups mirrored previous findings [40] which indicated microcochlear pathology that was not necessarily indicated on pure tone audiometry, when basic audiometry (250Hz-8000Hz) was used. This microcochlear pathology was however not sub-clinical in the current study as it was depicted on the extended high-frequency changes identified in the current study. It is clear from the current study that based on the objective nature of DPOAE measures, subclinical auditory changes occurred as early as 3 months, with clinical changes clearly identifiable by 9 months following HAART initiation in both groups. These findings firstly, highlight the importance of the use of such sensitive measures (DPOAE) in monitoring the possible effects of toxins on the ear since DPOAE have been shown to have an arguably important role to play in this regard. Secondly, these findings reveal the crucial need for including extended high-frequencies in ototoxicity monitoring to be able to identify clinical changes on the audiogram early enough before these changes include frequencies important for speech perception.
The presence of extended high-frequency and DPOAE changes indicating changes in hearing status suggested hearing loss that could have possibly been due to medications used by participants in the two groups (Group A: nevirapine, 3TC-lamivudine, and D4T-stavudine; and Group B: AZT-azidothymidine, 3TC, and efavirenz). These results were consistent with the reports that have associated iatrogenic hearing loss with many of the drugs used to treat HIV/AIDS [11,14,40].
Although one cannot draw definitive conclusions that HAART regimens used in the current samples had a direct effect on hearing – because of the difficulty in controlling extraneous variables in such a population, and also because of the lack of a control group; findings are supported by previous evidence. Current findings are also consistent with ototoxic hearing loss in terms of nature and configuration of the loss on audiograms–where high frequencies are the primary initial site of clinical change. Controlling for extraneous variables in human subjects with AIDS is an impossible task, and the current researcher is of the strong opinion that isolating all the possibly contributing confounding variables may provide a more definitive answer with a clearer cause-and-effect relationship, but may not necessarily provide a practical, relevant, and context-sensitive finding. Within the South African AIDS population, it may be impossible to find participants who are only exposed to just one strict HAART regimen without any other medications prescribed for the numerous other conditions the patient might present with, including TB. Furthermore, the possible effects of the use of alternative/complimentary medications by a large majority of South Africans alongside HAART cannot be ignored. Current results are believed to be valuable evidence for the South African context, and provide more realistic and context specific implications, those of the importance of audiologists’ involvement in the drug development process, the audiologists’ inclusion in the treatment teams where ototoxic medications are prescribed, the need for establishment and implementation of ototoxicity monitoring protocols as part of routine clinical management of adults with HIV/AIDS, and the inclusion of both DPOAEs and extended high-frequency audiometry in ototoxicity monitoring protocols.
Current findings, confirm earlier findings by Khoza-Shangase [40] where ototoxicity of lamivudine-3TC, stavudine-D4T and efavirenz was monitored in a group of adults, with an additional new finding illustrating the usefulness of extended high-frequency audiometry in early identification of drug-induced hearing loss. Firstly, the importance of analysing both clinical and statistical significance in findings was re-affirmed. Current findings highlight the importance of including both these means of establishing significance in such longitudinal audiological studies, where one might find statistically non-significant but clinically significant changes, and vice versa–or the ideal where clinically and statistically findings are obtained.
Conclusion
The current study provides further evidence from a developing country context for the need to expand the role for the audiologist in Food and Drug Administration processes of drug development, drug approval, and drug monitoring [40]. The clinically and statistically significant changes at the extended high-frequencies (frequencies not routinely included in an audiology assessment) highlight the importance of including these frequencies for early identification of ototoxicity initiatives. Furthermore, the sub-clinical hearing changes (cochlea function changes detected before the hearing loss is seen on an audiogram) again highlight the importance of DPOAEs in ototoxicity monitoring studies [40]. Current findings further demonstrate the significant role audiologists have at Primary Health Care Level in the assessment and treatment of patients with AIDS to serve as part of the team looking at enhancing quality of life once it is preserved by HAART. Medical awareness of HAART doses, methods of administration, populations at risk, as well as possible synergism with other factors (such as noise exposure) is important in order to develop appropriate care in the prescription of drugs with possible or established ototoxic side effects. Khoza-Shangase [40] further asserts that issues such as risk-benefit analysis, patient-informed consent, and quality-of-life considerations, are also crucial factors to be considered in the management of patients with HIV/AIDS, and this isregardless of whether the effects of the drug are negligible or not. This author argues that such effects still require categorization so that proper patient adherence counselling can occur to prevent patients abandoning treatment due to unexpected side-effects. It is also important that audiologists become intimate with ototoxic effects of medications used to manage chronic conditions such as HIV/AIDS, and medications prescribed to significant numbers of people–such as the 17% of adults aged 15-49 years afflicted by HIV/AIDS in South Africa [52]. Audiologists’ knowledge and their constant updating of the catalogue of ototoxic medications is crucial if appropriate patient education is to occur, particularly since patients may not notice ototoxic hearing loss until a communication problem becomes evident, indicating at that stage that hearing loss within the frequency range which is important for understanding speech, has already occurred [40].
It is important to interpret findings from the current study having taken cognizant of the identified methodological limitations. The main limitations of the current study included, firstly, that for ethical and practical reasons there was no control group, but this was partially overcome by the fact that each participant served as their own control within the longitudinal study design. Secondly, the nature of the HIV/AIDS disease and the population being studied precluded complete control over confounding variables that could have had an influence on the results such as interactions of ARVs with other therapies, especially traditional medicines which have been reported to be in widespread use. Nevertheless, current findings add to the growing evidence on links between HAART and ototoxicity, and aid in attempting to provide an answer to the question: Does HAART sound toxic? Current findings clearly demonstrate the ototoxic nature of HAART; and also present an argument for pharmaco-audiology vigilance when HAART is used in South Africa: a continued need for pursuing ototoxicity monitoring.