
Superficial Acral Fibromyxoma: A Case Report of an Uncommon Tumor of the Foot
*Corresponding Author(s):
Santiago PacheInstituto Nacional De Ortopedia Y Traumatologia Inot, Universidad De La República (UdelaR), 3326, Av. Luis A. De Herrera, Montevideo 11600, Uruguay
Email:santiagopache@hotmail.com
Abstract
This study presents a case report of a 52-year-old female patient with a Superficial Acral Fibromyxoma (SAF) of her left foot fifth toe. This is a very uncommon soft tissue tumor that affects mainly hands and feet, with a special predilection fortoes, with the hallux most frequent. The tumor in this case was 3cm long and 2.5cm wide, which was unusually large. Few cases are larger than 2 cm long and localized on the fifth toe. The treatment was wide resection of the tumor through amputation of the fifth toe.
Keywords
INTRODUCTION
CASE REPORT
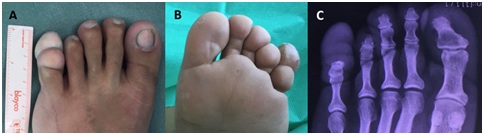
Figure 1: A) Dorsal view; B) Plantar view. A 3.5cm lobulated tumor that disrupt and eliminates the nail architecture can be observed; C) Dorsal view x-ray. A soft tissue mass can be observed distal to the distal phalanx of the fifth toe that erodes its distal border.
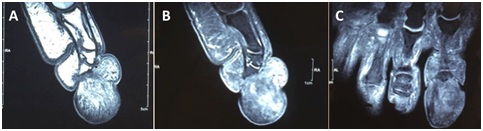
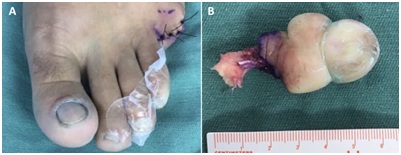
Figure 3: A) Trans-proximal phalanx amputation of the fifth toe; B) Resected tumor.
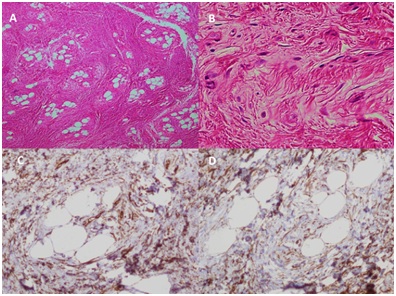
On the macroscopic analysis, a 30mm diameter mass, with dermis and subcutaneous tissue compromise was observed. On microscopic analysis, it featured benign mesenchymalcellproliferation with a multinodular morphology of expansive growth. Each of these foci shows a myxoid matrix with thin collagen fibers, stellate cells without atypia, and slight vascularization. A good surgical margin was obtained from the entire tissue resected (Figure 4A and 4B). The Immunohistochemistry (IHC) showed markedly positive reaction for CD34 and CD10 and negative for EMA. It also showed negative reaction for S100 Protein, Chromogranin, and Actin which ruled out Schwan cell tumor, glomus tumor, and a tumor of smooth muscle origin respectively (Figure 4C and 4D). The clinical findings, location, imaging studies, morphology and IHC profile, confirmed a superficial acral fibromyxoma.At 14 months of followup, she has no pain, no signs of relapse and good functional outcome.
DISCUSSION
On routine radiographs, SAF appears as a soft tissue mass with or without bone compromise. This could be scalloping or sclerosis of the underlying bone, which is present in more than 30% of cases [2]. In contrast, our case showed slight bone erosion at the distal aspect of the phalanx. However this finding probably results from chronic pressure over the underlying bone rather than from an aggressive biological behavior of the tumor [10]. On MRI, a hyperintense image could be observed on the T2 images. SAF typically appears as a solitary lesion growing mainly in dermal or subcutaneous tissue areas and less commonly reaching the deep fascia layer.
Histologically, it shows a spindle cell and stellate proliferation, enclosed in a myxoid or collagen matrix. Some regions may show a storiform pattern and blood vessels and stromal mast cells are often observed. Mitotic figures are usually sparse, averaging < 1 per 10 HPF [11]. SAF shows multinucleate cells in 50% of cases but with minimal nuclear atypia. Immunohistochemistry typically shows positive reaction to CD 34 in every case, while Epithelial Membrane Antigen (EMA) and CD99 are positive in many cases. S100 protein, Glial Fibrillary Acid Protein (GFAP), actin, desmin and keratin are typically negative in the SAF [2,3].
Given its rare appearance, SAF is often mistaken for other myxoid soft tissue tumors. The differential diagnoses can be classified into benign or malignant tumors. In the benign myxoid group, periungual fibroma and acquired digital fibrokeratoma are among the most common differential diagnoses.They typically extend into the dermis and have more cellularity on microscopy [12,13]. Neurofibroma can also be part of the differential diagnosis although it shows an S100 Protein expression. In the malignant myxoid group, Dermato Fibrosarcoma Protuberans (DFSP), Low-Grade Fibromyxoid Sarcoma (LGFMS) and myxo fibrosarcoma are the main differential diagnoses [14]. DFSP predominately presents on the trunk, with an extremely low incidence localized to the hands and feet, and it is negative for EMA [2]. The LGFMS has a more aggressive behavior and disorganized cell growth pattern than SAF. It affects deeper structures and acral localization is uncommon [14].
In his series of 37 patients with SAF, Fetsch described two cases with significantly more focal atypia and a low mitotic rate, which suggested that these cases might become low-grade malignant neoplasms, although there was no evidence of an aggressive progression of these two tumors [3]. In order to reduce the risk of recurrence, which is low, a wide margin at the resection site is recommended [3]. In the study by Holloman, the recurrence rate was 24% with an average followup of 27 months. However, there were no recurrences in those cases with a free margin at the resection [2].
We have a followup of this patient of 14 months with excellent clinical results. The clinical history and examination findings in this patient, together with the clear imaging studies, histology and IHC, provide a unique study of this rare soft tissue tumor. Localized to the fifth toe, and 3cm long x 2cm wide, this case was quite unusual in light of the less than 170 cases previously published in the literature.
CONCLUSION
REFERENCES
- Mine C, Support D (1982) Chapter 12. Quality (1969) 224-250.
- Hollmann TJ, Bovée JV, Fletcher CD (2012) Digital fibromyxoma (superficial acral fibromyxoma): A detailed characterization of 124 cases. Am J Surg Pathol 36: 789-798.
- Fetsch JF, Laskin WB, Miettinen M (2001) Superficial acral fibromyxoma: A clinicopathologic and immunohistochemical analysis of 37 cases of a distinctive soft tissue tumor with a predilection for the fingers and toes. Hum Pathol 32: 704-714.
- Al-Daraji WI, Miettinen M (2008) Superficial acral fibromyxoma: A clinicopathological analysis of 32 tumors including 4 in the heel. J Cutan Pathol 35: 1020-1026.
- Pinheiro M, Schettini A, Rodrigues C, Santos M (2017) Superficial Acral Fibromyxoma. An Bras Dermatol 92: 589-590.
- Lee S, Reid MAR (2018) Superficial acral fibromyxoma: A case report with radiological review. Skeletal Radiol 47: 1021-1028.
- Lenz R, Kafka R, Jules K, Bakotic BW (2017) Pedal Presentation of Superficial Acral Fibromyxoma. J Am Podiatr Med Assoc 107: 72-75.
- Lamberti A, Miracco C, Fimiani M, Rubegni P (2017) Superficial Acral Fibromyxoma of the Toe: Unusual location of the mixoid variant. Am J Dermatopathol 39: 849-852.
- Hashimoto K, Nishimura S, Oka N, Tanaka H, Kakinoki R, et al. (2018 ) Aggressive superficial acral fibromyxoma of the great toe: A case report and mini-review of the literature. Mol Clin Oncol 9: 310-314.
- Cullen D, Díaz Recuero JL, Cullen R, Rodríguez P, José L, et al. (2017) Superficial Acral Fibromyxoma: Report of 13 cases with new immunohistochemical findings. Am J Dermatopathol 39: 14-22.
- Jo VY, Fletcher CDM (2014) WHO classification of soft tissue tumours: An update based on the 2013 (4th) edition. Pathology 46: 95-104.
- Vinson RP, Angeloni VL (1995) Acquired digital fibrokeratoma. Am Fam Physician 52: 1365-1367.
- Ma D, Darling T, Moss J, Lee C-CR (2011) Histologic variants of periungual fibromas in tuberous sclerosis complex. J Am Acad Dermatol 64: 442-444.
- Sawaya JL, Khachemoune A (2015) Superficial acral fibromyxoma. Int J Dermatol 54: 499-508.
- Wakabayashi Y, Nakai N, Takenaka H, Katoh N (2012) Superficial acral fibromyxoma of the great toe: Case report and mini-review of the literature. Acta Dermatovenerol Croat 20: 263-266.
Citation: Pache S, Fratelli R, Cedrani J, Filomeno P, Clanton T (2019) Superficial Acral Fibromyxoma: A Case Report of an Uncommon Tumor of the Foot. J Orthop Res Physiother 5: 040.
Copyright: © 2019 Santiago Pache, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.

