
A Novel Regional Interdependent Approach using Primal Reflex Release Technique on Patellofemoral Pain: A Case Study
*Corresponding Author(s):
Joshua K.UnderwoodDepartment Of Kinesiology And Sport Sciences, University Of Nebraska, Kearney, NE, United States
Tel:+1 3088658014,
Email:underwoodjk@unk.edu
Abstract
Introduction: Patellofemoral pain (PFP) is a very common injury seen in both athletic and civilian populations. Current treatment approaches focus on stretching and strengthening of the tissues surrounding the knee, while any decrease in symptoms associated with the PFP can take anywhere from 6 weeks to 8 months. While it is understood that many biomechanical factors effect symptomology in PFP, there are no current studies using a Regional Interdependent (RI) approach. Primal Reflex Release Technique (PRRT) is a treatment that focuses on down-regulating tissues via stimulation of the startle reflex that results in instant and long lasting effects. The purpose of this case was to examine the instantaneous and long lasting effects of PRRT on a patient with PFP.
Case: A 17-year-old female with recurring PFP symptoms for 56 months. The patient had failed other forms of therapy prior to the study and had no short-term or long-term decrease in pain at any time. Numeric Pain Scale, the Disability in the Physically Active (DPA) Scale, Patient Specific Functional Scale (PSFS), and the Global Rating of Change (GRC) Scale were administered to identify patient-reported pain and dysfunction.
Outcome: The utilization of PRRT in a RI approach to the ipsilateral scalene resulted in instantaneous reduction in pain and improved function; whereas only 4 treatment sessions were required to resolve her pain. Statistically and clinically significant improvements were observed for NRS, DPA, PFSF, and GRC immediately following her initial treatment; however, while all improvements were kept prior to follow-up treatments only significant improvements were seen in individual PSFS at 3 weeks (Stairs) and at 6 months (Squat & Row).
Discussion: In this case, the use of PRRT in a RI approach resulted in positive changes in terms of function and pain while also doing so in less time than previously reported using more traditional methods of treating PFP. Clinicians should consider either RI style evaluations or the addition of PRRT into rehabilitation programs of patients with PFP, especially if those patients have failed other treatment methods prior.
Keywords
Patellofemoral pain; Primal reflex; Regional interdependence
INTRODUCTION
General knee pain accounts for approximately 25% of patient medical appointments [1]. While there are no current classification criteria for PFP and is essentially diagnosed from excluding other causations, there are some consistently seen complaints from these patients [1-6]. Activities such as stairs, prolonged sitting, squatting, kneeling, running, and jumping are all common complaints from patients with PFP [1-6]. However; consensus among healthcare providers is the cause of PFP stems from a multi-factorial complications of musculature asymmetry, latency dysfunctions, compromised tissue restraints of the patella, decreased flexibility, hip dysfunctions, and/or problematic foot postures [1-6]. Thus there is a significant focus on strengthening and stretching of the lower extremities which take on average 6 weeks to 8 months for symptoms to decrease [1-6]. During that period, patients may not be compliant with home exercise programs due to the increase of pain from the exercises [3]. One explanation of why the resolution of PFP related dysfunction is so difficult is that clinicians may be treating a source of pain, not the root causation of the condition.
Regional Interdependence (RI) is defined as a seemingly unrelated impairment in a remote anatomical region that contributes to or is associated with, the patients’ primary complaint [7]. For example; poor body posture while sitting for long periods can lead to neck and shoulder pain. The hypertonic shortened or lengthened muscles in the neck and shoulder region or even lumbosacral regions can change the nature of a patient’s biomechanical state. Pulling them out of homeostasis and impeding the biotensegritis functioning of the body. Be that as it may, individual’s may complain of cervical neck pain but the underlying condition may lay in upper cross syndromes, lower cross syndromes, neurological impairments, or even arthrokinematic dysfunctions in their extremities. However; for many pathological or disease states, the focus of therapeutic interventions is around the locale of the pain and may not be treating the origin of the condition. Due to the various body regions and systems, more than one aspect (fascia, neuromuscular, arthrokinematics, psychosocial, etc.) within a RI model can be the cause of an observed dysfunction [7-10]. While far from being an exact science currently, the concept of RI is being studied in terms of evaluation and treatment in regards to several pathologies [7-10].
Primal Reflex Release Technique is a treatment that focuses on down-regulating a painful autonomic nervous system response by using the body’s primal reflexes to bring the tissues back into a homeostatic state [11-14]. Depending upon the tissue structures that involved, PRRT treatments utilize light oscillations, tapping, or stimulations to stimulate the startle reflex response desired [11-14]. The hypothesized theory on explaining how PRRT works is rooted in how the spinal cord and brain react to reflex stimulation. Patients who are stuck in a fight or flight response can have repetitive reflex stimulations that are continuously being produced long after the initial stimulus as stopped [11-14]. Unable to allostatically break the cycle, the body remains in a sympathetic response causing tissues surrounding the trauma to suffer from hypertonicity and neuormetabolic cascade of events [13,14]. Primal Reflex Release Technique may cause the brain and spinal cord to reset by giving the tissue a new stimulation, similar to proprioceptive neuromuscular facilitation, giving the brain a chance to reevaluate the current circumstances [11].
CASE PRESENTATION
A 17-year-old female crew member at a secondary school clinic was examined for bilateral PFP which caused significant pain while performing squats/rowing, going downstairs, running, and hiking. The participant was diagnosed by her primary care provider with bilateral PFP 56 months prior to her appointment with the primary researcher. She stated that while traditional rehabilitation exercises and modalities helped over the previous 56 months, they never resolved the pain and only had therapeutic effects for a day or two. Due to the participant’s lengthy history of PFP and lack of impactful interventions, she was evaluated while using an RI approach to locate fascial chain dysfunctions. Within the primary researcher’s clinical setting, PFP dysfunctions had been observed to be caused by a specific fascial adhesion at the anterior scalene that had a cascading restrictive effect down to the ipsilateral plantaris tissue structures leading to a compressive influence to the anterior structures of the knee initiating the painful stimuli. As previously observed in other cases at the primary researcher’s clinic over the past three years, the participant presented with Tender Points (TP) along bilateral anterior scalene, pectoralis minor, psoas, and plantaris while using osteopathic methods of palpation.In an effort to pinpoint the exact hyperirritable muscle/fascial tissue, once a TP was located the primary research had the subject perform the primary movement of the theorized muscle while gauging whether the tissue contracted or not with the palpatory finger. The treatment protocol was approved by the secondary school and University Institutional Review Board. The research participant and parent/guardian(s) signed an informed consent form before involvement and were informed of their rights before PRRT treatment and outcomes collected.
Initial outcomes collected before treatment included the Patient-specific Functional Scale (PSFS), Numerical Rating Scale (NRS), Disablement in The Physically Active Scale (DPA), and Kujala Scale (KS).The utilization of the Patient-Specific Functional Scale (PFSF) was added to assess the patient’s perceived functional ability in performing more active or sports related movements deemed meaningful to the patient. Each movement/activity is scored from 0 (“unable to perform”) to 10 (“able to perform the activity/movement at the same level before injury”) [15]. Scores for PFSF can be analyzed individually or as an average score of all activities/movements [15]. The MCID for PFSF is 2 points for analyzing an average score or 3 points for an individual movement/activity [15].The NRS is an 11 point Likert scale for patients to self-report pain and is intended for adults and children aged 10 year old and older [16]. A score of 0 indicates no pain, a score of 1-3 indicates mild pain, a score of 4-6 indicates moderate pain, and 7-10 indicates severe pain [16]. A Minimal Clinically Important Difference (MCID), which is the smallest amount of change that is meaningful to the patient for the NRS is any change ≥ 2.0 [16]. The DPA is a patient related outcome designed to assess a patient’s perception of their injury and how it effects the quality of life and/or physical activity. The DPA is completed by the patient and ranges in scores from 0 to 64, with a lower score indicating less impact on daily life functions [17,18]. The MCID values related to DPA have been calculated at nine points, for acute injuries, and six points, for chronic injuries [17,18]. The KS is a Patient Related Outcome (PRO) screening tool that is made up of 13 questions where the higher the score suggests the patient is not suffering any patellofemoral dysfunction. The maximum score a patient can score is 100 and MCID values have been calculated to be any change ≥10 [19]. Upon finishing the participant’s PRRT session, all initial outcomes were collected again and a Global Rating of Change (GRC) was collected (Table 1). The GRC has been used to collect PRO to determine the effect of treatments from the patient’s point of view. The MICD for such tools, were an 11 point Likert scale was used, has been found to be changes ≥ 2 [20].Outcome collection was gathered once a week before the PRRT session for the duration of the case study until discharge.
|
Outcome |
Initial |
Post Treatment |
1 Week Follow-up |
2 Week Follow-up |
3 Week Follow-up |
Discharge |
6 Months Post Discharge |
|
PFSF- avg |
4 |
8* |
8.1 |
8.4 |
8.8 |
9.4 |
9.9 |
|
-Hiking |
5 |
9* |
9 |
9 |
9 |
10 |
10 |
|
-Stairs |
4 |
7* |
8 |
8 |
9* |
10 |
10 |
|
-Squats/Row |
2 |
8* |
7.5 |
8 |
8 |
9 |
10* |
|
-Run |
4 |
8* |
8 |
9 |
9 |
9 |
10* |
|
Kujala |
70 |
97* |
95 |
97 |
99 |
100 |
100 |
|
DPA |
29 |
8* |
9 |
8 |
5 |
0 |
0 |
|
NRS- Stairs |
3 |
0* |
1 |
1 |
0 |
0 |
0 |
|
- Scalene TP |
6/7 |
0/0* |
2/2 |
6/0 |
0/7 |
0/0 |
0/0 |
|
-Pec Minor TP |
7/7 |
0/0* |
4/4 |
7/0 |
6/6 |
0/0 |
0/1 |
|
-Psoas TP |
6/7 |
0/0* |
3/3 |
6/0 |
5/0 |
0/0 |
0/0 |
|
-Plantaris TP |
5/7 |
0/0* |
2/2 |
6/0 |
0/0 |
0/0 |
0/0 |
|
GRC |
N/A |
4.5* |
4 |
4 |
4.5 |
5 |
5 |
|
NRS TP= Right/Left; Minimal clinically importance differencesmet or exceeded = * |
|||||||
Table 1: Outcome Measures.
The participant was treated once a week with only PRRT scalene release until all TP were non-painful. Treatment began by having the participant lay supine on a plinth so that the head was positioned towards the primary researcher. In figure 1, the clinician’s hands were placed in a cupping manner so that the participant’s elbows rested in their palms and the clinician’s chest gently making contact with the participant’s head. The participant’s hands were then conveniently placed on their abdomen. The PRRT scalene release involves the clinician using quick, but gentle finger flicks to the participant’s elbows generating a slight shoulder shrug in an oscillating manner for 10 seconds per one repetition. Participants were treated in the manner for 2 sets of 10 cycles of oscillations before TP was re-evaluated. Therapeutic sessions ended when TP NRS was 0, at which time stair NRS was measured. The primary research has over 3 years of PRRT experience in treating similar cases. During the case study, the participant was allowed to participate in all crew related activities as tolerated and rowed in 3 races before discharge during the course of this study.
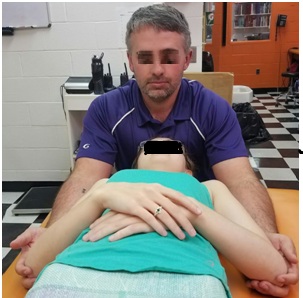 Figure 1: Clinician Positioning for PRRT Scalene Release.
Figure 1: Clinician Positioning for PRRT Scalene Release.
As evident in table 1, the participant showed significant improvement immediately after the first treatment. There was an overall average improvement in PSFS of 4 points, with individual improvements to hiking (4), stairs (3), squat (6), and running (4). A significant increase in knee-related function or pain report in Kujala (27) and DPA (21) were additionally described. The participant reported an overall instant improvement of 4.5 (GRC) at the end of the initial treatment and no pain while performing stairs. The participant was not limited in physical activities and competed in a race a few days later for the first time in the season. A week later the participant filled out outcomes before treatment and received another PRRT scalene treatment. While the effect of the first treatment session was retained, sequential weekly follow-ups and treatments had a much slower effect in full resolution of her PFP knee pain. However; after 4 treatments the participant reported no knee pain during activities for the first time in 56 months and was discharged at 5 weeks. The effects of the treatment were sustained for 6 months post-discharge (Table 1).
A variety of outcomes measures were chosen to evaluate the effect of a RI PRRT approach in treating PFP. The NRS was selected to assess perceived levels of pain with TP evaluations and performing a 10” stair-stepping activity. The NRS is an 11-point Likert scale for participants to self-report pain and is intended for adults and children aged 10 years and older [16]. A rating of 0 indicates no pain, a score of 1-3 indicates mild pain, a score of 4-6 indicates moderate pain, and a score of 7-10 indicates severe pain [16]. The utilization of the PSFS, DPA, and KS was picked to evaluate the effect of the treatments on the participant’s perceived physical activity. Lastly; an 11 point GRC was used to assess the participant’s perception of overall improvement in their physical condition [20].
OUTCOMES
Minimal Clinical Importance Differences (MCID) is the amount of change for a specific outcome measure that reflects the most minuet change a participant would recognize as being meaningful. For example, an MCID for the NRS is any change greater than or equal to 2.0 [16]. The participant experienced an MCID improvement performing stair activity (3 point change) after the first treatment; however, there was no MCID observed post-treatment at any other point. Conversely; there was MCID improvement with TP NRS after every therapeutic intervention (Table 2). While there was no TP along the plantaris before the 4th treatment, there were still abnormal fascial tensions within the fascial chain leading to the clinical decision to treat the chain one last time.
|
TP Location |
Pre-Treatment 1 |
Post-Treatment 1 |
Pre-Treatment 2 |
Post-Treatment 2 |
Pre-Treatment 3 |
Post-Treatment 3 |
Pre-Treatment 4 |
Post-Treatment 4 |
|
Scalene |
6/7 |
0/0 |
2/2 |
0/0 |
6/0 |
0/0 |
0/7 |
0/0 |
|
Pectoralis Minor |
7/7 |
0/0 |
4/4 |
0/0 |
7/0 |
0/0 |
6/6 |
0/0 |
|
Psoas |
6/7 |
0/0 |
3/3 |
0/0 |
6/0 |
0/0 |
5/0 |
0/0 |
|
Plantaris |
5/7 |
0/0 |
2/2 |
0/0 |
6/0 |
0/0 |
0/0 |
0/0 |
|
NRS values are listed as right/left |
||||||||
Table 2: NRS TP Pre and Post Treatment.
A significant decrease of 21 points was described by the participant immediately after their initial treatment as measured by the DPA. An MCID value for the DPA for chronic conditions has been established at 9 [17,18]. The immediate effect of the treatment far exceeds the MCID which means the participant felt a noteworthy difference pre-post intervention. Conversely; it wasn’t until discharge (4 weeks later) that another MCID would be observed, but signified total resolution of pain stemming from PFP.
A similar effect was observed within the PSFS immediately after the PRRT treatment. An average of a 4 point increase (4.0-8.0) among all activities measured within the PSFS was recounted by the participant. The increase exceeded the necessary MCID for average scores on the PSFS of 2 points [15]. The MCID for individual activities in the PSFS is 3 points; however, individual increases ranged from 3 points to 6 points which again exceeds the MCID [15]. On the contrary; no MCID values were obtained after the initial intervention but nearly had perfect scores (10 being able to perform the activity as normal) at discharge. The outcomes for KS were very similar. There was an initial increase in scores (27 points) which far exceeded the MCID of 9, but no further meaningful changes were seen over the course to discharge [19].
DISCUSSION
The participant conveyed within their outcomes that an MCID was felt immediately after the first treatment using a RI approach of PRRT to the anterior scalenes. The prompt increase in function and decrease in pain measured by the participant oriented outcomes suggest that a RI approach to fascial chain dysfunctions causing PFP can be a holistic treatment option. The participant in this case study received 4 treatments of only PRRT to the anterior scalenes over 4 weeks, while simultaneously never missed a practice, conditioning session, or crew race over that period. Current literature suggests that it takes an average of 6 weeks to 8 months for symptoms to decrease while using traditional methods; however, this participant showed a drastic improvement in pain and function within the first treatment and was healed in 4 weeks while using a RI approach [1-6].
While this specific Deep Fascial Spiral Pattern (DFSP) hasn’t been documented or correlated in causing knee pain, there are a few similar patterns that have been discussed in various texts. In a prominent text written by Tom Myers called “Anatomy Trains”, elements of this pattern can be seen in his spiral line and deep front line myofascial lines [21]. However; they don’t match perfectly to what is observed in clinical evaluations versus what is written in the text. Theoretically this DFSP could begin with dysfunction breathing patterns utilizing secondary breathing muscles as primary breathers or forward head postures shifting the bodies’ center of gravity leading to biotensegrital breakdown over the course of weeks, months, or years. As the dysfunction progresses, the fascial tissue begins to tighten not unlike a dish towel being twisted causing the associated tissues of the DFSP to tighten and place additional pressure into the anterior knee structures via posterior knee capsule tension and altered biomechanics. This could explain why certain muscles test weak during evaluation (antagonists of the pattern) and why current methods of treating PFP result in short term gains in relations of pain resolution or pathobiomechanical corrections. Resetting of the startle reflex at the scalene, the perceived origin of dysfunction, allows the body to break the sympathetic cycle causing the pain and also resets the central nervous system in recognizing a more homeostatic postural position.
Several limitations should be considered with this case study. The general diagnosis and the pathological causation of PFP is relatively unknown. Further studies need to be performed in narrowing down local and RI causations of PFP or other ambiguous anterior knee pain pathologies. Additionally; there is no known fascial chain that follows the pathway described in this case study and further study of this specific chain is needed. While there are many validated participant related outcomes around the knee, the KS was chosen for its simplicity and is currently considered the top outcome as it relates specifically to PFP. The use of other knee-related outcomes may have been better suited to capture the full picture of this study or be more relatable to previous studies on PFP. Lastly; scheduling and staffing conflicts did not allow for multiple treatments to occur in a single week. If multiple treatments could have been carried out in a single week, the healing time to discharge could theoretically be decreased.
CLINICAL BOTTOM LINE
The use of the RI approach or treatment on PFP with PRRT has never been examined within the current literature. In this case study, a clinician was able to use PRRT to the anterior scalenes to produce clinically significant improvement in multiple outcome measures in just one treatment and have total resolution of PFP in just 4 treatments with no physical limitations or other interventions. The participant never missed a single day of practice or competition during the entire process. When patients are diagnosed with PFP or come into the clinic with no specific knee pain, RI causations like the one outlined in this case study could be utilized a part of the patient’s evaluation. Further clinical research is needed to substantiate the findings of this study.
REFERENCES
- Ismail MM, Gamaleldein MH, Hassa KA (2013) Closed Kinetic Chain exercises with or without additional hip strengthening exercises in management of Patellofemoral pain syndrome: a randomized controlled trial. Eur J Phys Med 49: 687-698.
- Keays SL, Mason M, Newcombe PA (2014) Individualized Physiotherapy in the Treatment of Patellofemoral Pain. Physiother Res Int 20: 22-36.
- Monson J, Arendt EA (2012) Rehabilitative protocols for select patellofemoral procedures and nonoperative management schemes. Sports Med Arthrosc Rev 20: 136-144.
- Rixe JA, Glick JE, Brady J, Olympia RP (2013) A review of the management of patellofemoral pain syndrome. Phys Sportsmed 41: 19-28.
- Smith TO, McNamara I, Donell ST (2013) The contemporary management of anterior knee pain and patellofemoral instability. Knee 20: S3-S15.
- Tjoumakaris FP, Forsythe B, Bradley JP (2010) Patellofemoral instability in athletes: treatment via modified Fulkerson osteotomy and lateral release. Am J Sports Med 38: 992-999.
- Wainner K, Whitman J, Cleland J, Flynn T (2007) Regional interdependence: a musculoskeletal examination model whose time has come. J Orthop Sports Phys Ther 37: 658-660.
- Cook G (2010) Movement. Aptos, CA: On Target Publications; 2010.
- Myers T (2009) Anatomy Train: 2nd Ed. New York, NY: Elsevier; 2009.
- Sueki D, Cleland J, Wainner R (2013) A regional interdependence model of musculoskeletal dysfunction: research, mechanisms, and clinical implications. J Man Manip Ther 21: 90-102.
- Hansberger B, Baker R, May J, Nasypany A (2015) A Novel Approach to Treating Plantar Fascitis- Effects of Primal Reflex Release Technique: A Case Series. Int J Sports Phys Ther 10: 690-699.
- Iams J (2005) When Reflexes Rule: A new paradigm in understanding why some patients don’t get well. Advance for Physical Therapists 16: 41-43.
- Iams J (2012) Primal Reflex Release Technique. What is the primal reflex release technique for pain relief? 2012.
- Bianco L, May J, Nasypany A (2019) A Novel Apporach to Treating Acute Hamstring Functional Neuromuscular Disorder-Effects of Primal Reflex Release Technique. Clinical Practice in Athletic Training 2: 19-31.
- Stratford P, Gill C, Westaway M, Binkley J (1995) Assessing disability and change on individual patients: a report of a patient specific measure. Physiotherapy Canada 47: 258-263.
- Salaffi F, Stancati A, Silvestri CA, Ciapetti A, Grassi W (2004) Minimal clinically important changes in chronic musculoskeletal pain intensity measured on a numerical rating scale. Eur J Pain 8: 283-291.
- Vela LI, Denegar C (2010) Transient Disablement in the Physically Active with Musculoskeletal Injuries, Part I: A Descriptive Model. J Athl Train 45: 615-629.
- Vela L, Denegar C (2010) The disablement in the physically active scale, part 2: the psychometric properties of an outcomes scale for musculoskeletal injuries. J Athl Train 45: 630-641.
- Crossley K, Bennell K, Cowan S, Green S (2004) Analysis of outcome measures for persons with patellofemoral pain: which are reliable and valid? Arch Phys Med Rehabil 85: 815-822.
- Kamper SJ, Maher CG, Mackay G (2009) Global Rating of Change Scales. Journal of Manual & Manipulative Therapy 17: 163-170.
- Myers TW (2009) Anatomy Trains Posters: Myofascial Meridians for Manual and Movement Therapists. United Kingdom, Elsevier Science Health Science Division, 2009.
Citation: Underwood JK (2020) A Novel Regional Interdependent Approach using Primal Reflex Release Technique on Patellofemoral Pain: A Case Study. Sport Med Inj Care 2: 008.
Copyright: © 2020 Joshua K.Underwood, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

