
Dual Mobility Acetabular - Cup Total Hip Arthroplasty after Femoral Neck Fracture in the Elderly: Prospective Study on Risks of Early Dislocation in 80 Total Hip Replacements
*Corresponding Author(s):
K LahrachDepartment Of Trauma And Orthopedic Surgery A, Hassan II Teaching Hospital, Faculty Of Medicine And Pharmacy, Sidi Mohammed Ben Abdellah University, Fes, Morocco
Email:k.lahrach@hotmail.com
Abstract
ackground
Total Hip Arthroplasty (THA) for femoral neck fractures in the elderly is still lauded as one of the most successful surgeries of the century with good short and medium term outcomes. Postoperative dislocation remains the mainset back of hip replacement in the elderly. This study mainly sees keto assess early outcomes of total hiparthroplasty using dual mobility acetabular cup for femoral neckfractures in the elderly with emphasis on dislocation.
Patients and Methods
We carried out 80 consecutive total hip replacements using a double articulating acetabular component. We assessed dislocation rates after 6 months and cumulative risks in the years following replacement.
Results
After a mean follow-up of 50 months, only 8 (10%) deaths were recorded. We observed 1 case of dislocation at 4 months postoperatively that required revision arthroplasty. No case of instability was recorded.
Conclusion
Dual mobility acetabular cups remain suitable implants in the face of postoperative dislocation after total hip replacement for femoral neck fractures in the elderly.
Keywords
INTRODUCTION
Patients and methods
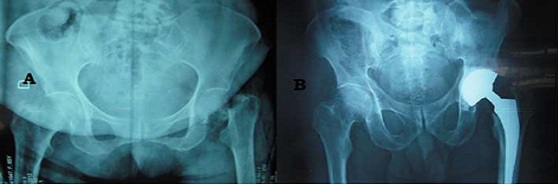
Figure 1: (A) preoperative X-ray showing a displaced femoral neck fracture in a 65 year old woman who underwent hybrid total hip arthroplasty using dual mobility cemented cup (B).
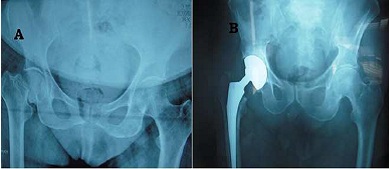
We included in this case series all patients who underwent primary THA for femoral neck fractures aged above 55 years. Thus we excluded all cases of neglected femoral neck fractures and cases associated with femoral shaft fractures.
54 women and 26 men, aged between 60 and 90 years with right side femoral neck fractures in 65% of cases were involved. 79% of the patients were autonomous with aided ambulation prior to injury. Parker score averaged 5/9. Average time between fracture and surgery was 3 days.
THA was done mostly under spinal anesthesia (n = 70 87.5%) with patient in a lateral decubitus position using a modified posterolateral Moore (Southern) approach in all cases.Dual mobility THA applying Charnley’s low friction torque principle using a 28 mm diameter head that articulates against polyethylene to decrease wear with a secondary larger diameter articulation between polyethylene liner and metal shell of acetabular component further enhancing implant stability (Figure 3 and 4) was carried out. Acetabular component was cemented in 75% of the cases.

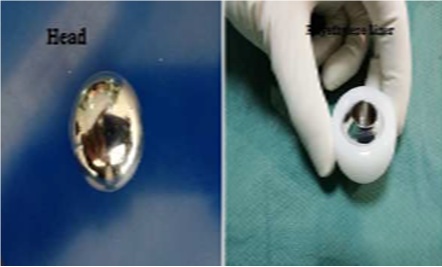
Rehabilitation was commenced after the first postoperative day withfull weight bearing and braced ambulation. Patients were discharged on the third postoperative day with leaflets explaining prohibited maneuvers and physical therapy protocol.
Follow-up was carried out monthly up to 6 months and twice yearly afterwards with routine x-rays and physical exams. The Merle d'Aubigné and Postel hip score was used to assess outcomes after THA. We also assessed cumulative risks of dislocations in the years following replacement.
RESULTS
|
Number of Patients |
Indications of THA |
Femoral Head size |
Acetabular component tilt |
Anteversion |
Cemented |
|
80 |
Femoral neck fractures |
28mm |
40 ± 5° |
15 ± 5° |
60 |
After a mean follow-up of 50 months (between 12 and 65 months), we observed a single case of dislocation at 4 months postoperatively, following a fall that required open reduction (Figure 5). A single case of deep venous thrombosis of the lower limb was managed with heparin with favorable outcome. We recorded 8 (10%) deaths on the last follow-up. 5 cases were due to acute kidney failure, 3 due to congestive heart disease. No case of instability or atraumatic dislocation wasreported. No cases of acetabular or femoral implant loosening have been reported on postoperative radiography during this period.The Merle d’Aubigné and Postel score averaged 15.8 versus 7.2 preoperatively.
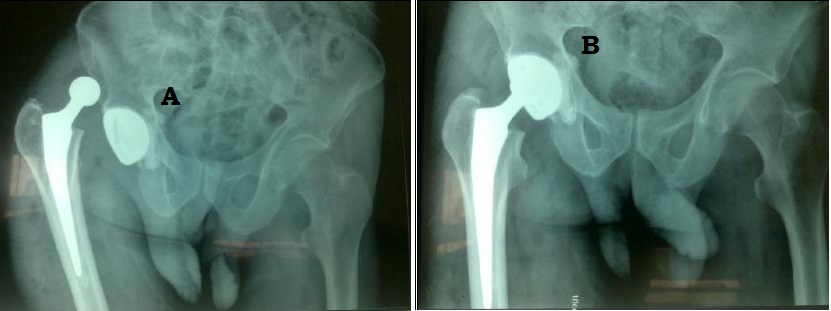
DISCUSSION
Choice of implant in primary hip replacement for femoral neck fractures remains a popular source of debate among orthopedic surgeons. Many often divided along the lines of either partial or total arthroplasty in what is a population with low life expectancy. Factors that may affect the stability after THA include surgical approach, patient-related factors like neurological disorders component orientation and geometry, and more particularly, head diameter and head-neck ratio [3].The use of low friction torque and dual mobility cups has gained popularity recently under several designations and descriptions including “unconstrained tripolar cups” and “mobile bearing cups” by manufacturers [4,5].
In our study postoperative mortality at 3 months was similar to rates reported by similar prospective studies of femoral neck fractures in the elderly. Skinner, et al., [6] observed that mortality rate was identical between partial and total arthroplasty for displaced femoral neck fractures in the elderly. Nonetheless some authors have reported dislocation rates up to 4 times higher in hemiarthroplasty after femoral neck fractures [7].
Dislocation rates following primary THA is estimated at 2.2% after one year, 3.8% at ten years, reaching up to 6% after 20 years [8]. A meta-analysis [9] observed an average dislocation rate of 10.7%, five times higher than primary replacement for degenerative osteoarthritis.Althoughcerebral palsy, Parkinson’s disease, poliomyelitis and history of cerebrovascular accident, spinal injury or Charcot arthropathy are risk factors for instability,early dislocation is directly linked to surgical approach and component positioning. Popular theory suggests a decrease in muscle control associated with ligamentous laxity following femoral neck fracturesin elderly patients [10]. Dual mobility cups have gained more interestin primary replacement for femoral neck fractures and revision arthroplasty as they exhibit less wear, restore near normal range of motion with increased implant stability [11, 12].
The concept of dual mobility was developed initially by Bousquet in the late 1970s. Its main purpose was to prevent dislocation by combining two articulating systems, one with a large diameter, between a metal cup and a polyethylene liner, and the other with a small diameter between the femoral head and its retentive insert. Generally, as rule of thumb the use of large diameter femoral head could address the problem of instability and mechanical studies have exhibited low dislocation rates with 28 mm femoral head components [13-15].This concept does not exhibit complications pertaining to simple implant retention, which solicits attachment through bony press fit, with less wear as the larger joint allowed additional range of motion during dislocation manoeuvers. Pituckanotai, et al., [16] in a recent network meta-analysis recommend dual mobility and big head as safer implants in THA with less risk of dislocation and revision.
Studies assessing survivorship of dual-articulation acetabular cup systems have reported good long-term results. The main drawback of hybrid primary THA remains aseptic loosening [17]. Tripolar prosthesis with a mobile cup and large-diameter heads are also deemed a reliable solution in highly unstable hips though the thickness of the polyethylene cup presents a considerable limitation which may affect long-term outcome due to a higher risk of wear [18]. A study by Tarasevicius [19] involving 42 patients who underwent dual mobility THA did not report any case of postoperative dislocation.
CONCLUSION
LIST OF ABBREVIATIONS
DECLARATIONS
Ethics approval and consent to participate
Consent to publish
Availability of data and materials
Competing interests
Funding
Author’s Contributions
REFERENCES
- Berry DJ, von Knoch M, Schleck CD, Harmsen WS (2004) The cumulative long-term risk of dislocation after primary Charnley total hip arthroplasty. J Bone Joint Surg Am 86: 9-14.
- Marottoli RA, Berkman LF, Cooney LM (1992) Decline in physical function following hip fracture. J Am Geriatr Soc 40: 861-866.
- Philippot R, Camilleri JP, Boyer B, Adam P, Farizon F (2009) The use of a dual-articulation acetabular cup system to prevent dislocation after primary total hip arthroplasty: Analysis of 384 cases at a mean follow-up of 15 years. Int Orthop 33: 927-932.
- Roberts KC, Brox WT, Jevsevar DS, Sevarino K (2015) Management of hip fractures in the elderly. J Am Acad Orthop Surg 23: 131-137.
- Guyen O, Chen QS, Bejui-Hugues J, Berry DJ, An KN (2007) Unconstrained tripolar hip implants: effect on hip stability. Clin Orthop Relat Res 455: 202-208.
- Skinner P, Riley D, Ellery J, Beaumont A, Coumine R, et al. (1989) Displaced subcapital fractures of the femur: A prospective randomized comparison of internal fixation, hemiarthroplasty and total hip replacement. Injury 20: 291-293.
- Gjertsen JE, Vinje T, Lie SA, Engesaeter LB, Havelin LI, et al. (2008) Patient satisfaction, pain, and quality of life 4 months after displaced femoral neck fractures: A comparison of 663 fractures treated with internal fixation and 906 with bipolar hemiarthroplasty reported to the Norwegian Hip Fracture Register. Acta Orthop 79: 594-601.
- Berry DJ, Vonknoch M, Schleck CD, Harmsen WS (2005) Effect of femoral head diameter and operative approach on risk of dislocation after primary total hip arthroplasty. J Bone Joint Surg Am 87: 2456-2463.
- Iorio R, Healy WL, Lemos DW, Appleby D, Lucchesi CA, et al (2001) Displaced femoral neck fractures in the elderly: outcomes and cost effectiveness. Clin Orthop Relat Res 383: 229-242.
- Hudson JI, Kenzora JE, Hebel JR, Gardner JF, Scherlis L, et al. (1998) Eight- year outcome associated with clinical options in the management of femoral neck fractures. Clin Orthop Relat Res 348: 59-66.
- Lebeau N, Bayle M, Belhaouane R, Chelli M, Havet E, et al. (2017) Total hip arthroplasty revision by dual-mobility acetabular cup cemented in a metal reinforcement: A 62 case series at a minimum 5 years' follow-up. Orthop Traumatol Surg Res 103: 679-684.
- Darrith B, Courtney PM, Della Valle CJ (2018) Outcomes of dual mobility components in total hip arthroplasty: A systematic review of the literature. Bone Joint J 100: 11-19.
- Lombardi AV Jr, Skeels MD, Berend KR, Adams JB, Franchi OJ (2011) Do large heads enhance stability and restore native anatomy in primary total hip arthroplasty? Clin Orthop Relat Res 469: 1547-1553.
- Pedersen DR, Callaghan JJ, Johnston TL, Fetzer GB, Johnston RC (2001) Comparison of femoral head penetration rates between cementless acetabular components with 22-mm and 28-mm heads. J Arthroplasty 16: 111-115.
- Kelley SS, Lachiewicz PF, Hickman JM, Paterno SM (1998) Relationship of femoral head and acetabular size to the prevalence of dislocation. Clin Orthop Relat Res 355: 163-70.
- Pituckanotai K, Arirachakaran A, Tuchinda H, Putananon C, Kongtharvonskul J, et al. (2018) Risk of revision and dislocation in single, dual mobility and large femoral head total hip arthroplasty: systematic review and network meta-analysis. Eur J Orthop Surg Traumatol 28: 445-455.
- Aubriot JH, Lesimple P, Leclercq S (1993) Study of Bousquet’s non-cemented acetabular implant in 100 hybrid total hip prostheses (Charnley type cemented femoral component). Average 5-year follow-up. Acta Orthop Belg 59: 267-271.
- Beaule PE, Roussignol X, Schmalzried TP, Udomkiat P, Amstutz HC, et al. (2003) Tripolararthroplasty for recurrent total hip prosthesis dislocation. Rev Chir Orthop Reparatrice Appar Mot 89: 242-249.
- Tarasevicius S, Busevicius M, Robertsson O, Wingstrand H (2010) Dual mobility cup reduces dislocation rate after arthroplasty for femoral neck fracture. BMC Musculoskelet Disord 11: 175.
Citation: Lahrach K, Abdulrazak S, Marzouki A, Boutayeb F (2019) Dual Mobility Acetabular - Cup Total Hip Arthroplasty after Femoral Neck Fracture in the Elderly: Prospective Study on Risks of Early Dislocation in 80 Total Hip Replacements. J Orthop Res Physiother 5: 041.
Copyright: © 2019 K Lahrach, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

