
Clinical Experiences and Midterm Results of the Treatment of Clubfoot with the Ponseti Method
*Corresponding Author(s):
Emrah SayitDepartment Of Orthopedics And Traumatology, Samsun Education And Research Hospital, Samsun, Turkey
Tel:+90 5056708662,
Email:dremrahsayit@gmail.com
Abstract
Introduction: Among the current treatment options for Talipes Equinovarus (TEV), also known as clubfoot, is the Ponseti method, which is currently the most popular treatment method worldwide. The aim of this study is to report our results of using the Ponseti method in the treatment of TEV patients.
Materials and methods: We reviewed 92 feet from 60 patients who were treated with the Ponseti method and evaluated their conditions via the Pirani and Dimeglio scoring systems. Of the 60 patients, 32 patients (53%) had clubfeet bilaterally, 18 (30%) patients were affected in only the right foot, and 10 (17%) patients were affected in only the left foot. Furthermore, 43 (72%) of the 60 patients were males and 17 (28%) were females. Lastly, 10 (16%) patients had a family history of the disease. The mean age for starting treatment was 7.55 days. The mean number of casts applied per patient was 5.73 ± 0.8. The mean follow-up duration was 31.2 months.
Results: The mean Pirani score for the 92 feet studied was 3.62 ± 0.58 before the treatment. This score dropped significantly to 0.36 ± 0.42 after the course of treatment (p<0.05). The mean Dimeglio score was 14.75 ± 1.55 before therapy and 4.76 ± 0.91 after the course of treatment (p<0.05). Fifty-five patients (92%) required a percutaneous achillotenotomy. At the time of the follow-up examinations, 25 feet from 17 patients (28%) required additional interventions beyond achillotenotomy. Regarding responsiveness to treatment, we found no statistically significant differences between males and females, left and right feet, and those with or without a family history for the disease (p>0.05).
Conclusion: Although the Ponseti method requires a significant effort for both clinician and family, every orthopedist should know and apply the Ponseti method in the treatment of clubfoot due to its successful results.
Keywords
INTRODUCTION
Although the Ponseti method of treatment was first described many years ago, it recently became the standard method of treating TEV due to its successful long-term results.
Several scoring methods have been developed to assess the foot before, during, and after treatment for TEV. For this study, we incorporated data from two of the most commonly used scoring systems, Dimeglio and Pirani. Dimeglio and his colleagues divide a clubfoot deformity into four measurable anatomical features, or subgroups, which are scored on a scale of 20 points. These subgroups are equinus in the sagittal plane, varus deviation in the frontal plane, derotation around the talus of the calcaneo-forefoot block, and adduction of the forefoot on the hindfoot in the horizontal plane. Each subgroup is assessed in severity from 1 to 4 points. In the presence of a posterior or medial fold, extreme cavus and/or muscle weakness, another point is added to each category for a possible total of 5 points [3]. The second scale, the Pirani scoring system, evaluates six parameters of the foot separately as normal (0 points), moderate to severe (0.5 points), or severe (1 point). These anatomical parameters are the curvature of the lateral border of the foot, degree of medial skin fold, covering of the head of talus, degree of posterior skin fold, equinus or extreme plantar flexion at the ankle joint, and the presence of a free heel [4]. The Dimeglio and Pirani scoring systems are useful in evaluating the degree of correction of the foot as well as the potential for the prognosis of the disease.
In the following study, we examine the components of the Ponseti method and share our experiences and results.
MATERIALS AND METHODS
For casting the legs after manipulation, we used the classic casting method of combining 5 or 10 cm of cotton with plaster of Paris. No synthetic casting materials were used. A trained orthopedic surgeon and a resident performed the Ponseti manipulations. We encouraged feeding of the infants prior to cast molding and placement.
We followed up with all patients for at least one hour after each cast was set in order to check for proper circulation to the leg. Additionally, we explained the symptoms of failed circulation to family members and instructed them to contact our emergency services in case they were unsure about interpreting the patient’s symptoms correctly.
A new cast was set on each patient once per week. Old casts were removed at the clinic just before the new ones were applied. When we observed a full recovery in the cavus, adductus, and varus components of the foot, we evaluated the dorsiflexion of the foot to see if an achillotenotomy was necessary. If residual equinus was observed after the correction of other components, an achillotenotomy was performed blind in a percutaneous way with the patient in the operating room under local anesthesia. Although tenotomy does not require suturing, we used a single suture to close the wound and prevent additional bleeding. Afterwards, a long leg cast was applied with 15 degrees of dorsiflexion and 70 degrees of abduction. Patients were watched for 24 hours at the clinic to ensure the legs received proper circulation. There were no further complications during or after surgical interventions. Sutures were taken out after the removal of the casts at the end of the third week of treatment.
Patients started using orthoses the same day we removed the casts at the end of the third week. Each orthosis was made of a pair of laced boots and an iron bar that connected them, which is also known as a “Denis Browne bar”. The back and front of the boots were left open in order to see the feet from outside the boots and to be sure they were fitted properly. The orthoses had no medial arch supports. If the disease affected only one foot, the boots were set to 75 degrees of external rotation on the deformed side and 45 degrees of external rotation on the normal side. If a patient exhibited bilateral deformities, both boots were set to 70 degrees of external rotation. The iron bars were thick enough and long enough to maintain the distance of the heels at about shoulder width. Boots that became too small for patients were renewed at follow-up meetings.
Orthoses were used 24 hours a day for the first three months. Families were allowed to remove the orthoses only once in a 24-hour period for taking baths. Parents were trained to fit and remove the orthoses on their children. For any problems or difficulties with the orthoses, parents were instructed to contact us. After the third month, the orthoses were used 12 hours per day until the age of three. To make compliance easier, parents were encouraged to use the orthoses when the babies were sleeping. Follow-up meetings with the patients were scheduled every three months during the first year and then every six months for subsequent years (Figure 1). Every treated foot was monitored and evaluated using both the Dimeglio and Pirani scoring systems. Statistical analyses were conducted by using a chi-squared t-test to assess the distribution of scores with 1 degree of freedom. A p value of p<0.05 was selected as the level of statistical significance.
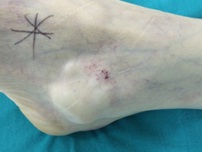
Figure 1: Photographs before and after treatment with the Ponseti method.
RESULTS
Of the 43 males in the study, 13 (30%) had deformities in the right foot only, 5 (12%) had deformities in the left foot only, and 25 (58%) had bilateral involvement of the disease. Of the 17 females in the study, 5 (29.5%) had deformities in the right foot only, 5 (29.5%) had deformities in the left foot only, and 7 (41%) had bilateral involvement of the disease. The distribution for occurrence of the deformity between legs was more homogeneous in females than in males.
The mean age for commencement of the treatment was 7.55 days. Excluding one late-onset patient, whose treatment began in third month of life, the mean age for patients when they presented was 6.45 days.
The mean number of casts applied was 5.73 ± 0.8. The mean number of casts applied before the achillotenotomy was 4.81 ± 0.76. Fifty-five patients (92%) required a percutaneous achillotenotomy in conjunction with treatment. The other five patients (8%) did not need an achillotenotomy because they did not experience dorsiflexion restriction. The mean follow-up period was 31.2 months.
The mean Pirani score for the 92 feet from all 60 patients was calculated to be 3.62 ± 0.58 before treatment. After treatment, the mean score fell to 0.36 ± 0.42 on the Pirani scale. The mean Dimeglio score was calculated as 14.75 ± 1.55 prior to treatment; this mean fell to 4.76 ± 0.91 after treatment (Table 1).
| Before the treatmeant | After the treatment | p | |
| Pirani Score | 3.62 ± 0.58 | 0.36 ± 0.42 | p<0.05 |
| Dimeglio Score | 14.75 ± 1.55 | 4.76 ± 0.91 |
For males alone, the mean Pirani scores before and after treatment were 3.59 ± 0.58 and 0.33 ± 0.4, respectively. The mean Pirani scores for the females alone before and after treatment were 3.71 ± 0.58 and 0.44 ± 0.47, respectively. The mean Dimeglio scores for the males alone before and after treatment were 14.6 ± 1.51 and 4.71 ± 0.85, respectively. The mean Dimeglio scores for the females alone before and after treatment were 15.17 ± 1.63 and 4.92 ± 1.05, respectively (Table 2).
| Before the treatmeant | After the treatment | p | ||
| Pirani Score | Male | 3.59 ± 0.58 | 0.33 ± 0.4 | p<0.05 |
| Female | 3.71 ± 0.58 | 0.44 ± 0.47 | ||
| Dimeglio Score | Male | 14.6 ± 1.51 | 4.71 ± 0.85 | |
| Female | 15.17 ± 1.63 | 4.92 ± 1.05 |
There were no statistically significant differences between the mean Dimeglio and Pirani scores of males and females before and after treatment (p>0.05). No statistically significant difference was found between the mean Pirani and Dimeglio scores for left and right feet before and after treatment (p>0.05). Moreover, there were no statistically significant differences between the mean Dimeglio and Pirani scores before and after treatment for patients who had a family history of the disease and those who did not (p>0.05) (Table 3).
| Gender | N | Mean | Std. Dev. | p | |
| Pirani Score before the treatmeant (Right) | Female | 12 | 3.58 | 0.6 | 0.874 |
| Male | 38 | 3.55 | 0.58 | ||
| Pirani Score before the treatmeant (Left) | Female | 12 | 3.83 | 0.58 | 0.322 |
| Male | 30 | 3.63 | 0.59 | ||
| Pirani Score after the treatment (Right) | Female | 12 | 0.5 | 0.52 | 0.17 |
| Male | 38 | 0.3 | 0.39 | ||
| Pirani Score after the treatment (Left) | Female | 12 | 0.38 | 0.43 | 0.954 |
| Male | 30 | 0.37 | 0.41 | ||
| Dimeglio Score before the treatmeant (Right) | Female | 12 | 14.83 | 1.64 | 0.466 |
| Male | 38 | 14.46 | 1.5 | ||
| Dimeglio Score before the treatmeant (Left) | Female | 12 | 15.5 | 1.62 | 0.192 |
| Male | 30 | 14.79 | 1.52 | ||
| Dimeglio Score after the treatment (Right) | Female | 12 | 5.08 | 1.24 | 0.163 |
| Male | 38 | 4.64 | 0.84 | ||
| Dimeglio Score after the treatment (Left) | Female | 12 | 4.75 | 0.87 | 0.885 |
| Male | 30 | 4.79 | 0.86 |
At the follow-up examinations, 25 feet (27%) from 17 patients (28%) required intervention in addition to the percutaneous achillotenotomy because of relapse. Of these patients requiring additional interventions, 12 feet from 8 patients had a posteromedial release, 8 feet from 5 patients had a complete subtalar release, and 5 feet from 4 patients had an anterior tibial tendon transfer.
DISCUSSION
Comparing the results in males and females, right and left feet, and the presence or absence of family history revealed no significant differences. However, the results showed males had better improvements after treatment. Although left feet had higher Pirani and Dimeglio scores before the treatment, left feet in females and right feet in males showed better improvements after treatment. Left feet had higher Pirani and Dimeglio scores in patients with and without a family history of TEV. Left feet had better improvements in the group without a family history, whereas right feet had better improvements in the patients with a family history. Although many studies investigate the outcomes of clubfoot, none reveals differences according to gender, side, or family history. Likewise, this study found no statistical differences. However, the homogeneous distribution according to side in females and higher scores and improvements of the left foot should be investigated by other studies including larger case studies.
Although Ponseti recommended initiating treatment in the first days of life due to the properties of fibroelastic connective tissue in the structure of tendons, ligaments, and joint capsules, Iltar and colleagues propose initiating treatment one month after birth or when the length of the involved foot is 8 cm or more [9]. A study by Alves and colleagues investigates the initiation of treatment with the Ponseti method before and after patients are six months old and finds no significant difference in the correction rates, number of casts, recurrence rates, and the need for tenotomy or other surgical interventions [10]. In another study, Yagmurlu et al., show that initiating the Ponseti treatment after 20 months results in less improvement of varus, adductus, and medial rotation of the calcaneopedal block [11]. Through our clinical experience, we find that early initiation and continuous treatment and observation results in higher correction rates. We therefore recommend that specialists such as radiologists, gynecologists, and pediatricians should be informed about the importance of early treatment in order to correct the deformity. They should be proactive in referring patients to orthopedists in the first day of a patient’s life, if possible, despite the finding that the Ponseti method produces good results in neglected patients as well [12].
Family members are commonly asked to soften a patient’s cast by soaking it or to remove the cast at home in order to shorten the time between new casts. Lafargue and Morcuende show a significant preference for removing the cast at the clinic rather than removing the cast the previous night at home. Accordingly, removing the cast at the clinic reduces the number of casts required for correction, the duration of correction, and the number of recurrences [13]. We strongly suggest that an old cast should be removed at the clinic just before the new one is applied to limit the amount of time that the foot is not held in a manipulated position.
Although the Ponseti method prescribes weekly casting intervals, some authors, including Ponseti himself, report that two or three castings per week have the same efficiency as weekly castings [14-16]. In addition, two or three castings a week can be safely applied to patients who live nearby or to patients whose families travel from long distances and stay near the clinic or hospital during treatment.
Achillotenotomy is the only part of the Ponseti method that involves surgical intervention. Before achillotenotomy, all deformities except equinus must be corrected. Percutaneous achillotenotomy is a minor intervention compared to other major surgical techniques. Several achillotenotomy techniques are described in medical literature. Dogan et al., compares percutaneous achillotenotomy and lengthening with Z-plasty in rats and finds no biomechanical difference [17]. Many surgeons prefer to perform a tenotomy under local anesthesia to avoid possible adverse effects of general anesthesia. However, a retrospective study by Prada et al., reports no apnea or general anesthesia-related complications in a series of tenotomies for 182 patients [18]. The most important complication of percutaneous achillotenotomy is neurovascular injuries. Dobbs et al., reports 2% of 200 patients had serious bleeding complications, which were all controlled with compression only [19]. Throughout our clinical experience performing the procedure, we have not encountered cases where patients suffered neurovascular injuries or complications related to anesthesia. It is our opinion that an achillotenotomy should be performed (under general or local anesthesia) as soon as possible when plantar convexity of the foot is first achieved.
The use of orthosis after surgical correction has an important role in the Ponseti technique. The rate of success decreases without the proper use of orthosis [20-21]. In addition, using the appropriate orthosis is equally as important. A study comparing a Denis Brown orthosis with an ankle foot orthosis reveals that patients wearing the Denis Brown orthosis have significantly fewer recurrences [22]. However, Hemo et al., find no significant difference between Denis Brown and Mitchell braces after a minimum two-year follow-up period [23]. Furthermore, there is no scientific proof about the timing of ending the use of orthoses. They can be used three years for patients with a mild deformity or four years for patients with a severe deformity.
If a deformity recurs, the patient’s foot should be placed in a cast as soon as possible because the deformity has not yet been treated. Although a number of studies support the finding that surgical treatments have good results after recurrences [24-26], the Ponseti method should be tried before surgery to avoid fibrosis, scar tissue, and possible anesthetic complications. The success rate of the Ponseti method has been corroborated after recurrences of the deformities. This is the case even if the primary treatment technique was the Ponseti method itself. Nagaraju report that when treating 18 feet from 13 patients via the Ponseti method, they achieve well-formed plantigrade feet where previously they had used the Kite method and experienced recurrences of the disease [27]. Nogueira reports that for patients who had unsuccessful surgical treatments, 71 out of 83 feet (86%) were corrected with the Ponseti method and the patients developed plantigrade, fully corrected feet [28]. Recurrences of the deformity are characterized as metatarsus adductus, abduction of foot, loss of dorsiflexion, and dynamic supination, which appears during gait analysis when the patient is walking. Dynamic supination is due to weakness in the peroneal muscles and overcontraction compensation by the tibialis anterior muscle.
CONCLUSION
The literature so far clearly points to the Ponseti method as being the gold standard in clubfoot treatment [29]. We therefore feel that the efficacy of new methodologies should be compared with the Ponseti method in order to evaluate their benefit.
REFERENCES
- Carroll NC (2012) Clubfoot in the twentieth century: where we were and where we may be going in the twenty-first century. J Pediatr Orthop B 21: 1-6.
- Parker SE, Mai CT, Strickland MJ, Olney RS, Rickard R, et al. (2009) Multistate study of the epidemiology of clubfoot. Birth Defects Res A Clin Mol Teratol 85: 897-904.
- Diméglio A, Bensahel H, Souchet P, Mazeau P, Bonnet F (1995) Classification of clubfoot. J Pediatr Orthop B 4: 129-136.
- Pirani S, Outerbridge H, Moran M, et al (1995) A method of evaluating the virgin clubfoot with substantial inter-observer reliability. POSNA, Miami, Florida, USA.
- Laaveg SJ, Ponseti IV (1980) Long-term results of treatment of congenital clubfoot. J Bone Joint Surg Am 62: 23-31.
- Morcuende JA, Dolan LA, Dietz FR, Ponseti IV (2004) Radical reduction in the rate of extensive corrective surgery for clubfoot using the Ponseti method. Pediatrics 113: 376-380.
- Colburn M, Williams M (2003) Evaluation of the treatment of idiopathic clubfoot by using the Ponseti method. J Foot Ankle Surg 42: 259-267.
- Abdelgawad AA, Lehman WB, van Bosse HJ, Scher DM, Sala DA (2007) Treatment of idiopathic clubfoot using the Ponseti method: minimum 2-year follow-up. J Pediatr Orthop B 16: 98-105.
- Iltar S, Uysal M, Alemdaro?lu KB, Aydo?an NH, Kara T, et al. (2010) Treatment of clubfoot with the Ponseti method: should we begin casting in the newborn period or later? J Foot Ankle Surg 49: 426-431.
- Alves C, Escalda C, Fernandes P, Tavares D, Neves MC (2009) Ponseti method: does age at the beginning of treatment make a difference? Clin Orthop Relat Res 467: 1271-1277.
- Yagmurlu MF, Ermis MN, Akdeniz HE, Kesin E, Karakas ES (2011) Ponseti management of clubfoot after walking age. Pediatr Int 53: 85-89.
- Verma A, Mehtani A, Sural S, Maini L, Gautam VK, et al. (2012) Management of idiopathic clubfoot in toddlers by Ponseti’s method. J Pediatr Orthop B 21: 79-84.
- Terrazas-Lafargue G, Morcuende JA (2007) Effect of cast removal timing in the correction of idiopathic clubfoot by the Ponseti method. Iowa Orthop J 27: 24-27.
- Morcuende JA, Abbasi D, Dolan LA, Ponseti IV (2005) Results of an accelerated Ponseti protocol for clubfoot. J Pediatr Orthop 25: 623-626.
- Xu RJ (2011) A modified Ponseti method for the treatment of idiopathic clubfoot: a preliminary report. J Pediatr Orthop 31: 317-319.
- Harnett P, Freeman R, Harrison WJ, Brown LC, Beckles V (2011) An accelerated Ponseti versus the standard Ponseti method: a prospective randomised controlled trial. J Bone Joint Surg Br 93: 404-408.
- Dogan A, Korkmaz B, Cengiz N, Kalender AM, Gokalp MA (2009) Biomechanical comparison of Achilles tenotomy and achilloplasty techniques in young rats: An experimental study. J Am Podiatr Med Assoc 99: 216-222.
- Parada SA, Baird GO, Auffant RA, Tompkins BJ, Caskey PM (2009) Safety of percutaneous tendoachilles tenotomy performed under general anesthesia on infants with idiopathic clubfoot. J Pediatr Orthop 29: 916-919.
- Dobbs MB, Gordon JE, Walton T, Schoenecker PL (2004) Bleeding complications following percutaneous tendoachilles tenotomy in the treatment of clubfoot deformity. J Pediatr Orthop 24: 353-357.
- Dobbs MB, Rudzki JR, Purcell DB, Walton T, Porter KR, et al. (2004) Factors predictive of outcome after use of the Ponseti method for the treatment of idiopathic clubfeet. J Bone Joint Surg Am 86: 22-27.
- Thacker MM, Scher DM, Sala DA, van Bosse HJ, Feldman DS, et al. (2005) Use of the foot abduction orthosis following Ponseti casts: is it essential? J Pediatr Orthop 25: 225-228.
- Janicki JA, Wright JG, Weir S, Narayanan UG (2011) A comparison of ankle foot orthoses with foot abduction orthoses to prevent recurrence following correction of idiopathic clubfoot by the Ponseti method. J Bone Joint Surg Br 93: 700-704.
- Hemo Y, Segev E, Yavor A, Ovadia D, Wientroud S, et al. (2011) The influence of brace type on the success rate of the Ponseti treatment protocol for idiopathic clubfoot. J Child Orthop 5: 115-119.
- El-Mowafi H, El-Alfy B, Refai M (2009) Functional outcome of salvage of residual and recurrent deformities of clubfoot with Ilizarov technique. Foot Ankle Surg 15: 3-6.
- Ferreira RC, Costa MT (2009) Recurrent clubfoot-approach and treatment with external fixation. Foot Ankle Clin 14: 435-445.
- Park SS, Kim SW, Jung BS, Lee HS, Kim JS (2009) Selective soft-tissue release for recurrent or residual deformity after conservative treatment of idiopathic clubfoot. J Bone Joint Surg Br 91: 1526-1530.
- Nagaraju KD, Vidyadhara S, Shetty AP, Venkatadass K, Rajasekaran S (2008) Use of Ponseti’s technique in recurrent clubfeet following Kite’s method of correction. J Pediatr Orthop B 17:189-193.
- Nogueira MP, Ey Batlle AM, Alves CG (2009) Is it possible to treat recurrent clubfoot with the Ponseti technique after posteromedial release?: a preliminary study. Clin Orthop Relat Res 467: 1298-1305.
- Emrah Say?t, Vedat Uruç (2014) The Treatment of Clubfoot with the Ponseti Method: A Systematic Review. J Clin Anal Med.
Citation: Sayit E, Sayit AT (2015) Clinical Experiences and Midterm Results of the Treatment of Clubfoot with the Ponseti Method. J Orthop Res Physiother 1: 004.
Copyright: © 2015 Emrah sayit, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

