Screening for Anaemia at Different Phases of the Menstrual Cycle among Female Students in a Nigerian University
*Corresponding Author(s):
Moses D LugosDepartment Of Medical Laboratory Science, Faculty Of Health Sciences & Technology, College Of Health Sciences, University Of Jos, Nigeria
Tel:+234 8034869343,
Email:LugosM@UniJos.Edu.Ng, mlugos2003@yahoo.com
Abstract
Background
Menstrual cycle is the periodic physiological bleeding that characterises much of a woman’s reproductive life. It is hypothesized that this blood loss could predispose women to anemia.
Aim
Therefore, this study was designed to employ haematocrit values to assess for anemia in women within reproductive age at different phases of the menstrual cycle.
Materials and Methods
Fifty-one (51) apparently healthy, regularly menstruating female students of the University of Jos, Nigeria between the ages of 19-30 years were followed up in a single cycle. We determined the haematocrit values of the study subjects using the micro haematocrit method during the pre-menstrual, menstrual and post-menstrual phases of the menstrual cycle. Variations in Haematocrit (Hct) values at the different phases of the menstrual cycle were analyzed using paired student t-test.
Results
The average haematocrit value at pre-menstrual phase was 40.04 ± 1.89 (%), the menstrual was 37.40 ± 3.25 (%) and the postmenstrual was 39.70 ± 2.18 (%). The decrease in the mean haematocrit value observed at the menstrual phase when compared to the average values reported at premenstrual and postmenstrualphases was shown to be statistically significant (P < 0.005).
Conclusion
The data revealed that menstrual bleeding could be responsible for the decreased in the haematocrit values of the study participants.
Clinical significance
Although the decrease in haematocrit values may not necessarily lead to an anaemic state, it is important to maintain a regular check on this parameter to avoid eventual onset of anemia in menstruating women as a result of blood loss.
Keywords
INTRODUCTION
The average length of the menstrual cycle is 28 days although a variation of between 21-40 days is normal [4]. Some factors, including age, weight, diet, amount of physical activity, level of stress and genetics have been identified to affect the cycle and the amount of blood loss. The length of the menstrual cycle is counted from the first day of menstrual bleeding until the day of the next menstrual bleeding [3].
Menstrual bleeding could be heavy or light. Blood loss in menstruation ranges from 30-80ml [5]. The blood loss during menstruation results in a negative iron load in women and increases the risk for developing iron-deficiency anemia [1,6]. Anemia in adolescent girls has been shown to contribute to maternal and foetal mortality and morbidity later in life [7].This makes the measurement of Packed Cell Volume (PCV) across the menstrual cycle very important. Packed cell volume is also known as haematocrit. It is the percentage of total volume of whole blood occupied by packed red blood cells when a known volume of blood is centrifuged ata constant speed for a constant period [8]. The measurement of PCV is used as a screening test for anemia which could be as a result of blood loss or other underlying disorders [9].
This study, therefore, seeks to measure the haematocrit values of apparently healthy volunteer female students attending University of Jos who have a regular menstrual cycle, at different phases of the menstrual cycle; the pre-menstrual, menstrual and post-menstrual phase. This study aimed at assessing for anemia at the different phases of the menstrual cycle and show whether or not menstruation could be a predisposing factor to anemia in females.
MATERIALS AND METHODS
Study area/Population
Sampling/Study consent
Ethical clearance
Inclusion and exclusion criteria
Blood sample collection/Experimental design
All the samples were taken between 11:00 am - 12:00 noon to avoid diurnal variation and for consistency. Also, the samples were analysed immediately after collection to avoid any variations due to storage.
Laboratory methodology
Data analysis/Statistical methods
RESULTS
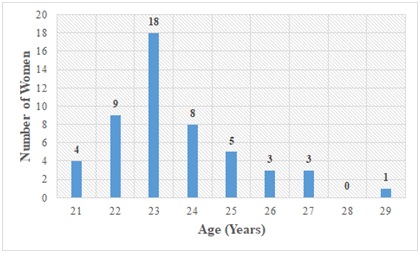
Figure 1: Distribution of study participants by age.
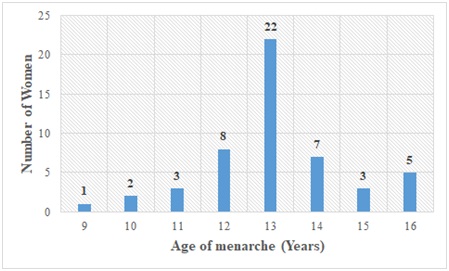
Figure 2: Distribution of study participants according to age of menarche (A.O.M) in years.
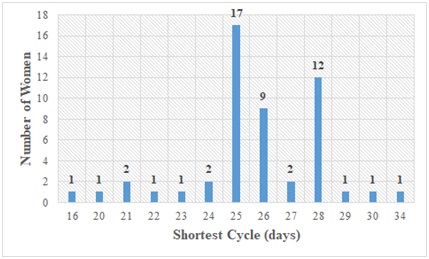
Figure 3: Outlook of study participants according to the shortest cycle (S.C) in days.
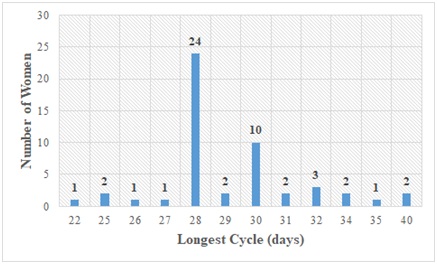
Figure 4: The spread of study participants according to longest cycle (L.C) in days.
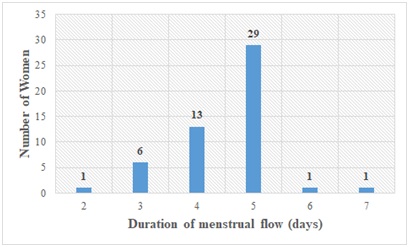
Figure 5: Distribution of study participants according to duration of menstrual flow (D.M.F) in days.
Table 1 shows the mean and standard deviation of haematocrit values of study subjects at the premenstrual (40.04 ± 1.89), menstrual (37.40 ± 3.25) and postmenstrual (39.70 ± 2.18) phases of the menstrual cycle. Significant rise in haematocrit values were recorded in the premenstrual and postmenstrual phases of menstrual cycle when compared to the menstrual phase (p = 0.0001). However, the difference seen between the premenstrual and postmenstrual PCV values was not significant (p = 0.4070).
|
The Phase of Menstrual cycle |
Mean ± SD |
T-test value |
P-value |
|
Pre-menstrual |
40.04 ± 1.89 |
4.9677 |
0.0001 |
|
Menstrual |
37.40 ± 3.25 |
4.3664 |
0.0001 |
|
Post-menstrual |
39.7 ± 2.18 |
0.8327 |
0.407 |
DISCUSSION
Most ladies who participated were 23 years of age. The length of the menstrual cycle of majority of the subjects ranged from 25-30 days. The duration of menstrual flow of majority of the study subjects ranged between 3-5 days with 5 days having the highest frequency of 29 occurrences.
From the menstrual history of each subject recorded, abnormal patterns were not seen in the menstrual bleeding phase. The age of menarche recorded had majority having menarcheal age of 12 years and above. Earlier studies by Kulkarni et al., reported that there is no association between status of menarche, menarcheal age and anemia [7]. These findings are supported in this study as subjects showed similar menstrual patterns irrespective of their age of menarche.
The menstrual, postmenstrual and premenstrual PCV values were also estimated for each subject. The mean pre-menstrual PCV (%) was found to be 40.04, menstrual 37.40 and post menstrual was 39.7. The T-test values of premenstrual and menstrual PCV was 4.9677 which gave a P value that was statistically significant (P = 0.0001). Likewise, the menstrual and post menstrual T-test value (4.3664) also gave a P value which was statistically significant (P = 0.0001). The postmenstrual and premenstrual T-test value (0.8327) however, did not give a statistically significant P value (0.4070). The significance in p values obtained reflects that menstrual bleeding indeed could be a predisposing factor to anemia in females supporting our earlier hypothesis.
This study focused on apparently healthy unmarried young ladies with no abnormal menstrual bleeding. Hence, any decrease in haematocrit value seen was due to the physiologic condition being experienced. We however, did not estimate the blood loss for each study participant and interaction of factors such as weight, body mass index, level of physical activity; stress and nutritional status were not studied. These findings are similar to findings by Malini K who reported a minimal rise in PCV in the proliferative (post menstrual) and secretory (pre-menstrual) phases when compared to the menstrual phase [12]. However, the rise in both phases in that study was not found to be statistically significant. Rajnee et al., also reported a non-significant difference in the hemoglobin concentration and haematocrit during the menstruation and follicular phase of the menstrual cycle [13]. Our findings however proved to be statistically significant. This might be as a result of the narrow age group we considered and also the health status of our study subjects.
In this study, the blood loss was not estimated. However, the loss was sufficient enough to cause a significant decrease in haematocrit which was shown to be statistically significant when compared to the pre-menstrual and post menstrual haematocrit values. This decrease however, cannot be interpreted in isolation without putting into consideration the mean PCV of the menstrual phase. The mean PCV was found to be 37.4%. This value when compared to the normal range of PCV for females 37-47% is not alarming despite the statistical significance of the decrease [14,15].
Further studies could be carried out in order to find out why women have symptoms of anemia such as dizziness during the menstrual bleeding phase since the PCV does not qualify them to be anemic. In order to reduce the discomfort caused by the physical changes experienced during menses, women should ensure they take on a healthy diet; reduce the consumption of salt, caffeine and alcohol and also ensure regular exercise [16].
The menstrual bleeding phase of the menstrual cycle can lead to a decrease in haematocrit value. This is due to the blood loss during this phase. However, menstruation does not lead to anemia among healthy regularly menstruating females.
REFERENCES
- Fatima S, Kamal RB, Bajpai M, Gupta P, Chawla K (2017) Variation of Haemoglobin level during Follicular and Luteal Phases of menstrual cycle. IJAR 3: 973-975.
- Guyton AC (1991) Female physiology before pregnancy and the female hormones. Textbook of medical physiology, Saunders, USA, Pg No: 899-914.
- Mtawali G, Pina M, Angle M, Murphy C (1997) The menstrual cycle and its relation to contraceptive methods: A reference for reproductive health trainers. INTRAH, USA, Pg No: 1-90.
- Xiao S, Coppeta JR, Rogers HB, Isenberg BC, Zhu J, et al. (2017) A microfluidic culture model of the human reproductive tract and 28-day menstrual cycle. Nat Commun 8: 14584.
- Kim I, Yetley EA, Calvo MS (1993) Variations in iron-status measures during the menstrual cycle. Am J Clin Nutr 58: 705-709.
- Javaid A, Hasan R, Naim T (2007) A Comparative Study of Body Weight, Hemoglobin Concentration and Hematocrit During Follicular and Luteal Phases of Menstrual Cycle. J Med Sci 7: 146-149.
- Kulkarni MV, Durge P, Kasturwar N (2012) Prevalence of anemia among adolescent girls in an urban slum. Natl J Community Med 3: 108-111.
- Sa'adu B (2013) Effect of Water Restriction and Ascorbic Acid Supplimentation on Rectal Temperature, Body Weight and Hematological Indices in Japanese Quails in Sokoto, NIGERIA. UDUS-OER, Nigeria.
- Fortney S, Beckett WS, Carpenter AJ, Davis J, Drew H, et al. (1988) Changes in plasma volume during bed rest: effects of menstrual cycle and estrogen administration. J Appl Physiol 65: 525-533.
- Petersson K, Jakobssona O, Ohlssona P, Augustssona P, Scheding S, et al. (2018) Acoustofluidic hematocrit determination. Analytica chimica acta 1000: 199-204.
- Silotry N, Kumari NH, Kumari R (2011) A comparision of haemoglobin levels in women with and without premenstrual syndrome during premenstrual, menstrual and postmenstrual stages. International Journal of Biological & Medical Research 2: 1017-1022.
- Malini K (2006) Haematological Profile in Different Phases Of Menstrual Cycle. Rajiv Gandhi University of Health Sciences, India.
- Rajnee, Chawla VK, Choudhary R, Binawara BK, Choudhary S (2010) Haematological and electrocardiographic variations during menstrual cycle. Pak J Physiol 6: 18-21.
- Akinbami AA, Ajibola SO, Rabiu KA, Adewunmi AA, Dosunmu AO, et al. (2013) Hematological profile of normal pregnant women in Lagos, Nigeria. Int J Womens Health 5: 227-232.
- Kueviakoe IM, Segbena AY, Jouault H, Vovor A, Imbert M (2011) Hematological reference values for healthy adults in Togo. ISRN hematology, Article ID: 736062.
- Price WA, Giannini AJ (1983) Binge eating during menstruation. J Clin Psychiatry 44: 431.
Citation: Lugos MD, Vwamdem NI, Polit UY, Ofojekwu MJN, Damen JG (2019) Screening for Anaemia at Different Phases of the Menstrual Cycle among Female Students in a Nigerian University. J Hematol Blood Transfus Disord 6: 022.
Copyright: © 2019 Moses D Lugos, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.